Male Breast Cancer: Surgery of the Breast
John Vincent Kiluk
Blaise P. Mooney
Hatem Soliman
Roberto Diaz
History
Male breast cancer is a rare form of cancer that comprises approximately 1% of all cases of breast malignancies. Males carry a 0.1% lifetime risk of developing breast cancer that is significantly less than the 12% risk of women. In 2019, there will be an estimated 2,670 new cases of male breast cancer in the United States compared to 268,600 cases of the female variant (1). As a result of the rarity of this cancer, studying male breast cancer has been challenging, as prospective trials would be difficult to accrue. Current recommendations toward management have mostly been based on retrospective male data and the assumption that outcomes of treatments would be similar as female breast cancer, for which data are more robust.
Risk Factors
Even though most patients present without any risk factors, several potential features have been identified to increase the risk of male breast cancer. Risk assessment should always start with genetic testing. Male patients often carry a family history of malignancies with 15% to 20% of patients reporting a family member with either breast or ovarian cancer (2). Many genes have been associated with male breast cancer including BRCA1, CHEK2, P53, PTEN, PALB2 but the most common association is with BRCA2 mutations. BRCA2 carriers demonstrate a 5% to 10% lifetime risk of developing cancer that is interestingly less than the average woman’s lifetime risk of breast cancer (3). Despite a lack in data supporting prophylactic mastectomy in genetic carriers, results in genetic testing are critical for assessing other family members risk of cancer (daughters, sisters, etc.) and may affect screening of other cancers (BRCA2 carriers are increased risk of prostate and skin cancers).
Hormonal factors that lead to increased estrogen to testosterone levels appear to be influential in patients developing male breast cancer (4). Klinefelter syndrome, which is characterized with the XXY karyotype, has been reported in to up to 7.5% of patients with male breast cancer (5). These patients have low testosterone levels and high gonadotropin concentrations. Other factors that increase estrogen and/or lower testosterone (prostate cancer treatment, hormonal therapies, testicular/liver damage) have been associated with male breast cancer as well.
Additional risk factors are similar to females with breast cancer. Male patients with a history of radiation treatments for Hodgkin disease may be prone to developing a future cancer within the treatment field years after the completion of treatment. Age is a risk factor of breast cancer with the peak risk of developing breast cancer to be approximately 75 years of age (2). Environmental exposures while working with chemicals, synthetics, or electromagnetic fields have also demonstrated increased risks of male breast cancer (4).
In discussing risk of male breast cancer, it is important to mention gynecomastia. To date, there has been no association between gynecomastia and male breast cancer.
Clinical Presentation
The most common presentation for male breast cancer is a painless, subareolar breast mass. Nipple discharge, skin involvement, axillary lymphadenopathy are additional features that may be present on examination. Nonpalpable breast cancers are rare as males do not undergo routine, screening mammography.
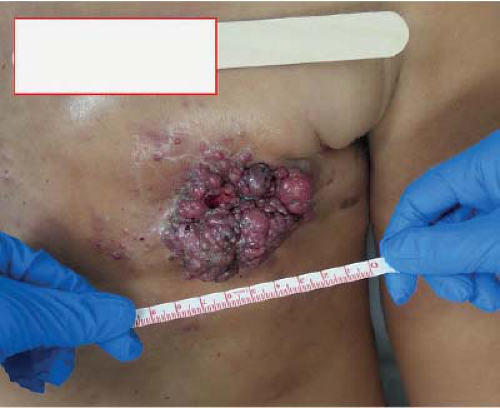
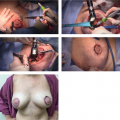
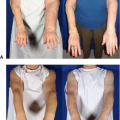
Compared to females, males may present at more advanced stages of disease. Multiple factors may play a role in this later presentation ranging from less routine screening to a possible lack of awareness of male breast cancer by both patients and providers. Figure 19-1 demonstrates a locally advanced male breast cancer at presentation. A SEER review by Leon-Ferre compared stage at presentation between male and female breast cancer demonstrated more advanced stages in male patients (6). Stage 2 (43% vs. 28%), stage 3 (8% vs. 5%), and stage 4 (3% vs. 2%) disease were all more common in male patients with breast cancer.
Radiology
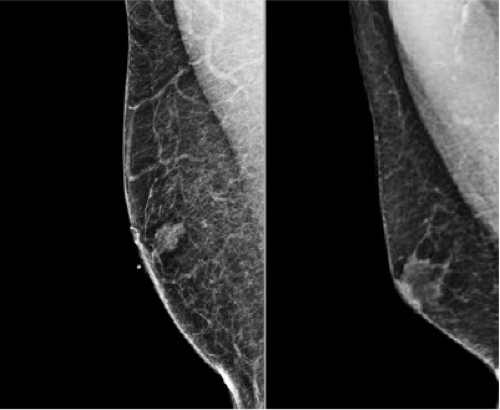
Radiologic workup of the male breast for a palpable mass or clinical finding begins with a diagnostic mammogram (7). A bilateral mammogram is extremely useful. Even if symptoms are unilateral, having the opposite side as a comparison is helpful in making diagnosis and deciding if Ultra Sound (US) is appropriate. The finding is often gynecomastia, which can be bilateral or unilateral. Gynecomastia, proliferation of ducts and stroma, is the most common abnormality in the male breast. There are three main imaging patterns of gynecomastia (nodular, dendritic and diffuse glandular). It is classically described as flame shaped and should have indistinct borders, existing in harmony with surrounding tissue. The most important thing to remember about gynecomastia is that it must be subareolar. From an imaging perspective, differentiating a malignancy from gynecomastia in the subareolar region relies upon evaluation of the borders (Fig. 19-2). Malignancies often have convex borders, however when the borders are spiculated, this can cause some confusion and mimic gynecomastia. Even though male breast cancers most commonly occur in the subareolar location, they can be located anywhere. Any mass in the male breast that is not subareolar is not gynecomastia, and will require additional action (8).
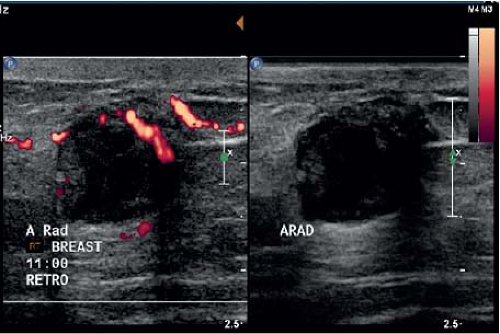
If the appearance is classic “flame shaped” on mammogram and there is NO evidence of a mass, then US should be avoided as this will usually lead to an unnecessary biopsy. US is indicated if the mammogram demonstrates a visible mass or the palpable breast mass is located away from the nipple (Fig. 19-3). Figure 19-4 demonstrates a left subareolar mass with convex borders and coarse calcifications on mammography. Calcifications seen on mammography deserve workup in the male breast. Magnification views should be performed to determine extent and
plan safe core biopsy. US of the area of calcifications is recommended, as this might facilitate a safer US-guided biopsy. A negative US should not dissuade one from sampling calcifications in the male breast as calcifications are frequently associated with ductal carcinoma in situ (DCIS). MRI of the breast offers little advantage other than assisting in ruling out chest-wall involvement.
plan safe core biopsy. US of the area of calcifications is recommended, as this might facilitate a safer US-guided biopsy. A negative US should not dissuade one from sampling calcifications in the male breast as calcifications are frequently associated with ductal carcinoma in situ (DCIS). MRI of the breast offers little advantage other than assisting in ruling out chest-wall involvement.
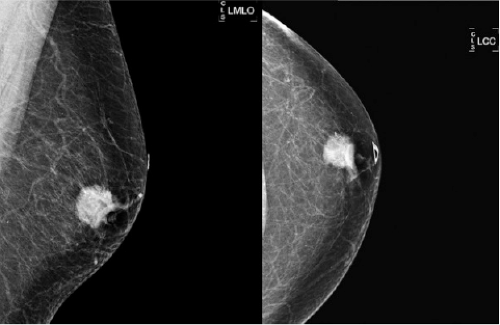 FIGURE 19-4 LEFT MLO and CC digital mammogram demonstrate a spiculated mass with calcifications in the retroareolar location. Note that no LEFT axillary nodes are seen on the LEFT MLO mammogram. |
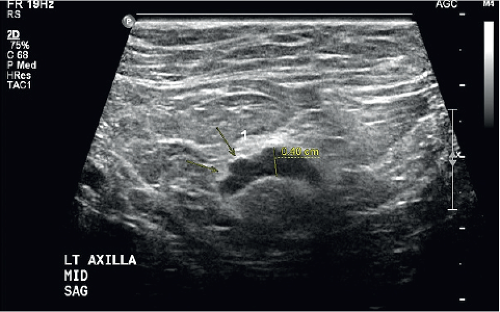
In the male breast, the majority of malignancies are subareolar and metastasis to the axilla is common. It has been reported that 50% of men have axillary nodal metastasis at initial presentation (9). US of the ipsilateral axilla should be included. It is important to note the morphology of the nodes matters more than the overall size. Displacement of the fatty hilum, increased cortical thickness >3 mm or irregular contour of the cortex are suspicious findings and warrant tissue sampling (Fig. 19-5). If US-guided axillary lymph node biopsy reveals metastatic disease, then additional staging examinations similar to what female breast cancer patients undergo are indicated. Computed tomography (CT) of the thorax and abdomen and Tc99m-HDP whole-body bone scan are recommended.
Pathology
The most common histology encountered in male breast cancer is invasive ductal cancer. Isolated ductal carcinoma in situ (DCIS) is very uncommon as this usually presents with calcifications on mammography and males do not receive screening mammography. Other histologic subtypes (lobular, papillary, metaplastic, mucinous, or tubular) are rare.
The vast majority of male breast cancers are estrogen receptor (ER) positive. The most comprehensive pathologic review of male breast cancer was performed by the EORTC 10085/TBCRC/BIG/NABCG International Male Breast Cancer Program (10). In this study, close to 1,500 male breast cancer cases were centrally reviewed by pathology. Using immunochemistry, 41.9% of cases were classified as Luminal A and 49.2% of cases were Luminal B, HER2 negative. ER-negative tumors were exceeding rare as Basal subtypes and Nonluminal HER2 subtypes comprised 1% and 0.1% of cases, respectively. Clinically, we have become suspicious of any male
presenting with an ER- male breast cancer. Upon further workup, many of these “male breast cancers” turn up having a nonbreast primary, most commonly a skin malignancy.
presenting with an ER- male breast cancer. Upon further workup, many of these “male breast cancers” turn up having a nonbreast primary, most commonly a skin malignancy.
HER2 is usually negative in male breast cancer but up to 8% may be HER2 positive. These tumors are important to identify, as HER2 results would strongly influence decisions on chemotherapy and trastuzumab (Herceptin).
Surgical Management
Surgical management of male breast cancer is similar to female breast cancer in that both mastectomy and lumpectomy are options for patients. As most male breast cancers are in a subareolar location and may be closely associated with the nipple, most males elect to pursue mastectomy. Not only does this option remove the nipple ensuring clear margins, it may spare the patient the need for radiation that would absolutely be required in a lumpectomy. For tumors not directly associated with the nipple, lumpectomy is a potential alternative to mastectomy (11,12).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree