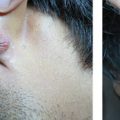
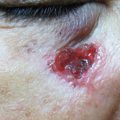
Fundamental features of radiofrequency surgery
The clinical effects of radiofrequency (RF) surgery are very much dependent upon the physical characteristics of the equipment as developed by the manufacturer. Among the physical characteristics, the clinical tissue effects depend upon the combination of RF parameters and the method of application to the tissues.
Physical Characteristics1
Radiofrequency in physics relates to the radio waves in the electromagnetic spectrum from 3 kHz to 300 GHz. But, in medicine only those between 200 kHz and 40 MHz are used. At radiofrequency below 100 kHz the nerve and muscle stimulation is very high, which can cause major or fatal side effects. The dermatological effects are observed best at frequencies above 500 kHz.
The principle of radiofrequency surgery is that the human tissues are heated to the extent of necrosis leading to a cut due to tissue impedance to radio waves delivered through the electrode. While the tissues are exposed to an alternating current (AC) at frequencies higher than 500 kHz there are chances of tissue burns or charring. To minimize the lateral tissue damage and to minimize chances of charring while doing surgery, there are some important physical parameters that when understood one can deliver the best results.
The physical parameters of utmost importance when using radiofrequency surgery are the following:
Frequency of radio waves—The higher the frequency above 1 MHz, the finer the cut, that is, the lateral heat dispersion is inversely proportional to the radiofrequency.
Electrode size—The larger the size of the electrode, the more the lateral heat dispersion, that is, the lateral heat dispersion is directly proportional to the size of electrodes.
Time of tissue contact—The higher the electrode contact time of the treated tissue, the more the lateral tissue damage, that is, lateral heat dispersion is directly proportional to time of electrode–tissue contact.
Radiofrequency power—Optimum power gives the best results, that is, lateral tissue damage is directly proportional to power.
Waveform—A fully filtered or cut waveform is least damaging to lateral tissues, whereas the blend (cut + coag) and electrocoagulation waveforms are more damaging to lateral tissues.
The practical applications of the physical characteristics can be summed up as follows: The radiofrequency of the equipment used will always remain constant in all procedures. Hence, to deliver the best results, one has to control the other parameters mentioned earlier. The higher the lateral tissue thermal dispersion, the higher the tissue damage. To deliver the best results, select the smallest or the thinnest electrode, use the cut or blend mode, keep the contact time of the electrode with tissue to a minimum, and use minimum required power.
Biological Characteristics
Advancements in the knowledge of electromagnetism and electronics have helped in development of newer RF equipment having different functions to suit and expand applications in clinical practice. This has been possible by developing these functions to suit the practitioner’s needs when operating on skin.
When operating on skin any dermatologic surgeon expects the following:
Cutting should be fine.
Bloodless cutting is preferable.
Coagulation ability after excision and for removing vascular lesions.
Ability to work very finely on superficial skin lesions.
Avoid postoperative sequelae of scarring.
The aforementioned expectations of a dermatologic surgeon are fulfilled successfully by the generation of waveforms. Refer to the upcoming section on functionality for the details about waveforms and their exact usefulness for versatility of applications. In brief, each waveform causes a different biologic outcome ranging from dehydration (electrodesiccation) to destruction or hemostasis (electrocoagulation) to tissue cutting (electrosection).
All radiofrequency surgery units are monopolar. Monopolar RF devices have an active electrode used for treating and a return electrode or ground plate/antenna plate that completes the electrical circuit. The treated patient is part of the electrical circuit. These units are also described as monopolar and biterminal (Figure 7.1). These functions are used for excision, destruction, and coagulation.
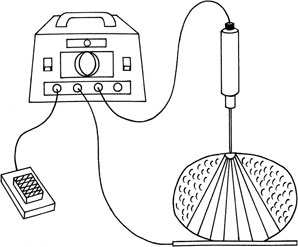
Figure 7.1Electrical circuit including patient (how electrical current flows during surgery). (Modified from Brown J, Minor Surgery: A Text and Atlas, 4th edition, Arnold Publishers, 2000, p. 312, Figure 42.1.)
The same radiofrequency surgery unit can be used without connecting the antenna plate. This application is termed monopolar monoterminal. Here, the radio waves generated are delivered through the active electrode at the lesion. This function is used only for superficial epidermal lesions at optimum power. This dehydrates and destroys the lesion, which can be immediately peeled off or allowed to peel off later. This is further described later as electrodesiccation and electrofulguration.
The principle on which the radiofrequency surgery works is the electrothermal effect. The high-frequency radio waves are generated by the AC current when they contact the skin. The electrode tip is always cold. The electrode tip upon reaching the skin delivers the radio waves, which travel through the human body toward the antenna plate. The skin and subcutaneous tissues resist the passage of radio waves. The resistance or impedance to the passage of radio waves creates subcellular water molecular friction. Water molecular friction generates tremendous heat to make subcellular water boil (see Figures 7.2 to 7.5). The generated heat dehydrates all concerned cells leading to necrosis and splitting of epidermis, dermis, and subcutaneous tissues as the case may be. The generated heat also coagulates proteins, coagulates blood vessels, and cuts nerve endings. The injury created by radio waves will depend on the waveform used, electrode tip size (spot size), and power used. In waveforms of electrodesiccation and electrofulguration, the absence of an antenna plate makes radio waves concentrate only over surface lesions without traversing through the body.
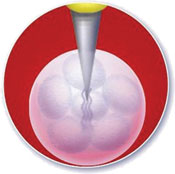
Figure 7.2Electrode touches skin.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree