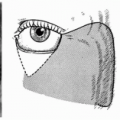
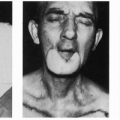
Latissimus Dorsi Musculocutaneous Flap for Pharyngoesophageal Reconstruction
F. E. BARTON JR.
J. M. KENKEL
W. P. ADAMS JR.
Despite recent advances in microsurgical techniques, regional pedicled flaps remain the mainstay of reconstructive options for pharyngoesophageal reconstruction. The island pectoralis major musculocutaneous flap continues to be the preferred flap of many reconstructive surgeons; however, the latissimus dorsi musculocutaneous flap is a safe and reliable alternative for reconstruction of partial and circumferential cervical esophageal defects (1, 2, 3).
INDICATIONS
The latissimus dorsi musculocutaneous flap may be used for any one-stage pharyngoesophageal reconstruction, but it should be considered the flap of choice in patients with large soft-tissue or cutaneous deficits, infected wounds, or irradiated beds that could not support microvascular transfer. The following are the advantages of the latissimus dorsi musculocutaneous flap for pharyngoesophageal reconstruction:
A large area of skin can be transferred while still closing the donor site primarily.
The cutaneous paddle is usually hairless, in contrast to flaps from the anterior chest in men.
The donor site is on the back, which is more acceptable to women than donor deformities on the anterior chest.
There is minimal functional loss from latissimus dorsi harvest.
The long vascular pedicle allows for a wide arc of rotation that easily reaches the nasopharynx.
The flap can be split into separate musculocutaneous units to be used for lining, soft-tissue fill, and skin cover or to preserve motor function at the flap donor site (4).
The vascular pedicle is away from the field of resection or irradiation in head and neck malignancies.
ANATOMY
The latissimus dorsi is a flat muscle extending obliquely across the back. It originates from the lower six thoracic vertebrae, lumbar and sacral vertebrae, iliac crest, and external surface of the lower four ribs, and it inserts on the intertubercular groove of the humerus (5, 6). The neurovascular anatomy of the latissimus dorsi flap was expertly described previously (7, 8, 9, 10, 11). The thoracodorsal artery originates from the subscapular artery and is the principal blood supply to the latissimus dorsi muscle. One to three arterial branches to the chest wall are given off before the thoracodorsal artery enters the latissimus dorsi muscle (7). The neurovascular pedicle enters the muscle on its undersurface about 8 to 10 cm from its origin (8) and 8 to 12 cm below its humeral insertion. The vessels bifurcate about 2 cm after entering the muscle. The superior branch traverses the muscle parallel to its border approximately 3.5 cm from the upper edge. The lateral branch parallels the posterior border of the muscle some 2 cm from its edge (7). Cutaneous perforators emanate from these branches and appear at regular patterns 3 to 5 cm apart (1, 12, 13). In cadaveric injection studies of the thoracodorsal artery, the lower third of the muscle and its overlying skin consistently do not fill with contrast medium, which indicates this portion of the muscle and skin are unreliable for use as a musculocutaneous flap (1, 12).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree