(1)
Klinik für Plastische Gesichtschirurgie, Marienhospital Stuttgart, Stuttgart, Germany
Electronic supplementary material
The online version of this chapter (doi:10.1007/978-3-662-49706-7_6) contains supplementary material, which is available to authorized users.
Keywords
Dorsal irregularitiesOverresected dorsumSaddle nosePolly-beak deformityHump residualConchal graftRib graftFree diced cartilageFDCSupratip excision6.1 Surgical Principles
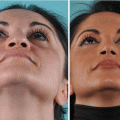
The most common cosmetic profile deformity in secondary rhinoplasty is irregularity of the nasal dorsum. Dorsal irregularities can be minor or major and can arise from overresection, underresection, or insufficient skeletal camouflage. In the overresected dorsum, restoration requires replacement grafting similar to treatment of a saddle-nose deformity. Conversely, the underresected dorsum merely needs removal of the overprojected segment, and in minor cases this may be accomplished with a sharp rasp or power drill (Fig. 6.1).
Another common postsurgical dorsal irregularity is the polly-beak deformity. In this deformity, the cartilaginous dorsum represents the highest point in the nasal profile, and there are a wide variety of underlying causes for this kind of deformity. According to Foda, postoperative tip droop is the most common cause of the polly-beak deformity, but the deformity may also arise from overresection of the bony dorsum, underresection of the cartilaginous dorsum, or scar-mediated thickening of the supratip skin where the soft tissues are comparatively thick. Postoperative tip droop occurs more often with the closed rhinoplasty approach, because many surgeons fail to adequately compensate for the fact that ligamentous soft-tissue support mechanisms are disrupted during exposure of the tip cartilages. Various techniques can be used to reconstitute disrupted tip support, including columellar strut graft placement, the tongue-in-groove technique, or the application of tip suspension sutures.
Another cause of compromised tip support and loss of tip projection is overresection. Similarly, overresection of the lower lateral cartilages (LLCs) may also reduce tip support, and this commonly results from misguided attempts to create a more delicate tip using only extended cartilage resection. In addition to loss of tip support, overresection of the LLCs can also produce unsightly deformities of the ala and nasal tip. Combined overresection of the LLCs and anterior septum can also result in a multifaceted deformity of even greater magnitude.
6.2 Treatment of the Undersupported Nasal Tip
Treatment of the poorly supported nasal tip depends upon identifying and eliminating the underlying root cause. Therefore, a careful surgical analysis is paramount, and removal of overlying scar tissue is necessary before the true etiology of tip droop can be correctly identified. In summary, postsurgical tip droop may result from a variety of causes, including inadequate ligamentous support, weak medial crura, overresection of the caudal septum, and/or overresection of the LLCs. Frequently postsurgical tip droop is also produced by more than one cause.
In the case of inadequate ligamentous support to the medial crura, a columellar strut graft can be highly effective at restoring lost tip support and projection. Donor graft material is preferentially harvested from the septum, since it is well suited to strut grafting and easy to harvest (Fig. 6.2). Although a large portion of the quadrangular septum may have already been removed in secondary cases, frequently the long cartilaginous “tail” of the quadrangular septum may still be available for graft harvest. We have found that this portion of the quadrangular cartilage makes an ideal columellar strut graft. However, if surplus septal cartilage is unavailable, cartilage from the concha cymba can be used for creation of a “sandwich”-type columellar strut graft (Fig. 6.3). The advantage of the conchal graft is derived from suturing two reciprocally curved opposed segments together to create a single, straight, and stable strut graft that will resist warping over time. Usually the concha cymba provides adequate graft length and can be harvested from the anterior approach to include the posterior perichondrium. The cartilage can be divided along its long axis (while keeping the perichondrium intact) and folded upon itself. A modified Aiach clamp is then used to immobilize the bivalved cartilage halves during suture fixation to create the double-layered conchal sandwich (Fig. 6.4). If a longer graft is necessary, it can be created by harvesting larger portions of the conchal bowl or by suturing both conchae together (Fig. 6.5). When necessary, rib cartilage can also be used for columellar strut grafting. However, in the past we rarely used rib grafts, not only because of the risk of warping but also because suture fixation with transseptal mattress sutures often leads to infection, which can be avoided when using auricular grafts. The differences in susceptibility to infection may be explained by the presence of intact perichondrium, which is absent from carved rib grafts. These days, we use more and more rib grafts after developing instruments for easier harvesting (Rollin Daniel at Medicon), using the ninth or tenth rib instead of the sixth rib, which is quicker to dissect and yields more firm cartilage in revision cases in which septal and conchal cartilage have already been used. Further, our actual concept includes a final touch-up with paste-like free diced cartilage (FDC).
Inadequate tip support and nasal tip ptosis can also result from overly weak medial crura. When tip ptosis occurs in the presence of an overly long septum, the tongue-in-groove technique can be used to suspend the weak medial crura and correct the drooping nasal tip (Fig. 6.6). By suturing the medial crura to the anterior edge of the overprotruding caudal septum, the tongue-in-groove technique restores tip projection, rotation, and support while simultaneously reducing excessive columellar protrusion.
In secondary cases, tip ptosis often results from previous overresection of the lower lateral cartilages. Treatment of overresected tip cartilage inevitably involves cartilage augmentation grafting, and various options are available for reconstruction. In general, we prefer using septal cartilage because of its favorable biomechanical characteristics, but rib or conchal cartilage can also be used when surplus septal cartilage is unavailable. Preoperative planning is essential to maximize utilization of limited septal graft material, especially when multiple grafts are needed (7 see Fig. 6.2), and the maximum amount of cartilage is harvested as a single piece to permit the greatest flexibility in treatment planning. When available, residual septal cartilage remnants should be placed back into the septum to minimize unwanted movement of the donor site mucosa. In cases in which donor septal cartilage has been depleted, our next choice is rib cartilage graft material harvested from the 9th, 10th, or 11th rib through a small horizontal incision. Despite the donor site morbidity associated with rib graft harvest, we prefer rib cartilage over conchal cartilage because it is easily sculpted with a motor-driven fraise to produce thin and delicate lower lateral cartilage replacement grafts.
Regardless of the donor source, long, thin, and flexible cartilage strips are needed to repair damaged or missing segments of the overresected LLCs, and we employ various techniques, depending on the status of the residual framework. In every case we first assemble the reconstructed framework with small needles before securing the grafts with 6-0 nylon sutures.
Previously we used nylon sutures for permanent fixation of all tissue grafts. However, we occasionally observed minor suture abscess formation probably caused by foreign-body reaction of the nonresorbable suture material. For that reason, we have since switched to resorbable 5-0 or 6-0 polydioxanone (PDS) suture material and have subsequently noticed a significant reduction in the incidence of suture abscess formation, although without apparent change in graft stability.
In thin-skinned patients, we cover the reconstructed domes with onlay grafts of fascia or soft tissue to prevent visible contour irregularities (7 see Fig. 6.13). When the residual LLC framework is missing large portions of both the lateral and intermediate crura, we employ a graft bending technique (Fig. 6.7) in which the entire lateral crus, dome unit, and intermediate crus are simultaneously reconstructed using a single anatomically shaped replacement graft. To achieve adequate bending at the nasal dome, autologous septal or rib cartilage must be carefully thinned at the tip-defining point using a cylinder-shaped, motorized diamond fraise (Fig. 6.8). Although thinning can also be performed with a scalpel, it is difficult to achieve the uniform and precise thinning required to prevent fracture of the graft. In cases where adequate bending cannot be achieved with thinning alone, we use a scoring technique in which the domes are also carefully scored to attain additional flexibility (Fig. 6.9). However, in some cases, such as partially calcified rib cartilage, the graft material is overly brittle, and through-and-through fractures of the tip-defining point cannot be avoided. In this situation, the fractured graft resembles a vertically divided alar cartilage in which the lateral and intermediate crura are divided at the tip-defining point. When such fractures occur, we employ a dome division technique in which the opposite dome is divided for symmetry, and the graft edges are reapproximated with horizontal mattress sutures (Fig. 6.10). Alternatively, if a thick columellar strut graft is available, we use a split graft technique in which a sagittal split is created in the distal end of the strut to permit simultaneous reconstruction of the columella and infratip with only a single strut graft (Fig. 6.11). Finally, when tissue replacement is confined to the lateral crus, we use a batten graft technique to reconstruct deformed or missing segments of the lateral crus (Fig. 6.12). Alternatively, when the crus is severely deformed or absent, we prefer lateral crural strut grafts, which extend farther laterally than batten grafts to better restore support and contour to the alae. Only when the patient refuses the use of rib cartilage do we resort to conchal cartilage. Our experience indicates that conchal cartilage is the least desirable graft material owing to its predetermined shape, which is often difficult to modify with sutures or other techniques described earlier. After reconstruction of the cartilaginous tip framework, we may cover the cartilage with soft-tissue grafts for camouflaging (Fig. 6.13), but this technique has been mostly replaced recently by using free diced cartilage (FDC).
In all cases of nasal tip reconstruction, it is essential to reunite the newly reconstructed framework with the cartilaginous dorsum using long-lasting but resorbable suture material such as PDS fixation sutures. Two main types of suspension suture are used for this purpose: a combination of spanning and suspension suture (Fig. 6.14) and a simple sling-type suspension suture (Figs. 6.15 and 6.16). Although elimination of lateral crural flaring and tip suspension are accomplished simultaneously with the combination suture, this technique is contraindicated in weak cartilage, since an unsightly concave lateral crural deformity usually results. However, when the reconstructed crural cartilages have adequate rigidity, as they most often do following skeletal reconstruction, the combination suture technique is preferred. Placement of the combination suture is a two-step process in which the suture first is passed through both lateral crura in the manner of a standard (bilateral) spanning suture to eliminate crural flaring and then is knotted to prevent further crural movement. The suture is then passed through the dorsal septum, tightened until the desired degree of tip suspension is established, and then knotted a second time to complete the suspension (7 see Fig. 6.14).
When the lateral crura do not require suture modification, a simple (buried) suspension suture is preferred. However, unlike the combination suture, which uses both lateral crura as suspension points, the simple suture uses only the columella for suspension. To prevent exposure of the nonabsorbable suture material, the stitch must be buried beneath the overlying vestibular skin and the medial crura using a cannulation technique. In the first step, a permanent suture is sewn to the caudal septum at the designated upper suspension point. Next, a second suspension point is selected along the infratip lobule that is oriented to produce the desired profile configuration. A small hollow-bore needle is then inserted at the columellar suspension point and passed between the vestibular skin and medial crus to the designated fixation point on the dorsal septum. One end of the suspension suture is then threaded retrograde through the needle until it emerges from the opposite end. The needle is then removed and reinserted at the equivalent point on the opposite side of the columella to permit antegrade passage of the suture back to the septal fixation point, where it is knotted and tied. In this manner, the knot is buried internally within the membranous septal pocket, where it is neither visible nor palpable. We refer to this configuration as a simple suspension suture with posterior sling (7 see Fig. 6.15). Alternatively, both ends of the suspension suture can be passed anteriorly and tied over the columella—the so-called tip suspension suture with an anterior sling. Although this placement is easier, knot placement may result in a visible and/or palpable irregularity of the columella in thin-skinned patients (7 see Fig. 6.16). The advantage of this type of suspension suture is the exact positioning of the tip after flipping back the flap.
When revising the overresected nasal tip, skin thickness often becomes an important factor in treatment planning. In dealing with the thick-skinned nose, it is generally preferable to enlarge the skeletal framework as much as cosmetic tolerance will allow, thereby stretching the overlying soft-tissue envelope and maximizing tip definition. However, aggressive skin stretching is sometimes contraindicated because it occasionally results in an unacceptably large nose. On the other hand, attempting to create a smaller skeletal framework often results in soft-tissue polly-beak formation, since the supratip skin may fail to contract and give rise to dead space, excessive subcutaneous fibrosis, and unwanted skin thickening. In this uncommon scenario, a direct vertically oriented fusiform excision of the supratip skin can be used to eliminate the polly-beak deformity by excising the scarred skin and reducing the overall skin volume, what we call a “supratip excision” (Fig. 6.17). To prevent conspicuous scar formation, closure is accomplished only with subcutaneous sutures, and in our series of 36 patients, only three developed significant scarring.
Unsuccessful treatment of a nasal hump deformity can result in either overresection or underresection of the nasal dorsum. In the overresected dorsum, treatment requires augmentation to restore lost height. Options for dorsal augmentation vary according to the location of the deformity and to the extent of overresection. For minor deformities, tragal cartilage or fascial grafts, either autologous or allogenic, are suitable. Cartilage remnants from cephalic resection of the LLCs cartilages are also well suited to this purpose, but in recent years our workhorse for such a problem has been FDC, which is diced so finely that it can be pressed easily through the tip of a tuberculin syringe and then used like a paste. However, for medium-sized defects, greater volume is required, and layered fascial grafts or cartilage harvested from the septum or auricle can be used for this purpose (Fig. 6.18). When using septal cartilage, a flat graft with beveled edges or a lightly morselized graft is preferred. Crushed septal cartilage is not recommended because chondrocyte survival is unpredictable. When using conchal cartilage, a soft malleable graft is obtained by cross-hatching the cartilage while leaving the opposite perichondrium fully intact; layered conchal grafts are preferred for the correction of saddle deformities confined to the cartilaginous dorsum. Finally, major defects involving the entire nasal dorsum are best reconstructed with DC-F grafts to create a uniform and natural-appearing restoration of the nasal bridge. However, in the complete absence of underlying skeletal support, a solid rib cartilage construct is first used to rebuild the L-strut, and the DC-F graft is used merely as an onlay graft to camouflage the underlying solid construct.
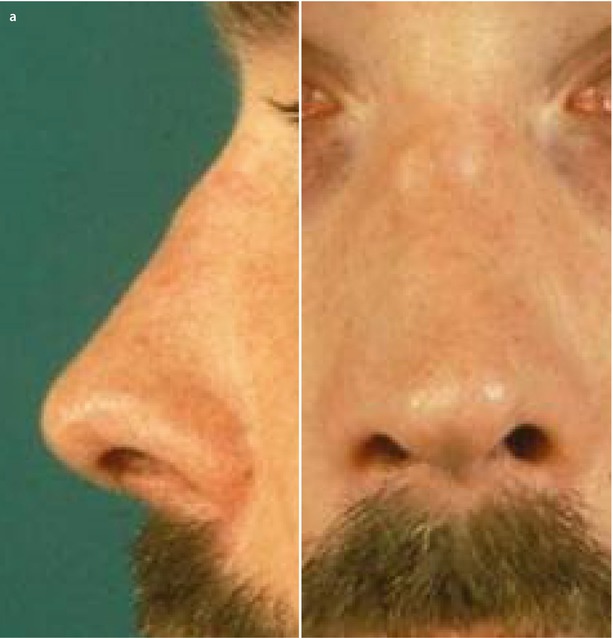
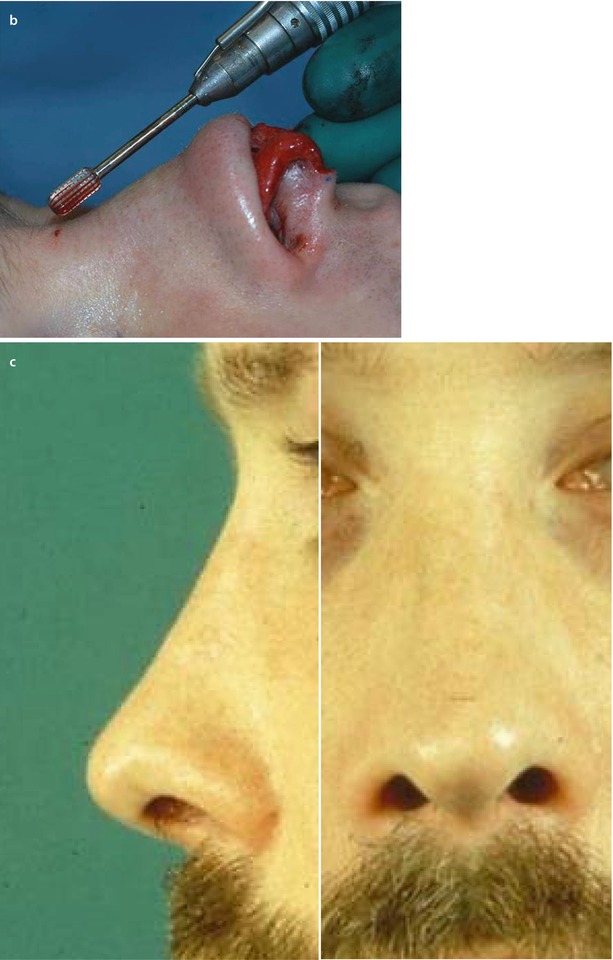
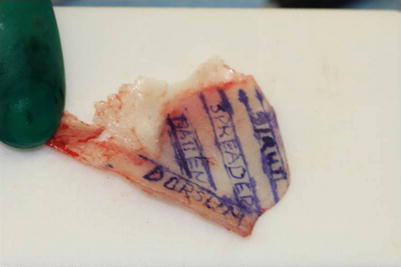
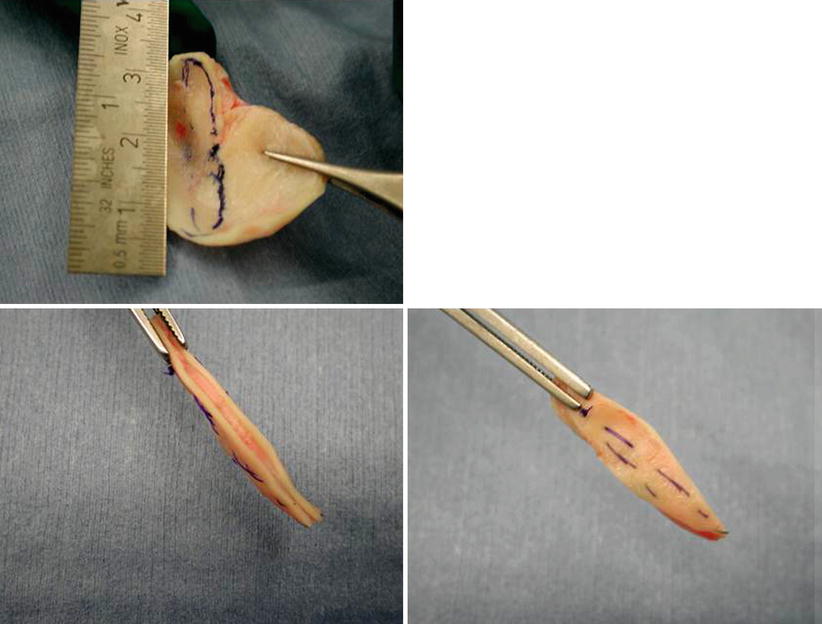
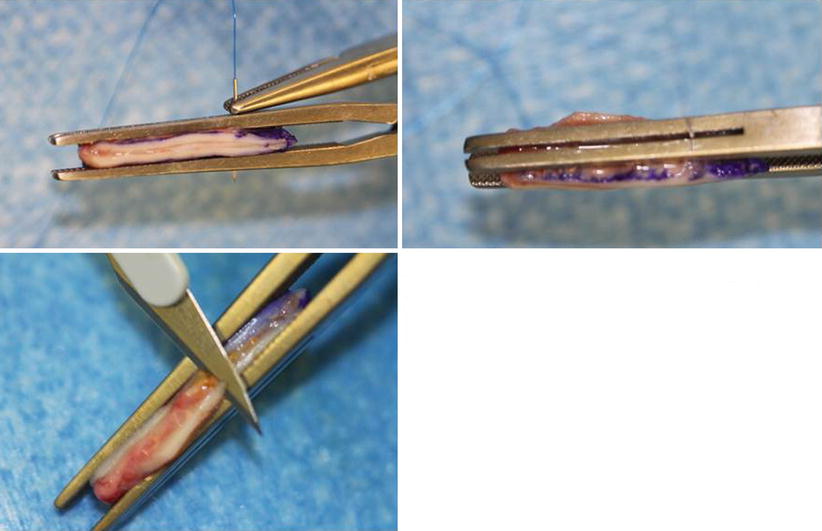
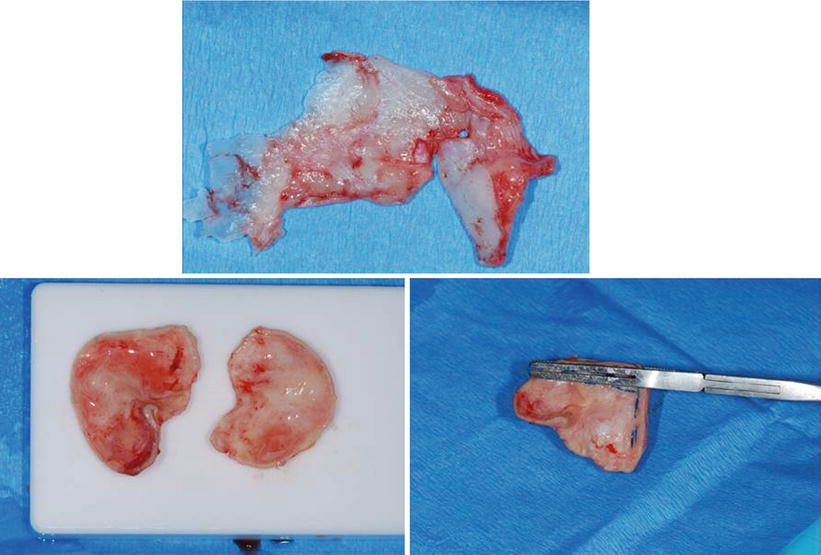
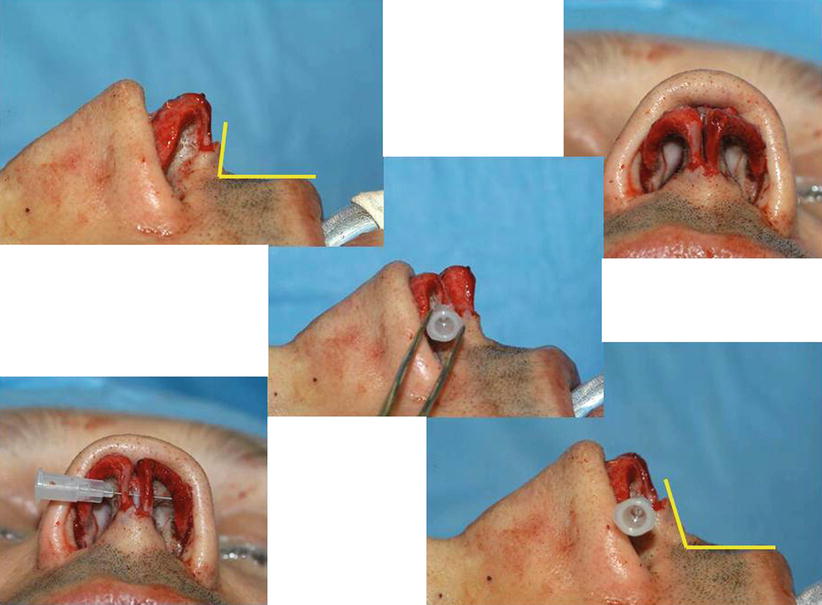
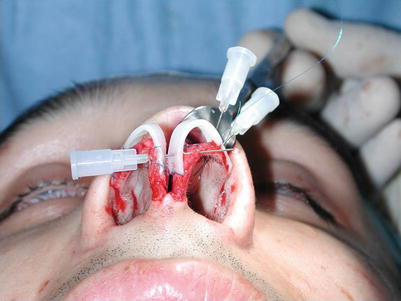
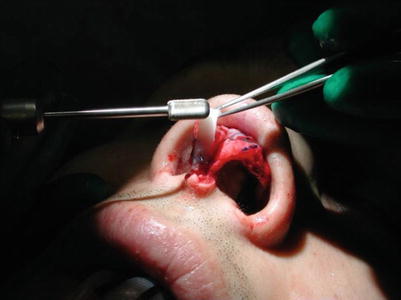
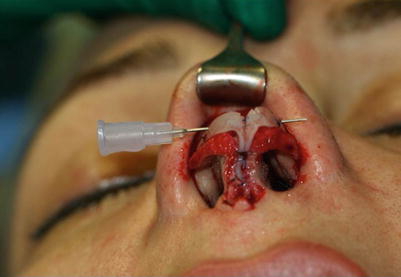
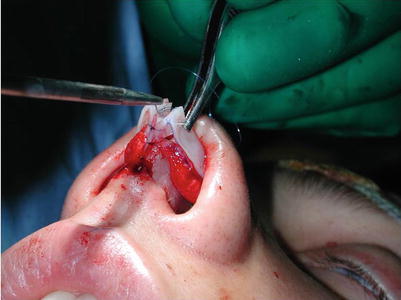
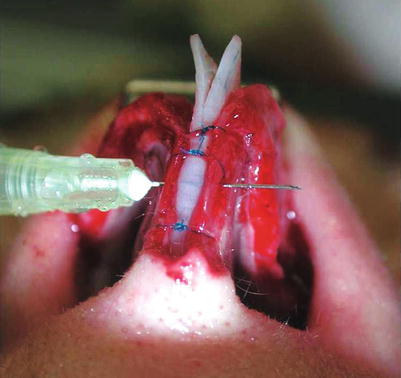
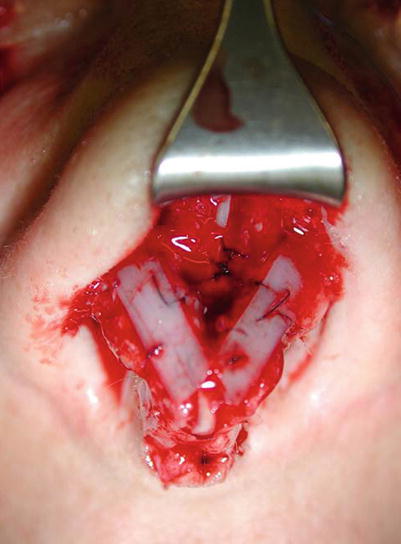
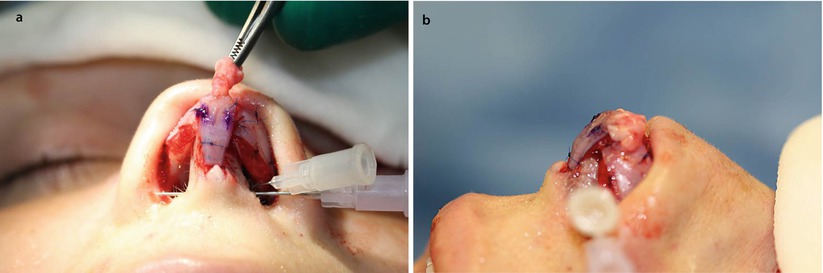
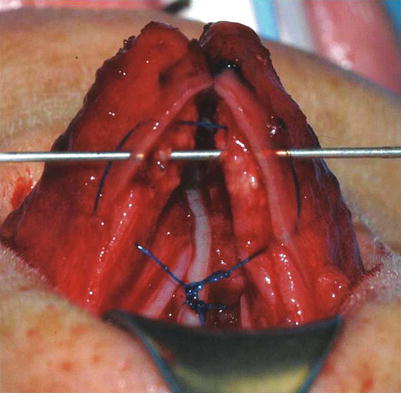
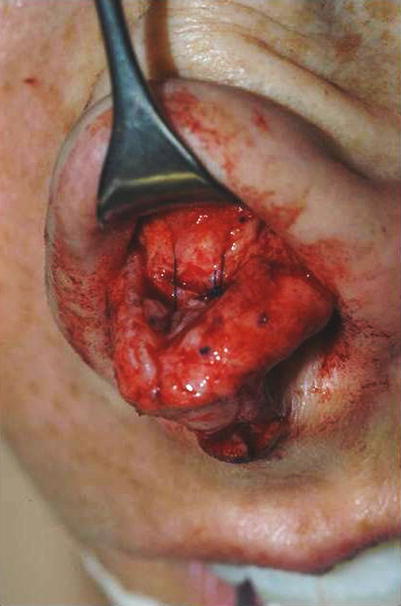
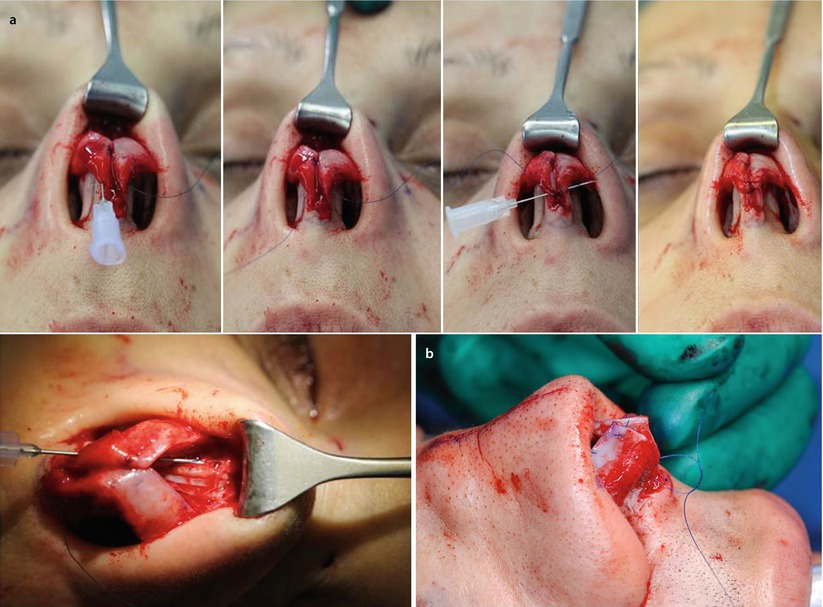
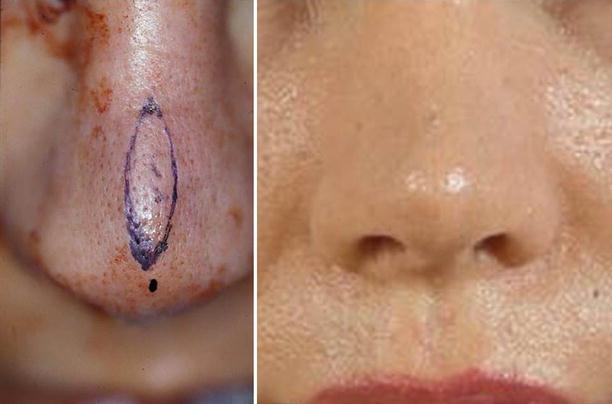
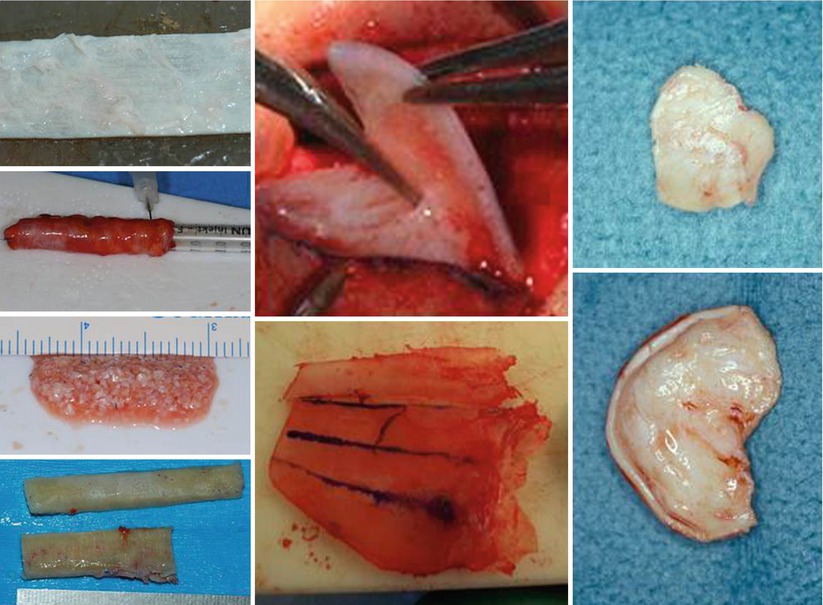


Fig. 6.1
(a–c) Motor drill for correcting bony irregularities

Fig. 6.2
Planning of the grafts

Fig. 6.3
Sandwich graft from the concha

Fig. 6.4
Modified Aiach clamp creating a sandwich graft

Fig. 6.5
Septum reconstruction from both conchae

Fig. 6.6
Tongue-in-groove technique

Fig. 6.7
Bending technique

Fig. 6.8
Thinning the cartilage by a motor fraise

Fig. 6.9
Scoring technique

Fig. 6.10
Dome division technique

Fig. 6.11
Split technique

Fig. 6.12
Batten graft technique

Fig. 6.13
(a, b) Covering the reconstructed framework with soft-tissue graft

Fig. 6.14
Spanning suture combined with tip suspension suture

Fig. 6.15
Posterior sling suspension suture

Fig. 6.16
(a, b) Anterior sling suspension suture

Fig. 6.17
Supratip excision

Fig. 6.18




Material for augmentation
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree