What organism is found in all the hand infections?
Staphylococcus aureus. Seen in 50% to 80% of infections.
 What are the most common bacteria involved in acute hand infections?
What are the most common bacteria involved in acute hand infections?
Staphylococcus aureus (up to 60%) and beta-hemolytic streptococci.
 What proportion of hand infections are polymicrobial?
What proportion of hand infections are polymicrobial?
Over half.
 What is the basic treatment principle when dealing with infections of the hand?
What is the basic treatment principle when dealing with infections of the hand?
DICE. Drainage and Debridement. Immobilization. Chemotherapy (antibiotics). Elevation.
 What is the most common site of hand infections?
What is the most common site of hand infections?
Dorsal subcutaneous tissue. Followed by tendon, joint, bone, and the subfascia.
 What is the most common mechanism of hand infections?
What is the most common mechanism of hand infections?
Trauma, such as penetrating injuries or bites.
 How do superficial hand infections tend to be treated? Exception?
How do superficial hand infections tend to be treated? Exception?
With antibiotics, which can be supplemented with splinting depending on severity. Typical course if 14 to 21 days. Exception is necrotizing fasciitis, which requires early surgical intervention.
 How do deep hand infections tend to be treated?
How do deep hand infections tend to be treated?
Surgical irrigation and debridement in conjunction with antibiotics and splinting as indicated.
 What patient risk factors predispose them to hand infections?
What patient risk factors predispose them to hand infections?
Immunocompromised state, Intravenous (IV) drug abuse, diabetes mellitus, and steroid use. Microvascular disease and damage to blood supply, as in trauma, also impairs host immune response.
 What are the common pathogens found in diabetic patients with hand infections?
What are the common pathogens found in diabetic patients with hand infections?
Gram–negative and polymicrobial infections. Subepidermal abscesses are unique to this patient population.
 How do hand infections in immunocompromised patients behave?
How do hand infections in immunocompromised patients behave?
Hand infections in this population tend to run a virulent course; for example, herpetic whitlow will not resolve spontaneously and require antiviral agents.
 What characterizes cellulitis in the hand?
What characterizes cellulitis in the hand?
Characterized by erythema, swelling, and tenderness. Associated lymphangitis may indicate a more severe infection.
 What is the most commonly involved organism in cellulitis of the hand?
What is the most commonly involved organism in cellulitis of the hand?
Group A β-hemolytic Streptococcus.
 What other organism is also involved, specifically in less severe cases of cellulitis?
What other organism is also involved, specifically in less severe cases of cellulitis?
S. aureus.
 What are the oral antibiotics of choice in cellulitis of the hand?
What are the oral antibiotics of choice in cellulitis of the hand?
Nafcillin, dicloxacillin, and cephalexin; erythromycin, if allergic to penicillin.
 How do subcutaneous abscesses typically occur in the hand?
How do subcutaneous abscesses typically occur in the hand?
After a puncture wound or as a response to a retained foreign body.
 What are the most commonly isolated pathogens in human-bite infections?
What are the most commonly isolated pathogens in human-bite infections?
α-Hemolytic Streptococcus and S. aureus.
 What is the area most commonly involved in human bites?
What is the area most commonly involved in human bites?
The metacarpophalangeal joint, commonly referred to as “fight bites.”
 Where is the most common topography for occurrence of hand infections?
Where is the most common topography for occurrence of hand infections?
Flexor tendon zone injury II.
 What organism is commonly isolated in one-third of human bite wounds?
What organism is commonly isolated in one-third of human bite wounds?
Eikenella corrodens. Cultured in 7% to 29% of human bites. Must be cultured in 10% carbon dioxide. Destroys articular cartilage quickly.
 What is the recommended treatment of a human bite injury?
What is the recommended treatment of a human bite injury?
Surgical extension and debridement with arthrotomy and culture acquisition. The wound is left open.
 What organism commonly infects animal bites and scratch wounds?
What organism commonly infects animal bites and scratch wounds?
Pasteurella multocida.
 Why do you need an x-ray if the patient had a simple animal bite?
Why do you need an x-ray if the patient had a simple animal bite?
To rule out a retained foreign body like a broken tooth.
 How should animal bites be treated?
How should animal bites be treated?
Irrigation and oral amoxicillin-clavulanate, or IV ampicillin-sulbactam.
 What are the common cultures requested in hand infections?
What are the common cultures requested in hand infections?
Aerobic cultures, anaerobic cultures, cultures Löwenstein–Jensen medium for atypical Mycobacterium (Mycobacterium marinum at 32°C, Mycobacterium tuberculosis at 37°C).
 What are the common stains needed in hand infections?
What are the common stains needed in hand infections?
Gram stain, Ziehl–Neelsen stain (atypical Mycobacteria), Tzanck smear (herpes simplex virus).
 When evaluating a hand infection and a fungus is suspected, what preparation should be done for examination?
When evaluating a hand infection and a fungus is suspected, what preparation should be done for examination?
Potassium hydroxide preparation.
 What is the most common infection in the hand in human immunodeficiency virus (HIV)–positive patients?
What is the most common infection in the hand in human immunodeficiency virus (HIV)–positive patients?
Herpes simplex infection.
 When using an aminoglycoside (e.g., gentamicin) for gram-negative coverage, what adverse effects are commonly overlooked?
When using an aminoglycoside (e.g., gentamicin) for gram-negative coverage, what adverse effects are commonly overlooked?
Nephrotoxicity and ototoxicity.
 What is the drug of choice for methicillin-sensitive S. aureus (MSSA) infections of the hand?
What is the drug of choice for methicillin-sensitive S. aureus (MSSA) infections of the hand?
Cephalexin, amoxicillin clavulanate (orally).
 What is the drug of choice for methicillin-resistant S. aureus (MRSA) infections of the hand?
What is the drug of choice for methicillin-resistant S. aureus (MRSA) infections of the hand?
Vancomycin.
 What is the current reported incidence of MRSA hand infections, and is it rising?
What is the current reported incidence of MRSA hand infections, and is it rising?
34–73% of all hand infections, Yes.
 What is the recommended empirical oral antibiotic for MRSA?
What is the recommended empirical oral antibiotic for MRSA?
Sulfamethoxazole/trimethoprim (Bactrim) covers 90% community-acquired MRSA, current recommendation is for 2 double-strength Bactrim tablets twice a day. Clindamycin and ciprofloxacin are also appropriate, however they have 50% and 40% resistance to community-acquired MRSA, respectively. The mecA gene, which codes for penicillin-binding protein 2A, provides its resistance to methicillin.
 Which is the most common hand infection?
Which is the most common hand infection?
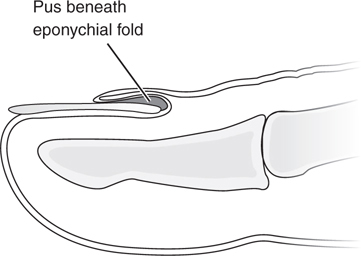
Paronychia. It is an infection beneath the eponychial fold or along the paronychial fold and nail plate. Not to be confused with perionychium, which is the skin around the nail margin (see Fig. 32-1).
Figure 32-1 Paronychial infection.
 Which is the area around the fingertip most resistant to infection?
Which is the area around the fingertip most resistant to infection?
The hyponychium is the most resistant area to infection.
 How do you treat an acute paronychia without abscess?
How do you treat an acute paronychia without abscess?
Warm water soaks with or without povidone or chlorhexidine and oral antibiotics. With and abscess in place, incision and drainage is recommended, routinely with removal of the nail plate.
 What is a runaround abscess?
What is a runaround abscess?
A paronychial infection that forms an abscess that tracks around beneath the entire nail fold superficial to the nail plate.
 In what type of patient population is chronic paronychial infection often seen?
In what type of patient population is chronic paronychial infection often seen?
Patients exposed to constant moisture such as dishwashers, swimmers, or medical professionals. Also, children who frequently dig in dirt.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree