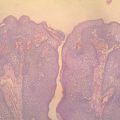
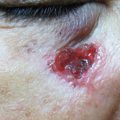
Specific applications: Radiofrequency commonality
This chapter covers the most common of indications for which radiofrequency (RF) surgery is used and is famous for or is always referred to for. These indications are the bread and butter of a radiofrequency office surgery. Everyone who desires to use radiofrequency surgery in dermatologic surgery or those who have decided to start dermatologic surgery in an office using radiofrequency surgery must be thoroughly acquainted with the minutest details of these indications for the best results.
Refer to Table 13.1 for general guidelines in treating these indications. The power settings are given as per my experience (with the Ellman Surgitron), hence the reader is advised to modify the settings according to individual choice and experience.
Skin lesion | Waveform | Electrode | Power* |
|---|---|---|---|
Moles or melanocytic nevus | RFE | L | 3–5 |
Verruca vulgaris | RFE/RFB | L/T | 3–5 |
Verruca plana | RFD | S/D | 1–2 |
Skin tags | RFE/RFB | S/L | 3–5 |
Skin tags | RFD | S/D | 1–2 |
Dermatosis papulosa nigra | RFD | S | 1 |
Milia | RFD | S | 1 |
Corns/calluses | RFE/RFB | S and L/T | 3–8 |
Keratoses | RFE | L | 3–4 |
Sebaceous cysts | RFE | TW/S | 3–4 |
Note: D, broad needle electrode for desiccation and fulguration; L, round loop electrode; RFB, radiofrequency blend waveform; RFD, radiofrequency desiccation waveform; RFE, radiofrequency excision (cut) waveform; S, straight needle electrode; T, triangular electrode; TW, thin wire electrode.
* Power settings vary with the equipment used.
Perhaps the most impressive result of radiofrequency surgery is the excision of moles or intradermal nevi, also called melanocytic nevi. However, warts or verrucae are among the most common of all conditions to be treated because of the higher incidence and potential for infection and recurrence.
A stepwise guide to treat the aforementioned common indications are given in the following sections.
Moles or intradermal nevi or melanocytic nevi
People are very conscious of their appearance today. Any moles on the face and neck bring so many young patients to demand removal. These people feel embarrassed by the moles, thinking they spoil their looks. Or they would like to have a blemish-free face or neck.
Moles are generally removed for cosmetic purposes. Occasionally, patients seek advice for a fast growing mole or new mole appearance fearing possibility of cancer.
Following are some important criteria for selecting moles for excision by radiofrequency surgery:
Moles should be significantly raised above the skin surface. Only such moles can be easily removed without much scarring as their depth does not extend into the lower dermis.
Flatter moles can be deeper in depth, hence can cause easy recurrence. Hence, such cases should be counseled against removal.
All moles must be sent for histopathology as a routine to confirm diagnosis and as a precaution to rule out dysplastic changes of malignancy.
Mole excision technique
See Figures 13.1 to 13.20.
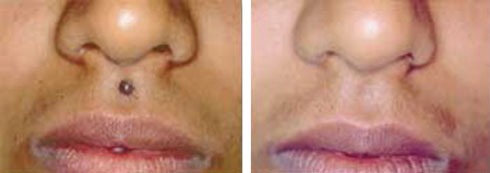
Figure 13.1Excellent removal of mole without residual scar. (From Biju Vasudevan, Procedural Dermatosurgery, A Step by Step Approach, Jaypee Brothers Medical Book Publishers Pvt. Ltd., 2018.)
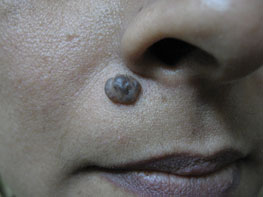
Figure 13.2Mole before removal.
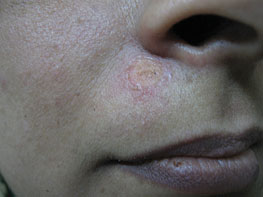
Figure 13.3Immediately after mole excision (excellent and clean postoperative wound).
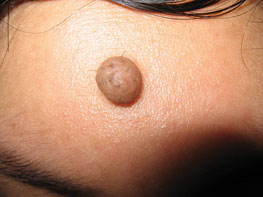
Figure 13.4Mole before removal.
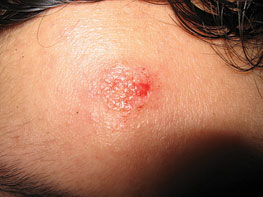
Figure 13.5Immediately after mole excision (excellent and clean postoperative wound).
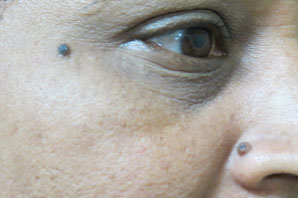
Figure 13.6Two moles before excision.
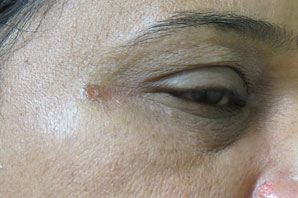
Figure 13.7Immediately after mole excision.
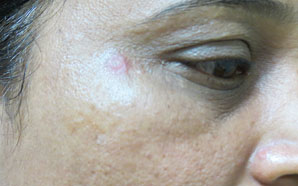
Figure 13.8Two weeks after mole excision.
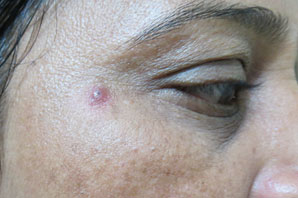
Figure 13.9One month after mole excision.
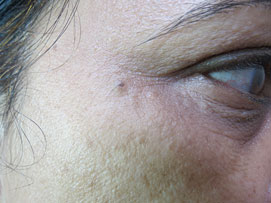
Figure 13.10One year after mole excision, mild recurrence seen near right eye.
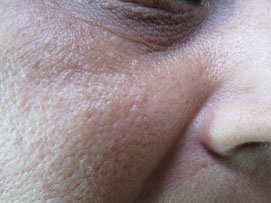
Figure 13.11One year after mole excision (no recurrence on nostril), no scar seen.
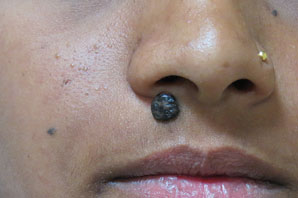
Figure 13.12Mole near right nostril.
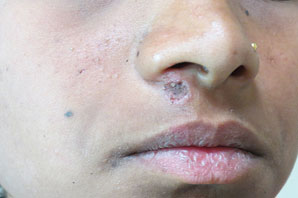
Figure 13.13Immediately after mole excision (black mole tissue persists in deeper skin layer).
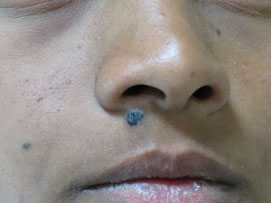
Figure 13.14Recurrence after 2 months.
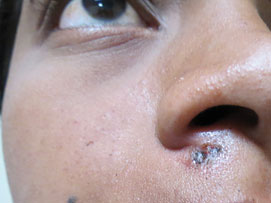
Figure 13.15Immediately after second excision. If mole tissue still persists, it will require removal by a cosmetic surgeon.
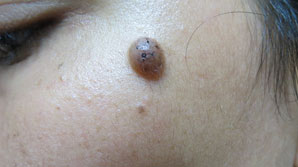
Figure 13.16Mole on left cheek.
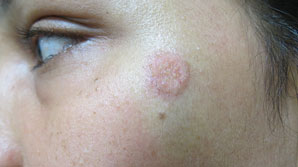
Figure 13.17Mole on left cheek immediately after excision.
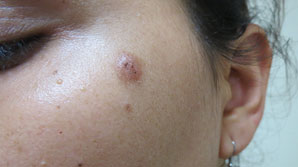
Figure 13.18One month after mole excision shows recurrence.
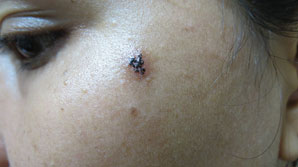
Figure 13.19Two months after mole excision shows significant recurrence.
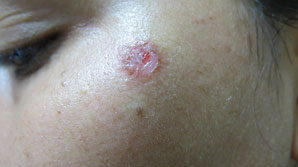
Figure 13.20Mole excised again.
All preoperative requisites are checked and completed.
Local anesthetic testing done, informed consent taken, photo documentation completed.
After sterilization, a lignocaine with adrenaline injection is given underneath the nevus intradermally.
Wait 5 minutes to start the procedure.
Electrode choice is almost always round loop.
The waveform is always cut or fully filtered.
Power is set to 3 and the handpiece containing the electrode is held at a right angle or perpendicular to the skin surface.
A rough assessment is made to confirm whether the power selected is optimum to make a microsmooth incision.
Once the optimum power is set, the first aim is to remove a small piece or in toto of the skin lesion to be sent for histopathology. This requires operative experience and skill to take a biopsy piece in one stroke. Holding and slightly stretching the adjoining skin between the index finger and thumb of the inactive hand, the bulk of the mole tissue is excised in a single stroke. The excised mole tissue is put in formol saline for histopathology.
The rest of the mole tissue is trimmed with the shave excision method until all remnants of mole tissue have cleared.
If in case after reaching the level of the papillary dermis the mole tissue is still visible in some portion, especially in the center, it is desirable to leave it as it is to prevent scarring. The patient is shown the condition on-table and explained the possibility of scarring if efforts are made to remove deeper mole tissue, and that it is desirable to wait and watch for 6 to 8 weeks to see if it regrows. In that case, if the patient is still demanding to remove it, this will require deeper excision leading to scarring.
Once the mole tissue is excised, pressure hemostasis is employed with saline-soaked gauze for 5 minutes, which usually stops the capillary bleeding. I prefer not to use electrocoagulation unless required.
The most important job of blending is done now to blend the open wound tissue with the adjoining epidermis of intact skin with the same electrode at a lower power of 1 or 2 only. The electrode is kept at a right angle or tilted to achieve this result. Good experience is required to do this skillfully. It is a very critical step for superior cosmetic results.
A postoperative photograph is taken.
The wound is dressed with antibiotic ointment.
Postoperative care is explained and medicines prescribed (refer to Chapter 17).
Follow-up
All patients are advised to come for a follow-up visit after one week.
Wound healing is closely observed (whether complete or not).
If wound has fully healed, the patient is advised to revisit after 2 weeks.
In the next visit, the healed wound is closely observed for the start of hyperpigmentation or erythema in the healed scar.
Any signs of hyperpigmentation is treated with standard bleaching creams for 2 to 4 weeks until it clears.
Patient is later called at the end of one month approximately to see the response to bleaching creams to find out whether there are any early signs of recurrence of the mole.
If there is no recurrence at the end of 8 weeks after surgery, it is unlikely to recur.
Some patients (<10%) show recurrence in the form of a small, black-colored, dotlike spot or frank mole recurrence.
Decision about repeat excision is taken at the end of 6 to 8 weeks.
The recurrent mole is always reexcised under local anesthesia in a similar fashion but with a slightly deeper excision to prevent further recurrence. The patient is well informed beforehand about a deep excision and the possibility of a superficial scar later.
A small dotlike clump of melanocytes may not increase in size and may be left untreated as the dot is hardly seen. This position can remain stable for years.
Any superficial scar resulting from excision can be effectively resurfaced using a special technique of radiofrequency for scar resurfacing later.
Any postoperative hyperpigmentation or erythema or superficial scar becomes virtually invisible after 2 months as the collagen remodeling is completed.
Warts (verruca plana, verruca vulgaris, digitate, or filiform warts)
Warts, or verrucae, are some of the most common indications for RF surgery. These occur in all age groups and there is no effective oral treatment for it. They affect the skin of any area from the scalp to the soles. Being of viral origin with the potential to spread to other areas or to other people, urgent removal remains the best option. Being symptomless, patients commonly neglect them until the warts affect some area on the face or start causing discomfort or pain, especially the periungual and the plantar ones. Patients usually try all kinds of alternate therapies such as home remedies or advertised products, or alternative medicines like homeopathy or herbal medicine before considering RF surgery.
Approach to warts treatment
Always take a detailed history of patients and examine them thoroughly to have a proper idea of the number of warts and their distribution on the body.
Sometimes only a few warts are present with the rest likely to be microscopic and thus invisible, whereas sometimes there could be numerous warts spread all over the body.
Patient’s immune status should be assessed and may have to be investigated if in doubt.
If there are a few on the face, a treatment has to be planned that will give the best cosmetic result.
If the warts are on the scalp, the whole area must be thoroughly examined because this and beard areas are notorious for recurrence and warts can be hidden in hairy areas.
If the number of warts is in the dozens, plan treatment in two to three sessions at intervals of 1 to 2 weeks.
If plantar warts are multiple, again all cannot be treated in one session.
Periungual, plantar, and scalp warts are likely to bleed more.
Sometimes skin warts are seen spread over mucosal areas such as nasal, oral, and genital areas. These require a different approach (see later).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree