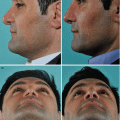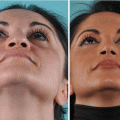
Fig. 3.1
Patient with valvular collapse (a) at rest; (b) mildly forced inspiration; and (c) Cottle maneuver. Endoscopic view of left nostril and internal valve area (d) at rest; and (e) collapsing under forced inspiration. Endoscopic view of the spreader graft test: (f) narrow inner valve at rest, (g) opening the valve with a glass stick (spreader graft test), and (h) glass sticks for endonasal examination (originally ophthalmologic device). Endoscopic view of lateral alar support test (i) at rest; (j) support with glass stick at the lateral aspect of the inner valve, here at the area of the LLC recurvature
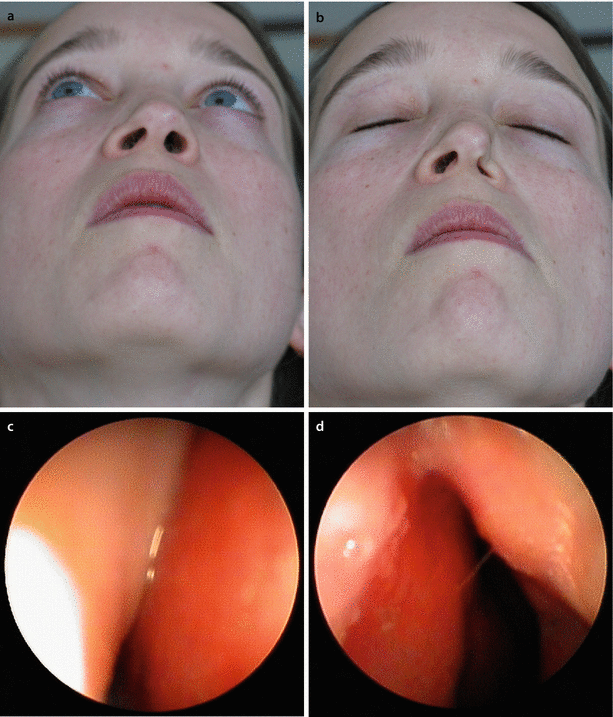
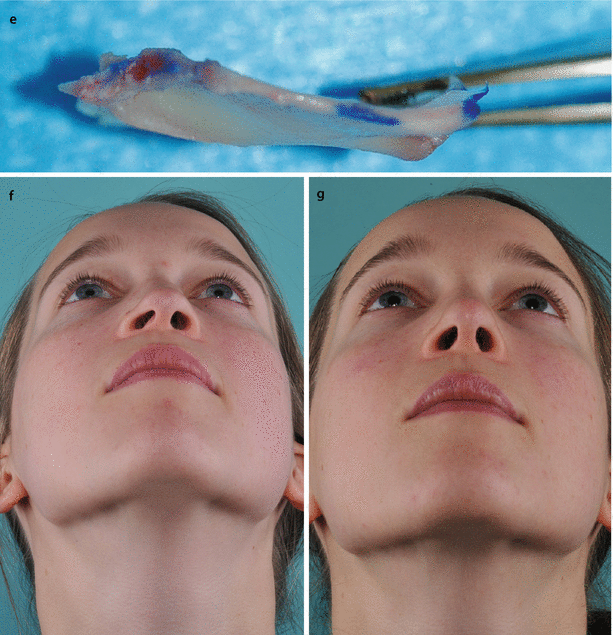
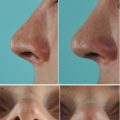
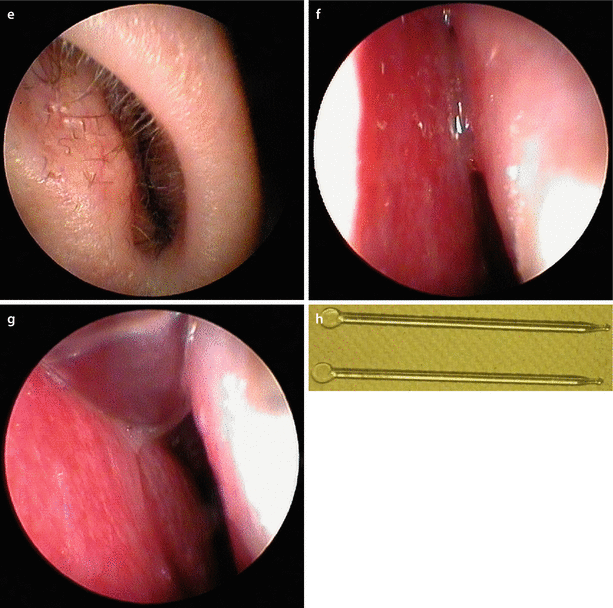
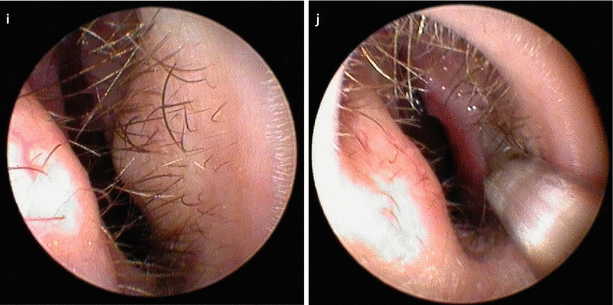
Fig. 3.2
Left-sided alar collapse caused by right-sided airway obstruction from septal deviation, (a) at rest and (b) under gentle forced inspiration. Endonasal view of (c) right and (d) left of internal valve. (e) Completely harvested septum. Note narrowing of the right nasal valve from septal impingement. Septal deviation corrected by extracorporeal septoplasty and replantation. Base view (f) preoperative and (g) postoperative
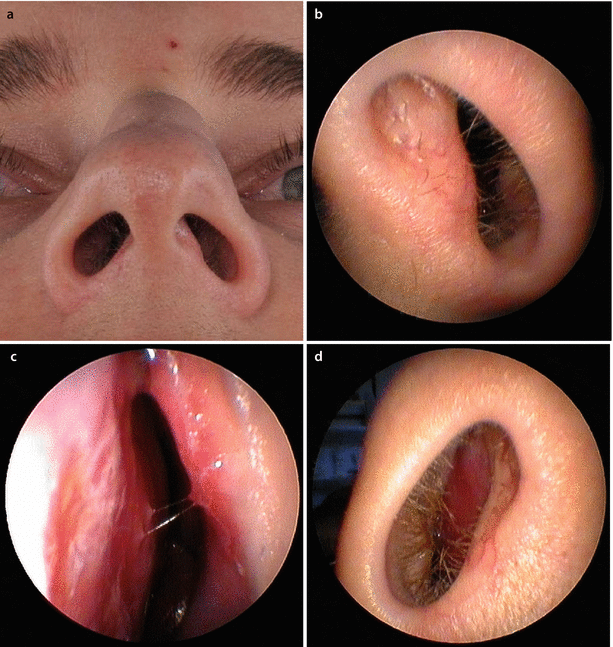
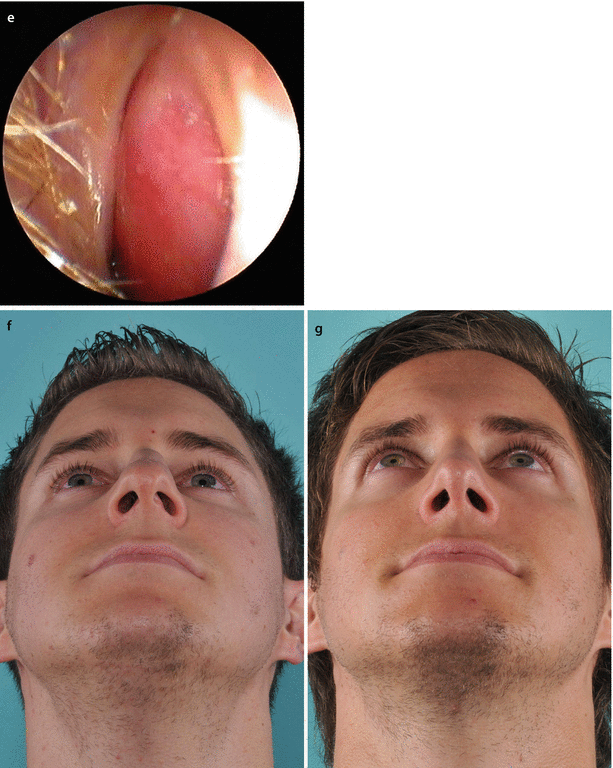
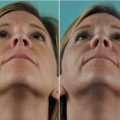
Fig. 3.3
Example of obstruction on the side opposite the narrow external valve. (a) Base view; (b) endoscopic view of left nostril; (c) internal nasal valve area. Subluxation of the anterior septal border into the left vestibule is not the reason for the patient’s breathing impairment, which is located at the right side. Examination of the patient’s contralateral (right) airway revealed severe septal deviation obstructing the right internal nasal valve area. (d) Endoscopic view of right nostril, and (e) internal nasal valve subtotally obstructed. Endonasal septoplasty, osteotomies for axial realignment, and spreader flap technique for cartilaginous vault reconstruction result in normal airflow bilaterally upon reexamination. (f) Preoperative and (g) postoperative base view
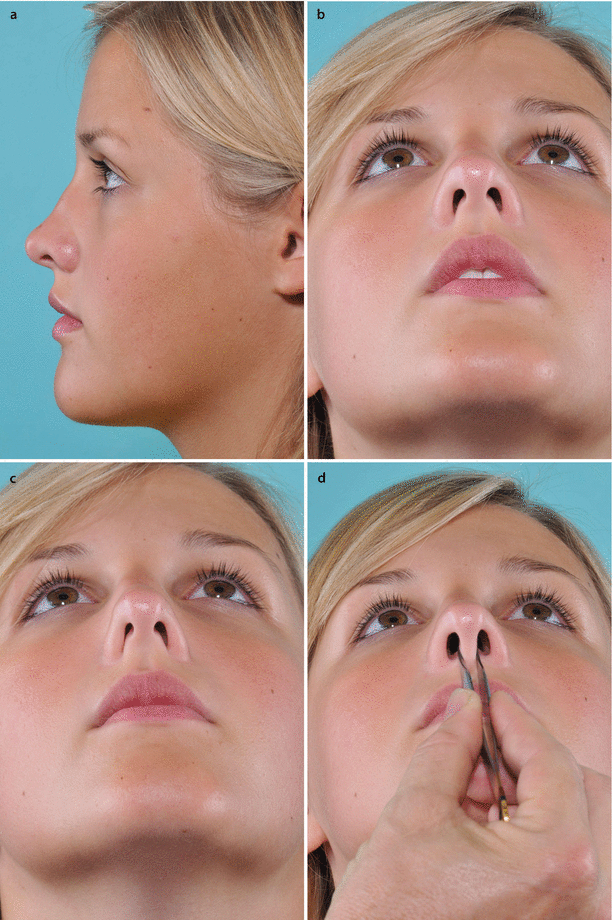
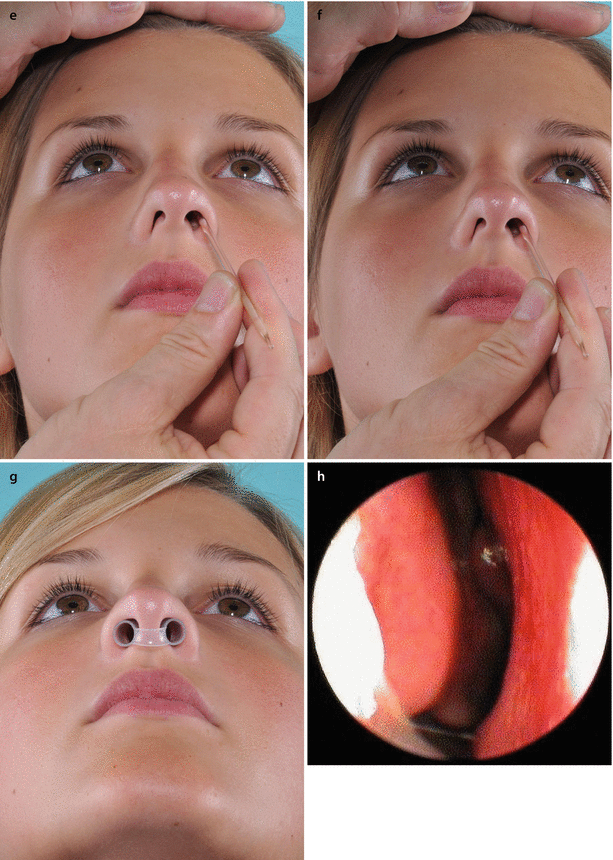
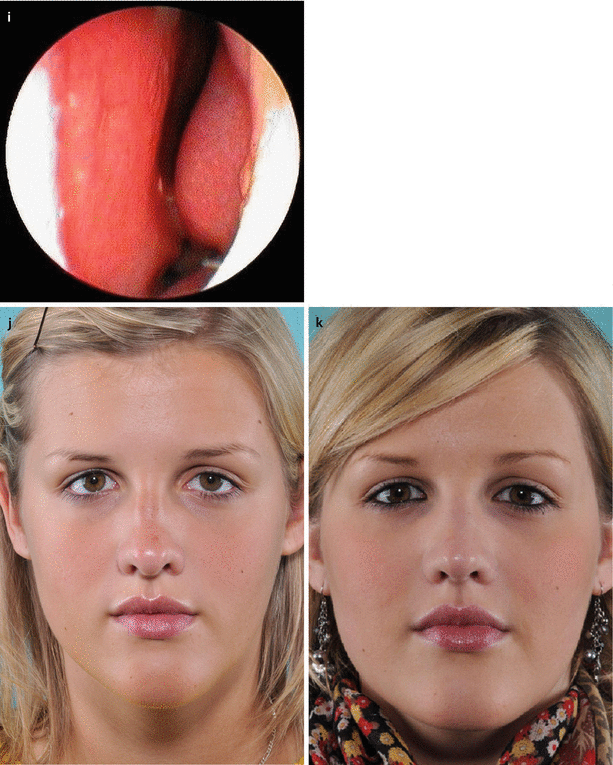
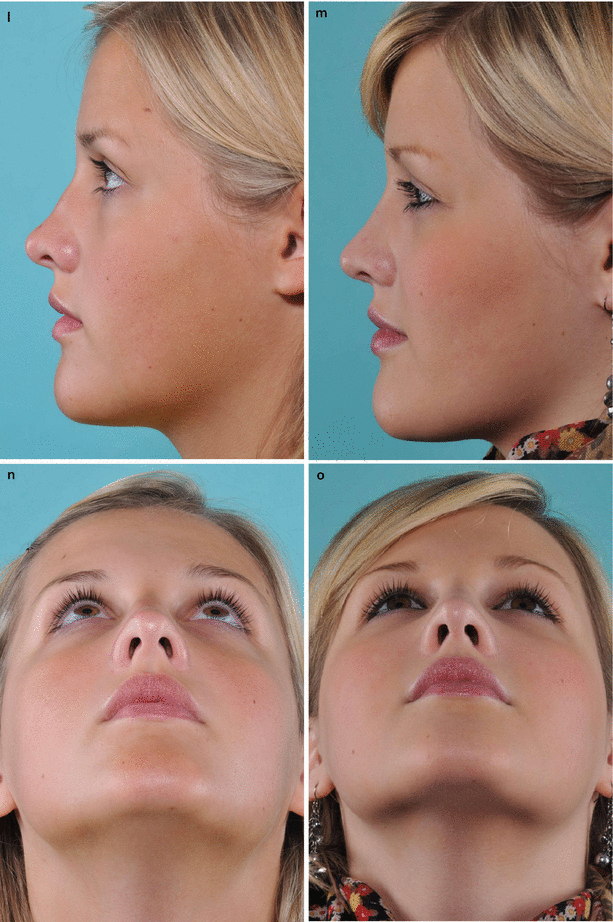
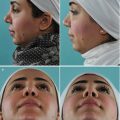
Fig. 3.4
Examination of the influence of columellar width on the airflow. (a) Left profile; (b) base view at rest, and (c) under forced inspiration. (d) Columella pinch test revealed the influence of columellar width and nostril cross section on the airflow. Examination of the influence of increasing nostril cross section by alar support on the left side—the right nostril still collapsed as a deeper left side obstruction was not corrected by this maneuver. (e) At rest, and (f) under gentle forced inspiration. (g) Long-term test with a pair of silicone tubes to assess the functional importance of the subsequent anatomic airway structures downstream in the nostrils (external nasal valves). Endoscopic view (h) of a patent right airway, and (i) left-sided airway obstruction from septal deviation. The turbinates appeared normal in size at the time of examination. Frontal view (j) preoperatively and (k) postoperatively. Profile view (l) preoperatively and (m) postoperatively. Base view (n) preoperatively and (o) postoperatively
3.2 Surgical Principles
3.2.1 Septoplasty
Eliminating septal deformities is a critical aspect of both functional and cosmetic nasal surgery, and in many noses both simultaneous functional and cosmetic enhancement is required. Preoperative evaluation of the entire septal partition, from the caudal and dorsal margins to the posterior bony segment, is a prerequisite for accurate diagnosis and effective surgical management.
The functional and cosmetic importance of the anterior septum is increasingly recognized in contemporary nasal surgery. However, surgical correction of anterior septal deformities is among the most difficult tasks in both functional and cosmetic rhinoplasty. Moreover, the importance of septal support cannot be underemphasized, since it is pivotal to the support, symmetry, and patency of the cartilaginous nasal framework. Minor septal deviations in the area of the internal nasal valve—which is the natural isthmus of the nasal airway—may also have a disproportionately negative impact on nasal airflow and may be exacerbated by anatomic abnormalities and structural deficiencies of the adjacent alae and nasal side walls. Moreover, traditional techniques used to straighten a deformed anterior septum are often doomed to failure, since scoring, curfing, and morselizing may compromise long-term structural support and lead to progressive skeletal distortion as the nose gradually seeks a new structural equilibrium. And while contemporary rhinoplasty techniques can be used to both strengthen and reshape the cartilaginous nasal framework to produce a well-functioning and attractive nose, overaggressive reduction rhinoplasty will severely impair nasal airway function and should be avoided. The following sections address functional aspects of individual skeletal elements impacted by cosmetic nasal surgery.
3.2.2 Spreader Grafts and Upper Lateral Cartilage (ULC) Suture Techniques
Reduction of the typical dorsal hump for profile enhancement obligates the surgeon to consider reconstruction of the nasal dorsum in order to prevent both functional and cosmetic complications caused by surgical destabilization. Preventing “pinched” upper lateral cartilages (Fig. 3.5c) is a fundamental goal of hump reduction, and in our hands spreader grafts, suture techniques, and/or a combined approach was the preferred means of middle vault reconstruction after hump reduction (Fig. 3.5d–f) before the spreader flap era. Conventional spreader graft techniques are now familiar to most nasal surgeons. After obtaining satisfactory graft material from the cartilaginous hump resection and/or from cartilage harvest of the posterior quadrangular cartilage, spreader graft thickness is carefully adjusted to preserve middle vault width, thereby preventing an inverted-V deformity while simultaneously avoiding excessive middle vault width from overcorrection. Spreader grafts are first sutured flush with the newly created cartilaginous dorsum to form a three-layered reconstruction (7 see Fig. 3.5d). The upper lateral cartilages are then sutured to the construct in a symmetrical fashion (7 see Fig. 3.5f). This is accomplished by temporarily displacing the tip cartilages caudally and then applying equal tension to the ULCs so they are held symmetrically while being reattached.
In some patients, thin nasal skin and a large open roof resulting from bony hump reduction necessitate extending the spreader grafts cephalically to avoid bony side wall collapse with lateral osteotomies. Prophylaxis of bony vault collapse will often prevent both functional and cosmetic deformities of the upper nasal vault. A large clinical experience with revision rhinoplasty also attests to the benefits of prophylactic spreader grafts.
In patients with weak cartilaginous side walls, a personal modification of the spreader graft technique is sometimes preferable. Using the modified technique, the upper lateral cartilages are sutured to the top of the dorsal septum rather than to its sides (Figs. 3.6b and 3.7c). This minor change in cartilage placement improves side wall support in noses with weak upper lateral cartilage and functions much like a ULC flaring suture. However, we feel that this technique provides better long-term support in our hands when compared to flaring sutures. In order to prevent overprojection of the dorsum, the spreader grafts must also be recessed slightly below the dorsal line so that the ULC remains flush with the newly established profile line (Figs. 3.6 and 3.7). Suture techniques can also be used in the absence of spreader grafts by lowering the septum approximately 1 mm to compensate for the ULC width (7 see Fig. 3.5e). However, care must be taken to adjust the profile line precisely to prevent polly-beak deformity. When functional considerations prevent adequate lowering of the cartilaginous dorsum in order to prevent a polly-beak type deformity, onlay grafts of cartilage or fascia must be used to augment the adjacent bony vault and create an aesthetically pleasing dorsal profile. Spreader graft and suture techniques are equally effective for both primary and revision cases.
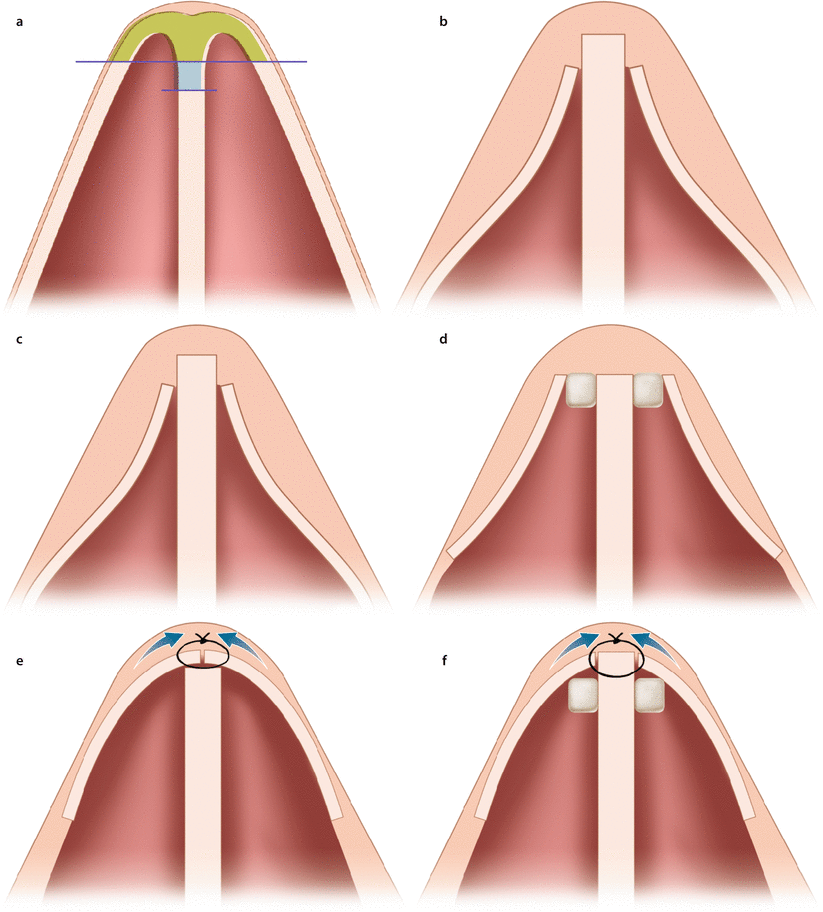
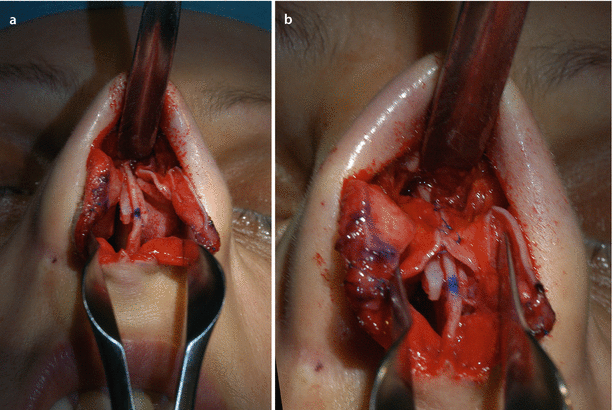
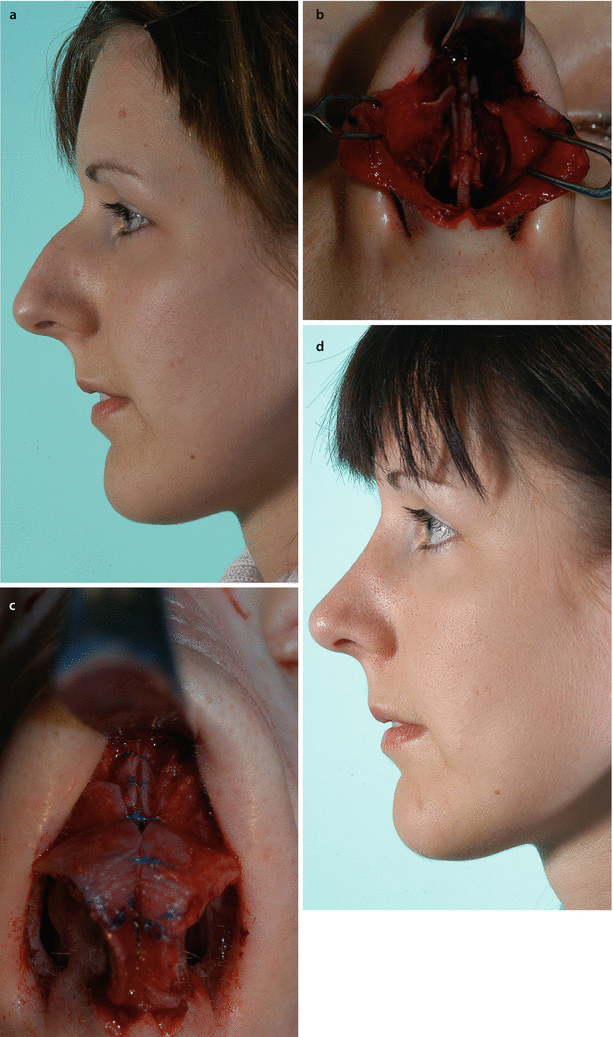
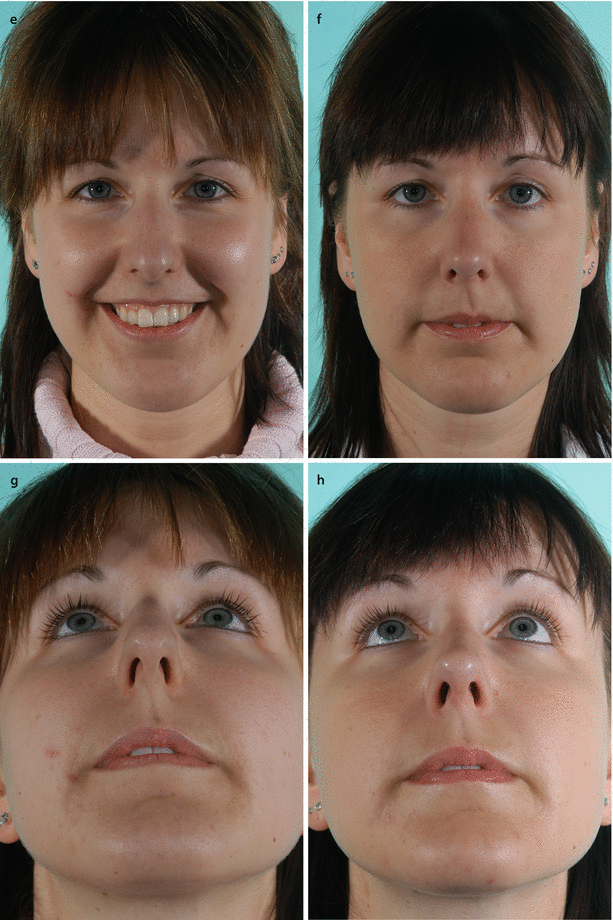

Fig. 3.5
Schematic drawings of classic reduction rhinoplasty technique: (a) monoblock hump reduction and additional septal reduction for dorsal alignment; (b) without cartilaginous vault reconstruction, early situation; (c) not rarely later side wall collapse occurs. Some alternatives to Hump reduction with cartilaginous vault reconstruction: (d) spreader grafts, (e) suture techniques, (f) combination of spreader grafts and suture techniques

Fig. 3.6
Intraoperative examples of (a) spreader grafts and (b) additional ULC suture suspension for vault reconstruction on top of the dorsal septal rim widened with spreader graft


Fig. 3.7
A patient for primary reduction rhinoplasty surgically managed with a similar technique to that shown in Fig. 3.6. (a) Profile view preoperatively; (b) spreader grafts in place 1 mm lower than the dorsal septal border; (c) ULCs sutured at the septum over the spreader grafts. The septum had to be lowered adequately to avoid a parrot-beak formation. (d) Profile view 8 months postoperatively. Frontal view (e) preoperatively and (f) 8 months postoperatively. Note: despite the applied technique of cartilaginous vault reconstruction, the dorsum is not overly widened. Base view (g) preoperatively and (h) postoperatively
3.2.3 Spreader Flaps and Anatomic Details of the Nasal Dorsum
In primary hump reduction, spreader flaps are becoming an increasingly popular means of reconstituting middle vault support, particularly since they don’t require additional cartilage for reconstruction. However, not all noses are well suited to spreader flaps. Noses with long nasal bones and/or overly short ULCs are poor candidates for spreader flap reconstruction, since invagination of the ULCs is often impossible. Conversely, some ultra-long and narrow middle vaults have cartilage that is too thin or soft to use as spreader flaps. Various other anatomic variations must also be considered. Of primary importance is the extension of the ULC beneath the nasal bones, since the overlap between cartilage and bone varies widely in length, width, and strength. Long extensions of the ULC can fill an open roof deformity created by nasal hump reduction—the ideal configuration—whereas in other cases there may be little if any cartilage to conceal an open roof deformity. Nasal bones also show distinctive features in the bony cartilaginous transition zone of the dorsum. These are displayed by separating the bone from the ULCs in a previous case of composite (en bloc) hump reduction (Fig. 3.8).
Important anatomic variations exist in the distance between the central bony extension and the lateral bony extensions as well as in their length and symmetry. One of the most important variables is the height of the lateral bony extensions. In some noses the lateral extensions are equal in height to the dorsum, while in others the lateral extensions may be considerably lower. These skeletal variations are critical considerations in extracorporeal septoplasty because they determine fixation techniques. In noses with high lateral bony extensions, bones perforated with drill holes can be used for secure suture fixation of the reimplanted septal construct, whereas in the underprojected caudal nasal bones, extreme care must be taken not to disrupt the bony cartilaginous interface because the ULCs must be used for suture fixation. And while underprojected lateral extensions are not amenable to drill hole fixation, they are usually well suited to the application of spreader flaps.
To create spreader flaps, the ULCs must be released from the undersurface of the bony hump with blunt dissection. Once the ULCs have been divided from the dorsal septum (Fig. 3.9a), we initiate the dissection by scoring the caudal margin of the bony hump with a no. 15 blade (Fig. 3.9b) and then continue the dissection using either a semisharp (Haraldsson) suction dissector or some type of periosteal elevator such as a Freer, McKenty, or Cottle elevator. Care must be taken not to dissect below the desired profile line so that the remaining ULC/nasal bone attachments are preserved. Next, the cartilaginous dorsal hump is sharply resected (Fig. 3.9c), and submucosal pockets are developed on both sides of the dorsal septum to accommodate the spreader flaps. When necessary, such as with large cartilaginous humps, the ULCs are trimmed to avoid excessive bulk within the internal nasal valves (Fig. 3.9d, e). Finally, the ULCs are folded into the submucosal pockets and temporarily secured with small-bore needles (Fig. 3.9f). With the ULCs safely repositioned just below the desired profile line, elimination of the bony hump can proceed. We prefer to resect the bony hump using a thin and ultrasharp chisel (Fig. 3.9g) and to fine-tune the bony contour with a carbide rasp. Hump refinement with a carbide rasp is preferred because it removes bone effectively with little or no trauma to the underlying cartilage extensions.
Once hump reduction is complete, spreader flaps are secured with slowly resorbing 5-0 monofilament sutures (Fig. 3.9h, i). By using resorbable suture material, complications stemming from permanent suture material penetrating the nasal cavity are minimized, and extensive elevation of mucosa from the ULCs becomes unnecessary. It is also important to remember that while suturing the spreader flaps, they should be kept under constant symmetrical downward tension using a double-skin hook. Care must also be taken to ensure correct sagittal alignment, and in cases of pre-existing deformity, slight overcorrection of septal alignment is often needed to overcome intrinsic tissue memory. In addition to septal alignment, suture fixation can also be used to control dorsal width. Cranially, suture fixation can be used to control the width of the bony cartilaginous junction and reduce bony flaring. When bony drill holes are available, a cerclage suture can be used to aggressively narrow the bony cartilaginous junction and/or close a persistent open roof deformity. Excess middle vault width stemming from overly rigid ULCs can also be treated by perforating, scoring, or incising the spreader flaps for increased narrowing. Depending upon the site of cartilage modification, narrowing can be limited to the upper, central, or lower middle vault or combinations thereof. Furthermore, the kind of suture technique can be altered in weak cartilages (Fig. 3.9j, k).
In summary, spreader flaps are an effective technique for creating a natural-appearing nasal dorsum with attractive dorsal aesthetic lines in most noses. Spreader flaps are also easily fine-tuned using suture techniques, and they frequently obviate the need for spreader graft harvest. In our hands, the need for camouflage (fascia) grafts has also greatly diminished with the advent of spreader flaps. Unfortunately, intraoperative adjustments to middle vault projection require redoing flap fixation—a significant limitation of this otherwise user-friendly technique. Likewise, noses with ultra-pliable ULCs make poor candidates for spreader flap reconstruction since cosmetic and functional deformities may result.
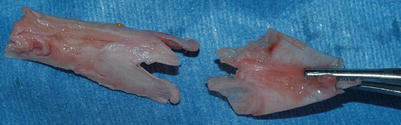
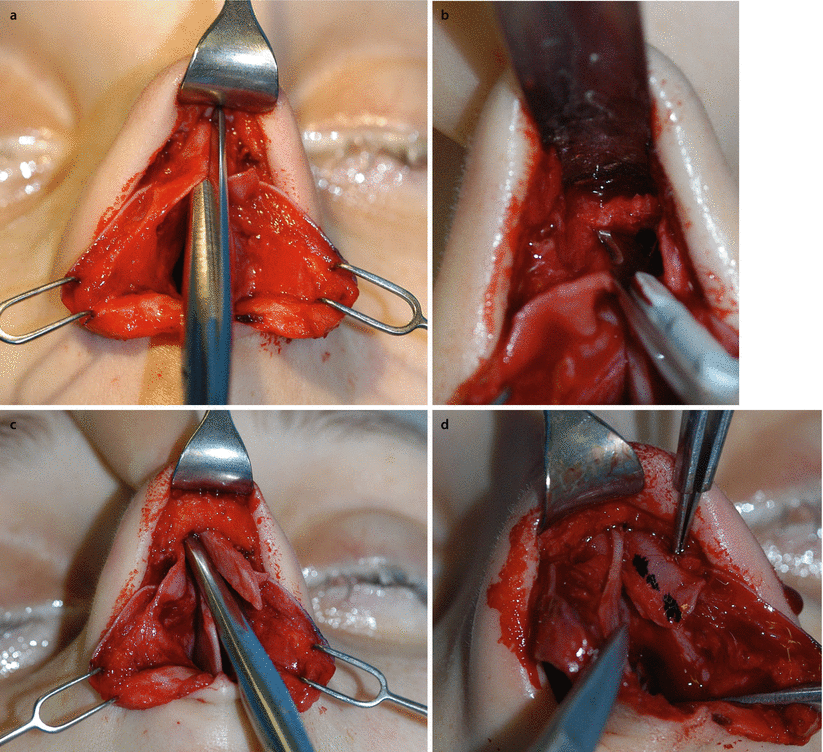
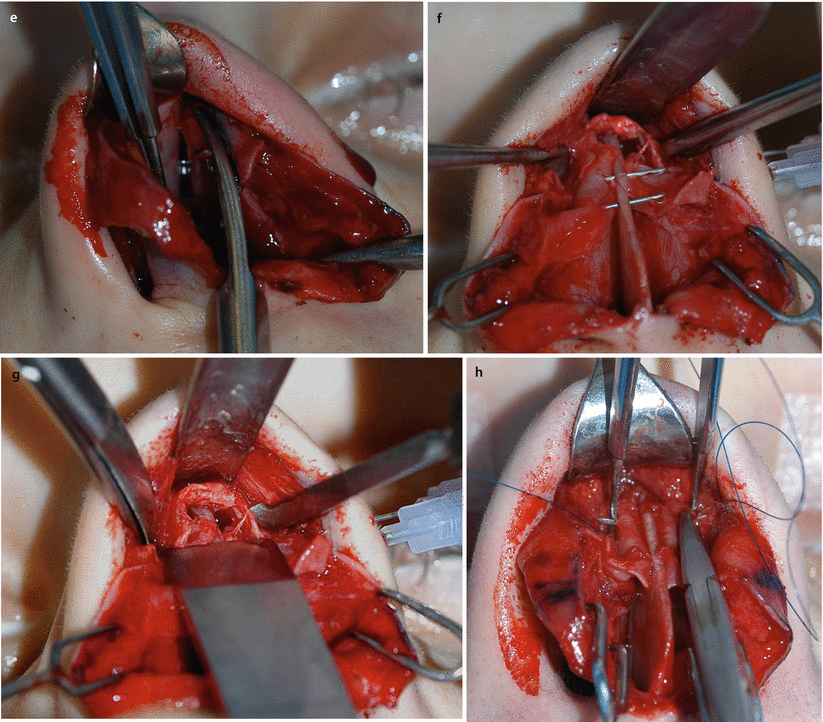
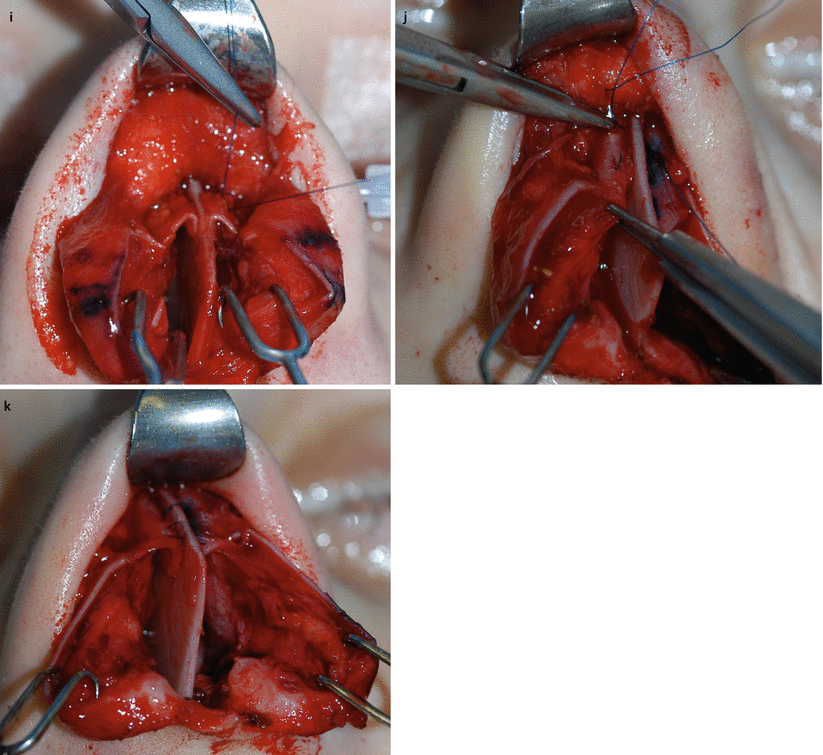

Fig. 3.8
Anatomy: dissection of the hump resected as a monobloc of bone and cartilage. Note the shape of bone and cartilage; the bone originally overlapped the cartilage



Fig. 3.9
Spreader flap technique. (a) ULC separation off the septum, and (b) from underneath the bony vault. (c) Reduction of the septal component of the cartilaginous hump. (d) Marking and (e) resection of the surplus of ULC to avoid partial upper airway obstruction. (f) Intermediate infolding of the ULCs for better access to (g) bony hump reduction with an extremely sharp chisel for the major part of the hump (and a rasp for residual adjustment, not shown). Spreader flap suturing with 5.0 PDS (h) horizontal mattress sutures, and (i) adjusting dorsal width by the degree of tension. Incisions or scoring on the apex of the vault is an option in very rigid cartilage or in the distal third of the dorsum (valve area). Spreader flap suturing with 5.0 PDS. (j) Alternatively, in very weak cartilage vertically double U-shaped sutures can be applied and (k) knotted over the septum provided that the dorsal height must not be further reduced
3.2.4 Batten Grafts or Lateral Crural Strut Grafts
Batten grafts are used mostly in revision rhinoplasty. They are indicated to strengthen lateral crura weakened by cephalic trimming and/or to strengthen collapsed (concave) lateral crura. Battens can be placed in pockets either superficial to the LLC (over the batten graft) or deep to the LLC (under the batten graft), or they can be sutured directly to the exposed overlying LLC (lateral crural strut graft). By adding rigidity to the lateral crura, batten grafts stabilize the lower nasal side wall against premature inspiratory collapse. Batten grafts are also especially useful in boxy tip correction (Fig. 3.10) to prevent exacerbating lateral crural recurvature deformity caused by tip sutures.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree