Noteworthy cases
Every practitioner has interesting, unique, and noteworthy experiences to share. I believe each and every one of us have done something very different from our colleagues. It could be in the number (volume) of cases, the application of newer methods to deal with old problems, development of a simpler method to deal with the same old problems, development of a cost-effective approach, combining different techniques for a case, or developing a new application altogether. Any of these are always worth mentioning or sharing. I always believe in sharing and learning, and have been doing this at many meetings, lectures, classes, or workshops over the past 18 years of my radiofrequency surgery practice experience.
I always believe the words of Dr. Bernie Siegel: “It is always in the interest of the patient’s recovery to try all kinds of promising therapies.”
I will share three cases in which I feel the best features of radiofrequency surgery are worth mentioning.
Case 1: Multiple tongue papilloma (papillomatosis)
I treated this case in the early days of my practice. This patient was carrying these multiple warts over his tongue for a year (Figure 21.1), and had consulted various doctors (general surgeon, otorhinolaryngologist, dermatologist, faciomaxillary surgeon, and homeopathic and Ayurvedic specialists). He was treated with electrocautery and excision, which were followed by recurrence. The patient was himself a radiologist.
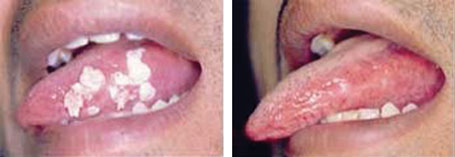
Figure 21.1Multiple warts on left side of tongue cleared completely with no recurrence. (From Biju Vasudevan, Procedural Dermatosurgery, A Step by Step Approach, Jaypee Brothers Medical Book Publishers Pvt. Ltd., 2018.)
How I treated this case:
I asked the patient to use a lignocaine viscous solution for topical anesthesia before coming to the clinic. This gave a sufficient numbing effect. In case the numbing was not up to the desired level, I injected lignocaine 2% underneath the warty lesions.
I used a broad needle electrode. Power was 2 to 4 maximum. The waveform selected was electrodessication.
The lesions were touched for 5 to 10 seconds at intervals of half a minute several times until the warts showed visible whitening due to dehydration or a bit of charring by the browning effect on warty tissue.
These lesions were then left to desquamate and fall off automatically. This happened in a week’s time.
The patient was treated fortnightly four to five times. This cleared all warts completely.
Follow-up was done fortnightly for 3 months for recurrence.
Any recurrences were immediately treated.
There were no other features of immunodeficiency.
There has been no recurrence in the past 15 years and the result is excellent to date.
Postprocedure pain was bearable and lasted for the whole day of the procedure. The treated lesions desquamated within one week each time. Recurrence is less because in electrodessication, the electrocoagulation waveform is used and the heat generated dissipates into surrounding tongue tissue deeper to cause necrosis at least a millimeter away from the lesion thus clearing off the newly invaded cells.
Take-home message: The electrodessication technique used judiciously and convincingly has the potential to deliver marvelous results. It may take a longer time to give a complete result but it is less painful, more acceptable, and more convincing. It scores over all other modalities and is definitely far better than surgical excision done by an otorhinolaryngologist, or oral or general surgeon.
Case 2: Giant condyloma acuminata on perianal area
This was a case of an 18-year-old male patient, who I treated two years back. He had consulted general practitioners and specialists near his native place outside India and was offered some treatment that did not help. He had come for a vacation to India where his grandparents lived. When I saw him he had huge masses of warty tissue (florid appearance) growing at the perianal area near the anal orifice. He had approached me for complaints of bleeding per rectum. He had developed sepsis in those masses and was foul smelling. He was treated with liquid podophyllum 2 days earlier by a dermatologist. I treated him with an oral antibiotic and called for review after 2 days. On the follow-up visit I started photo documentation and advised radiofrequency treatment in two to three sessions at 1- to 2-week intervals (Figures 21.1 to 21.9).
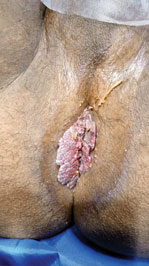
Figure 21.2Giant condyloma acuminata on perianal area.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree