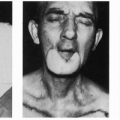
Reconstruction of The Cervical Esophagus With Skin Flaps
C. E. SILVER
R. J. BRAUER
EDITORIAL COMMENT
These adjacent skin flaps are of historical significance only.
Tumors of the hypopharynx and cervical esophagus are often treated by total pharyngolaryngectomy with partial or total esophagectomy. Repair of the surgical defect is a complex task. Reconstructions have been performed using many variations and combinations of local tissues, skin grafts, stents, regional flaps, free flaps, and transpositions or free transplantations of abdominal viscera. The ideal reconstruction would entail a single-stage operation, employ nonirradiated tissues, require no thoracic or abdominal surgery, and have minimal morbidity and mortality. Although marked improvements in reconstructive procedures have occurred, there is still no single procedure that can be applied to all patients with uniformly reliable results. Various methods of pharyngoesophageal reconstruction using skin flaps have the advantage of not requiring abdominal or thoracic operations, but they have other limitations.
INDICATIONS
Many of the standard cervical skin flaps have been replaced by either the deltopectoral flap (see Chapter 216) or the pectoralis major musculocutaneous flap (see Chapter 218) or a combination of these flaps. When these flaps are unavailable or contraindicated for some reason, the cervical skin flap (Wookey) (1, 2) or its modifications can be used.
FLAP DESIGN AND DIMENSIONS
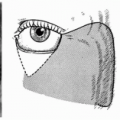
The procedure described by Wookey (2) employed a laterally based rectangular cervical skin flap for reconstruction following pharyngolaryngectomy. The upper edge of the flap was sutured to the cut edge of the pharynx and the lower edge to the esophagus. The flap was then folded back onto itself, creating a lateral fissure in the neck. All the pharyngeal and esophageal anastomoses were completed at the first stage. The opposite cervical skin was mobilized to resurface the neck, or if necessary, a skin graft was used. At a second stage, the lateral fissure was closed. In most cases, this could be accomplished by simple incision and direct suture along the edges of the defect (3).
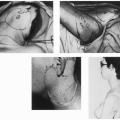
In a modified procedure (4, 5, 6, 7), the cephalocaudal length of the flap was increased by including the submental skin. This allowed a greater length of esophagus to be resected. The pharyngeal and esophageal anastomoses were only partially completed at the first stage in order to simplify the procedure. At the second stage, the neoesophagus was completed and the cervical defect was resurfaced by transfer of a thoracoacromial skin flap.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree