Successful lower blepharoplasties address patient-specific lower eyelid, canthal, and lid–cheek junction pathology. Various technical procedures have been described to address the lower eyelid lamellae and tarsoligamentous sling. The most appropriate procedure should be tailored for each patient in an algorithmic approach to ensure optimal esthetic outcomes and minimize risk.
Key points
- •
Lower blepharoplasty decisions should be based on patient-specific facial aging, changes at the lid–cheek junction, degree of midface descent, and lid laxity.
- •
Both transconjunctival and subciliary approaches allow for correction of lower lid problems such as the tear trough deformity, palpebromalar grooves, and pseudoherniation of orbital fat. The transconjunctival approach is most powerful at addressing orbital fat excess and other mild posterior lamellar concerns. Skin pinch, skin-only flap, and other adjunct procedures such as laser and chemical peel can be added to address the anterior lamella as well.
- •
Anterior lamellar excess, more complex deformities of the lid–cheek junction, and malar bags, are better addressed with skin–muscle flap or skin only flap techniques.
- •
Optimal approaches will always require a comprehensive understanding of the patient’s unique anatomic features and the specific clinical presentation.
Introduction
Early lower lid blepharoplasty procedures practiced aggressive skin and orbital fat resection to address the aging eyelid. In the 1970s, Furnas characterized components of the aging lower lid, recognizing the contribution of redundant orbicularis oculi muscle to lower eyelid bags. Skin–muscle flaps were popularized in the 1970s and reigned supreme for 20 years. Historically, over-resection of soft tissue often resulted in untoward effects, including rounding of palpebral fissure, hollowing of the orbit, periorbital tissue deflation, lower lid malposition, and orbicularis denervation.
Hamra expanded the concept of fat preservation, emphasizing complete release of the arcus marginalis with fat repositioning to soften the lid–cheek junction. In the 1990s, the focus shifted to transconjunctival blepharoplasty with fat resection and laser skin tightening. This transconjunctival approach to the orbital rim was originally advocated and described by Tessier, Tomlinson, and Hovey. ,
Lower eyelid blepharoplasty is now one of the most common surgical procedures performed on the face, and fifth most common surgical procedural overall according to ASAPS and ASPS 2022 statistics. Today, less aggressive approaches are commonly favored to obtain natural results and minimize complications associated with disruption of the anterior and middle lamellae. , , , This is especially true considering the availability of modern adjunct skin resurfacing technologies and fat grafting techniques that can further improve operative results. Modern blepharoplasty focuses on the following principles: (1) less aggressive fat resection, (2) fat repositioning through transconjunctival or subciliary approaches, (3) minimal skin resection, (4) lower lid support through canthopexy and canthoplasty techniques. ,
Today plastic surgeons have multiple approaches available to address lower eyelid aging. Isolated problems of fat pads, tear trough, and lid–cheek junction without overlying muscle or skin excess can be addressed safely and effectively with a transconjunctival approach. Skin and orbicularis excess, as well as more complex and severe lid–cheek junction deformities, are more appropriately addressed through a subciliary approaches such as the skin pinch, skin only flap, or skin–muscle flaps. , , , The entire midface can be lifted with an extended lower lid blepharoplasty/sub-orbicularis oculi fat (SOOF) lift, which adds further power by releasing orbital retaining ligaments by means of subperiosteal orbicularis oculi release along the lateral orbital rim as well. ,
This study reviews current approaches to lower lid blepharoplasty and provides a suggested treatment algorithm for correcting lower lid deformities.
Current Approaches to Lower Lid Blepharoplasty
Lower lid blepharoplasty is a nuanced surgical procedure with several approaches tailored to address specific anatomic and clinical challenges. The appropriate technique selection is influenced by the surgeon’s expertise and the patient’s unique presenting anatomy. Appropriate patient screening and lower eyelid clinical assessment is critical. This includes evaluation of the anterior lamella, orbital fat characteristics, lid–cheek junction (ie, tear trough deformity, palpebromalar groove), midface, and lid laxity. Patient evaluation is discussed in detail in .the Patient Evaluation chapter of this issue.
Transconjunctival Approach
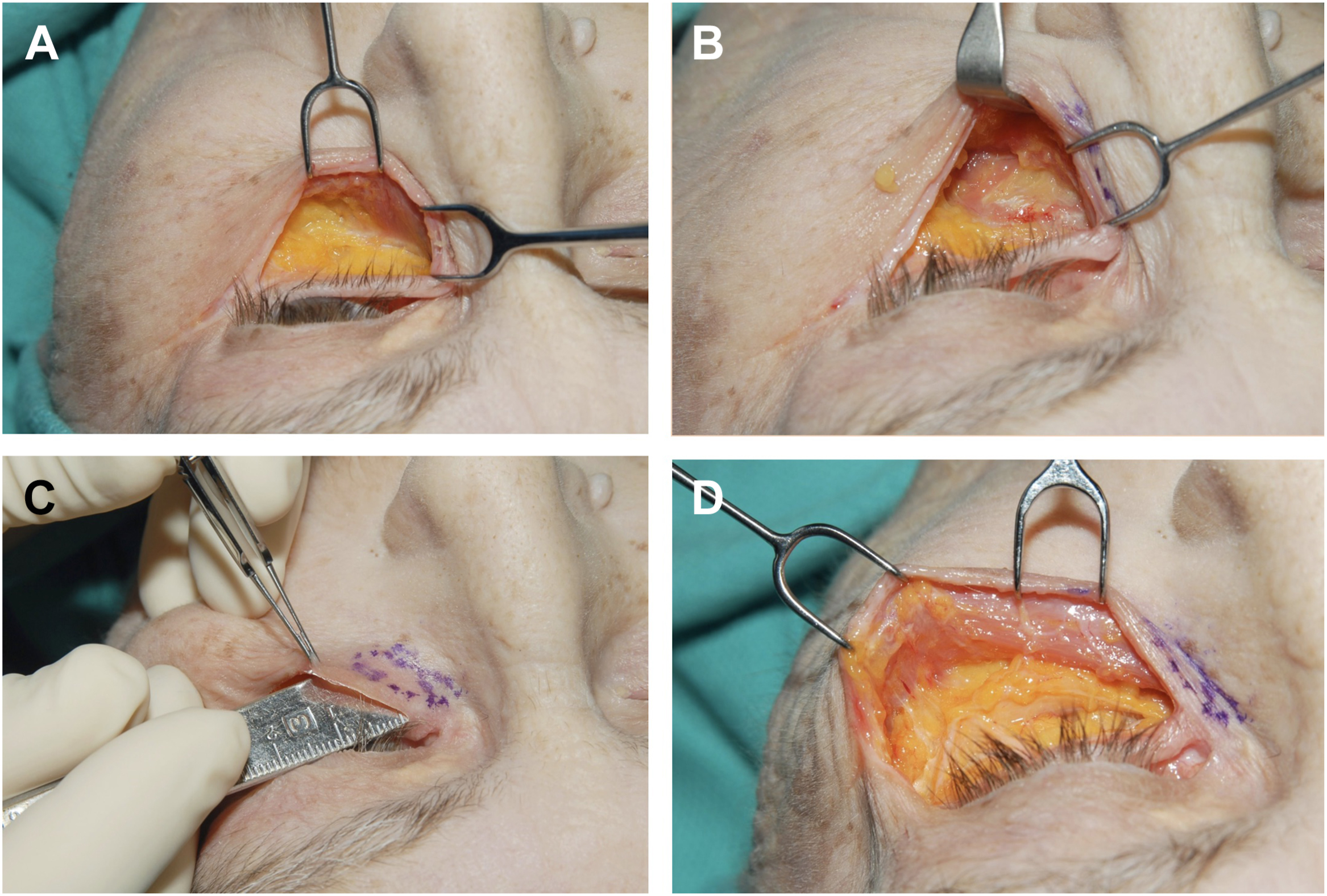
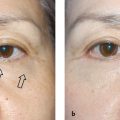
The transconjunctival approach to lower lid blepharoplasty places a concealed scar on the inner conjunctival surface of the eyelid. This method is primarily used to manage periorbital fat and when used as an isolated approach is particularly beneficial for patients who require fat repositioning or removal without the need to address excess skin ( Fig. 1 ). A notable advantage of transconjunctival approaches is that the orbital septum and orbicularis oculi are preserved, thereby preserving muscle function and reducing the risk of postoperative complications such as lower lid malposition. , Transconjunctival approaches are subdivided into pre-septal and post-septal dissection techniques, each with distinct advantages and disadvantages.
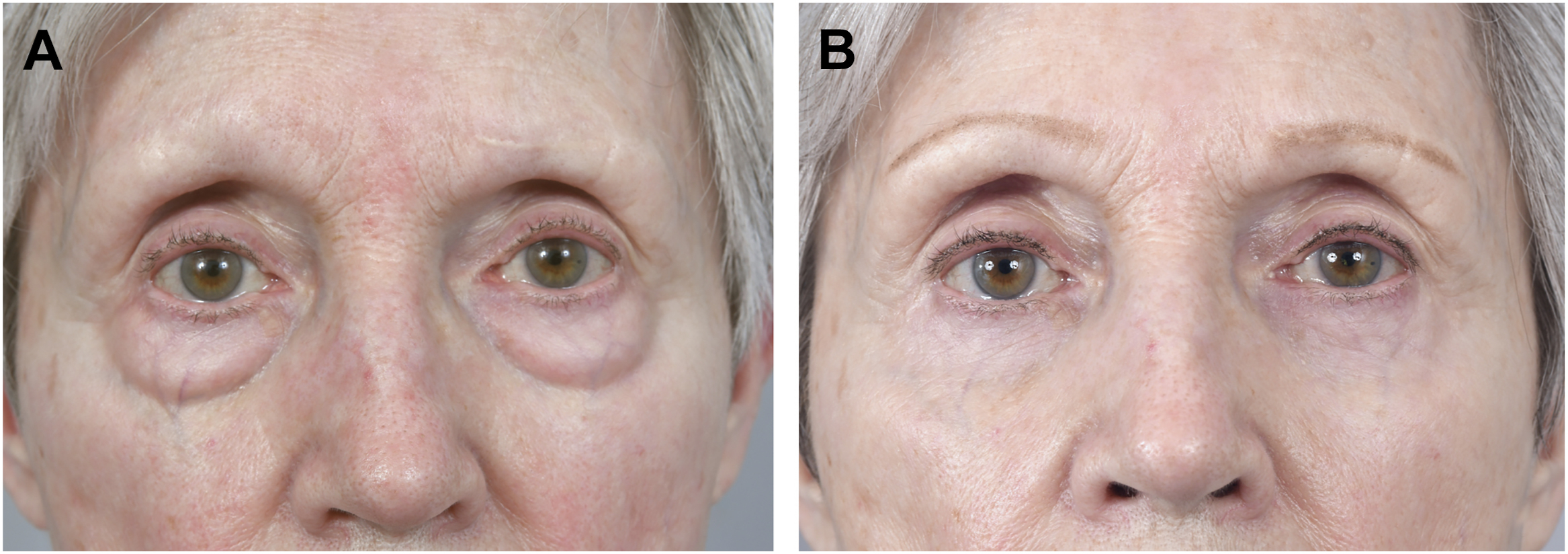
Some argue that the pre-septal dissection is most appropriate for patients with more advanced aging in the lower lid. It is ideal for patients with excess fat, minimal skin redundancy, and those with mild problems at the lid–cheek junction. This approach adequately addresses fat pseudoherniation, and can effectively blend the lid–cheek junction through by release of the orbicularis retaining ligament and fat resection, repositioning, or diced fat grafting. Excessive skin can be addressed via inside-out approach with skin flap undermining or skin pinch without violating orbicularis and minimizing middle lamellar scarring. , The pre-septal approach is more complex than the post-septal approach, requiring precise dissection between septum and orbicularis muscle. The procedure involves making a conjunctival incision just inferior to the lower tarsal border. Dissection proceeds between the orbicularis muscle and the orbital septum to the level of the orbital rim. The unviolated septum contains preaponeurotic fat within the orbit, which allows for clean dissection without visual obstruction by herniated orbital fat. Release of the medial orbicularis and orbicularis retaining ligament (ORL) allows fat repositioning along the anterior orbital rim. More complex problems including significant cheek ptosis can be addressed by incising lateral to the palpebral performing a canthotomy and using this combined approach to address problems involving the midface.
In contrast, the post-septal approach is technically straightforward. This technique provides direct access to orbital fat, enabling direct removal of excess orbital fat without violating the orbital septum. The reduced dissection in the post-septal approach typically results in a lower risk of postoperative edema and a faster recovery. The procedure involves making a conjunctival incision at least 5 mm below the tarsal border, as posterior as the conjunctival fornix. Dissection proceeds through the conjunctiva and capsulopalpebral fascia to directly access orbital fat. Fat resection and/or repositioning removal is precise and focused to improve contour. With these transconjunctival approaches access is more limited than when the subciliary approach is used. Therefore, when fat repositioning is performed suturing fat and septum along the anterior maxilla is performed transcutaneously.
Neither transconjunctival dissection technique addresses anterior lamellar excess, which may require additional procedures for optimal results. In patients with mild or moderate skin excess, adjunctive procedures such as skin pinch, “inside/outside” skin flap, fat grafting of the lid cheek junction or resurfacing techniques such as trichloroacetic acid, or phenol croton oil peel can be beneficial. ,
Subciliary approach
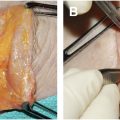
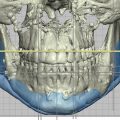
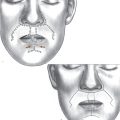
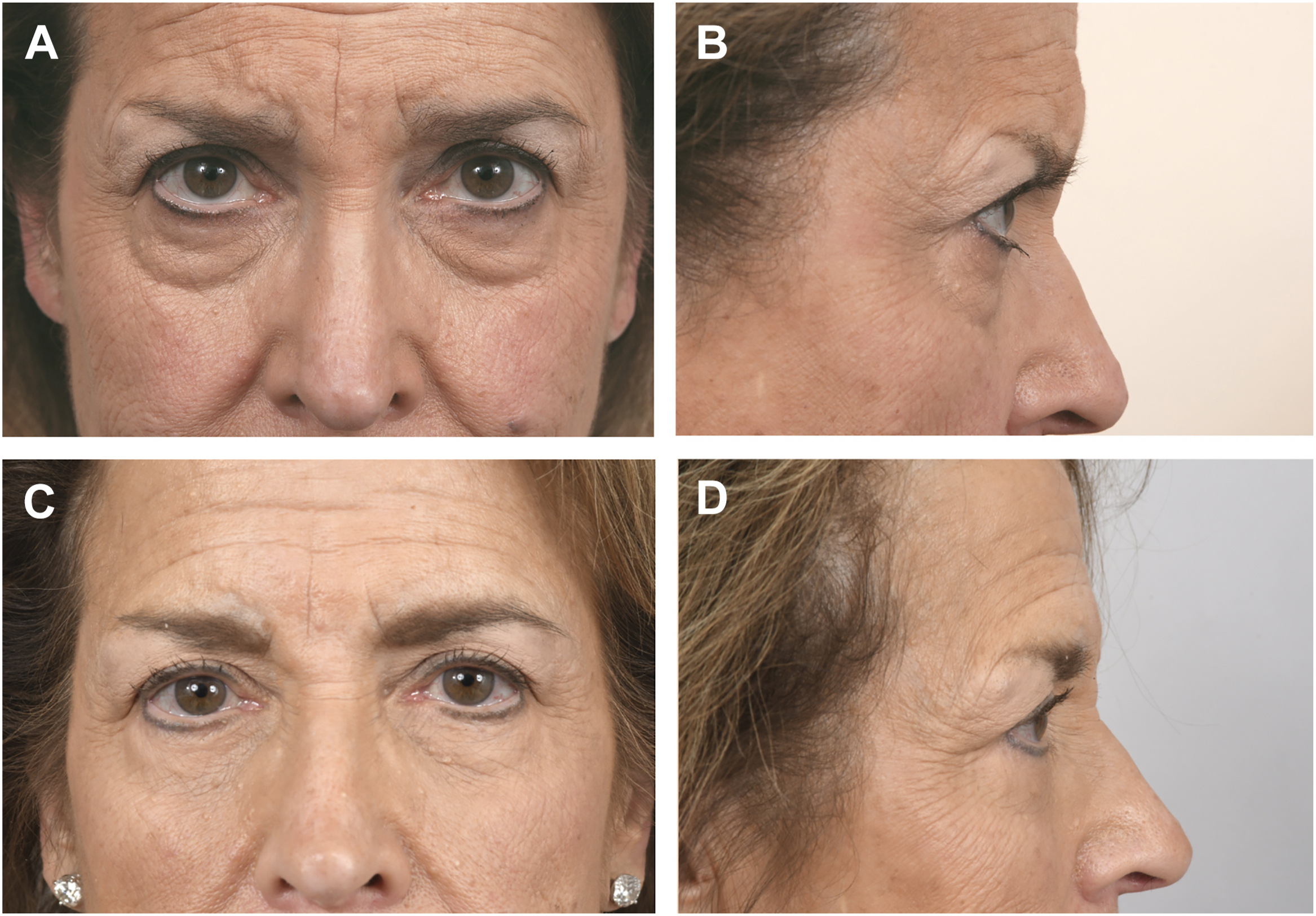
The subciliary approach provides significant versatility in addressing complex problems of lower lid. Appropriate patients for the subciliary approach are those patients with more significant anterior lamellar excess, more significant deformities of the lid–cheek junction, and prominent midface descent or malar mounds ( Fig. 2 ). Arcus marginalis release, fat removal or repositioning, skin–muscle flaps, skin pinch, skin only flaps, and lower lid tightening can all be accurately accomplished through this approach. Additionally, subciliary exposure of the lateral retinaculum provides additional flexibility to address lower lid laxity with canthal tightening procedures. Main drawbacks include a higher reported incidence of lid malposition due to manipulation, and risk for vertical shortening, of the anterior lamella.
Skin–Muscle Flap
The skin–muscle flap provides wide access to all structures associated with the lower lid. This allows effective treatment of excess lower lid skin and more significant lid–cheek junction and cheek ptosis problems. This technique allows for the tailored excision of muscle and skin components through either separate or composite flap elevation. Elevation of the orbicularis muscle flap and orbicularis suspension combined with lower lid canthopexy provides superior control of re-draping and augments lower lid support.
The procedure commences with an incision 2 to 3 mm below the lower lid margin, just below the lash line. A skin only flap is initially elevated for approximately 5 mm to maintain pretarsal orbicularis oculi muscle and thus preserve lower eyelid tone. The muscle is then incised, and a myocutaneous flap is dissected caudally in a pre-septal plane to the level of the inferior orbital rim ( Fig. 3 A ). The medial orbicularis muscle and the orbicularis retaining ligament are released to the medial corneoscleral limbus or extending laterally as needed to release the tear trough deformity and palpebromalar groove. Supraperiosteal dissection continues until the levator labii superioris muscle is visualized in order to effectively release the tear trough ligament (see Fig. 3 B and C). The orbital septum is released at the arcus marginalis to facilitate fat transposition over the orbital rim and further blend the lid–cheek junction.