Prevalence of Self-Reported Sensitive Skin in Selected Larger Cohorts
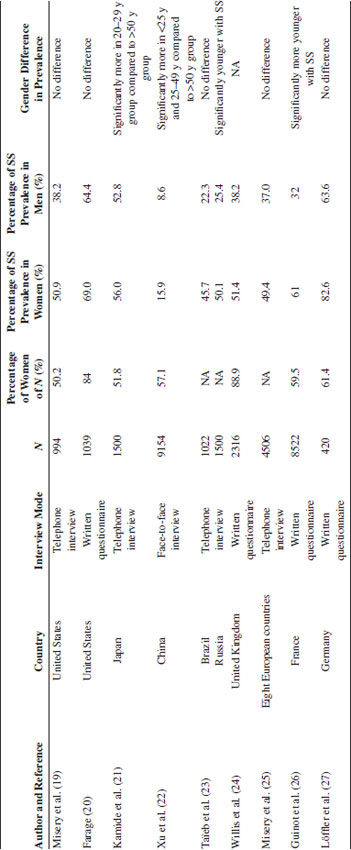
Note: N: number of participants; NA: not applicable; SS: sensitive skin; y: year.
A more varied picture appears with respect to age. About one-half of the studies report no difference. The rest report that significantly more young people than elderly complain of sensitive skin.
Potential Causes of Gender and Age Differences
Taking into consideration that it is well documented that more women than men suffer from self-declared sensitive skin and that there is tendencies toward more younger people than the elderly who experience this, surprisingly little research on gender- and age-related differences exist.
Age
As reported earlier, some studies indicate that the elderly exhibit a tendency to have higher sensation irritation thresholds (15–17), which was in accordance with the studies on visible skin irritants such as the tests with SLS (5–7). But if this was true, why do we only see a tendency of lower prevalence in elderly in half of the studies on self-reported sensitive skin? Xu et al.’s (22) and Guinot et al.’s (26) studies found significantly fewer persons with sensitive skin among the elderly compared to younger individuals in both genders (Table 15.1). They state that this finding might be linked to age-related experience and behavior and, therefore, a tendency to avoid environmental conditions and contact with certain triggering substances/products. Another possible explanation expressed by Xu et al. (22) is the fact that the elderly simply are not familiar with terms such as sensitive or skin susceptibility and, therefore, either do not express or experience suffering from it.
Gender
In general, more women than men report suffering from sensitive skin (Table 15.1). At this point, however, no evidence exists on the objective increase of skin susceptibility in women compared to men. Löffler’s group is the only one known to directly investigate a full cohort with prevalence of self-reported sensitive skin and physical skin tests (27). They investigated 420 volunteers, who completed a questionnaire with self-estimation of enhanced skin susceptibility. Volunteers were also tested with TEWL, cutaneous blood flow, and skin hydration. The researchers furthermore patch-tested 152 volunteers with SLS on the forearm. There were significantly more women than men reporting enhanced skin susceptibility, but no correlation was found between self-estimated skin susceptibility and the bioengineering values. Other groups have, as mentioned earlier, investigated variation in skin characteristics between genders, but unfortunately, it is not directly linked to prevalence of sensitive skin in the same cohorts. For example, it is shown that women have significantly thinner epidermis compared to men (but, curiously, it had no correlation with age) (4). It can be questioned if the right objective tests are being applied. As seen elsewhere in this book, many new modalities of physical examinations of patients reporting suffering from sensitive skin are in the pipeline, hopefully providing us with further knowledge.
Some have expressed that fluctuations in hormone levels in women could help explain why the reported prevalence of sensitive skin in women is around double that of men in some parts of the world. Among others, Misery et al. (19) expressed this theory, because the fluctuation in sex hormone levels seem to alter skin reactivity as demonstrated in 42 atopic women who underwent skin prick test and blood samples for sex hormones during their menstrual cycle. Others have also investigated this area and proposed that hormonal differences between genders may produce a greater inflammatory response in women compared to men (28–30).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree