Fig. 4.1
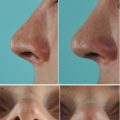
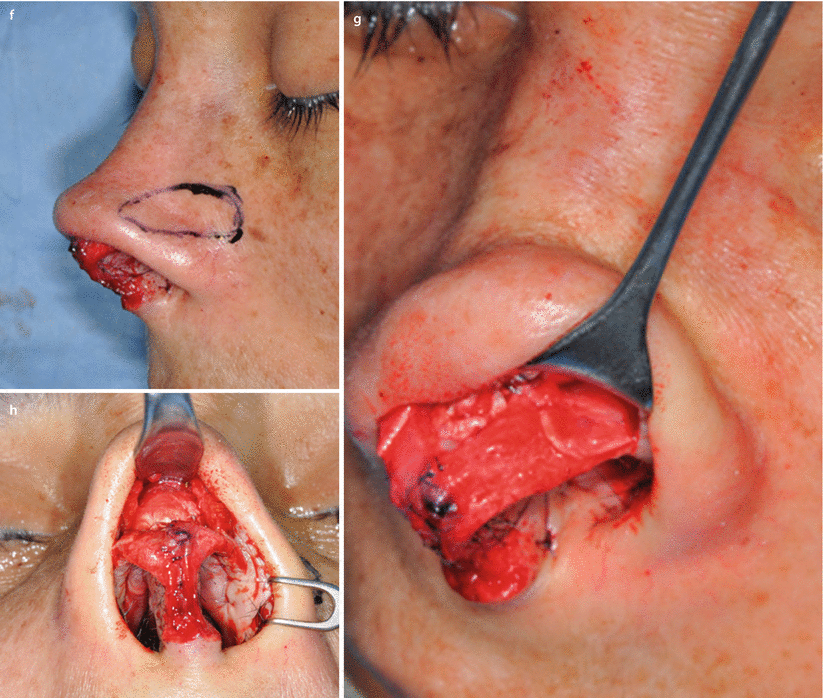
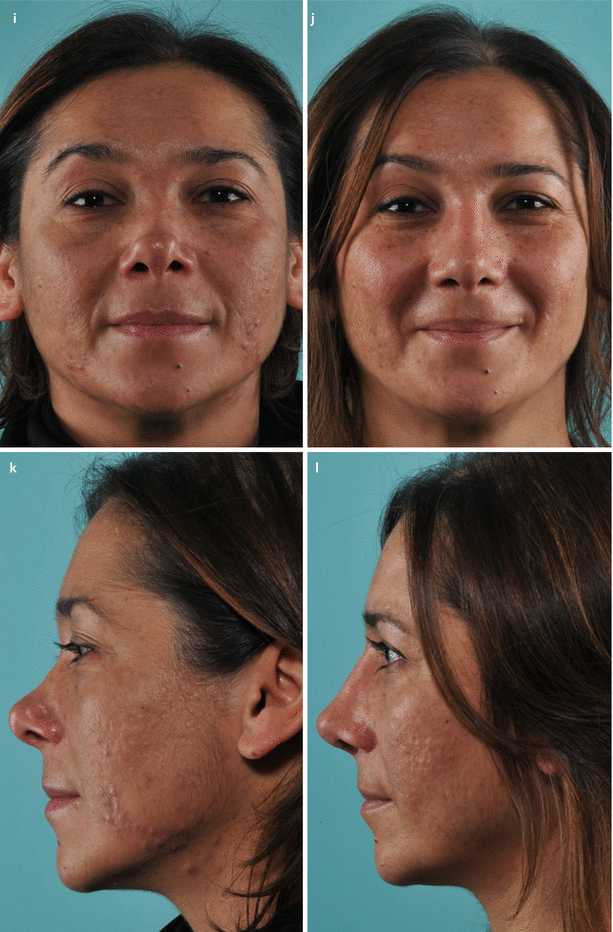
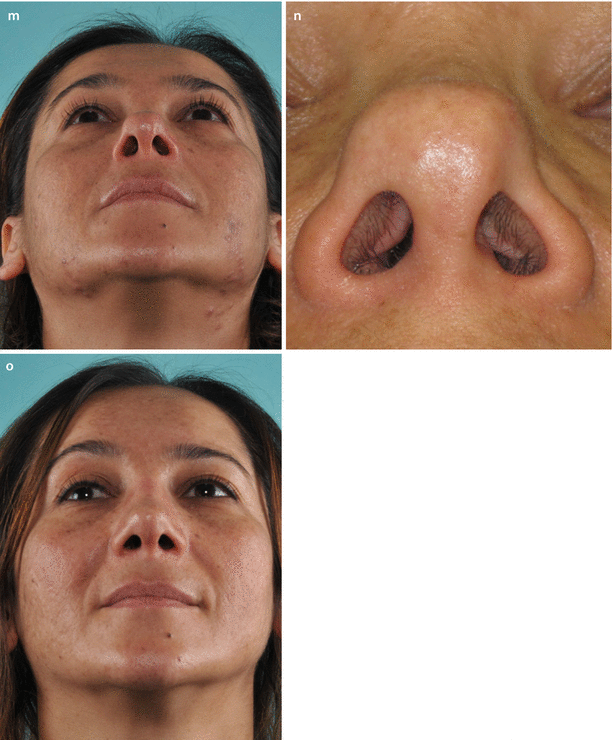
(a) Resected septal specimen with maximal anterior deviation corresponding to area of the left internal valve. (b) Profile view of the neoseptal construct with cephalically extended spreader grafts prior to reimplantation. Extended spreader grafts (needed to fill the open roof) sutured via multiple drill holes placed within the bony septum. (c) Dorsal view of the neoseptal construct. Drill holes placed in the nasal bones facilitate suture fixation of the construct at the keystone area. (d) Twisted alar cartilage framework and overresected lateral crura. (e) The axis was corrected by vertical dome division and suture reapproximation. A lateral crural strut graft was already fixated in its position. (f) Positioning of lateral crural strut grafts for increased support at the piriform aperture. Outline of desired graft position overlying the alar groove. (g) Fixated graft sutured to the left lateral crus. (h) Diced cartilage wrapped in allogenic fasciae used for dorsal augmentation (seen beneath the Aufricht retractor). (i) Frontal view demonstrating alar groove depressions and dorsal deficiency before and (j) result 6 months after revision rhinoplasty. (k) Preoperative profile view, (l) postoperative profile view. Base view (m) preoperatively; (n) closer base view demonstrating severe internal valve collapse; (o) postoperatively
4.3.2 Case 2: Spreader Grafts and Alar Batten Grafts
An 18-year-old female was seen after previous reduction rhinoplasty with complaints of postsurgical nasal airway obstruction and overprojection of the nasal tip and nasal root. Physical examination revealed pinched internal nasal valves and severe recurvature of the LLCs. LLC overresection was suspected. Revision surgery to widen and augment the middle vault was recommended rather than deprojecting the tip and nasal root. In this manner, a wider middle vault would help address the functional deficits, while a taller middle vault would avoid the visual impression of a significantly wider nose. Restructuring of the LLCs to eliminate concavity was also planned (Fig. 4.2).
Surgical Steps
- 1.
Harvest of septal cartilage.
- 2.
Spreader graft placement.
- 3.
Middle vault suspension by reattaching ULCs to the uppermost dorsal septum in near horizontal orientation.
- 4.
Intradomal and interdomal suture placement.
- 5.
Vertical infolding of the cephalic LLC, longitudinal scoring, and spanning suture placement.
- 6.
Bilateral batten graft placement.
- 7.
Dorsal augmentation with allogenic fascia grafts.
Ultimately the patient accepted the profile augmentation in exchange for much better breathing.
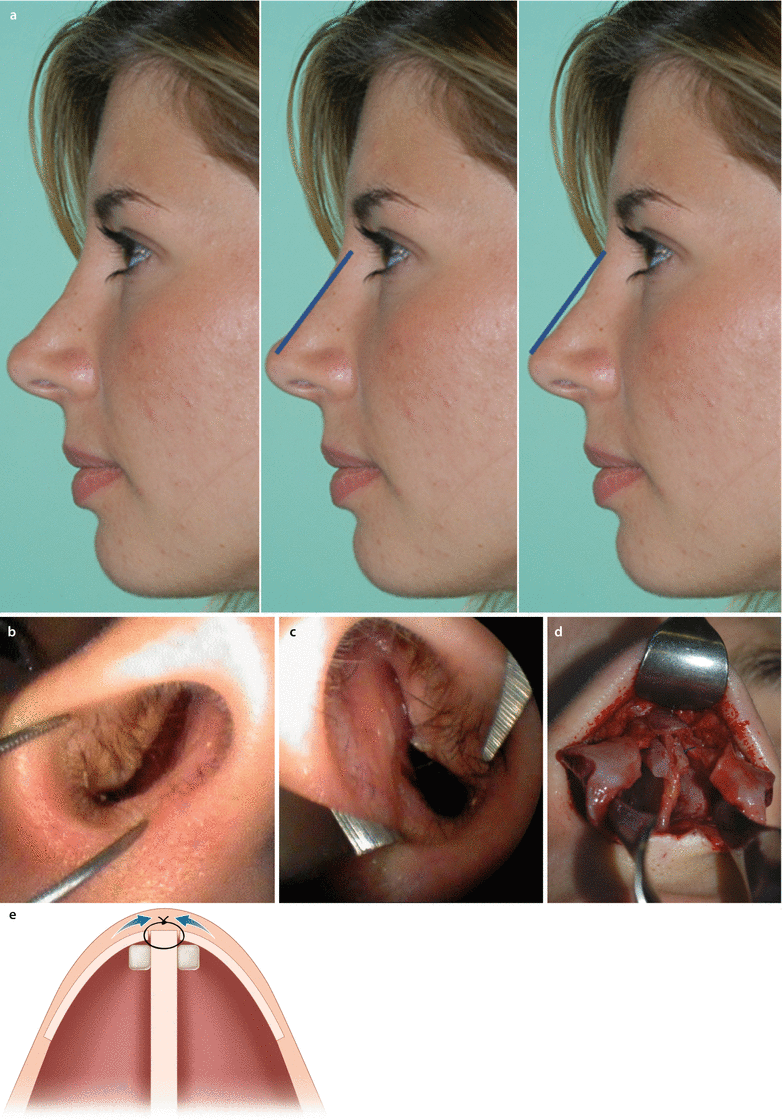
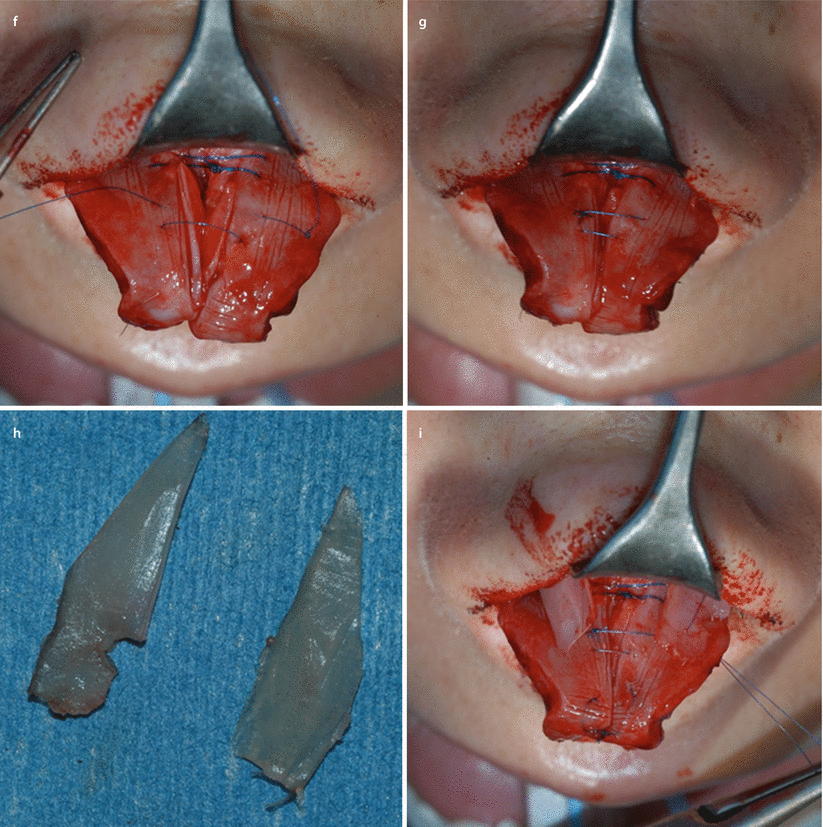

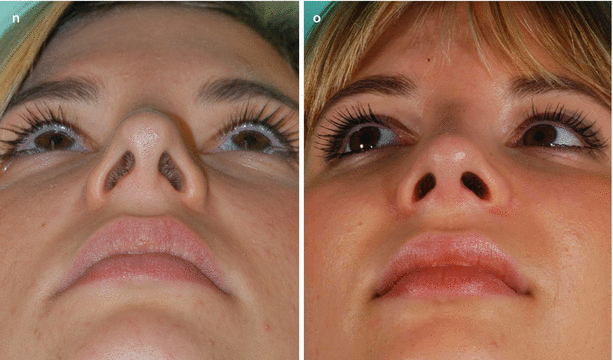
Fig. 4.2
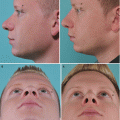
(a) Left, profile prior to revision surgery; center, patient’s (initial) desired profile; and right, the recommended profile. (b) Right prerevision endonasal view and (c) left prerevision endonasal view. (d) Intraoperative view of spreader graft and suture reattachment of ULCs and (e) schematic view of spreader grafts and suture reattachment of ULCs. (f) Rectangular infolding of the cephalic rim in L shape for improved rigidity against collapse and (g) simultaneous supratip narrowing effect by flaring sutures. (h) Septal cartilage batten grafts; (i) grafts sutured on top of the LLCs. (j) Prerevision frontal view and (k) postrevision frontal view with improved airway function. (l) Prerevision profile view and (m) postrevision profile view with improved airway function. (n) Prerevision base view and (o) postrevision base view with improved airway function
4.3.3 Case 3: Bony Out-Fracture and Spreader Grafts
A 44-year-old male hemophiliac (Fig. 4.3) with a history of multiple prior nasal surgeries, including septorhinoplasty, presented complaining of worsening nasal airway obstruction and frequent sinus headaches. Recurrent frontal sinusitis with multiple courses of antibiotic therapy led to the development of pseudomembranous colitis, making the patient extremely apprehensive about further treatment. His anxiety was heightened by the refusal of other surgeons to reoperate. Physical examination revealed an exceedingly narrow bony nasal vault with greater narrowing on the right. Endoscopic examination confirmed an ultranarrow bony vault. A surgically widened bony nasal vault was recommended to improve nasal airway obstruction and frontal sinus aeration. The patient was advised about the high probability of treatment failure. Increased tip projection and dorsal augmentation were also recommended to minimize the visual appearance of excessive nasal width and to create a balanced nasal contour.
Surgical Steps
- 1.
Harvest of left conchal and tragal cartilages.
- 2.
Parasagittal median, transverse, and low-low lateral osteotomies to open both the bony base and roof.
- 3.
Extended butterfly-type spreader graft placement to maintain widening of the bony vault.
- 4.
Septal extension graft placement to enable tongue-in-groove tip support.
- 5.
Excision of scarred soft tissues from the supratip area.
- 6.
Placement of diced cartilage wrapped in allogenic fascia to the nasal dorsum for additional augmentation.
The postoperative course was uneventful. Epistaxis was avoided with a combination of clotting factor replacement and application of inflatable nasal packs with hemostatic coating. At long-term follow-up, the patient reported a marked improvement in nasal airflow, a substantial reduction in sinus infections, and far less anxiety regarding his nose.
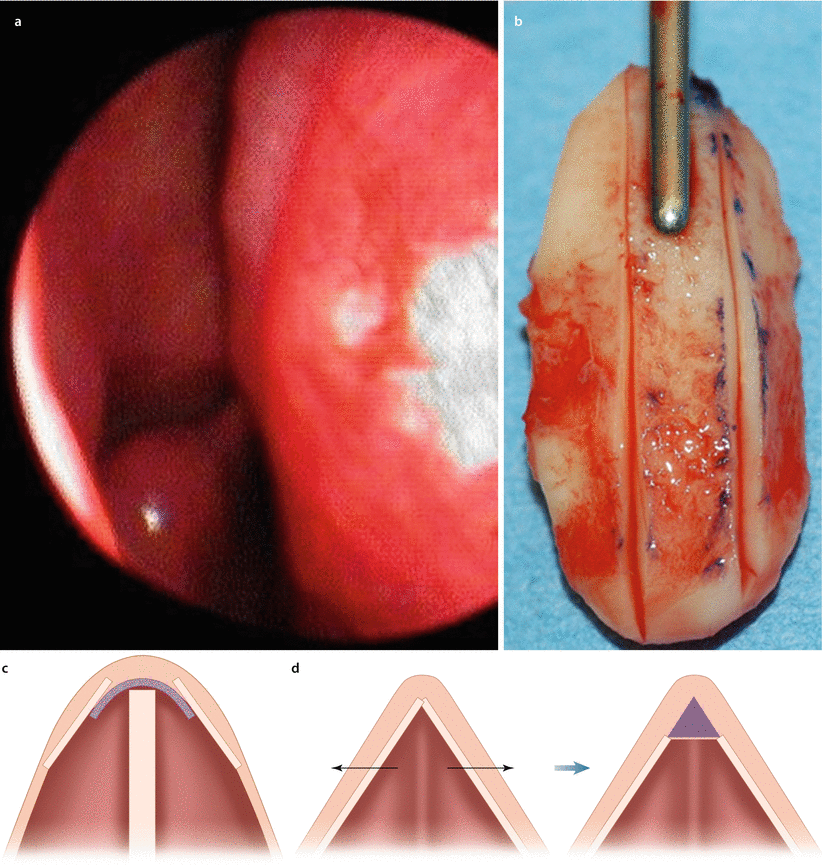
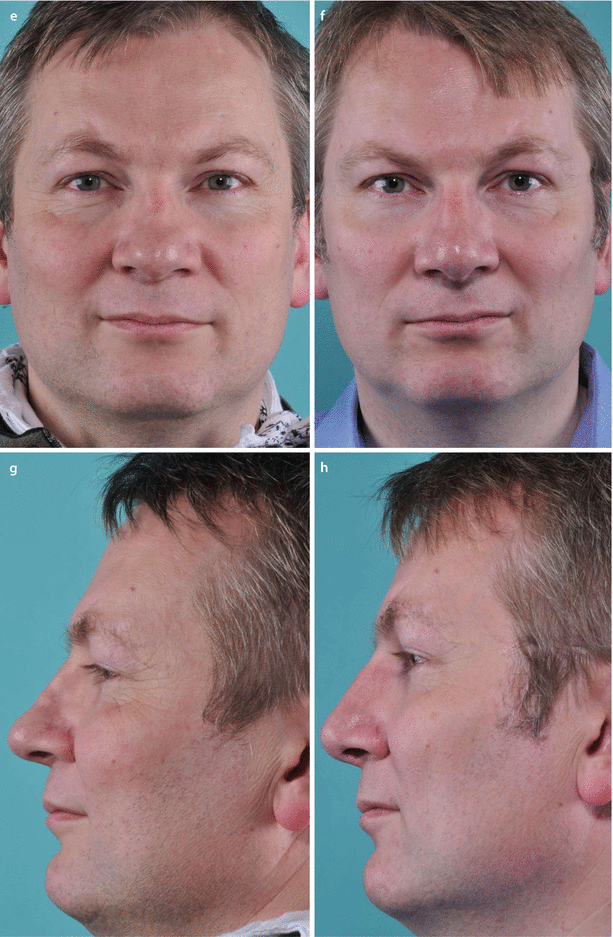
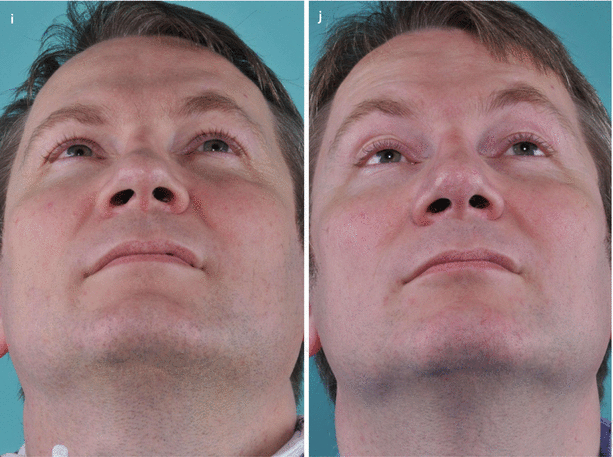
Fig. 4.3
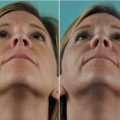
(a) Narrow upper airway on endoscopic view, (b) butterfly-type spreader graft, and (c) schematic showing graft placement beneath the dorsal side walls. (d) Schematic representation of bony out-fracture for airway enhancement followed by dorsal augmentation to maintain a slender frontal contour. (e) Prerevision frontal view demonstrating an asymmetrical and pinched bony and middle nasal vault and (f) postrevision frontal view. (g) Prerevision profile view and (h) postrevision profile view. (i) Prerevision base view and (j) postrevision base view
4.3.4 Case 4: Bony Out-Fracture
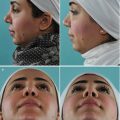
A 20-year-old male with a history of blunt nasal trauma at age 13 presented for primary rhinoplasty consultation. External examination (Fig. 4.4a) suggested a probable prior septal hematoma with loss of septal projection, but the endonasal examination showed only an intact quadrangular septum with a high leftward deviation and a minor deviation at the inferior aspect of the caudal septum. The left nasal bone was depressed, but rhinomanometry was normal. Ultimately the patient disagreed with the diagnostic assessment and was treated elsewhere.
Four months after initial presentation, the patient returned complaining of an unsatisfactory rhinoplasty outcome and development of severe breathing impairment. Examination revealed an overresected and pinched bony vault with persistent depression of the left nasal bone (Fig. 4.4b). A polly-beak profile deformity was also observed, and the endonasal examination revealed narrow internal nasal valves and narrow nasal cavities. Spreader graft simulation using a small glass spatula to widen the upper nasal valve resulted in significant breathing improvement, thereby convincing the patient to undergo widening of the lower nasal side walls. Repeat rhinomanometry showed (150 Pa): R 80 mL/s, L 416 mL/s.
Revision surgery was delayed until 1 year following primary rhinoplasty. Treatment recommendations included widening the cartilaginous and bony vaults with bony out-fracture if necessary and dorsal profile realignment by lowering the anterior septal polly-beak and augmenting the remaining dorsum.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree