The preoperative evaluation plays an important role in optimizing outcomes and minimizing morbidity for patients undergoing blepharoplasty. This article provides a detailed, systematic approach for the preoperative evaluation of patients undergoing upper and lower blepharoplasty. This article focuses on the critical steps of evaluating surgical blepharoplasty candidates to ensure optimal outcomes and high patient satisfaction, while minimizing risks and complications.
Key points
- •
Effective patient evaluation is paramount to achieving successful outcomes in blepharoplasty.
- •
A thorough medical and ophthalmic history, alongside a comprehensive physical examination, forms the core of patient assessment.
- •
Detailed photographic documentation and advanced diagnostic testing play crucial roles in preoperative planning and postoperative assessment.
- •
Effective communication regarding patient expectations and potential complications is essential for patient satisfaction.
- •
Proper patient selection based on clinical evaluation ensures better outcomes and minimizes postoperative complications.
Introduction
Blepharoplasty is a nuanced procedure designed to improve the aesthetic appearance and functionality of the eyelids. The procedure has historical roots in both reconstructive and cosmetic realms. Descriptions of reconstructive blepharoplasties appeared in the Sushruta Samhita and other texts as early as 600 BC. Modern blepharoplasty procedures combine detailed anatomic knowledge with advanced surgical techniques to achieve both functional and aesthetic goals. ,
Upper and lower blepharoplasties each target specific pathology of their respective regions. Upper blepharoplasty most commonly addresses excess skin and fat that contributes significantly to facial aging and can impair vision. Lower blepharoplasty tends to focus on the correction of under-eye bags and hollows, restoring a youthful eye shape, and enhancing overall facial aesthetics. Surgical techniques discussed in later articles include orbicularis retaining ligament release, resection and/or repositioning of post-septal fat, removal of excess anterior lamellar soft tissue with skin pinch, skin flap, or skin-muscle flap, canthal tightening procedures, and adjunct noninvasive procedures such as laser resurfacing, chemical peels, and fat grafting. Appropriate patient evaluation is critical to improve safety and outcome predictability in all cases. , This article highlights components of a comprehensive patient evaluation for the blepharoplasty patient.
Discussion
Patient Goals and History
Goals
Plastic surgeons should first understand the patient’s main aesthetic and functional concerns. Open-ended questions allow the patient to explicitly describe goals for consultation in his or her own words. The patient’s perception of their aesthetic issues should be in line with the surgeon’s pre-operative examination. Incongruity between the 2 is a red flag that should prompt further discussion and counseling prior to surgical intervention.
Medical history
A thorough medical and ophthalmic history is critical to optimizing patient safety. Certain systemic conditions are of particular importance, as they may increase case complexity or place patients at higher risk for postoperative complications. Uncontrolled hypertension, bleeding disorders, non-steroidal anti-inflammatory (NSAID)/anti-platelet use, and herbal supplementation may increase the risk of bleeding Thyroid disorders should be identified and stabilized prior to surgery, as worsening of hyperthyroidism can lead to post-operative lid lagophthalmos or proptosis. It is critical to inquire about previous periorbital surgery, glaucoma, and diabetes in the preoperative assessment. An ophthalmic evaluation that assesses visual acuity and screens for presence of any dry eye symptoms should also be performed. Up to 95% of patients undergoing laser-assisted in situ keratomileusis (LASIK) surgery report dry eye symptoms postoperatively. The procedure transects corneal nerves, which contributes to dry eyes through a combination of corneal hypoesthesia, impaired blink reflex, and interruption of aqueous tear production by the lacrimal system. It is thus recommended that patients undergoing LASIK should not have subsequent blepharoplasty procedures for at least 6 months. Patient evaluation is critical in diagnosing underlying problems, formulating a treatment plan, and identifying patients at elevated risk for complications.
Physical examination
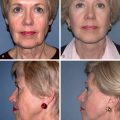
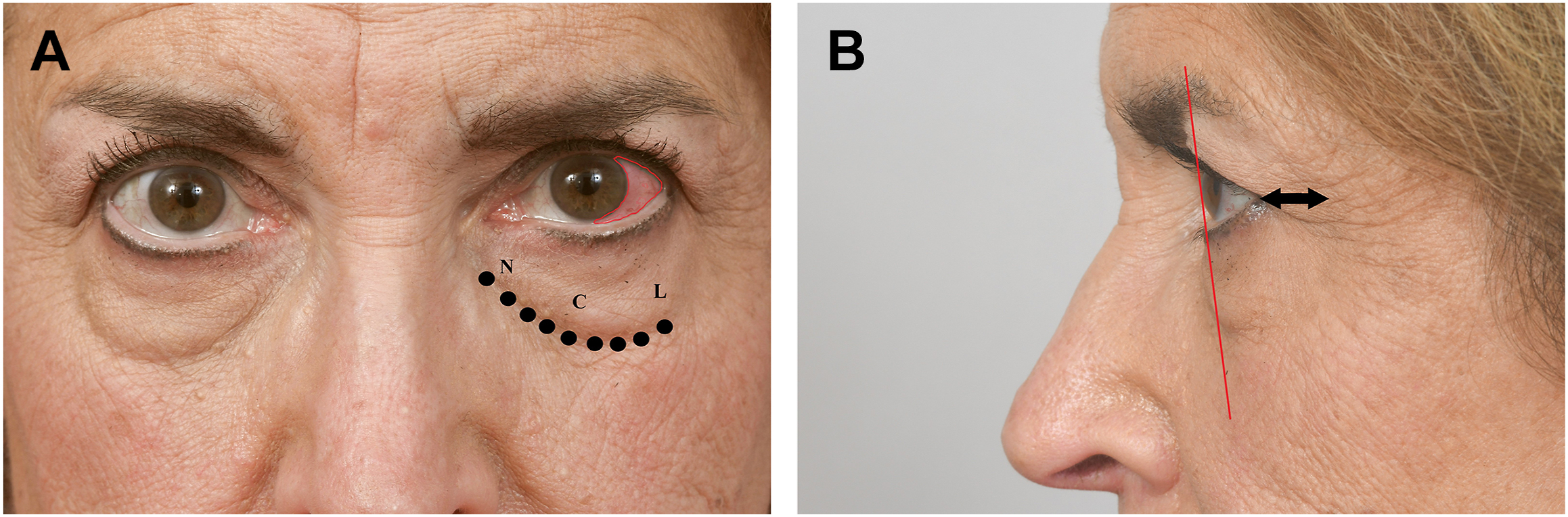
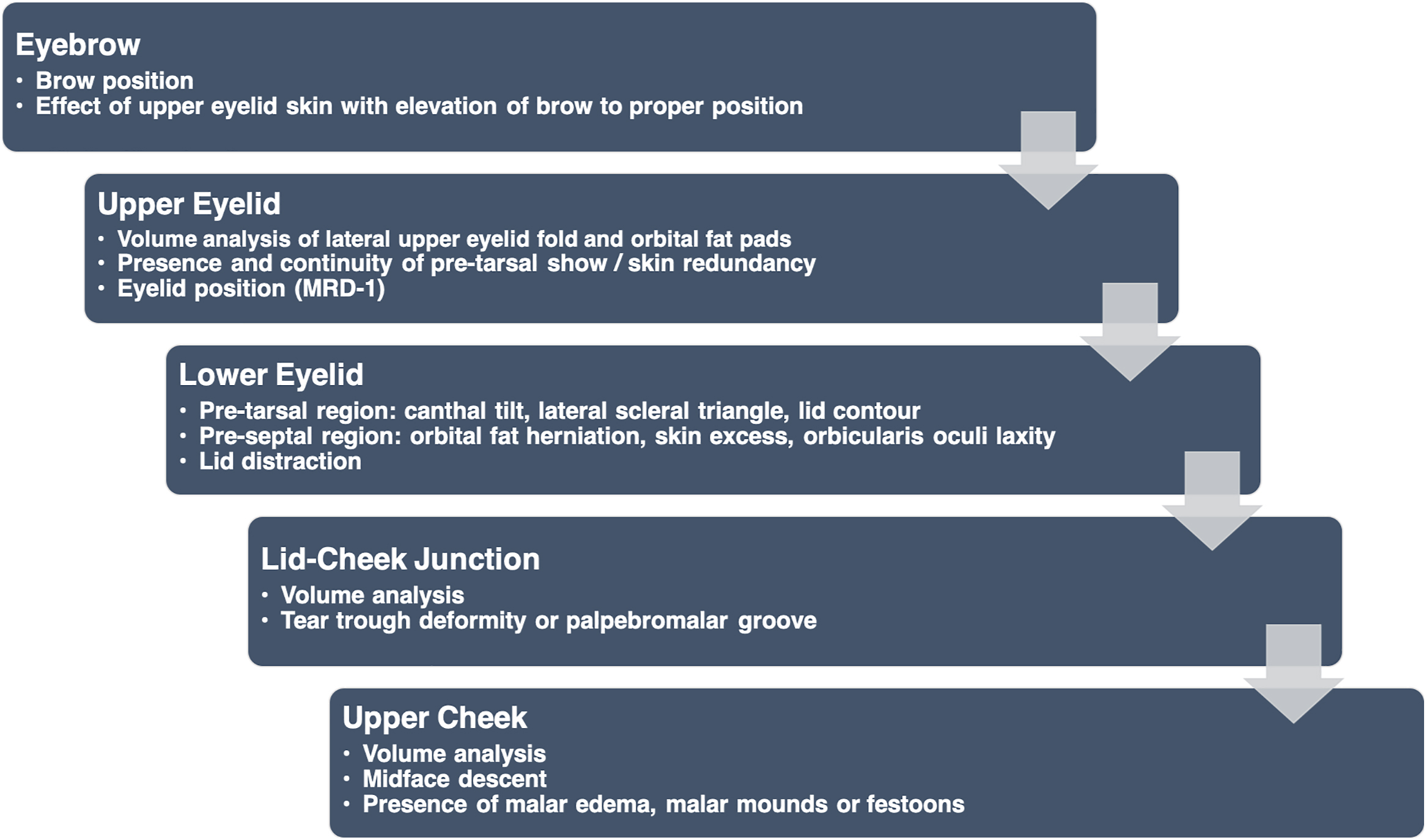
The blepharoplasty physical examination should assess both the functional and aesthetic aspects of the eyelids. Aesthetic evaluation will identify fat herniation and pseudoherniation, volume loss, skin quality, skin excess, eyelid shape, palpebral fissure shape, canthal tilt, and upper malar deformities ( Figs. 1 and 2 ). Functional analysis is imperative to recognize high risk patients and minimize post-operative complications. The senior author utilizes a systematic top-down-lateral approach to the preoperative blepharoplasty examination ( Fig. 3 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree