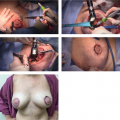
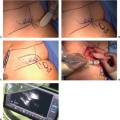
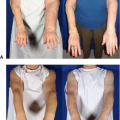
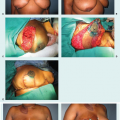
Management of Complications in Breast Reduction: The Displaced NAC
Nolan S. Karp
Ara A. Salibian
Jordan D. Frey
History
Reduction mammoplasty is a frequently performed procedure by plastic surgeons with a high rate of patient satisfaction (1). The majority of reported complications relate to “reconstructive” problems such as delayed wound healing, scarring, fat necrosis, and nipple ischemia (2), with aesthetic concerns such as asymmetry or nipple malposition less frequently described. However, upon closer examination, malposition of the nipple areola complex (NAC) seems to be a more pervasive problem than routinely reported, despite the wealth of discussions dedicated to the appropriate positioning, movement, and manipulation of this anatomic subunit. Moreover, it is a problem that is readily noticed by the patient and can be a source of significant distress for both the patient and the surgeon.
Rates of postoperative NAC asymmetry, malposition, or both vary with the presence of preoperative discrepancies, the techniques for reduction utilized, and the methods of analysis. Nipple overelevation has been reported in nearly 42% of cases in a systematic review of mastopexy and reduction (3). Lewin et al. reported only 26% of nipples in the optimal mediolateral position and 44% in the optimal craniocaudal direction after reduction mammoplasty (4). Rates of NAC asymmetry in vertical reductions have also been associated with preoperative asymmetry, increased NAC translocation, and more extensive reductions (5). In superomedial pedicle, Wise-pattern reductions, nipple position has been found to be almost 2 cm higher than initially positioned (6), and in vertical reductions around 1 cm higher than preoperative markings after 4 years (7). Regardless of particular values, the incidence of the ill-positioned nipple, whether symmetric or asymmetric, is not insignificant, and it behooves the plastic surgeon to know when and how to correct it.
The vast majority of discussions on correcting nipple malposition after breast reduction have focused on addressing superior displacement of the nipple. The “high-riding nipple” has likely received the focus of attention as it is the most common direction of malposition as well as the most difficult to correct; an undesirable combination. Strombeck commented on the significant difficulty of correcting the high-riding nipple in 1976 (8) and later reflected on the commonality of this error in positioning (9). In 1972, Rees et al. proposed performing a revision reduction with further resection of lower pole tissue to resituate the nipple (10). However, we know that parenchymal resection will help further shape the breast, but do little to reorient nipple position in true cases of superior nipple malposition. The same year, Millard et al. described similar inferior crescentic skin resections to shorten the distance between the nipple and the inframammary fold (IMF), but with the addition of small implants to further project the nipple and minimize flattening of the breast (11). In addition, the authors proposed a true downward repositioning of the nipple, which required incisions placed on the upper pole of the breast, above the new nipple position.
Elsahy et al. later described a revision Wise-type skin excision below the NAC to decrease the nipple to IMF distance (12). While this does not technically move the nipple, it alters the breast mound to have the nipple in a more favorable orientation relative to the lower pole. The need for additional skin above the nipple was realized soon thereafter as Raffel et al. proposed utilizing tissue expansion of the upper pole to allow for an absolute change in position of the nipple (13). This technique has continued to be utilized for more severe malposition today (14).
While superior malposition is usually the most frequently encountered direction of displacement, lateral and medial malposition (often a cause of asymmetry) and inferior malposition are not without occurrence. Taking steps to correct nipple malposition requires understanding the error that led to the initial incorrect placement. More often than not, it is an error in planning, rather
than one that is technical in nature. However, many factors, both in and out of the surgeon’s control, can influence the positional aesthetics of the nipple after reduction mammoplasty.
than one that is technical in nature. However, many factors, both in and out of the surgeon’s control, can influence the positional aesthetics of the nipple after reduction mammoplasty.
NAC Placement in Breast Reduction
The most important step in management of nipple malposition is prevention. Prevention involves familiarity with the morphometrics of the female breast and the divergence of these parameters in the individual macromastic patient. Furthermore, meticulous preoperative planning, precise marking, and obsessive repeated evaluation and alteration of these measurements are required both preoperatively and in the operating room.
In 1956, Wise first suggested that the optimal position of the nipple should be at “the most prominent portion of the breast” (15). Identification of the appropriate new nipple position in reduction mammoplasty has traditionally involved anterior translocation of the projected IMF position onto the breast mound with the surgeon’s nondominant hand as described and popularized by Arié (16) and Pitanguy (17), respectively. Manual translocation of the IMF is a subjective process that can be highly variable among different surgeons. The marked nipple position should therefore be checked with the IMF position laterally and visualized at the projecting portion of the breast repeatedly to ensure appropriate placement.
The top of the mosque/future areola is subsequently placed 2 cm above this marking for an areola that is planned to be around 38 to 45 mm in diameter. If a patient has severe grade III ptosis with a disproportionately long sternal notch-to-nipple distance, we prefer to mark the top of the area more conservatively, at only 1 cm above the planned nipple position. The contralateral nipple must be marked based on fixed landmarks, and not one that can further confer asymmetry to the other side. In other words, transposing the contralateral nipple from the IMF will only translate any asymmetries in IMF position to the nipples. For this reason, the sternal notch-to-nipple distance is measured on the initial side, and then used to determine the position of the nipple on the contralateral side. The medial to lateral position of the nipple is determined by the breast meridian, drawn through the midpoint of the breast which does not necessarily bisect the preoperative NAC.
When marking the nipple, it is important to remember that it is always easier to raise a nipple that is too low, than to lower a nipple that is too high. With this in mind, one should always defer to a lower position that offers a significantly more correctable discrepancy in the case of inappropriate placement. Similarly, the nipple is most aesthetically pleasing at a slightly lateral projection (18), and therefore one should err in this direction when questioning the appropriate placement in a particular direction.
In addition to planning based on the current preoperative measurements of the breast, one must also consider the evolution of breast shape over times, as changes in shape postoperatively will inevitably affect nipple position. In this regard, we place the nipple position at 1 to 2 cm below the level of the IMF when planning inferior pedicle breast reductions, as the breast has a greater tendency to bottom out over time under the weight of this pedicle. On the other hand, when a medial or superomedial pedicle will be utilized, regardless of the skin excision pattern, the new nipple position remains at the level of the IMF (19).
While new nipple position has traditionally been determined in relation to translocation of the IMF, others have suggested it is more appropriately placed according to the overall footprint of the breast mound. Hall-Findlay et al. advocate using the upper border of the breast as a landmark, and placing the new nipple position 10 cm below this border (for a C-cup breast) (18). This creates a nipple position at the projecting portion of the breast and in the more aesthetically appropriate lower half of the breast mound. Additional techniques utilize the patient’s breast width to determine the appropriate nipple-to-IMF length, and subsequently plan the correct new nipple position from a “bottom-up” approach based on the existing IMF (20).
Regardless of what techniques are used to determine the appropriate nipple position, the surgeon must be adamant about visualizing the final result, ensuring symmetry between both sides and constantly rechecking measurements prior to making incisions. While minor adjustments in the operating room can be made, it is best to have the ideal results preoperatively, and minimize changes to one’s plan in the operating room.
Indications and Contraindications
Indications for repositioning of the malpositioned NAC after breast reduction are dependent on several factors including the direction of displacement, the severity of the aesthetic deformity, the presence of asymmetry, the overall aesthetic outcome of the reduction, and the patient’s satisfaction with the initial result and desire for correction. Superior malposition is typically treated more aggressively, as this displacement will usually only progressively worsen with time as the weight of the residual breast parenchyma will cause some extent of lower pole expansion, lengthening the nipple-to-IMF distance. Inferior malposition, or an undercorrection of ptosis, on the other hand, can be treated more conservatively for similar reasons. Some degree of “bottoming out” of the breast is to be expected, especially with inferior pedicle reductions, and can make the slightly inferiorly placed nipple appear to be in a more favorable position over time. Though not always ideal, it is better to wait for at least a year and let the position of the breast settle. While this
may help mild discrepancies transition from being perceived as unacceptable to acceptable, more severe inferior displacement will require some form of mastopexy.
may help mild discrepancies transition from being perceived as unacceptable to acceptable, more severe inferior displacement will require some form of mastopexy.
Symmetric and asymmetric discrepancies are also inherently different complications in that slight asymmetry is inherently displeasing and more noticeable to the observer. Therefore, asymmetric malposition of the nipple tends to warrant correction more than symmetric malposition. For example, nipples that are positioned slightly too laterally or medially, but are symmetrically deviated, are often more acceptable than a unilaterally deviated nipple. These principles apply to mild-to-moderate malposition. Severely malpositioned nipples, in any direction, and regardless of symmetry, will require correction.
Importantly, these decisions are arrived upon with consideration of the patient’s satisfaction with the postoperative result and desire for further correctional procedures. Different degrees of malposition and asymmetry are acceptable to different patients. Intervention is pursued if the patient desires correction (21) and the surgeon believes an improvement in the outcome can be reasonably obtained. Preoperative consultation in their regard is paramount.
Contraindications to the correction of nipple malposition are limited. Revisions of the nipple should not be performed in active smokers to minimize the chance of NAC necrosis, given the baseline increased risk of ischemic complications of the nipple with secondary manipulation. Revisions should also not be planned with any ongoing wound healing problems and surgery should be delayed until well after complete resolution of these issues. The surgeon should be weary of demands for correction of negligible discrepancies that may not necessarily be improved with further surgery.
Preoperative Planning
Preoperative photos prior to the initial reduction should be reviewed and meticulously compared to the most recent postoperative photographs displaying the offending malposition. It is important to understand not only the positional changes needed to remedy the current deformity, but the sequence of changes that led from the planned preoperative markings to the current undesirable result. Ideally, preoperative markings for the initial reduction are also reviewed to identify an error in planning or perception that will be avoided at the secondary revision.
Regardless of the correctional vector or chosen revision technique, certain standardized markings are needed for all cases of nipple malposition correction. These markings are similar to those in primary reductions and provide topographic landmarks from which alterations in nipple position are planned. With the patient standing, the sternal midline is marked, as well as the breast meridians bilaterally and the IMFs. Any discrepancies in IMF height should be noted as this affects the relative position of the nipple on the breast mound. The desired new location of the nipple on the breast is marked and the direction and length of needed movement noted. This measurement is typically based on the position of the IMF; however, one must be careful to ensure that fold itself is in the correct position. The desired position of the nipple should be checked relative to the superior border of the breast and distance from the sternal notch in order to ensure its appropriate placement with regard to all important landmarks. Subsequently, changes in the contralateral nipple are marked, if needed, and symmetry of the two sides is confirmed and rechecked.
Intraoperative Care
Superiorly Displaced NAC
The high-riding nipple is a formidable challenge. The paucity of excess skin between the nipple and the clavicle and the poor aesthetic tolerance of incisions in the upper pole of the breast limits the available revisional procedures that do not further distort the breast.
These procedures can be classified into indirect and direct methods of correction. The former attempts to mold the remaining breast skin and parenchyma in order to shorten the distance between the nipple and the IMF. The latter involves actual translocation of the NAC, usually based on local flaps or as a free graft. While direct modifications are inherently more effective means of repositioning the nipple, certain situations, such as those with milder or relative malposition, can be amenable to indirect measures. The critical decision therefore is in the appropriate diagnosis of the deformity and its etiology, in order to be able to apply the correct revisional technique.
Different models have proposed methods to classify and subdivide types of superior nipple malposition (14,21). In general, these systems tend to rank the severity of the positional displacement of the nipple and also determine whether the nipple has remained in a stable position, but the change in the shape of the breast parenchyma has conveyed an appearance of malposition, therefore suggesting a pseudo- or relative deformity. While some argue that nipple position should be determined by its relation the breast mound irrespectively (22), the important deductions that one must determine from physical examination are (1) the severity of the nipple displacement and (2) the presence of an additional breast deformity, such as bottoming out, that may improve the perceived nipple position if corrected.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree