!DOCTYPE html>
Formulations for Sensitive Skin
Sensitive skin is a prevalent condition affection up to half of women and a third of men in some western societies (1–5). Unpleasant sensations of itching, burning, and stinging with exposure to various skin care products and/or environmental factors are experienced by affected individuals. The pathophysiological mechanisms are not yet fully elucidated; however, some biophysical and biochemical alterations such as impaired barrier function, smaller corneocytes, increased vascular reactivity, and decreased SC ceramides have been observed (6–10). Current evidence highlights a prominent role for increased sensory perception in the cutaneous nervous system (11). This chapter reviews the general considerations in formulations suitable for sensitive skin as well as targeted formulations based on our current understanding of involved pathomechanisms.
General Considerations
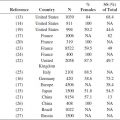
Sensitive skin is also known as reactive skin, hyperreactive skin, intolerant skin, and irritable skin. It is important to differentiate sensitive skin from sensitized skin, affected by specific allergens. Sensitive skin is very common, and as mentioned earlier, up to 50% of women in western countries and Japan complain of associated symptoms (5,12,13). Skin phenotype is not associated with the symptoms, but cultural conducts might affect the self-reported prevalence; large surveys from China report complaints in about 15% of women (14).
The high prevalence of sensitive skin creates challenges for patients, physicians, and the cosmetic industry. Product formulations for sensitive skin are somewhat challenging considering the lack of validated dermatotoxicological testing specific for sensitive skin. Recent surveys of more than 28,000 American adults showed that about 11% use skin care products directed toward sensitive skin (15). This highlights another challenging fact, which is lack of a standard definition for consumer products marketed for sensitive skin. Regulatory and marketing measures are exceedingly important topics that are beyond the scope of this chapter.
In addition to the considerations mentioned earlier, it is best to develop basic formulations with few ingredients to minimize the risk of overreaction. Specifically, avoid using ingredients with the potential to induce irritation or sensitivity such as glycolic acid, lactic acid, propylene glycol, fragrances, herbal or essential oil extracts, and lanolin (16). Alcohol-based formulations should also be avoided. Skin cleansers should preferably be nonfoaming, with a neutral PH, and contain no exfoliates. Physical sunscreens are generally better tolerated than chemical sunscreens. In general, shorter ingredient lists composed of elements with less potential to cause active sensitization and or irritation are favored. Key features can be summarized as follows:
• Short list of ingredients
• Avoiding sensitizers and irritants
• Increase hydration and TEWL
• Enhance barrier repair and function
• Active intervention such as anti-inflammatory and neuromodulatory ingredients may be considered Better understanding of the underlying pathomechanisms has helped with active targeted therapies, reviewed in the following.
Barrier-Enhancing Products
Some patients with sensitive skin have altered skin barrier function, decreased amount of lipids, and smaller corneocytes, affecting barrier stability (7,8,10,17), leading to increases (TEWL and decreased skin tolerance threshold (18,19). It has been shown that individuals with sensitive skin are more likely to react to an irritant patch test and have a higher risk of developing contact allergies up to five times more compared to controls (3,6,20). Therefore, using barrier-enhancing skin care products free of irritant and potential allergens is an integral part of management.
SC lipids are essential in establishing barrier hemostatic function.
Topical application of lipids can improve barrier repair and reduce TEWL. Physiological and non-physiological lipids enhance barrier function in different ways.
Main SC lipids include ceramides, cholesterol, and free fatty acids. Upon exogenous application, these lipids quickly travel through the SC to the nucleated epidermis and will be incorporated into the lamellar bodies (21,22). Lamellar bodies are secretory structures derived from the trans-Golgi network. They secrete their contents, including lipids (glucosylceramides, sphingomyelin, phospholipids, and cholesterol) into the upper layers of the epidermis and are crucial to SC homeostasis and barrier function (23).
Therefore, the composition of topically applied physiological lipids can affect the formation of normal and abnormal lamellar bodies and their subsequent function.
It has been shown that optimal benefit in barrier repair is achieved when equimolar mixtures of physiological lipids are used in topical products (24). Yang et al. (25) showed that the equimolar ratio of ceramides, cholesterol, and fatty acids (either the essential fatty acid, linoleic acid, or the nonessential fatty acids, palmitic or stearic acids) allows normal repair and accelerated barrier repair up to threefolds with the application of optimal lipid mixtures. The topical application of a lipid mixture of (cholesterol, ceramide palmitate, and linoleate 4.3:2.3:1:1.08) has been shown to accelerate barrier repair following extensive disruption of the barrier by acetone (25). The application of only one or two of these lipids to distressed skin can delay barrier recovery (24).
Nonphysiological lipids such as petrolatum and mineral oil can enhance barrier repair by forming bulk hydrophobic phase in the SC interstices (24,26–28).
The goals mentioned earlier apply when developing cleansers for sensitive skin. Attempts should be made to maintain the integrity of barrier function and skin surface lipids as well as SC hydration and surface pH. Ongoing research is being done to further advance formulations that are more appropriate for sensitive skin (16,29–31).
Neuromodulatory and Anti-Inflammatory Pharmacological Interventions
Increased sensory perception is a prominent part of sensitive skin. Unmyelinated sensory C fibers have a primary role in nociceptive sensations in the skin and are associated with sensitive skin symptoms. It is conceivable that the cutaneous nervous system is also involved in the perception of unpleasant sensations triggered by environmental exposures such as rapid temperature changes. Increased sensation can potentially be associated with increased neuronal stimulation due to insufficient barrier function (11,32). However, many patients with sensitive skin do not express biophysical or biochemical changes in their epidermis. Many patients with AD experience similar symptoms, while earlier studies suggested increased density of peripheral nerves in the patients with AD compared to controls; however, other studies do not confirm this (33,34). Tsutsumi et al. (35) showed normal epidermal nerve density in both patients with or without atopic dermatitis. Buhe et al. (36) recently showed that the number of peptidergic C fibers, which are involved in the perception of pain, temperature, and itching, were especially decreased in individuals with sensitive skin compared to controls, suggesting that this subtype of nerve endings may undergo degeneration following contact with environmental factors. Specific nociceptive channels on these nerve endings, such as TRP channels, could be overstimulated, leading to the release of neuropeptides including calcitonin gene-related peptide (CGRP) (36). Epidermal TRP channels are expressed on cutaneous nerve endings and are known to promote the release of neuropeptides, inducing cutaneous neurogenic inflammation (11,32,36
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree