Grafted fat has many qualities of ideal filler; it is autologous, easily available, and naturally integrated into the host tissues. From a lipoaspirate, the adipose-tissue-derived stromal vascular fraction can be isolated, which is an excellent source of stem/stromal cells, endothelial progenitors, and immune cells. Fat grafting is being increasingly applied in autoimmune diseases, and this article focuses on systemic sclerosis, a rare autoimmune disease characterized by skin fibrosis and microvascular damage. The authors’ approach of using fat graft in the face and adipose-tissue-derived stromal vascular fraction for hands is presented as innovative and promising therapy for patients with systemic sclerosis.
Key points
- •
Systemic sclerosis (SSc) is a rare autoimmune disease characterized by skin fibrosis, microvascular damage, and organ dysfunction.
- •
Facial manifestations in SSc are disfiguring and lead to social disability with psychological distress.
- •
Hand involvement in SSc can lead to a severe disability, with no effective therapy.
- •
Adipose-tissue-derived stem cell therapy has emerged as a therapeutic alternative for regeneration and repair of damaged tissues.
- •
Patients with SSc can benefit from fat grafting: microfat injection in the face to improve skin pliability and quality with esthetic benefit, and injection of the autologous adipose-tissue-derived stromal vascular fraction (ADSVF) in fingers for a trophic effect.
Introduction
SSc (scleroderma) is a chronic systemic autoimmune disease characterized by microvascular abnormalities and progressive skin and internal organ fibrosis. Life-threatening organ lesions leading to pulmonary arterial hypertension, pulmonary fibrosis, and scleroderma renal crisis only affect a minority of patients. By contrast, lesions of the hands and face are almost always present. Although not life-threatening, these manifestations are very obvious, hard to conceal, and lead to disability and worsening quality of life. Facial symptoms are associated with cosmetic disfigurement and limited expression with masklike stiffness of the face. Lesions in the hand lead to substantial difficulty in performing everyday tasks (such as dressing, eating, and applying makeup) as well as an increased risk of chronic digital ulcers (DUs). Therapeutic interventions in this disease are mainly based on the use of vasodilators. No antifibrotic treatment has proven effective. Unlike other autoimmune diseases, immunosuppressive drugs have a limited clinical interest. Thus, functional improvement of hand motion and face appearance represent a real challenge for physicians and a priority for patients who often feel that this aspect of their disease is neglected.
Use of adipose tissue as filling product in plastic and esthetic surgery is an ancient technique. Significant renewal of interest in this approach for the restoration of all volume defects was observed after the description of the LipoStructure ® technique by Coleman. Recently, identification and characterization of the ADSVF, a population that includes mesenchymal-like stem cells, endothelial progenitor cells, and hematopoietic cells, have revolutionized the science showing that adipose tissue is a valuable source of cells with multipotency as well as angiogenic and immunomodulatory properties that facilitate tissue repair. The ease of harvest by liposuction and the abundance of these cells (by comparison to bone marrow) avoid the need for ex vivo expansion before clinical use. Because of these practical factors and the stromal vascular fraction’s ability to differentiate and secrete immunomodulatory, angiogenic, antiapoptotic, and hematopoietic factors, use of adipose tissue is becoming more attractive and is expanding in regenerative medicine.
In this article, the authors present their clinical approach using adipose tissue in the treatment of the face and hands of patients with SSc.
Introduction
SSc (scleroderma) is a chronic systemic autoimmune disease characterized by microvascular abnormalities and progressive skin and internal organ fibrosis. Life-threatening organ lesions leading to pulmonary arterial hypertension, pulmonary fibrosis, and scleroderma renal crisis only affect a minority of patients. By contrast, lesions of the hands and face are almost always present. Although not life-threatening, these manifestations are very obvious, hard to conceal, and lead to disability and worsening quality of life. Facial symptoms are associated with cosmetic disfigurement and limited expression with masklike stiffness of the face. Lesions in the hand lead to substantial difficulty in performing everyday tasks (such as dressing, eating, and applying makeup) as well as an increased risk of chronic digital ulcers (DUs). Therapeutic interventions in this disease are mainly based on the use of vasodilators. No antifibrotic treatment has proven effective. Unlike other autoimmune diseases, immunosuppressive drugs have a limited clinical interest. Thus, functional improvement of hand motion and face appearance represent a real challenge for physicians and a priority for patients who often feel that this aspect of their disease is neglected.
Use of adipose tissue as filling product in plastic and esthetic surgery is an ancient technique. Significant renewal of interest in this approach for the restoration of all volume defects was observed after the description of the LipoStructure ® technique by Coleman. Recently, identification and characterization of the ADSVF, a population that includes mesenchymal-like stem cells, endothelial progenitor cells, and hematopoietic cells, have revolutionized the science showing that adipose tissue is a valuable source of cells with multipotency as well as angiogenic and immunomodulatory properties that facilitate tissue repair. The ease of harvest by liposuction and the abundance of these cells (by comparison to bone marrow) avoid the need for ex vivo expansion before clinical use. Because of these practical factors and the stromal vascular fraction’s ability to differentiate and secrete immunomodulatory, angiogenic, antiapoptotic, and hematopoietic factors, use of adipose tissue is becoming more attractive and is expanding in regenerative medicine.
In this article, the authors present their clinical approach using adipose tissue in the treatment of the face and hands of patients with SSc.
Pathology of scleroderma
Face
Involvement of the face with associated oral complications, esthetic changes, and impairment of the patient’s self-image is found in over 90% of patients with SSc.
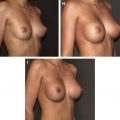
Fig. 1 and Table 1 illustrate the main orofacial findings in patients with SSc.
| Orofacial Findings | Commentaries |
|---|---|
| Skin sclerosis of the face | Very frequent, around 90% of cases. The face becomes amimic or without expression, cutaneous wrinkles disappear, vertical furrows develop around the mouth because of retraction of the skin, the nose becomes sharp, and the lips thin |
| Telangiectasia | Especially located in the face, lips, or the inside of the mouth; they can lead to severe esthetic concerns |
| Skin pigmentation abnormalities | Hypopigmentation and hyperpigmentation mostly observed in the diffuse cutaneous form of scleroderma. Vitiligo is possible |
| Sicca syndrome | Sicca syndrome is detected in approximately 70% of patients with SSc. It is secondary to salivary gland fibrosis |
| Diminished mouth opening | Frequent, around 60%. Thinning of lips and reduction of mouth width (microcheilia) and opening (microstomia) with consequent difficult dental care |
| Osteolysis of mandibular angles | Mandibular bone resorption is mainly encountered in patients with marked facial skin fibrosis: chewing and swallowing movements may be impaired, pain is often reported |
| Altered dentition and difficulties during dental care | Oromucosal involvement include ulcerations, dry mouth, periodontitis, wide periodontal ligament space, dental root resorption, and loose teeth |
Several validated tools have been developed for assessing the involvement of the face. Skin involvement is usually assessed by the Rodnan skin score. This semiquantitative score rates the severity of skin sclerosis from 0 (normal) to 3 (most severe). Xerostomia can be easily measured by sugar test (time to melt a sugar on the tongue, without crunching it) and with the xerostomia inventory index. Mouth opening is assessed in centimeters by measuring the distance between the tips of upper and lower incisive teeth. Elastosonography and three-dimensional photographs can also be used. Mouth-related disability can be assessed by the Mouth Handicap in Systemic Sclerosis (MHISS) scale, which is the first mouth-specific disability outcome measure designed for patients with SSc. This scale evaluates 3 factors: reduced mouth opening, sicca syndrome, and esthetic concerns. Although mouth disability seems to have less weight than hand disability in total disability, the MHISS score explained up to 36% of the variance of the Health Assessment Questionnaire score. This fact highlights the need to specifically assess disability involving the mouth in patients with SSc. Rehabilitation and management of the face is mainly based on physiotherapy with mimic exercises, massage, and self-administered home-based exercises. Mouth and dental care are not specific.
Some case reports have shown the efficacy of autologous fat grafting in the treatment of linear scleroderma. Besides the volumizing effect of mechanical lipofilling, autologous fat grafting also seems to produce trophic and angiogenic effects. The use of autologous grafting of adipose tissue seems to have substantial potential to correct signs of face involvement in SSc.
Hands
Involvement of the hand is common in patients with SSc and represents a large burden in work and daily activities. Hand disability has a multifactorial origin with microvascular lesions, skin sclerosis, tendon retraction, bone and articular involvement, and subcutaneous calcinosis. Each of these lesions causes pain, functional impairment, esthetic issues, and psychological distress.
Vascular involvement
Vascular dysfunction including Raynaud’s phenomenon (paroxysmal vasospasm) ( Fig. 2 ), acrocyanosis (permanent ischemia), and subsequently DUs with their potential complications (infections, digital necrosis, autoamputation) are the main manifestations. Raynaud’s phenomenon occurs in almost all (95%) patients with SSc. DUs, defined as necrotic lesions that occur either at the pulp of the digits (ischemic DUs) or over bony prominences (mechanical DUs), occur in up to 50% of patients with limited or diffuse SSc. DUs typically occur early in the course of SSc. A study assessing functional limitations owing to DUs among patients enrolled in the Digital Ulcer Outcome (DUO) Registry showed for patients with 0, 1 to 2, and 3 or more DUs at enrollment an increasing mean overall work impairment. Similarly, the ability to perform daily activities was impaired in patients with DUs and this impairment increased with the number of DUs.
Skin involvement
Skin sclerosis is characterized by variable extent and severity of skin thickening and hardening. Edematous swelling and erythema may precede skin induration. On the hands, this condition is called sclerodactyly (see Fig. 2 ). As the disease progresses further, however, the skin loses its ability to stretch and becomes shiny because it tightens across the underlying bone. Eventually, in severe cases, the fingers may lose the ability to move, with vicious attitude leading to claw deformities (see Fig. 2 ).
Flat red marks, known as telangiectasias (see Fig. 2 ), may appear in various locations, especially in the palms. Although they can cause esthetic concerns, they do not cause functional disturbance.
Calcinosis (see Fig. 2 ) is characterized by calcium deposition in skin and subcutaneous tissues. Calcinosis is commonly associated with SSc; approximately 10% to 30% of patients develop calcinosis. These deposits are typically found on the fingers, hands, and on the skin above wrists, elbows, and knees. Calcinosis can lead to functional impairment, painful ulcers, and infections.
Bone and joint involvement
Distal phalangeal resorption with bone loss (acro-osteolysis) can be observed in SSc (see Fig. 2 ). Arthralgia and arthritis are observed in around 50% of cases. Metacarpophalangeal and proximal interphalangeal arthritis are also frequent. This joint destruction is not as severe as it is in rheumatoid arthritis but can lead to finger deformities and claw hand deformity.
Clinical measures for hand involvement evaluation include: (1) the semiquantitative estimation of skin thickness (modified Rodnan skin score applied to hands, score 0–18); (2) a visual analog scale of pain in the hands; (3) mobility and strength tests such as Kapandji test, grip and pinch strength, and measurement of the intercommissural distances; (4) the Hand Mobility in Scleroderma index, which specifically assesses hand global mobility in patients with SSc, but does not evaluate hand disability for activities of daily living; and (5) the Cochin Hand Function Scale (CHFS), a functional disability questionnaire about daily activities validated in rheumatoid arthritis and hand osteoarthritis, as well as SSc. The CHFS is a valid instrument for assessing hand disability in patients with SSc. It was shown that hand functional disability is the major component of global disability, contributing to 75% of global disability in patients.
To date, therapeutic interventions for patients with hands affected by SSc have mainly focused on the treatment of vascular manifestations such as Raynaud’s phenomenon and DUs. Patients can get some relief with physiotherapy. Unfortunately, there is scant research showing that exercise stops the worsening of scleroderma ( [CR] and [CR] ). Full rehabilitation is rarely guaranteed, but function can be retained through physiotherapy. Movement can help retard the contractures and help the patient maintain strength and range of motion.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree