Finding the right first academic sports medicine job is a complex undertaking. There are a number of factors that go into the decision, including finding the job opening, limited regional availability, various academic affiliations, and organizational nuances, as well as payment structures. This article details the many facets of academic sports medicine that make up a position and can greatly affect surgeon workflow, productivity, and overall happiness.
Key points
- •
Academic sports medicine positions have limited availability each year, and are regionally restricted.
- •
Clarifying the clinical, research, and teaching expectations of the position are important to ensure a good fit.
- •
Many academic sports medicine surgeons change their jobs for professional advancement or as opportunities at other academic centers open.
Finding the first academic job is a complex decision based on a number of factors. While entering an academic sports medicine position appears to have multiple rewarding facets to it, there are multiple characteristics that can be unforeseen initially. The purpose of this article is to discuss how to initially find and prepare for academic sports medicine practice.
The job search
Most academic jobs, especially at larger university-based academic centers, have to be posted publicly. The requirements of many of these state or university positions mandate that they open up the application to all those who wish to apply. This often happens through the generic university or academic institution human resources website.
They are relatively easy to find through generic search engines because these are publicly posted. They are also often posted through sports medicine fellowship forums and the American Orthopedic Society for Sports Medicine job board.
Many of these jobs are cyclic in nature on the academic calendar and will begin recruiting over a year in advance. In accordance with the academic calendar, interviews often begin in the Fall months, the year prior to the anticipated start date. This is in contrast to many private practice positions, in which recruitment can move rapidly and interviews may only start a few months before the expected start date.
A surgeon moving to another institution and leaving a vacancy can have a ripple effect throughout the academic sports medicine positions. If someone leaves a particularly desirable job, then a more senior person at another institution may move into that role. Therefore, the initial institution that was left may not actually be the vacancy that is available.
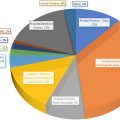
There may only be a few job openings available in any given year, as there is a finite supply of academic sports medicine positions due to the relatively limited number of academic medical centers. A 2019 review of sports medicine job postings found only 12.5% was for academic positions. Therefore, the desire to be purely academic may require the candidate to be open to a wide range of regional locations.
The academic medical center also hires generally based on a certain need. Due to the bureaucracy, many conversations and decisions have already been made through the medical center leadership in order to post a position. As such, there is likely a plan in place for the new surgeon, which may or may not be obvious from the initial posting. Therefore, it is important to understand and investigate what specific reason they have for hiring. Such reasons can include: vacancy or retirement, special niche, or pathology that needs to be addressed, expanding service line or geographic expansion.
If the opening exists because of a vacancy or retirement, it is important to know why that vacancy exists. Did the former surgeon leave for a better opportunity? Did they leave due to being unhappy? Were they fired? It is also useful to understand what the department and division’s intent on filling that vacancy may be. Do they want to just jump right into the prior surgeon’s practice doing the same thing? Or do they have additional plans or change of direction for the position?
In summary, it is important to know that the academic sports medicine jobs will often be cyclical in nature, with few university medical centers hiring in any given year, and will often be approved to fill a particular need. Additional details are obviously important, but will need to be investigated further into the interview process.
Interviewing and clarifying details
While the applicant can get a good idea of the position from the posting and word-of-mouth, specific details will often have to wait to be discovered further into the process and during the interview. The overall goal for the interview is to determine what the position will actually be like, and to discern if this is a good fit for your academic sports medicine aspirations. The previously mentioned reasons for hiring and particular niche they may be hiring for can be further confirmed at this stage.
In this section, the authors will cover the general format for academic position interview process, as well as the details that should be clarified to ensure the position is a good fit.
Once the official application has been completed, the interview process can involve multiple steps. Initially, the process starts with shorter, screening type of interactions, which then evolve into more of a recruiting and enticement environment when a desired candidate has been found. The first round of interviews in the most recent era has transitioned to a videoconference with some form of the ‘faculty search committee.’ This is often a somewhat formulaic basic interview with members of the division or department of orthopedics as a whole. During this first round, a screening interview is conducted to determine basic personality, as well as to see if the applicant’s responses mesh with the hiring goals of the institution. For example, the sports medicine division may need someone to do hip arthroscopy, but the applicant may only have interest in complex knee or the sports medicine division may want the hire to work as a satellite, independent practitioner, but the applicant desires to be core faculty working within the full traditional academic lines. This first-round interview serves as a low-cost and time-saving way to evaluate those who might be good candidates to bring for an in-person interview.
The in-person interview is a time- and resource-intensive process for the university. They will likely have you meet with a number of departmental and divisional personnel, and this is where the additional details of the position can easily be clarified.
An early detail that needs to be clarified is how closely aligned with the department they expect the position to be. The roles and responsibilities from an academic medical center vary based on whether you are core faculty within the medical school and residency, or if you will be essentially a satellite private practitioner with no direct academic expectations. Other important factors to consider and delineate during the interview process can be broken down into the categories of clinical, teaching, and research.
Clinical Practice Details
From a clinical perspective, determining what the operating room (OR) looks like will have an effect on your ability to be efficient and will need to be clarified. The distinction of whether you are core faculty will also determine whether you are directly involved in resident or fellow education and what assistance you will have in the OR. The expectations when interacting with a first assistant or physician’s assistant can be drastically different than those of educating a resident or fellow. As such, your daily work flow can depend on this distinction. Along these same lines, the respective roles of clinical support staff such as a nurse, medical assistant, and athletic trainer varies significantly across institutions. Some academic medical centers have a large pool of support staff, whereas others are more bare bones. Managing this wide group of people can be challenging, yet helpful. The clinical team should be apparent to you during the interview process. While they can be helpful, this clinical team is often hired by the hospital or department, and are assigned to you. You may not have much say in changing or altering these personnel in a large academic setting.
Another clinical factor that is important to determine is available OR time. If you are replacing a faculty member, you may be inheriting their OR days and block time. Otherwise, you may or may not have guaranteed OR time and may have to earn additional time as your practice becomes busier. These are important distinctions to know because adding on cases to inconsistent surgical time can be a source of frustration and would be an unpleasant surprise after showing up.
Expected case mix is an important factor which shapes your practice. This can correspond with the specific niche you were hired for. However, as the newest addition, you will have the most availability in clinic for add-ons. As such, much of the pathology that the more senior faculty would prefer to defer from their practice will become part of your practice early on. Furthermore, there are often behind-the-scenes discussions among the division or department about what pathology or particular surgical cases they expect you to take on. The interview process is a good opportunity to ask everyone in the division and get a clear picture of what they expect your responsibilities to be.
One often-cited difference between academia and private practice is amount of control you have over the schedule. Determining the expectation at the institutional and departmental level of how you can control your own clinical schedule is important. Some institutions have set expectations about how many clinic sessions and how many patients per session you are to see. Others only focus on overall productivity and give discretion as to how to achieve that to the surgeon. Making sure the control aspect matches with your own personality and work expectations can be important for job satisfaction. For example, if you desire to change your clinic template to shorten the day on Friday afternoons because there are a lot of no-shows or it is very low yield, some institutions have a utilization team that has to approve that. This administrative team may also require you to open additional slots elsewhere, so as to not decrease your overall ‘patient access’. Some institutions have blanket clinic rules for every department across the university, which state how long a clinician has to see patients in each clinic session. While these are meant to increase productivity in some less-efficient specialties, this can place an additional time-burden on a fast-paced sports medicine practice that does not necessarily yield additional efficiency.
Teaching and Research
Another job characteristic that should be established during the interview process is the academic and teaching expectation. The amount of resident and medical student involvement, as well as lectures for didactics across the medical center can significantly affect your weekly schedule. Putting together a good academic lecture takes time and effort, which may detract from time spent on clinical productivity knowing these expectations ahead of time will play a role in framing your calendar. Similarly, academic positions generally include protected academic time, so there may be a percentage of your effort and time that the department plans to have set aside for research. While research and other academic endeavors are often just incorporated into the academic position, some institutions will compensate or provide incentives for academic achievement. This might include financial bonuses for publications and podium presentations, or additional academic resources for involvement in medical center and professional society committees. Previous survey studies have shown that those going into academic sports medicine specifically show higher propensity for leadership positions within the academic environment, and those coming from higher ranked residency programs tend to lean more toward leadership positions. ,
As such, many of these positions will expect some level of integration and involvement within departmental and hospital leadership.
The research infrastructure and capability of orthopedic departments at different universities varies significantly. The interview process will often include a meeting with research faculty, wherein you can glean what resources and staff are available, how much support, and how quickly the Institutional Review Board (IRB) can turn around proposals can greatly affect research productivity. Asking for a list of current ongoing projects can give a good idea of what the division and department is capable of. Research support staff such as research fellows and coordinators, will also provide a sense of the structure and capabilities of the division and department.
Overall, there are many academic aspects to consider, and you as the applicant need to be honest with yourself regarding academic aspirations and desires. If you enjoy teaching but are not passionate about research, then a job that is a set percentage of research is likely not a good fit for you.
Compensation
Another detail that needs to be clarified during the interview process (and some would say one of the most important details) is compensation. At some point during the interview, you will likely meet with the executive administrator or finance person in the department. This individual will elucidate the compensation, and is a good person to ask the difficult-to-ask financial questions.
Most orthopedic surgery jobs will include a guaranteed salary for the first few years, and the ability to transition to the compensation plan afterward. The initial contract may have some productivity bonus attached to it for meeting certain milestones. There is also often an academic component from the university or academic institution itself and a separate clinical salary from the university physician’s group. The breakdown of university versus physician group salary percentage varies across institutions. Often the university salary is fixed and based on academic rank, whereas the variable clinical salary comes from the physician’s group.
There are 2 primary compensation models that university orthopedic departments utilize once the surgeon progresses from their guaranteed salary: relative value unit (RVU) and collections based. The ways you prove productivity and earn income will need to be clarified in the interview process, so that it is not a surprise once the salaried time-period has ended.
The RVU-based system considers only the amount of work done, and not what money is paid by insurance or collected. In this way, the RVU system is somewhat agnostic to insurance status or patient’s ability to pay. The earnings in this model is found by multiplying number of RVUs by the “RVU multiplier” or how many dollars the institution is giving the surgeon credit per each work RVU. This multiplier is very important to clarify, and how the department or university arrives at this number would ideally be transparent and easily understandable.
Productivity Salary = ($/RVU) x (number of work RVUs)
Another large determinant of compensation in this system is if the RVUs get discounted for subsequent codes. This is often poorly understood by many surgeons and even the departmental administrator, as it is decided on an institutional level. It is advantageous to receive full credit for subsequent procedures, as it increases the number of RVUs you get credit for. For example, if you perform a rotator cuff repair, subacromial decompression, arthroscopic biceps tenodesis, and arthroscopic distal clavicle excision, there are several subsequent procedures, and the RVU credit the surgeon receives can change dramatically if they were only to receive 50% credit for each subsequent code after the first (as some institutions do). This should be very clearly delineated beforehand, as it can significantly affect compensation.
The other type of productivity-based compensation plan is collections-based. This is essentially a balance sheet of how much money from billing and insurance the surgeon has collected. This type of system is dependent on more insured patients and their ability to pay. Payment is also not consistent from patient-to-patient or insurance-to-insurance. This means that a particular surgery may earn the surgeon differing amounts of money based on the patient’s insurance or ability to pay. This differs significantly from the RVU-based system, which is consistent across patients. Therefore, the surgeon’s income is highly dependent on the patient population. If you will serve a high uninsured or under-insured population, a collections-based system might have limited potential in that market.
Aside from the direct monetary compensation, many people go into academia for a calmer work environment with the backing and reputation of a larger academic medical center and the ability to teach. This traditionally has meant less upside potential from a salary standpoint, as there is often not a true partnership to buy into, and the medical center owns the infrastructure. However, there may be some situations where the academic surgeon has potential for ancillary income. In some circumstances, the department may own the physical therapist service or the durable medical equipment and bracing. It would be helpful to ask if this is the case, and if there are any bonuses or extra income that would flow to the surgeon as a result. On very rare occasions, the medical center or university may contract with a separate surgery center, in which the surgeon may have ability to participate in partial ownership. It is appropriate to ask about these ancillary sources of income during the interview process since they can have a significant effect on the surgeon’s income level. This would provide not only a glimpse into the early salary, but also long-term financial incentives at the position.
Overall, though academic sports medicine has a higher research and teaching component, a large portion of your income will be dependent on clinical productivity. The institutional limits or limiting factors to productivity should be elucidated from the current surgeons in the division. While the system may not be purely RVU-based or collections-based, the payment schema generally falls into one of those categories. Asking the right questions during the interview process can mitigate any financial surprises going into the academic sports medicine position.
Team Coverage
Sports medicine as a specialty inherently involves care of the athlete. This is especially true at an academic medical center, as the sports medicine division often takes care of the university athletics, as well as contracts with many high schools and potentially professional teams. While these can be very good business leads and help bring in potential patients, high level athlete care is complex, and can take significant amounts of time and effort. Knowing what the expectations are beforehand can help the applicant determine if it is a good fit.
If there is an expectation or set team coverage role the institution is hiring for, that is the first detail that needs to be clarified. If they are hiring because of a senior staff member is retiring, you cannot often expect that the new role will immediately assume the sports medicine responsibilities of the person leaving. The senior faculty will have the more desirable coverage responsibilities, so others in the division will likely take on their now vacant responsibilities. You are likely to get a more junior role, or potentially less ‘desirable’, glamorous, or productive coverage responsibilities as those in the division move up the ranks. The sports medicine division may also be hiring for expanded roles due to recently expanded contracts and gaining additional team responsibilities. In any case, if there is a definitive coverage plan for your role, it should be clarified before starting.
High level team coverage and becoming an expert team physician is a skillset that develops over time. When starting the new job, there are often political or set relationships within the athletics department that would be good to know beforehand. The head athletic trainer can significantly affect the way in which care is organized and who each athlete sees. Getting a sense of the general organization and key players, as well as their personalities and expectations is good to know as well. This is especially true if you are being hired to take primary coverage over a new team for the division or stepping into an immediate head team physician role. A new head team physician role or chief medical officer for a professional team can be a significant amount of extra phone calls and work that is likely uncompensated. This responsibility includes devising emergency action plans, protocols for injuries and return, and overall being the dispatcher and primary contact for the team no matter what the medical ailment may be. Due to the increased workload, setting expectations beforehand can save a significant number of unhappy surprises later.
Even though you may take on a team physician role, it can take time to establish good rapport with team coaches and athletic trainers. As such, the referral patterns and trust may be somewhat rigid at first, and they may still send injuries to more senior surgeons. This is part of the learning and practice establishment process, and there is not much to be done regarding this.
Team coverage can be very rewarding, but can also take significant effort and time on part of the surgeon. This is often seen as outreach and business development for the division and department, but there may be instances, where it is compensated from the institution. While that should not be the expectation, it behooves the interviewing surgeon to ask specifically what to expect. There have been studies evaluating the cost-benefit analysis of high school team coverage, demonstrating that it can be financially beneficial. However, university and professional coverage responsibilities and time requirements may drastically differ and sway this calculation. While direct monetary compensation is not common at the university level, some institutions will provide additional time or protection against clinical duties if there is significant effort spent on team care. This can come in the form of additional protected academic time while still being considered a full-time employee or a decreased call schedule burden. If it appears that there will be significant time and effort spent on team coverage, it never hurts to ask very specifically and potentially negotiate these ‘in-kind’ compensations. These after-hours additional responsibilities can truly affect professional and personal lives, so it is necessary to ensure you are willing to pursue a position with significant team coverage responsibilities.
Family and Personal Preferences
While finding the right academic job has many facets professionally, these cannot exist in a vacuum. As just discussed in the ‘team coverage’ section, establishing practice and after-hours expectations can be an unpleasant adjustment. This is especially true as many applicants at this point in their lives may have a spouse or family that they need to consider as well. Just because it is a good professional opportunity does not mean it will be good for you and your desired life.
Many of the available academic jobs may not be in a place where you have much family or social support, so it is very important that the professional considerations are weighed against the cost to personal interests or family. A consideration should be given to the age of your future partners, and whether there will be colleagues or colleagues’ children of similar age. Family support from the department and institution can go a long way to ease this transition. Although the job may be a good professional opportunity, it may still not work out well. Would it be worth it to have to move after a few years for a better job? Would your potential family be comfortable with relocating when another future opportunity arises?
It is important to consider how your personal interests align with the region of interest as well. For example, if you grew up in the mountain west enjoying outdoors and skiing and there is an opportunity in the southeast, lifestyle, and personal preferences should be weighed in the calculation. It may not matter how professionally fulfilling a job can be if you are miserable and not able to do the things that bring you joy outside of your career.
Many interviews will occur in several stages, and there may be an opportunity to bring your family or spouse for a visit in order to get a sense of what the city, university, and region have to offer. It is encouraged to meet or discuss with another recent faculty that moved from out of the region in order to gain their perspective on the area. This can not only inform how the transition would be, but also help start the process of where you may want to live if relocating.
Planning for Advancement
Academia is often a world of advancement and rank. Climbing the professorial ladder is generally encouraged at a university, so understanding the timeline and expectations from the department are useful for setting long-term goals. Some questions that can be asked include:
- •
How long does it take for people to advance from assistant to associate professor?
- •
Is there an expectation to meet the milestones for advancement?
- •
Are there any common reasons for not advancing?
- •
Does higher rank provide any tangible benefits? (more protected time, significantly higher benefits or salary, etc)
- •
Have any surgeons left due to academic advancement issues?
These professorship ranks matter variably at different institutions. Some will pay significantly different, and it may afford additional resources based on rank. This may even flow over into clinical benefits, as some centers pay variably for specific clinical work based on academic rank. While this is a longer-term goal, it is always good to keep in the back of your mind to make sure all the pieces are in place for you to flourish academically early in your career. Advancement has been previously linked primarily to research and publications, however, this formula is often a complex mix of clinical excellence, research, as well as teaching.
Summary
In the end, finding the right academic job is a multi-faceted and complex undertaking. While all the details we have outlined here are important, there may be no way to know all of them and make the exact right decision. Always remember that no job is perfect. There are benefits and detriments to every position. Academic jobs often have a large institution and research in addition to difficult clinical practice problems to contend with. These career choices can be very rewarding, but looking comprehensively at the position to determine if it is right for you is important. Also remember that a very high percentage of orthopedic surgeons change jobs after the first few years, and it is not uncommon for academic surgeons to move from one institution to another for additional opportunities. However, choosing the right starting point can significantly affect the type of academic sports medicine surgeon you become from a teaching and clinical standpoint. Keeping in mind the points contained herein will enable an informed assessment of the available academic sports medicine positions, and hopefully aid in finding a holistic fit.
1 Present address. 218 Poinciana Drive, Homewood, AL, 35209.
References
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree