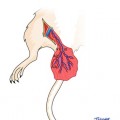
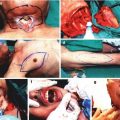
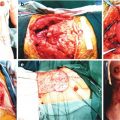
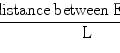Fig. 1.1
Triangulation technique, (a) Placing three stay sutures at equal distances (b–d) Suturing each equal segment with enough number of sutures
Basic Concepts in Reconstructive Microsurgery
Appropriate technical skill is necessary but not sufficient for a successful reconstructive microsurgery. There are some basic concepts that should be known by the surgeon before, during and after the operation.
Vessel Injury and Regeneration
During all microsurgical operations, first an arteriotomy and/or venotomy are performed and then vessel repair is undertaken. Thus, during all microsurgical operations the endothelium of the vessels is disturbed, exposing subendothelial tissues to the bloodstream. This exposition is a first step for blood coagulation, which may result in vessel thrombosis. In order to prevent this coagulation process, the vascular damage and regeneration during microvascular surgery should be well understood.
Following a microsurgical vessel anastomosis, a layer of thrombocytes covers the denuded endothelium. If these thrombocytes are not exposed to sub-endothelial structures (medial layer) and fail to activate the coagulation cascade, they begin to disappear over the next 2–3 days [2]. The healing of the vessel wall begins with a pseudointima formation within the first 5 days [3]. Thus, the critical period for thrombus formation following a vessel anastomosis is 3–5 days.
When the endothelium of a vessel wall is damaged, the endothelial layer is repaired by the regeneration of the nearby cells. However, if the subendothelial structures such as media and adventitia are also damaged, then the healing of the subendothelial structures is achieved by fibroblast proliferation and collagen synthesis. Thus, gentle dissection of the vessels and careful/controlled placement of the sutures through the vessel wall is very important for successful microvascular anastomosis [4]. Small vessels need a special concern, because if desiccated they may loose the endothelial cell layer and cause platelet aggregation. All exposed vessels should be kept in a moist environment in order to prevent desiccation-related intimal damage.
Prolonged vasospasm is another cause of vascular intimal damage and it is shown that vasospasm longer that 2 h results in loss of the endothelial layer [5]. Generally, in order to prevent vessel spasm, topical lidocaine is used. Papaverine solution is also commonly used for vasodilatation.
Vascular clips are used to temporarily stop the blood flow and help for anastomosis. Since the closing pressure of clips is directly related to damage, it should be below 30 g/mm2 [6]. The suturing technique is also very important. Needle and suture penetration, technique of suture placement, repeated needle puncture, unequal intersuture distances, tension of the vessels, too many sutures and too tight sutures can cause endothelial sloughing and subsequent thrombosis [5].
Clotting Mechanism
Perhaps the most devastating morbidity related to microsurgical reconstruction is the flap loss, which is the result of thrombosis at the anastomose site. It is crucial that microsurgeons should know the clotting mechanism and prevention techniques. Thrombocytes do not aggregate to undamaged endothelium and, in case of intimal damage, exposed collagen triggers platelet activation, resulting in platelet aggregation. Activation of platelets also causes fibrin formation, which forms the red and white clot.
Various steps of the coagulation cascade can be manipulated in order to prevent platelet aggregation and clot formation. Current antithrombotic treatments in microvascular surgery include heparin, aspirin, dextran, proteolytic enzymes, and tissue plasminogen activator. There are also experimental studies using monoclonal platelet glycoprotein IIb/IIIa receptor antibody to prevent platelet aggregation [7].
Tissue Ischemia and Reperfusion Injury
During microvascular tissue transfer, tissues undergo ischemia for a certain time. Each tissue type has a period of tolerance to ischemia, which is directly related its metabolic activity. We all know that muscle is much less tolerant to ischemia than other tissues and cooling prolongs tolerance to ischemia in all types of tissues [8, 9].
It is well established that in addition to ischemia; tissues may also be injured during, reperfusion by means of free oxygen radicals. This phenomenon is called reperfusion injury and is related to the local inflammatory response [10, 11]. Following reperfusion of ischemic tissues, leucocytes begin to adhere to the capillary endothelium. These rolling, sticking and transmigrating leucocytes are accepted to be the primary responsible for ischemia-related inflammation [12].
Technical Factors in Microsurgery
Microvascular surgery is a surgical procedure including the anastomosis of small diameter vessels using microscopic assistance. Reconstructive microsurgery basically has three major categories: free tissue transfer, replantation and transplantation. Transplantation may be considered as a form of free tissue transfer, in which a part of a body is transferred as a free tissue to another body.
A standard microsurgical tray includes the following: microbipolar cautery, 5-French Baron angular suction tip, jeweler’s forceps for handling tissue and vessels, a vessel dilator that can be used for both vessel handling and dilation, straight scissors that are typically used to cut suture, curved scissors with blunt tips used for dissection and vessel preparation, a curved non-locking needle holder, and hemoclip appliers.
Both disposable and reusable vessel clamps may be used according to the preference of the surgeon. These clamps may also be used as approximators. Magnification is achieved by a system of convergent lenses, and dissection and anastomosis can be performed with either loupe magnification or with the operative microscope.
The success of microvascular surgery depends on many technical factors such as instruments, sutures and the technique of anastomosis. Donor and recipient vascular structures, tobacco usage, and personal experience of the surgeon are other important factors. It should be kept in mind that microsurgery is a teamwork, which begins preoperatively and continues at the postoperative period.
Magnification
Magnification is essential for microsurgery and may be obtained by operating microscope or loupe. Both have been used successfully, however, many authors advocate using loupe magnification for microvascular anastomosis of vessel smaller than 1.0 mm in diameter [13, 14]. Whether dissection and anastomosis are performed with loupe or operative microscope, appropriate focus depth, field size, and lighting are indicated. Microscopic magnification that is placed on the surgeon’s head (Varioscope) has recently developed [15]. When compared to the operating microscope, loupes are cost effective, portable and easier to use.
Sutures
Both the number and the type of sutures are important for a successful result. The aim is to provide a well approximated, sealed, non-bleeding anastomosis with a minimum number of sutures. When too few sutures are used for anastomosis, there may be excessive bleeding causing thrombus and hematoma formation; when too many sutures are used the endothelial damage may activate a coagulation cascade.
During suture anastomosis, the suture materials are also important. Absorbable and non-absorbable sutures may be used for microvascular anastomosis; however, most surgeons currently use non-absorbable prolene (polypropylene) or nylon (amide polymer) sutures in their practice. Needle design is another important factor. The needles used during microsurgery must be sharp tipped, smooth bodied, adequately shaped for ease of handling and smoothly swaged to the suture material.
Anastomosis Technique
The most frequently used anastomotic techniques are interrupted, continuous and sleeve techniques. Adhesives are also used for anastomosis. For the interrupted suture technique, simple interrupted full thickness sutures are preferred, which are modified from Carrel’s triangular technique. This technique is the most frequently used and accepted technique and all new anastomotic techniques are compared with this technique. Continuous and interrupted sutures have similar patency rates; however, although performed faster than interrupted sutures, the continuous suture technique may narrow the caliber of the vessel lumen [16]. The spiral interrupted suture technique is a combination of continuous and interrupted techniques [17]. It is faster than simple interrupted technique but may cause a purse-string like constriction, especially in end-to-end venous anastomosis.
The sleeve technique is faster and simpler to perform, and sutures cause less trauma to the vessels [18]. There are some experimental studies about usage of adhesives for vessel anastomosis. Synthetic adhesives and fibrinogen are the most commonly used adhesives but this technique is not accepted to be versatile in microsurgery [19].
Cuffs, couplers, staplers and other automatic suturing devices are used for anastomosis [20, 21]. The most important advantage of these devices is shortening the anastomosis time. Coupler is the only routinely accepted anastomosis device in the clinical practice and the other techniques are still only used experimentally. Laser-assisted microvascular anastomosis is performed by the tissue fusion effect of the laser beam and, to date, laser assisted microvascular anastomosis is considered investigational [22].
Anastomosis Types
The most common anastomosis type in microsurgery is end-to-end vessel anastomosis (Fig. 1.2). If a discrepancy smaller than 2:1 occurs in diameters of vessels, then the smaller vessel may be dilated and end-to-end anastomosis can be performed. Another option is cutting the end of the smaller vessel at a slightly oblique angle. For larger discrepancies, end-to-side anastomosis should be preferred (Figs. 1.3 and 1.4




Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree