Excision of Bone Tumors of the Femur
Raffi S. Avedian
DEFINITION
Bone tumors of the femur may be benign or malignant (bone sarcoma) and exhibit a variable natural history ranging from latent to rapid growth. Aggressive benign tumors and malignant tumors typically cause pain, dysfunction, and fracture.
ANATOMY
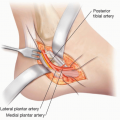
The femoral artery, sciatic nerve, and femoral nerve are important structures that need to be accounted for during surgery of the femur.
The common femoral artery enters the thigh under the inguinal ligament. As it travels distally, it gives several branches, the largest of which is the profundal femoral artery (PFA), which travels on top of the adductor brevis until the muscle inserts onto the linea aspera at which point the distal half of the PFA continues just posterior to the femur.
Several perforator branches from the PFA pierce the lateral intermuscular septum and go into the anterior compartment. The PFA is located near the linea aspera and is often ligated when resecting segments of the femur.
The superficial femoral artery (SFA) is the most important blood vessel when considering tumor excision. It must be preserved or reconstructed if excised, to maintain viable limb perfusion. As the SFA travels distally, it is located on the anterior surface of the psoas, adductor longus, and then adductor magnus until it courses through the adductor canal into the popliteal fossa. The sartorius muscle acts as a cover to the superficial femoral vessels throughout the middle of the thigh.
The sciatic nerve travels in the posterior compartment. It branches into the common peroneal nerve, which can reliably be dissected and found just medial and anterior to the biceps femoris in the popliteal fossa. The tibial nerve portion of the sciatic nerve stays midline with the popliteal vessels.
PATHOGENESIS
The mechanism for bone tumor formation is not known.
Risk factors for sarcoma development include radiation exposure, radiotherapy, pesticide exposure, and hereditary conditions including Li-Fraumeni syndrome and retinoblastoma gene mutation.
NATURAL HISTORY
Active benign tumors, such as giant cell tumor of the bone, chondroblastoma, and aneurysmal bone cyst, will progress over time and may recur after excision but are not lethal.
All bone sarcomas have the potential for local recurrence and metastasis.
Some bone sarcomas such as low-grade chondrosarcoma exhibit a slow rate of growth and low risk of metastasis, whereas aggressive tumors like high-grade osteosarcoma and dedifferentiated chondrosarcoma grow rapidly and have a relatively high risk of metastasis.
Tumor variables that are associated with increased risk of metastasis include high grade and large size (greater than 8 cm).
Lungs and other osseous sites are the most and second most common location of metastasis, respectively.
PATIENT HISTORY AND PHYSICAL FINDINGS
Pain is a common presenting symptom for aggressive bone tumors.
A thorough history and examination are important to assess duration of symptoms, comorbidities, physical dysfunction, organ involvement, overall health, and patient expectations to best tailor treatment strategy for the individual patient.
Neurovascular examination is mandatory for any extremity tumor.
IMAGING
Plain radiographs are used to formulate a differential diagnosis and a preoperative plan (FIG 1A).
Magnetic resonance imaging is routinely used to determine the extent of intramedullary tumor involvement, presence of soft tissue extension, status of the neurovascular structures, and preoperative planning (FIG 1B).
DIFFERENTIAL DIAGNOSIS
The differential diagnosis for a bone tumor includes benign tumors, sarcomas, lymphoma of the bone, infection, and metabolic lesions (eg, hyperparathyroidism).
The most common bone sarcomas are osteosarcoma, chondrosarcoma, and Ewing sarcoma.
SURGICAL MANAGEMENT
The appropriate treatment for any musculoskeletal tumor is based on its diagnosis and natural history.
Biopsy incisions are considered contaminated and must be resected at the time of definitive surgery. Care should be taken to place the biopsy in a location that does not interfere with the final surgical plan.
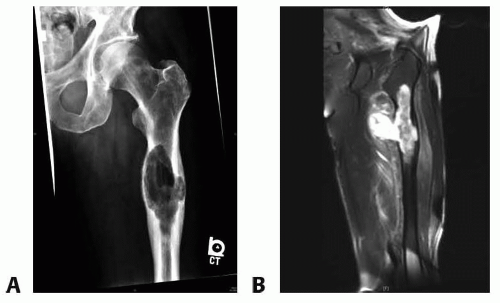
FIG 1 • A. Anteroposterior radiograph of a 67-year-old man with highgrade chondrosarcoma of the proximal femur seen as a large lucent lesion. B. Coronal T2-weighted MRI of the same patient demonstrating extensive soft tissue component and intramedullary involvement by chondrosarcoma.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree

 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access