Treatment of the aging lower eyelid is determined by the anatomic variables noted for each surgical candidate. Although surgeons have traditionally considered dermatochalasis, fat pseudoherniation, and eyelid position as the main treatment objectives in lower blepharoplasty, the vector of the infraorbital rim and the anterior plane of the cornea, tear trough, and aging in the midface also merit critical consideration. In this article, indications and technical aspects, the transconjunctival and external approaches, fat excision versus fat repositioning, and suborbicularis oculi fat lifting and fat transplantation are discussed and the authors’ preference for the various methods of lower blepharoplasty is presented. Common adjunct procedures used to supplement lower blepharoplasty techniques and the role of injectable fillers in periocular rejuvenation are also mentioned.
Lower eyelid rejuvenation requires careful consideration of all layers of the eyelid and the transition to the midface. Hereditary anatomic variations in these structures and the changes typically observed with aging must be considered in optimizing periocular treatment outcomes. In the preoperative period, a thorough periocular examination is critical in determining optimal treatment strategies. The patient’s medical history, expectations, and motivations must also be clearly defined before further surgical planning. Fat pseudoherniation, dermatochalasis, orbicularis hypertrophy, and prominent tear trough deformity are the most common indications for lower eyelid rejuvenation. Most commonly, fat pseudoherniation and prominence of the tear trough are addressed through lower eyelid blepharoplasties using either transcutaneous or transconjunctival techniques, with or without fat repositioning. Suborbicularis oculi fat (SOOF) lifting and fat transplantation have also been described as methods for softening the prominent tear trough in select cases. The indications and methods for each approach are described, with particular attention dedicated to the senior author’s (KAL) technique for transconjunctival lower eyelid blepharoplasty with orbital fat repositioning, the most commonly indicated lower eyelid procedure in the author’s experience. Adjunctive procedures for skin resurfacing and the utility of tear trough augmentation with fillers are also briefly described.
Anatomic changes with aging
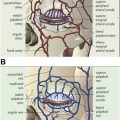
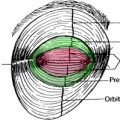
The periorbital area demonstrates some of the earliest signs of facial aging. The integrity of the septum diminishes with advancing age such that orbital fat pseudoherniation leads to the appearance of bags or fullness in the lower eyelid. With advancing age, increased laxity in the structurally supportive tissues of the orbit also leads to relative settling of the globe, further exacerbating fat pseudoherniation through the areas of septal weakening. Laxity in the lower eyelid septum can also be hereditary, as evidenced by the appearance of fat pseudoherniation in many adolescents and young adults. Orbital fat pseudoherniation contributes to the observed deepening of the nasojugal fold, or tear trough, that is associated with aging and gives the eyes a more fatigued, haggard appearance.
Below the tear trough and orbital rim, the fatty tissues of the midface and cheek lose volume and descend as aging progresses. In a similar fashion, the SOOF loses volume and descends over time. In a youthful face, cadaveric studies have demonstrated that the SOOF attaches to the arcus marginalis at the level of the inferior orbital rim. With aging, SOOF descent and volume loss contribute to deepening of the tear trough deformity and lengthening of the lower eyelid. Concurrently, the orbicularis oculi muscle of the lower eyelid can hypertrophy, leading to heaviness, sagging, and deeper rhytids in the lower eyelid. These changes in midfacial fat, SOOF, and orbicularis oculi contribute to the increasing potential for eyelid malposition, deepening of the tear trough, and rounding of the eye. Lower eyelid skin also progressively loses its elasticity with aging, leading to progressive dermatochalasis with fine and deep rhytids.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree