How is nerve conduction in the carpal tunnel reported?
Nerve conduction is reported as “latency” in milliseconds (ms).
 What is “latency”?
What is “latency”?
Latency is the time it takes for an electrical stimulus to travel along a nerve from the site of stimulation to a recording electrode in a target muscle.
 What is the normal value for motor latency at the carpal tunnel?
What is the normal value for motor latency at the carpal tunnel?
Less than 4.0 ms.
 How is nerve conduction at the elbow reported?
How is nerve conduction at the elbow reported?
Nerve conduction is reported as velocity in meters per second (m/s).
 What is a clinically significant decrease in velocity at the elbow?
What is a clinically significant decrease in velocity at the elbow?
A decrease in velocity of 10 m/s or more is considered clinically significant.
 What is the difference between compressive neuropathies and peripheral neuropathies?
What is the difference between compressive neuropathies and peripheral neuropathies?
In peripheral (systemic) neuropathies, the nerve conduction is decreased diffusely both proximally and distally in multiple nerves. In compressive neuropathies nerve conduction is decreased distal to the site of compression.
 What are typical electromyography (EMG) findings for long-standing nerve compression and axonal damage?
What are typical electromyography (EMG) findings for long-standing nerve compression and axonal damage?
EMG will demonstrate wide biphasic fibrillation potentials in the presence of long-standing nerve compression with axonal damage.
 What is double crush syndrome?
What is double crush syndrome?
The double crush syndrome hypothesizes that a site of proximal nerve compression in series with a site of distal compression of the same nerve results in clinical neuropathy; whereas independently, neither site of compression is severe enough to result in clinical neuropathy.
 What is the treatment of choice for an ulnar neuroma-in-continuity with intact motor function?
What is the treatment of choice for an ulnar neuroma-in-continuity with intact motor function?
The current optimal therapy involves micro-dissection of the neuroma using electrostimulation to identify and preserve motor fascicles. En bloc resection of the neuroma is inappropriate, as this would sacrifice intact nerve fascicles.
 What are some nonsurgical modalities that can be used to desensitize an amputation stump neuroma?
What are some nonsurgical modalities that can be used to desensitize an amputation stump neuroma?
Vibration, massage, and transcutaneous nerve stimulation.
 What is complex regional pain syndrome?
What is complex regional pain syndrome?
Complex regional pain syndrome (CRPS) is recognized as a constellation of symptoms including pain at rest, vasomotor instability, and swelling that results in functional impairment of the affected hand or limb. It is usually the result of previous limb trauma or surgery.
 What diagnostic study can help establish the diagnosis of CRPS?
What diagnostic study can help establish the diagnosis of CRPS?
Three-phase bone scintigraphy has been shown to be highly specific for the diagnosis of CRPS in the upper limb.
 ULNAR NERVE
ULNAR NERVE 
THORACIC OUTLET SYNDROME
 What nerve is affected with thoracic outlet syndrome (TOS)?
What nerve is affected with thoracic outlet syndrome (TOS)?
Lower trunk of brachial plexus with symptoms mimicking cubital tunnel syndrome.
 What are the contents of the “thoracic outlet”?
What are the contents of the “thoracic outlet”?
Subclavian vein, subclavian artery, and brachial plexus.
 In what gender is TOS more prevalent?
In what gender is TOS more prevalent?
Female (3.5:1).
 Among the population of patients with cervical ribs, how many are bilateral?
Among the population of patients with cervical ribs, how many are bilateral?
50%.
 When do patients with TOS typically get their symptoms (ulnar-sided numbness)?
When do patients with TOS typically get their symptoms (ulnar-sided numbness)?
Patient’s symptoms worsen when their hands are elevated above their head.
 What is Adson maneuver?
What is Adson maneuver?
Dampening of radial pulse with inhalation, neck extension, and head rotation to the affected side in patients with TOS. There are varying descriptions of how to perform this maneuver.
 How accurate is an Adson maneuver?
How accurate is an Adson maneuver?
False positives are very common and thus the Adson maneuver is valued in terms of historical interest only.
 What is Wright maneuver?
What is Wright maneuver?
The Wright maneuver is reproduction of TOS symptoms and/or dampening of radial pulse with arm hyper-abducted with the patient’s head positioned in neutral or turned contralateral.
 How accurate is Wright maneuver?
How accurate is Wright maneuver?
The Wright maneuver is positive in 7% of normal patients thus should be used only to support a diagnosis of compression in patients with arterial symptoms.
 What is Roos maneuver?
What is Roos maneuver?
The Roos maneuver involves placing both arms into 90 degrees of abduction and external rotation and the patient is asked to open and close the hands for 3 minutes. Patients with TOS have reproduction of their symptoms, while those without TOS generally experience forearm fatigue.
 How accurate is Roos maneuver?
How accurate is Roos maneuver?
Of the three maneuvers described, the Roos is the most accurate. However, some patients with carpal tunnel syndrome (CTS) and no TOS will develop symptoms limited to the median nerve distribution.
 What are the electrodiagnostic testing results seen with TOS?
What are the electrodiagnostic testing results seen with TOS?
Negative EMG for ulnar nerve, positive somatosensory-evoked potentials with arm in offending position.
 What is the first-line therapy for TOS?
What is the first-line therapy for TOS?
Conservative treatment with exercises to strengthen the shoulder girdle, weight loss, and occasionally breast reduction in women are first line.
 Name the two approaches to the thoracic outlet.
Name the two approaches to the thoracic outlet.
Supraclavicular and transaxillary.
 What is similar and what is different about the presentation of TOS and cubital tunnel syndrome?
What is similar and what is different about the presentation of TOS and cubital tunnel syndrome?
Both TOS and cubital syndrome can present with ulnar distribution numbness, although TOS also presents with medial forearm numbness whereas cubital tunnel syndrome does not.
CUBITAL TUNNEL COMPRESSION
 How do you tell the difference between ulnar nerve compression at the cubital tunnel from compression at the wrist (Guyon canal)?
How do you tell the difference between ulnar nerve compression at the cubital tunnel from compression at the wrist (Guyon canal)?
Diminished sensation on the dorsoulnar hand is present with cubital tunnel syndrome. This is due to the fact that the dorsal sensory branch of the ulnar nerve exits the ulnar nerve approximately 7 cm proximal to the pisiform, to provide sensation to the dorsoulnar hand.
 What is the distribution of motor weakness seen with cubital tunnel syndrome?
What is the distribution of motor weakness seen with cubital tunnel syndrome?
Motor weakness is seen in the flexor digitorum profundus (FDP) of ring and small fingers, as well as the ulnar intrinsic muscles.
 Describe Froment sign.
Describe Froment sign.
With ulnar nerve palsy, patients compensate for lack of adductor pollicis (ulnar innervated) function by flexing the thumb interphalangeal (IP) joint (pinch power is then provided entirely by the median-innervated flexor pollicis longus [FPL]).
 What are potential sites of ulnar nerve compression?
What are potential sites of ulnar nerve compression?
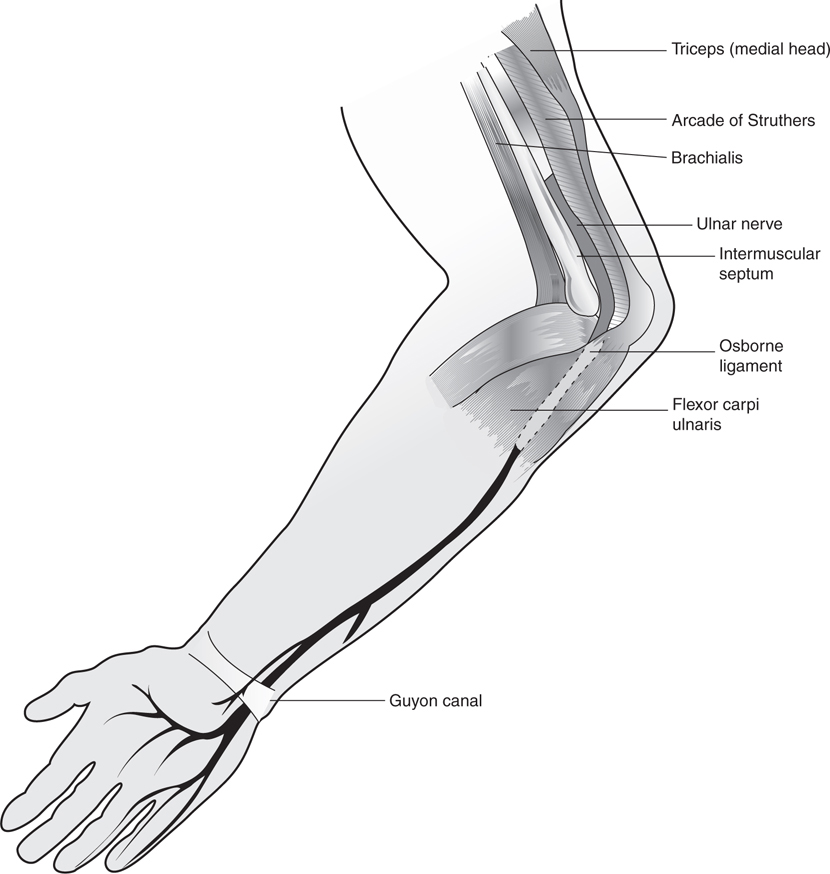
See Figure 34-1.
Figure 34-1 Potential sites of ulnar compression.
1. Arcade of Struthers—an upper arm fascial arcade through which the nerve passes. Present in 70% of patients.
2. Intermuscular septum between the brachialis and medial head of triceps. Can cause compression even in the absence of arcade of Struthers so they are distinct.
3. Medial head of triceps—can cause compression by triceps hypertrophy (bodybuilders) or anterior subluxation of the ulnar nerve over medial epicondyle.
4. Osborne ligament—Most common site of ulnar nerve compression. This is a fascial arcade formed between the two heads of the flexor carpi ulnaris (FCU).
5. Flexor-pronator aponeurosis—a fascial band between the flexor digitorum superficialis (FDS) and the FDP.
6. Guyon canal—Second most common site of ulnar nerve compression. Located at the wrist (see Fig. 34-1).
 Where is the arcade of Struthers?
Where is the arcade of Struthers?
Located 8 cm proximal to the medial epicondyle of the elbow.
 What are the boundaries of the cubital tunnel?
What are the boundaries of the cubital tunnel?
Floor—medial collateral ligament of elbow (spans from medial epicondyle to olecranon).
Roof—Osborne ligament.
Sides—medial epicondyle and olecranon (to which the above two structures attach).
 Explain why the elbow hyperflexion test elicits symptoms of cubital tunnel syndrome?
Explain why the elbow hyperflexion test elicits symptoms of cubital tunnel syndrome?
Elbow flexion increases the distance the ulnar nerve has to travel to traverse the elbow.
Try it yourself: Palpate your own olecranon and medial epicondyle with your elbow extended. Now flex your elbow and notice how the distance between them grows, tightening Osborne ligament and compressing the nerve.
 How sensitive is electrodiagnostic testing at the elbow?
How sensitive is electrodiagnostic testing at the elbow?
Electrodiagnostic testing has a 50% false-negative rate for nerve compression at the elbow.
 What is a Martin–Gruber anastomosis, and what is its significance in relation to cubital tunnel syndrome?
What is a Martin–Gruber anastomosis, and what is its significance in relation to cubital tunnel syndrome?
Naturally occurring anatomic variant involving an interconnection between the median and ulnar nerves at the level of the forearm. The presence of this anomalous interconnection can result in spared intrinsic muscle function with cubital tunnel syndrome (because the median nerve innervates the intrinsics in this situation).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree