and Emir Q. Haxhija2
(1)
Department of Plastic Surgery and Burns, Institute for Mother and Child Health Care of Republic Serbia, University of Belgrade, New Belgrade, Serbia
(2)
Department of Pediatric and Adolescent Surgery, Medical University Graz, Graz, Austria
Keywords
AuriculaeChildrenPinnaplasty2.1 Introduction
Surgical correction of prominent ears (otoplasty) is a cosmetic procedure commonly performed in the pediatric population, mostly by plastic and pediatric surgeons, and otorhinolaryngologists [1–13]. Children with prominent ears older than 5 or 6 years are generally complaining of being teased about their ears and usually style their hair to camouflage their deformity [3, 4, 10].
There is almost unlimited number of procedures for correction of the prominent ear [1, 5–14]. Parents are often the initiators of the idea for ear correction, and in most cases they have to bring a decision about the surgical treatment for their children [2]. The understanding between the surgeon, child, and parents has to be well established, and it is very important that the child cooperates with the surgeon (most surgeons wait until awareness of the deformity arises) [3, 10, 13]. Psychological aspect of this procedure and its impact on the child are also extremely important [2–4, 13].
Different terminologies have been used for this deformity: prominent ears, “bat” ears, apostasis otis, prominauris, etc. [4, 6, 8–13].
2.1.1 Epidemiology
2.1.2 Embryology
At about 40 days of gestation, the auricle is derived from the mesoderm of the first two branchial arches (six hillocks of His) [4, 10–12, 15–17]. During the third month of gestation, the auricle’s protrusion increases, and by the end of the sixth month, helix and antihelix are nearly completely formed [15]. The auricle is fully shaped at birth, approximately 85% of auricular growth is finished at 3 years of life and nearly adult size is achieved by age 5 or 6 years [4, 6, 11, 12, 15]. At 6 years, the ear size values are nearly the same for both sexes: 34 mm width in boys and girls, 55 mm length in boys and 54 mm in girls, and 22 mm protrusion in boys and 20 mm in girls [10, 12, 13]. Ear length is definitive by age of 15 years in boys and by age of 13 years in girls (60–65 mm), and ear width is complete by age 10 in girls and age 13 in boys (35 mm) [10–12]. Otoplasty in children aged 5–8 years has no significant influence on later auricular growth [4, 12].
2.1.3 Anatomy
The structures that formed the auricle are the helix, the antihelix, the antihelical scapha, the antihelical crura, the tragus, the antitragus, the cavum conchae, the cymba conchae, and the lobule (Fig. 2.1) [4, 9–11]. Fibroelastic auricular cartilage is medially covered by connective tissue and skin and laterally by skin only [4, 12]. The lobule is mainly composed of adipose and connective tissue [4, 16]. Several intrinsic and extrinsic muscles and ligaments influence the auricular shape [12]. The arterial supply to the auricle is derived from the posterior auricular, superficial temporal, and occipital arteries, and sensory innervation is provided by the auriculotemporal and great auricular nerve and branches of cranial nerves (CN) VII, IX, and X [11, 12, 15].
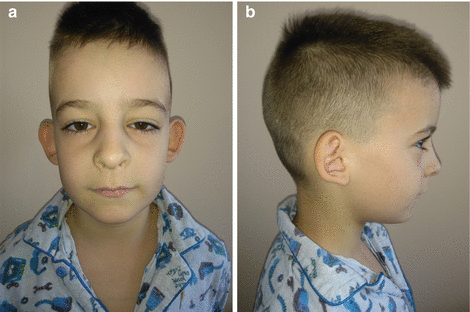
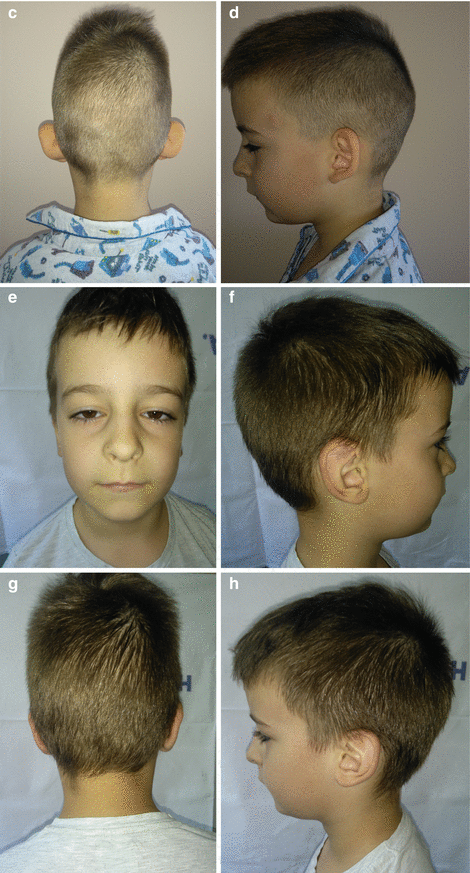


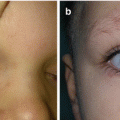
Fig. 2.1
Reconstruction of bilateral prominent auricle with suture technique: (a–d) preoperative view; (e–h) postoperative view
2.2 Psychosocial Aspects
Children have to be well motivated for correction of protruding ears because it can provoke long-term emotional consequences, and there is also parental responsibility since they give the consent for their children (if they are in preschool or in early school age) [2, 3]. The decision about surgery should be based on the needs of the child, not on pressure from the parents [2–4]. Children usually have better quality of life after correction of prominent ears, but an operation cannot guarantee that the child will be happier afterwards, even if the quality of surgical correction is good [1–4, 18].
2.3 Preoperative Evaluation
The precise anamnestic data should be taken (especially about excessive bleeding and poor wound healing) [1, 4, 12]. If there is a history of previous surgery and hypertrophic scarring or keloids, surgery has to be performed with maximum precautions [4, 14]. Both the patient and parents have to be well informed about every detail of the surgical procedure along with potential risk and complications [4, 6, 19]. The patient has to be intellectually and emotionally mature enough to cooperate [4, 12]. Otoplasty is contraindicated if patient has unrealistic expectations or if the patient is judged to be noncooperative postoperatively [3, 4, 13]. General anesthesia is recommended for children under 14 years of age (risks should be explained), and for teenagers local anesthesia with sedation can also be an option [4, 6, 11].
A careful preoperative examination of the auricles by thirds has to be performed, and any pre-existing asymmetry should be presented to patients [1, 4, 6, 8, 10, 13].
Cartilage consistency and thickness with the other ear abnormalities and associated anomalies should be evaluated; preoperative photography has to be obtained (for evaluation of the ear from the lateral direction, the patient should be in Frankfort horizontal plane) [4, 6, 8]. Distance between the lateral helical rim and the mastoid region is usually 17–21 mm, and the angle between mastoid and the auricle is approximately 30° [4, 6, 11–13, 18, 20].
2.4 Treatment Options
The goal of otoplasty is to restore normal anatomic features: however, perfection is hard to achieve [7, 8, 12, 13]. The decision about the technique that will be used depends of the deformity of the ears, patient demands, technical equipment, and surgeon’s experience [2–4, 6, 7, 9–13, 19–21, 23–27].
2.5 Time of Otoplasty
2.6 Techniques of Otoplasty
The basic goals of otoplasty according to Mc Dowell are as follows: all trace of protrusion of the upper one third of the ear must be corrected; from the front view, the helix of both ears should be seen beyond the antihelix; the helix should have a smooth and regular line through; the postauricular sulcus should not be markedly decreased or distorted; the ear should not be placed too close to the head; and the position of two ears should match fairly closely—to within 3 mm at any given point [6, 8, 12].
There are between 100 and 200 procedures that have been published for correction of prominent ears [4–12, 14, 16, 20, 22–27]. Surgical methods can be essentially divided into pure stitching techniques, pure incision techniques, and combined stitching-incision techniques (also are divided in cartilage-breaking and cartilage-spearing techniques) [1, 6, 12, 14, 27]. There has been increasing criticism of cartilage-cutting techniques [7, 19, 20, 27].
2.6.1 Pure Stitching Techniques
2.6.1.1 Mustardé Technique
This is one of the most widely used techniques to correct the prominent ear [4–6, 8, 11, 12]. Mustardé described an otoplastic technique which is suitable for folding an antihelical fold [4, 6, 22, 25]. The mattress sutures (nonabsorbable, transparent or white) are placed using a retroauricular access through the auricular cartilage and the perichondrium, without penetrating the ventral skin [22, 25]. This technique mainly addresses the superior third of the ear, it is suitable for soft or thin cartilage, and it can be combined with a lobulopexy and/or cavum rotation [4, 6, 12, 13, 25].
2.6.1.2 Furnas Technique
Furnas described a technique for overdeveloped conchal bowl and well-formed antihelical fold [4–6, 10, 12, 27]. Nonabsorbable sutures which penetrate entirely through both the auricular cartilage and the mastoid periosteum create a lasting correction of the conchal prominence [5, 6, 10]. It can be also used in conjunction with Mustardé mattress sutures for correction of antihelical fold underdevelopment [5, 6, 12]. Narrowing of external auditory canal is a complication of this technique described in literature if the mastoid sutures are placed too anteriorly [6, 12].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree