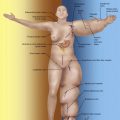
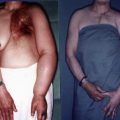
Key Points
- ▪
Cancer survivors who have had treatment affecting the lymph drainage system have a lifelong risk of developing lymphedema.
- ▪
Lymphedema management includes risk-reduction education and lymphedema treatment.
- ▪
While some risks are generally recognized, there is no consensus on other risk factors and further research is necessary.
- ▪
Risk-reduction education is a necessary component of cancer survivorship to maximize self-management and adherence to treatment.
- ▪
Early lymphedema detection and treatment improves outcome.
- ▪
Lymphedema is more than mechanical insufficiency due to reduced transport capacity. Lymphedema is an inflammatory edema associated with an increase in the adipose content of the subcutaneous layer.
- ▪
Complete decongestive therapy (CDT) is an accepted and effective combination of techniques which decongests the soft tissue swelling associated with lymphedema.
- ▪
Multimodal treatment approaches, including manual therapy, compression bandaging, exercise, pneumatic compression pumps, as well as complementary and alternative therapies, are available to clinicians for the treatment of lymphedema.
- ▪
The most studied group is patients with breast cancer-related lymphedema (BCRL) but more rigorous research with prospective studies and larger randomized control trials should be conducted in this and other populations.
- ▪
Lymphedema in populations other than BCRL has a paucity of research focused on epidemiology, risk-reduction and treatment intervention.
The Management of Lymphedema
Lymphedema management includes risk-reduction education and lymphedema treatment. Although cancer treatment-related lymphedema is the most common cause of non-filarial lymphedema in many developed countries, most of the management strategies described are also valid for individuals with primary lymphedema and associated disorders, such as phlebolymphedema and lipedema.
Educating At-Risk Individuals
Cancer survivors are a growing cohort—14.5 million Americans as of January, 2014. Survivorship presents a unique set of needs, including risk for developing lymphedema. While some survivors develop lymphedema as a late effect of treatment, limited empirical evidence prevents physicians from predicting likeliness of onset in individuals at risk. Epidemiological reports of breast cancer-related lymphedema (BCRL) and cancer-related lower limb lymphedema varies amongst researchers, with higher rates noted when researchers combine patient self-report or utilize multiple strategies for measurement and lower rates when the sample is studied for less than two years. A recent systematic review suggests 21% incidence of BCRL worldwide. Reporting of lymphedema following treatment for cancers other than breast varies from 4% for head and neck to 20–31% gynecological and genitourinary. Factors that may increase risk for lymphedema following cancer treatment are identified in multiple studies, but data are inconclusive for absolute risk ( Figure 9.1 ).
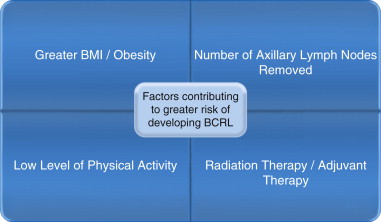
In contrast to the evidence for cancer-related secondary lymphedema, primary lymphedema remains an underdiagnosed, understudied, and untreated disorder. Compelling work in the field of genetics may one day allow improved predictability for lymphedema as a consequence of cancer treatment. While definitive criteria for determining lymphedema risk is lacking, medical professionals must educate any patient at risk to allow timely access to lymphedema care.
Early proponents of risk-reduction education urged health professionals to teach activity restrictions to limit potential triggers for lymphedema, basing recommendations on expert opinion and anecdotal evidence. Some past recommendations lack scientific rigor required for widespread adoption. Today, many advocate for teaching about risk reduction to allow patients to make behavioral changes that theoretically reduce risk of developing lymphedema, but some call for more rigorous science before broadly prescribing risk management strategies, especially in those with lesser risk, such as breast cancer survivors who have undergone sentinel lymph node dissection ( Box 9.1 ).
National organizations advocating for lymphedema risk-reduction education:
NLN : National Lymphedema Network
NAPBC : National Accreditation Program for Breast Centers
NCI / NIH : National Cancer Institute at the National Institutes for Health
ISL : International Society of Lymphology
ONS : Oncology Nursing Society
ALFP : American Lymphedema Framework Project
ILF : International Lymphoedema Framework
ACS : American Cancer Society
LIVE STRONG Foundation
Susan G Komen® Foundation
APTA : American Physical Therapy Association
AOTA : American Occupational Therapy Association
Medical committees acknowledge need for clinical trials to strengthen advice, but assert that sound understanding of lymphatic physiology and pathophysiology of lymphedema provide the basis of current risk-reduction practices. Patients search for health information from sources other than their healthcare providers and may find inaccurate information about lymphedema. Ultimately, patients are better served in receiving direction from healthcare providers.
Knowledge Leads to Early Intervention and Best Practice
Contemporary lymphedema literature emphasizes the need for self-monitoring, early diagnosis, and access to treatment. Educators teaching risk-reduction strategies have multiple aims:
- 1)
to teach patients to recognize personal risks and symptoms
- 2)
to encourage patients to make appropriate response should onset occur
- 3)
to provide facts about lymphatic system function to allow one to minimize stress on the system during typical activities of daily living (ADL)
- 4)
to restore confidence to mindfully resume the ADL
- 5)
to engage in health-promoting activities ( Figure 9.2 ).

Figure 9.2
Risk reduction. Traditional practices in lymphedema self-management. MLD = manual lymphatic drainage.
Educational components of lymphedema risk reduction include explanation of normal lymphatic anatomy and physiology, pathophysiology of lymphedema, signs and symptoms of lymphedema, signs and symptoms of infection, need for physician diagnosis, and patient-specific personal risk factors ( Figure 9.3 ).
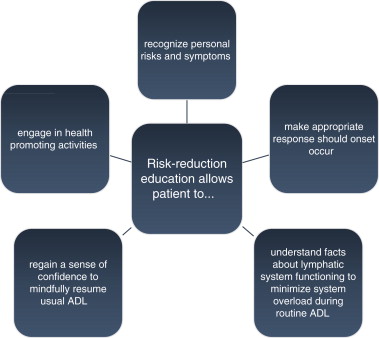
Risk Reduction is Important for Health-Related Quality of Life and Health-Promoting Behaviors
Research demonstrates that health-related quality of life (HR-QOL) is reduced in breast cancer survivors with lymphedema, compared to breast cancer survivors who do not have lymphedema. Some studies find that complete decongestive therapy (CDT) improves HR-QOL and lack of knowledge around lymphedema leads to reduced HR-QOL. Clinicians assert that milder stage of lymphedema leads to greater ease of treatment and long-term symptom management. Healthcare providers can facilitate engagement in health-promoting activities in patients at risk for lymphedema and support improved HR-QOL. A growing body of evidence demonstrates exercise improves HR-QOL and may have a protective effect countering the development of BCRL.
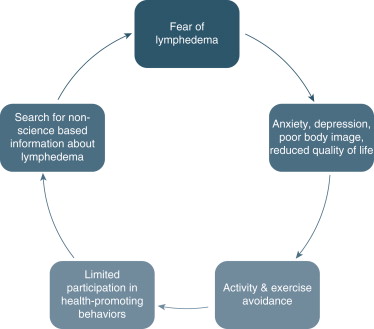
However, fear may drive patient decision-making and lead to avoidance behaviors, such as disusing the affected arm during routine ADL or avoiding physical exercise and developing weight-management difficulties. Patients may respond inappropriately to symptom management by either utilizing strategies not recommended by clinicians or by disregarding the need to address symptoms. If healthcare providers do not educate around risk reduction the patient will lack the ability to make educated decisions about lifestyle choices. Deconditioned muscle groups are more readily strained with addition of exercise or strenuous ADL, and research suggests that sedentary lifestyle can contribute to lymphedema risk. Consequences of soft tissue strain may trigger lymphedema, further reinforcing avoidance behaviors and reducing quality of life ( Figure 9.4 ).
Teaching the Layperson
Concepts of lymphatic anatomy, physiology, lymphatic load, and lymphatic transport capacity are complex subjects for the layperson to digest. Effective teaching requires lessons tailored to allow each individual to analyze personal risk for lymphedema, self-assess routine ADL, review the activities for impact on the lymph system, and apply appropriate risk-reduction behaviors ( Box 9.2 ).
I
Skin Care —Avoid trauma/injury to reduce infection risk
- ▪
Keep extremity clean and dry
- ▪
Apply moisturizer daily to prevent chapping/chafing of skin
- ▪
Attention to nail care; do not cut cuticles
- ▪
Protect exposed skin with sunscreen and insect repellent
- ▪
Use care with razors to avoid nicks and skin irritation
- ▪
If possible, avoid punctures such as injections and blood draws
- ▪
Wear gloves while doing activities that may cause skin injury (e.g., washing dishes, gardening, working with tools, using chemicals such as detergent)
- ▪
If scratches/punctures to skin occur, wash with soap and water, apply antibiotics, and observe for signs of infection (i.e., redness)
- ▪
If a rash, itching, redness, pain, increased skin temperature, increased swelling, fever or flu-like symptoms occur, contact your physician immediately for early treatment of possible infection
II
Activity/Lifestyle
- ▪
Gradually build up the duration and intensity of any activity or exercise. Review the Exercise Position Paper
- ▪
Take frequent rest periods during activity to allow for limb recovery
- ▪
Monitor the extremity during and after activity for any change in size, shape, tissue, texture, soreness, heaviness or firmness
- ▪
Maintain optimal weight. Obesity is known to be a major lymphedema risk factor
III
Avoid Limb Constriction
- ▪
If possible, avoid having blood pressure taken on the at-risk extremity, especially repetitive pumping
- ▪
Wear non-constrictive jewelry and clothing
- ▪
Avoid carrying a heavy bag or purse over the at-risk or lymphedematous arm or shoulder
IV
Compression Garments
- ▪
Should be well-fitting
- ▪
Support the at-risk limb with a compression garment for strenuous activity (i.e., weight lifting, prolonged standing, and running) except in patients with open wounds or with poor circulation in the at-risk limb
- ▪
Patients with lymphedema should consider wearing a well-fitting compression garment for air travel. The NLN cannot specifically recommend compression garments for prophylaxis in at-risk patients
V
Extremes of Temperature
- ▪
Individuals should use common sense and proceed cautiously when using heat therapy. Observe if there is swelling in the at-risk limb or increased swelling in the lymphedematous limb and cease use of heat such as a hot tub or sauna
- ▪
Avoid exposure to extreme cold, which can be associated with rebound swelling, or chapping of skin
- ▪
Avoid prolonged (greater than 15 minutes) exposure to heat, particularly hot tubs and saunas
VI
Additional Practices Specific to Lower Extremity Lymphedema
- ▪
Avoid prolonged standing, sitting or crossing legs to reduce stagnation of fluid in the dependent extremity
- ▪
Wear proper, well-fitting footwear and hosiery
- ▪
Support the at-risk limb with a compression garment for strenuous activity except in patients with open wounds or with poor circulation in the at-risk limb
NOTE : Given that there is little evidence-based literature regarding many of these practices, the majority of the recommendations must at this time be based on the knowledge of pathophysiology and decades of clinical experience by experts in the field.
National Lymphedema Network Position Statement, Lymphedema Risk Reduction Practices .
Following activity analysis, problem-solving, and behavioral changes, one may be able to minimize ongoing lymphatic burden that leads to system overload and lymphedema. In our clinical practice, we have found effectiveness in teaching the following basic concepts in a community-based cancer survivorship lecture: synopsis of lymphatic system function, simplification of microcirculation concepts, instruction in the body’s lymphatic load, and discussion of the transport capacity of an intact system contrasted with a system having impairment. We encourage discussion around current risk-reduction practices, exercise options, and compression garment recommendations. Streamlining complex medical information via use of simple analogies makes concepts accessible to attendees.
Physical medicine and rehabilitation departments and cancer survivorship programs may offer programming on lymphedema risk reduction. Occupational and physical therapists teach risk reduction as part of rehabilitation programs for patients who have lymphedema.
Lymphedema Risk Reduction as a Self-Management Behavior
Researchers studying health promotion with chronic disease demonstrate effectiveness of self-management in improved self-efficacy, personal problem-solving, decision-making, and action-planning. Self-management programs call for patient–practitioner collaboration to enable patients to engage in health-promoting behaviors.
Training in self-management is not curative, but provides patients with tools necessary for maximal function during ADL. Effective self-management requires healthcare providers to train around signs and symptoms of the condition, triggers for symptom exacerbation, and steps to manage the chronic condition ( Figure 9.5 ).
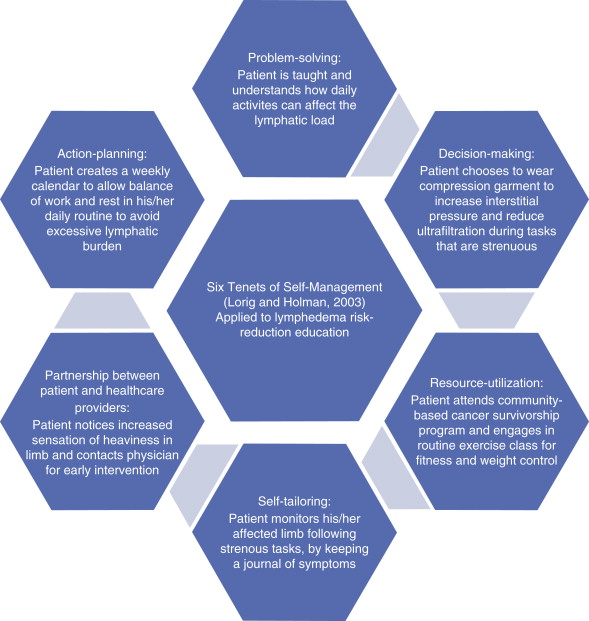
Preliminary data suggest that self-management reduces healthcare costs in the long run. Self-management fits into the context of the Affordable Care Act mandate for improved service quality with cost reduction. Self-management models may be appropriate to deliver in online formatting, in addition to informational leaflets, one-on-one teaching, and group settings ( Figure 9.6 ).
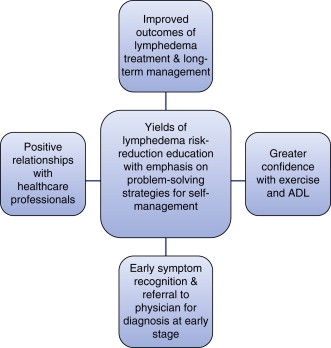
Activity Modifications and Best Practice
While lymphedema is not preventable, unnecessary stress on a system with lymphatic compromise is not recommended. Avoiding physiological burdens that increase load on the system is wise. Modifications are recommended around the following activities: skin care, limb constriction, body temperature, and healthy lifestyle.
National organizations provide accessible patient information for lymphedema risk reduction ( Box 9.3 ). Coupled with individualized instruction around personal needs, these resources allow training in risk reduction. Yet, advisory boards, such as the International Society of Lymphology (ISL), caution against prescribing lists of “Dos and Don’ts” to avoid eliciting unnecessary anxiety in vulnerable populations when science is inconclusive regarding which survivors will one day develop lymphedema.
Collaborative Care
Patient education in the traditional medical model practice assumes the patient functions as a passive recipient of information looking solely to the physician for expert opinion and guidance. Researchers argue that this model prevents patient engagement essential for self-reliance in the face of chronic disease. Collaborative care models empower patients by disseminating knowledge, then developing health partnerships supporting self-management. The prospective surveillance model for rehabilitation following breast cancer treatment, similarly, advocates for health partnership to allow early access to specialized care, rehabilitation and health-promotion education. Improving survivors’ sense of control over their lives and supporting healthy behaviors is the obligation of healthcare professionals during the survivorship phase of care.
Self-reported symptoms are shown to be a predictor of lymphedema onset, thus patients need to learn about signs and symptoms of lymphedema. Patient awareness allows early access to diagnosis, referral to treatment, and participation in normal ADL. Research suggests that healthy lifestyle, including normal BMI and regular exercise, may provide protective effects for the limb at risk for lymphedema. Researchers are challenged to continue working to identify factors that predispose individuals for developing lymphedema post-cancer treatment. Clinicians are challenged to become collaborative partners with patients to improve delivery of knowledge around lymphedema risk, management, and treatment.
Lymphedema Therapy
Complete decongestive therapy (CDT) is a multimodality approach to reducing and controlling lymphedema. CDT can also be effective for treating phlebolymphedema and lipedema. CDT involves patient education, specialized manual therapy, the application of multilayered short stretch bandages, skin care and specialized exercises. Therapists must have specialized CDT training.
CDT is divided into Phase I, treatment, and Phase II, maintenance ( Box 9.4 ). Phase I flows into Phase II. Ideally, Phase I therapy is performed daily until maximal volume reduction is achieved and the skin texture improves.
Phase I: Decongestion
Patient education
Meticulous skin and nail care
Manual lymph drainage (MLD)
24-hour compression bandaging with non-elastic bandages
Compression garment after the limb reduction stabilizes
Phase II: Maintenance
Compression garment
Compression bandages or a non-elastic appliance at night in cases of moderate to severe lymphedema
Lymphedema exercises in garment or bandages
Continued meticulous skin and nail care
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree