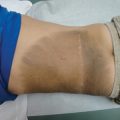
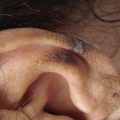
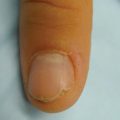
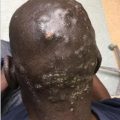
Disorders of skin pigmentation include those that make the skin lighter (hypopigmented). Appropriately recognizing disorders of hypopigmentation is important because many people assume that their skin will entirely depigment. Prompt diagnosis and treatment can assuage worries and improve outcomes. This chapter includes discussions of pityriasis alba, vitiligo, idiopathic guttate hypomelanosis, progressive macular hypopigmentation, and nevus anemicus. pityriasis alba vitiligo idiopathic guttate hypomelanosis progressive macular hypopigmentation nevus depigmentosus nevus anemicus Elizabeth Dupuy and Preeti Jhorar Pityriasis alba is a benign inflammatory skin condition that presents with poorly circumscribed hypopigmented oval or round macules, patches, or thin plaques. The important differential diagnoses include vitiligo, tinea versicolor, seborrheic dermatitis, nevus depigmentosus, nevus anemicus, postinflammatory hypopigmentation, mycosis fungoides, leprosy, and ash-leaf spots of tuberous sclerosis. Vitiligo is well demarcated, with a chalky-white appearance and no skin surface change, such as scale. Vitiligo is completely depigmented, whereas pityriasis alba is hypopigmented. A KOH preparation will reveal hyphae and spores in the case of tinea versicolor. It is commonly located on the upper chest and back, unlike pityriasis alba, which almost exclusively affects the cheeks. Especially in patients with darker skin tones, seborrheic dermatitis can present with hypopigmented macules or patches along the eyebrows, nasolabial folds, frontal hair line, and retroauricular skin. It may be associated with a greasy scale or scalp dandruff. Nevus depigmentosus is a congenital disorder of hypopigmentation that is present at birth or noticed shortly thereafter. It has an asymmetric distribution and is stable over time. Nevus anemicus is noticed at birth or in early childhood and presents as an irregular, hypopigmented patch. It is not truly a pigmentary disorder but is instead caused by vascular hypersensitivity that leads to vasoconstriction. It is typically a focal lesion. Pressing a glass slide onto the border of nevus anemicus will cause the hypopigmentation to expand out as the periphery blanches. Postinflammatory hypopigmentation can result from any inflammatory process on the skin, but there usually is a history of preceding rash. Mycosis fungoides involves multiple hypopigmented macules, usually in photoprotected areas. Referral to dermatology should be considered if there is a more extensive distribution of pityriasis alba-like lesions, especially in darker skin patients. Leprosy presents with hypoesthetic patches and can be considered with appropriate clinical history and geographic risk factor. In tuberous sclerosis, lesions are typically present at birth, can be tear-drop or ash-leaf shaped, and accentuate with a Wood lamp examination. In older patients, lesions can be associated with other features of tuberous sclerosis, such as facial angiofibromas. Referral to dermatology should be considered when there are doubts as to the diagnosis or if the clinical course is atypical. Pityriasis alba is included in the differential diagnosis of hypopigmented or depigmented patches. Patients and sometimes physicians may be concerned that these lesions represent a more ominous depigmenting condition or an infectious process. The white spots on your skin are caused by a condition called “pityriasis alba.” This is not an infection, and it is not contagious. The cause of this condition is unknown; however, some believe it is a feature of atopic dermatitis or eczema. This condition will improve over a period of a few months to years and gradually the skin will return to normal pigmentation. Treatment is not necessary but if your skin is itchy, or if you desire treatment, we can try to use a low-potency topical steroid. Topical steroids should not be used for extended periods of time because their use may lead to side effects, such as thinning of the skin. An alternative treatment is a nonsteroidal antiinflammatory called a “topical calcineurin inhibitor,” such as tacrolimus ointment or pimecrolimus cream. Although these are labeled with an FDA black box warning regarding a theoretical increase in risk for lymphoma, most dermatologists believe they are safe to use, and studies have not shown any increased risk for cancer with topical use. Other interventions that may improve the appearance of skin are the use of sun protection and moisturizers. Regina Liu, Amy R. Vandiver, and Preeti Jhorar Vitiligo is a common acquired disorder of pigmentation that results from the loss of functional melanocytes. Vitiligo affects approximately 0.5% to 2% of the population worldwide. The peak incidence is in the 10- to 30-year-old age group with an average age of onset of approximately 20 years, although it can manifest any time from shortly after birth to late adulthood.
8: Hypopigmented rashes
Abstract:
Pityriasis alba
Clinical features
Differential diagnosis
Vitiligo
Tinea versicolor
Seborrheic dermatitis
Nevus depigmentosus
Nevus anemicus
Postinflammatory hypopigmentation
Mycosis fungoides
Leprosy
Ash-leaf spots of tuberous sclerosis
Work-up
Initial steps in management
Warning signs/common pitfalls
Counseling
Vitiligo
Epidemiology
Clinical features
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Hypopigmented rashes