Repair of Patella Tendon
Patrick Horrigan
Michael Bellino
Julius Bishop
DEFINITION
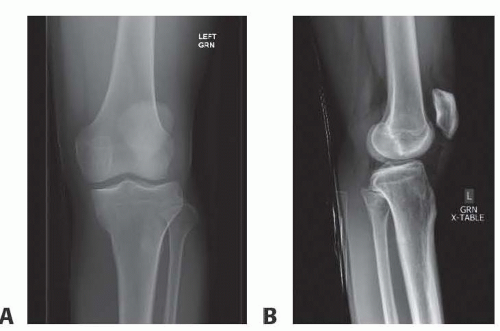
Rupture of the patellar tendon is a disruption of the knee extensor mechanism between the patella and the tibial tubercle.
Complete ruptures cause significant disability, pain, hemarthrosis, and an inability to extend the knee.
Prompt treatment nearly always involves surgery and early motion during rehabilitation.
Missed or delayed diagnosis and treatment can result in significant pain and dysfunction.1
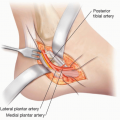
ANATOMY
The patellar tendon is a continuation of the quadriceps tendon, a confluence of the vastus medialis, intermedius, and lateralis tendons and the rectus femoris tendon. It is derived primarily from extending fibers of rectus femoris traversing the anterior surface of the patella.
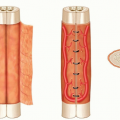
The tendon itself consists of 90% type I collagen. Its fibers are arranged longitudinally relative to the axis of the lower extremity.
It measures approximately 32 mm in width and narrows by several millimeters near its insertion on the tibial tubercle.
PATHOGENESIS
Because degenerative changes are present in most cases, tendinopathy is increasingly given the primary pathogenic role in rupture.5
Rupture can also occur in the setting of direct trauma, recent corticosteroid injections for tendonitis, and systemic disease (patients with chronic acidosis or nephropathy requiring hemodialysis, systemic lupus erythematosus).6
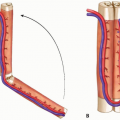
A classic described mechanism is forceful contraction of the quadriceps musculature with the knee in greater than 45 degrees of flexion.7
PATIENT HISTORY AND PHYSICAL FINDINGS
Patients will typically describe an acute popping or tearing sensation during a brief period of forceful quadriceps contraction. This is often followed by acute-onset knee pain, swelling, and inability to bear weight.
A palpable infrapatellar defect around a swollen joint can sometimes be appreciated on the symptomatic knee.
IMAGING
DIFFERENTIAL DIAGNOSIS
Quadriceps tendon rupture
Patella fracture
Medial/lateral collateral ligament rupture
Anterior cruciate ligament rupture
Meniscus tear
Patellar dislocation/subluxation event
NONOPERATIVE MANAGEMENT
Management of patellar tendon ruptures in medically stable adults is surgical. Nonoperative treatment predictably results in tendon retraction and loss of active knee extension strength and extensor lag.7
SURGICAL MANAGEMENT
Surgical goals include restoration of the knee extensor mechanism with strength to allow for early postoperative rehabilitation.
Secondary goals include avoidance of overcorrection resulting in patella baja and altered knee kinematics.
The most commonly described technique to date consists of an augmented primary repair using transosseous patellar tunnels and nonabsorbable suture fixation.8
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree