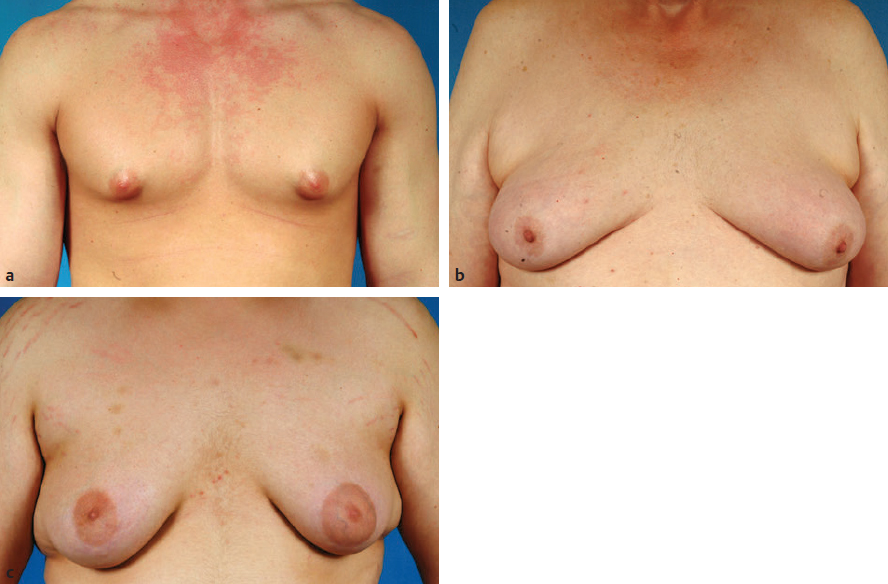
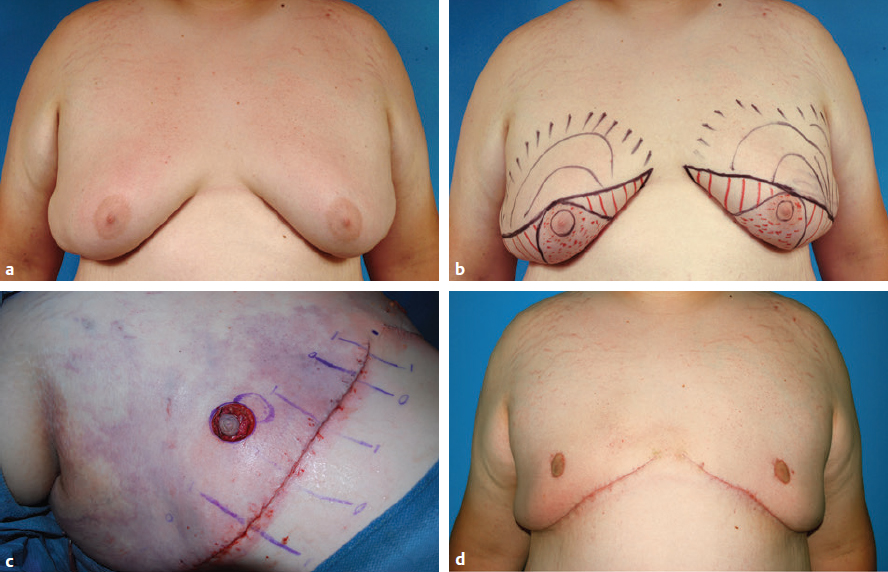
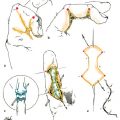
CHAPTER Gynecomastia is defined as an excessive development of mammary tissue of the male breast. It is the most common condition of the male breast, affecting up to 65% of normally developing adolescent boys.1 The severity of the condition may range from a small subareolar fibrotic bud to enlargement indistinguishable from the normal female breast (Fig. 37.1). Male breast enlargement is overwhelmingly a benign finding, but malignancy must be considered and ruled out in patients with asymmetric enlargement, a discrete lesion, or symptoms of pain and tenderness. Azzopardi2 and McDivitt et al3 demonstrated that although breast cancer is rare in men, it does occur and can account for 1% of all breast cancers. In particular, patients with Klinefelter’s syndrome show an association of breast cancer and gynecomastia.4,5 Gynecomastia can be subdivided into four categories based on the cause: (1) idiopathic (25%, most common), (2) physiologic, (3) pathologic, and (4) pharmacologic (Table 37.1). Pseudogynecomastia is an increase in breast size that occurs with weight gain. Typically, gynecomastia in adolescent males can be treated with patience and reassurance, because in most cases the breast simply regresses back to a normal appearance over a period of 1 to 2 years.6 However, the presence of hypertrophic breast tissue for more than 12 months warrants surgical treatment because of the tendency toward fibrotic transformation, which can be permanent.7,8 Also, if any degree of social withdrawal is noticeable as a result of even a mild condition, surgical correction is entirely reasonable and recommended. Fig. 37.1 Manifestations of gynecomastia. (a) A firm and fibrous mass of tissue may develop directly under the areola. This mass herniates through the elastic areolar skin and causes widening of the areolar diameter. (b) In more obese patients, accumulation of fibrofatty stroma surrounding the breast results in a more prominent breastlike contour. (c) As the subareolar breast bud enlarges along with a general increase in the volume of the breast, the breast bud herniates through the elastic areolar skin, resulting in a widened areolar diameter. Table 37.1 Types of gynecomastia
37
Gynecomastia
Cause | Comments |
Idiopathic | Most common (25%) |
Physiological | Neonatal: Influence of maternal estrogens Pubertal: Elevated estradiol to estrogen ratio Senile: Peripheral conversion of testosterone to estrogen by aromatase |
Pathologic | Liver cirrhosis; kidney failure; testicular, adrenocortical, or pituitary tumors; hypogonadism; hyperthyroid; adrenal hyperplasia; or bronchogenic carcinoma |
Pharmacologic | Estrogens, gonadotropins, androgens, antiandrogens, chemotherapy agents, calcium channel blockers, angiotensin-converting enzyme inhibitors, digitalis, central nervous system agents, antituberculosis medications, or drugs of abuse |
Table 37.2 Staging system of gynecomastia
Grade | Degree |
Grade I | Minimal hypertrophy (< 250 g) and no ptosis |
Grade II | Moderate hypertrophy (250 to 500 g) and no ptosis |
Grade III | Severe hypertrophy (> 500 g) and grade I ptosis |
Grade IV | Severe hypertrophy (> 500 g) and grade II or III ptosis |
To determine the appropriate means of treatment, the cause of gynecomastia must be identified and an evaluation of the extent of deformity should be completed. The cause is often ascertained by careful history taking, physical examination, and laboratory studies. The staging of gynecomastia is based on the degree of breast hypertrophy and ptosis9 (Table 37.2). The determination of the volume of the breast, fibrotic content versus fatty accumulation, and skin excess on the surrounding chest wall are important factors to assess in relation to the whole chest wall contour. These determinations will then guide the most appropriate treatment method.
Avoiding Unfavorable Results and Complications in Gynecomastia
Summary Box
Most Common Complications
• Seroma
• Contour irregularity
• Persistent subareolar mass
• Skin excess
• Insufficient volume reduction
• Hematoma
Preoperative Planning and Patient Selection
The character of the breast should be examined by palpation to assess for the presence of any type of discrete mass. Also, the consistency and size of the fibrous subareolar component is estimated as compared with the surrounding fibrofatty stroma. Fatty accumulation under the arm or up onto the chest wall must be noted along with the degree of areolar herniation or widening. Breast imaging is not usually recommended; however, when breast cancer is suspected, mammography should be performed.10
If surgery is indicated, the physician should thoroughly discuss the patient’s expectations. With patients with a high body mass index (BMI), there is sometimes a discrepancy between a surgeon’s perception of the appropriate chest wall contour in relation to the rest of trunk and the patient’s expectation from surgery. Setting realistic expectations and identifying areas of specific concern are helpful in allowing the surgeon to judge when an appropriate end point is reached intraoperatively. Specifically, any preoperative asymmetry and contour irregularity should be noted and patients should be informed about the need for further procedures, especially when liposuction is used alone or staged excision is planned.
There are various surgical options, chosen based on the individual patient characteristics. The two factors that must be addressed are the volume of the breast and the degree of skin redundancy. The breast tissue may be removed with either liposuction or direct excision or a combination of the two. Excision of the skin envelope is recommended if enough spontaneous skin contraction cannot occur in the setting of significant excess and poor elasticity.
Intraoperative Decisions
Volume Reduction
Direct Excision
Direct excision of glandular tissue through an inferior periareolar incision is preferable for cases of an isolated fibrous mass found directly under the areola without any significant surrounding fibrofatty stroma in the periphery of the breast. In this case, the subareolar mass creates a very obvious contour deformity as it herniates through the areola. Direct excision is especially helpful for young patients because the skin will often shrink to an acceptable diameter. The primary concern of this technique is leaving adequate tissue under the nipple to prevent nipple retraction (saucer deformity). The fibrous bud is sharply transected such that approximately 5 to 10 mm of evenly layered fibrous tissue remains attached to the underside of the areola. Because there is no fat directly under the areola, if the subareolar breast bud is removed at the dermal level, a step-off will be created at the junction of the areola, creating a postoperative contour deformity. After removing the subareolar tissue, if any contour irregularity is noticed, sharp dissection can be used to further thin the peripheral margins to create a smooth contour. With removal of the subareolar tissue, the areola will typically retract to a more normal diameter because the mass effect of the underlying breast bud has been removed (Fig. 37.2).
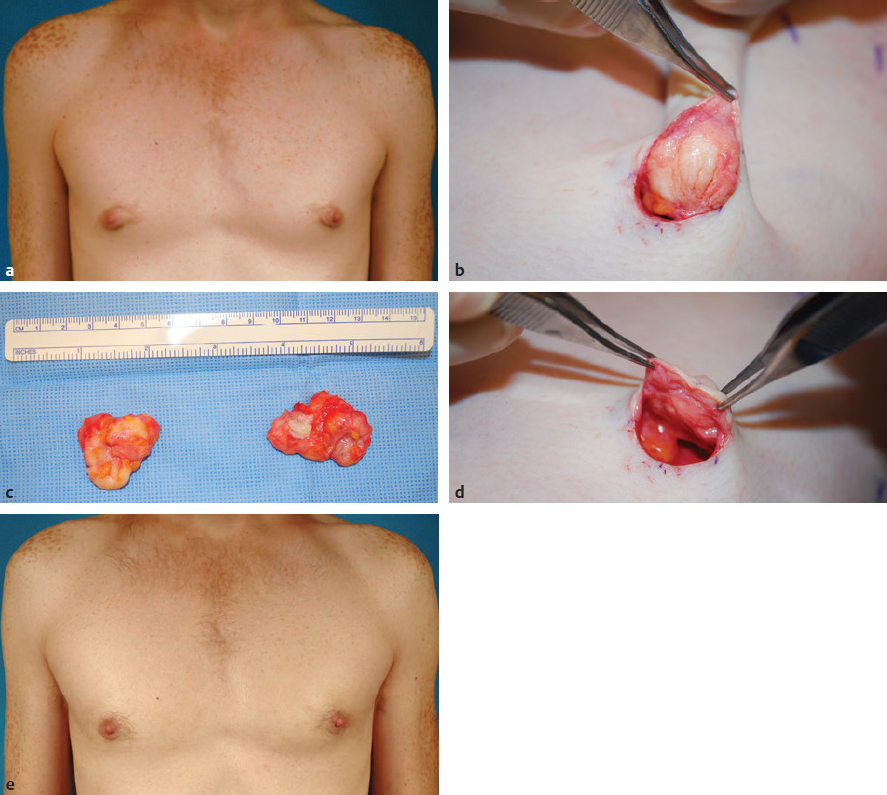
Fig. 37.2 This 14-year-old young man presented with bilateral gynecomastia of 2 years’ duration. (a) The breast enlargement consisted mostly of a firm subareolar fibrous mass with little surrounding fibrofatty accumulation. (b) At surgery, a well-demarcated subareolar fibrous mass was noted directly under the areola. (c) The mass was dissected free from the surrounding breast tissue through an inferior periareolar incision. (d) A thin layer of fibrous tissue remained attached to the underside of the areola to prevent a central depression deformity. (e) At 15 months postoperatively he has a smooth chest wall contour and the scar has healed well along the inferior border of the areola.
Liposuction
When gynecomastia presents as a largely fibrofatty accumulation of tissue, liposuction is recommended to restore a normal chest wall contour. The incision is placed at the junction of the pigmented areolar skin with the nonpigmented chest wall skin to hide the subsequent scar. Additional incisions can be made anywhere along the inframammary fold, or laterally along the chest wall. After infiltration using the tumescent technique, standard lipo suction is started with a small cannula first to feather and break up the fibrous tissue followed by a larger cannula to separate the fat from the surrounding fibrous stroma. Particular attention is directed to the subareolar area to reduce the possibility of any remaining residual subareolar bulge postoperatively. Pinch compression with the opposite hand can help drive the dense fat into the tip of the cannula to further reduce the volume of the breast. End points are determined by a pinch test and a contour assessment in a sitting position (Fig. 37.3).
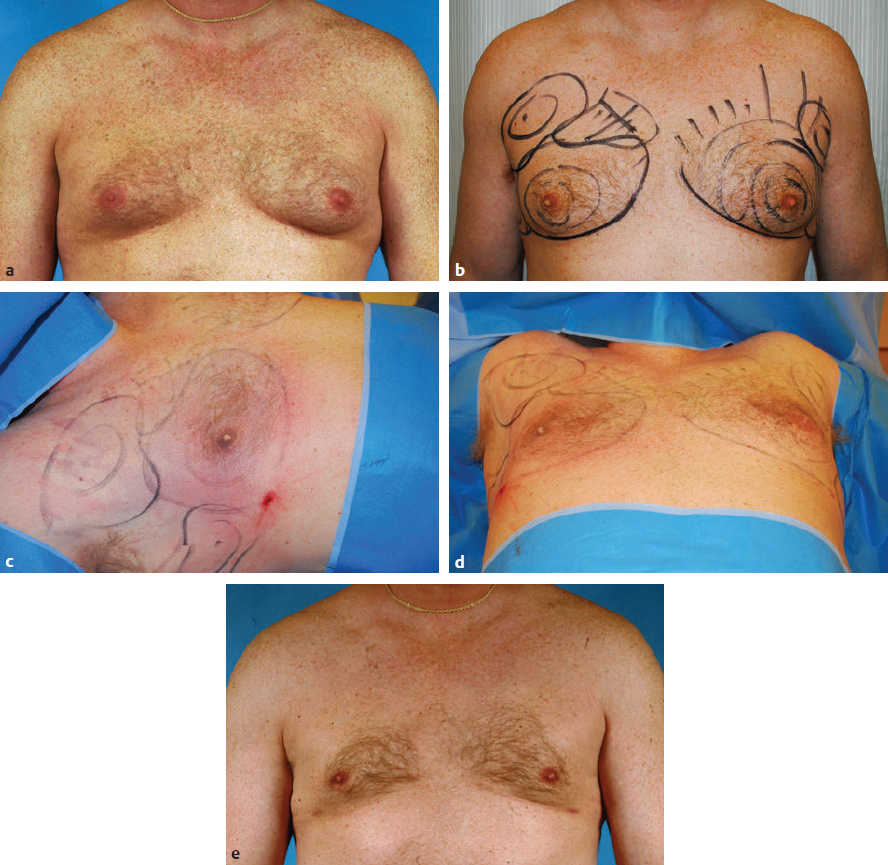
Fig. 37.3 (a) This 43-year-old man presented with bilateral gynecomastia. Because most breast enlargement consists of a fibrofatty component, simple liposuction can be used to manage the volume excess. (b) Preoperative markings outlining the areas to be treated. (c) The stab incision for liposuction was made in the lateral part of the inframammary fold, and liposuction was performed over the entire breast including under the arm, superiorly along the upper chest, and inferiorly below the fold to create a smooth contour. (d) When viewed from below, a flat and smooth contour of the chest wall can be confirmed on the right side; the left side was not yet treated. (e) At 2 months postoperatively he has a smooth chest wall contour.
Combination of Direct Excision and Liposuction
When a firm subareolar fibrous breast bud is present with a peripherally located supporting fibrofatty stroma, subareolar tissue is removed by direct excision. Liposuction is then used to reduce the general volume and recontour the peripheral margins. After the breast is tumesced through a stab incision, standard or ultrasonic liposuction is performed to evenly remove fatty tissue throughout the entire breast, including the centrally located fibrous component.11 Although the dense subareolar tissue is relatively refractory to liposuction, every effort should be made to honeycomb through the subareolar area as much as possible. Because the architectural integrity of subareolar tissue is interrupted by liposuction, the margin between the fibrous mass and fatty stroma becomes obvious, and it expedites the subsequent dissection of the fibrous bud through an inferior periareolar incision. When removing the subareolar mass by direct excision, leaving enough tissue under the nipple is critical to prevent a central depression or saucer deformity. Additional liposuction can be performed to feather the edges of the dissection to prevent a contour irregularity.
Skin Envelope Retailoring
With a reduction of breast volume, the skin may be excessive enough that some type of skin resection becomes necessary. In most patients, primary skin envelope retailoring is not required, because the skin envelope of the breast has a propensity to retract after direct excision or liposuction. However, if patients present with a significant skin excess along with extreme skin laxity and poor elasticity, a primary skin-reducing procedure may be indicated. One alternative is to perform the volume reduction initially and then proceed with a staged skin excision at a later time. This strategy allows the skin to retract and can make the subsequent skin resection a less involved procedure, possibly with a reduced scar burden (Fig. 37.4).
The design for skin envelope reduction in gynecomastia surgery is very similar to that used in mastopexy procedures in female patients. Based on the amount of excess skin, various patterns can be used to remove the excessive skin envelope, including direct local excision using either a periareolar pattern, a circumvertical pattern, or a simple horizontal ellipse. Drains should be used when extensive resection and undermining are performed to prevent seroma formation. The major goal of this procedure is the removal of the excess skin, lifting of the nipple–areola complex (NAC), and the reshaping of the breast to restore a normal chest wall contour with minimal cutaneous scars.
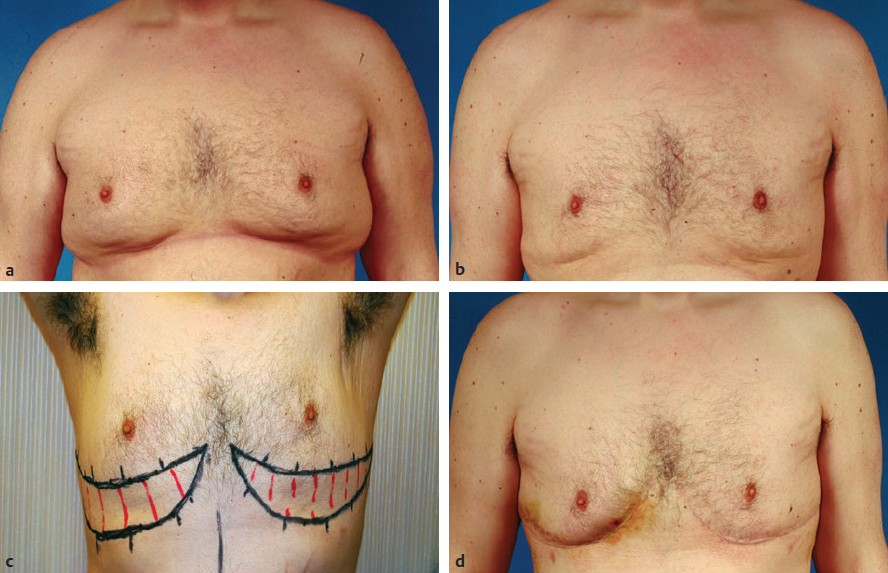
Fig. 37.4 (a) This 26-year-old man had bilateral gynecomastia. (b) At 10 months postoperatively, after liposuction treatment alone, the breast volume was significantly reduced; however, the skin envelope was redundant along the inframammary fold. (c) Preoperative marking in preparation for excision of the redundant skin. At surgery, the redundant skin and subcutaneous fat was excised to reshape the chest wall contour. (d) At 3 weeks postoperatively he has a smooth chest wall contour with a well-hidden scar in the fold.
Nipple–Areola Complex
Periareolar Pattern
When lifting of the NAC and a small reduction of the skin envelope are required, the periareolar pattern is a useful technique, because the resulting scar is camouflaged around the areolar border. The location and size of the NAC should be given special attention when marking a patient with gynecomastia. Because the nipple position is naturally located slightly lower than in females, the top of the periareolar incision should be located no more than 2 to 3 cm above the inframammary fold. The periareolar pattern is drawn in a circular fashion with the areola under stretch at a maximum diameter of 3 cm, a diameter that is somewhat smaller than that used for women. Once the marking is completed, the intervening skin is deepithelialized and the resulting defect is managed with a periareolar purse-string suture. From a technical perspective, the interlocking Gore-Tex technique is used to limit the amount of postoperative areolar spreading that occurs.12
Circumvertical Pattern
The circumvertical pattern has the advantage of lifting the NAC as well as reducing the skin excess in patients who need skin envelope reduction in both the vertical and horizontal directions. After most of the excess breast volume has been reduced by liposuction, the redundant lower pole skin is plicated by staples in the sitting position. After confirming the limits of skin resection, the inferior pedicle supporting the NAC is developed, leaving sufficient tissue on the pedicle to prevent compromise to the blood supply. The intervening skin on the vertical and periareolar segments is deepithelialized, and a purse-string suture is applied to close the periareolar incision.
Horizontal Pattern
A horizontally oriented pattern centered on the inframammary fold is a powerful technique that allows the removal of significant amounts of excess skin while leaving behind an inconspicuous scar. With this pattern, the blood supply to the NAC is provided by the inferior pedicle. The pedicle itself can be mildly undermined to create a smooth chest wall contour. When the horizontal incision is closed, the NAC is brought out through a separate incision to complete the procedure (Fig. 37.5).
Fig. 37.5 (a) This 23-year-old man had bilateral gynecomastia with significant volume and skin excess. (b) Preoperative marking in preparation for volume and skin reduction using an inferior pedicle technique in conjunction with a horizontal resection of skin. (c) Tissue is removed from around and under the inferior pedicle, and the apron flap is closed along the inframammary fold. The nipple–areola complex is brought out through a separate incision. (d) At 1 month postoperatively he has a normal chest wall contour and a well-healed scar located in the inframammary fold.
Postoperative Complications
Although the treatment of gynecomastia is usually straightforward, certain postoperative problems can occur that are unique to the procedure. Because the procedure is essentially a subcutaneous mastectomy, two problems that are common to all plastic surgery “undermining” procedures certainly come into play: seroma and hematoma. The rest relate to the contour of the chest wall left over after the tissue is removed. Perhaps the most important potential complication is irregularity of the soft tissue envelope after resection of the fibrous bud and fat. Every aspect of treatment is geared toward preventing this complication, and it is here that a considered operative technique becomes most important. Conversely, in an attempt to avoid an overdone resection, the opposite problem can occur from time to time: underresection of tissue, too much retained tissue under the NAC, or an excessive or ptotic skin envelope. It is achieving this balance between resection and result that distinguishes a technically adept approach (Video 37.1).
Managing Unfavorable Results and Complications in Gynecomastia
Asymmetry
All patients are asymmetrical preoperatively, but postoperative asymmetry is a very common complication noted by patients after any kind of breast surgery. Careful measurement of the amount of excised tissue and lipoaspirate removed and examination of the remaining tissue in the sitting position intraoperatively can minimize the possibility of significant postoperative asymmetry.
Incomplete Volume Reduction
Whereas overresection can create a concavity in the breast, underresection can result from too cautious an approach to management of the excess volume. Care must be taken to merge the two techniques of tissue removal, liposuction and direct removal of the fibrous bud from under the NAC, in such a way that a contoured chest wall is created while adequately reducing the size of the breast.
Surface Irregularity
Intraoperatively, the edges of the resection should be feathered by careful excision either with or without liposuction. These maneuvers are performed concurrently in an attempt to prevent an abrupt change in contour. Healthy skin flaps are left behind to ensure uncomplicated wound healing. When revision surgery is planned, it is recommended to treat the prominent areas first with specifically targeted liposuction using small cannulas, then treat any residual depressed areas using lipofilling.
Periareolar Scar Formation
Periareolar scar formation is a spectrum of complications in and around the NAC that includes hypertrophic scar of the incision site, nipple retraction, and areolar hypopigmentation. Nipple retraction can be preventable by leaving enough tissue under the NAC, and areolar hypopigmentation can be masked by tattooing.
Hematoma and Seroma
As with any soft tissue undermining procedure, the potential for hematoma formation and seroma accumulation must be anticipated. Direct hemostasis at the time of surgery and the use of a compression garment for several weeks postoperatively are helpful in preventing postoperative bleeding. When bleeding occurs, it generally develops within the first 24 hours. It is recommended that any type of hematoma be drained operatively to prevent subsequent scar contracture and deformation of the breast or NAC. The use of a drain is a matter of preference. Routine placement of a drain after tissue resection can certainly be supported; however, many patients can heal primarily without the inconvenience of dealing with a drain postoperatively. If a patient does develop seroma, simple intermittent aspiration until resolved will successfully treat the condition.
Infection
Although infection after gynecomastia excision is a very unusual finding, a short course of perioperative antibiotics is prudent, because surgery involves potentially contaminating lactiferous ducts. One dose given at the time of surgery is likely adequate prophylaxis.
Conclusion
The major goal in the surgical treatment of gynecomastia is to create a normal masculine chest wall contour with the least conspicuous scar possible. To develop a successful surgical plan for each patient, breast volume, degree of ptosis, amount of excess skin envelope, quality of breast tissue, and combined chest wall deformity should be assessed preoperatively. The volume reduction must be performed with precision to prevent overcorrection, undercorrection, or surface irregularity. Furthermore, the skin retailoring pattern must be strategically designed to address the skin excess with a minimal amount of scar. When these variables are carefully controlled, excellent results can be achieved.
References
2 Azzopardi JG. Problems in breast pathology. Philadelphia, PA: WB Saunders; 1979:322–324
6 Wise GJ, Roorda AK, Kalter R. Male breast disease. J Am Coll Surg 2005;200(2):255–269
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree