Key points
• Accurately identify the etiology of the asymmetry.
• Ensure that facial growth is complete before definitive treatment.
• 3D photographic imaging is an invaluable tool to educate the patient regarding the clinical findings and the anticipated outcome.
• Evaluate the contribution of both hard and soft tissues.
• Dermal fillers and structural fat can compensate for some skeletal volume deficiency, but there is no substitute for skeletal support to replace a skeletal deficiency—“replace like with like.”
• A combination of skeletal and soft tissue augmentation to create symmetry not only creates normal form but also restores normal texture.
Introduction
The chapter is not intended to be a detailed description of all etiologies of facial asymmetry; however, the most common are mentioned when the etiology impacts the treatment approach. Also, it is outside the scope of this chapter to address all aspects of pediatric asymmetry encountered in craniofacial surgery. The purpose of this chapter is to discuss the myriad of techniques and approaches that are incorporated into treatment of the adult who presents with facial asymmetry.
Our focus will be on those cases that range from mild asymmetry , to those cases in which there is gross deviation from the norm. What we hope to convey is the multitude of tools available to the surgeon. The traditional approaches to facial asymmetry were bone grafts, osteotomies, and microvascular flaps. Over the past decade, many new modalities have been well studied and found to have successful application in skeletal aesthetic surgery. Autologous fat grafting, although not new, has received much attention and research, providing surgeons with the ability to use it in the face more reliably and effectively. Dermal fillers that are long-lasting and permanent have been introduced and allow for precise application of volume in the facial region. Implant materials and computer-aided design and fabrication have rapidly advanced and gained acceptance for common use by maxillofacial surgeons. Finally, the relatively recent wide acceptance and use of virtual surgical planning (VSP) has given surgeons more accuracy in developing and executing treatment plans. With all these advancements, the surgeon is effectively an artist with a palette of tools with which he or she can use to create the desired facial form. It is with this philosophy that we embark on a journey to develop strategies to restore symmetry of the face.
Patient evaluation
Craniofacial asymmetries can be classified on the basis of etiology and on the anatomic structures involved. The causes of facial asymmetry are numerous and are best divided into three categories: congenital, developmental, and acquired ( Table 41.1 ). Congenital asymmetrical birth anomalies include such conditions as unilateral cranial synostosis, atypical facial clefts, and craniofacial microsomia, among others. These conditions perhaps represent not only the most severe forms clinically seen but also the most challenging in restoring the symmetry because many involve not only the facial structures but also the orbit, skull base, and cranial vault. The developmental asymmetries become evident later in childhood and adolescence, at a time when many are brought to the attention of the orthodontist primarily because of occlusal asymmetry. Perhaps the most common cause of the asymmetry in this group occurs because of a differential in condylar activity between the two sides in conditions of unilateral condylar hyperactivity. The etiologies of acquired asymmetrical deformity include facial trauma, surgical resections, and pathologic lesions. The varying etiology of facial asymmetry requires the surgeon to accurately diagnosis the patient’s condition because the indications and contraindications for each patient depend on the underlying cause of the asymmetry.
| Congenital | Developmental | Acquired |
|---|---|---|
Craniosynostosis
| Condylar hyperactivity | Facial trauma |
| Deformational plagiocephaly | Idiopathic causes | Parry-Romberg disease |
| Muscular torticollis | Fibrous dysplasia | |
| Facial clefts | Skeletal tumors | |
| Craniofacial microsomia | Soft tissue tumors |
Common etiologies of facial asymmetry
Craniofacial microsomia (congenital)
After cleft lip and palate, craniofacial microsomia is the second most common congenital anomaly of the head and neck region. The condition affects multiple tissue planes—the underlying skeleton, the overlying facial musculature, and the subcutaneous tissue—to varying degrees of deficiency. In the vast majority of the cases, the condition is unilateral; however, in 10% to 15% of the cases, there is bilateral involvement (bilateral craniofacial microsomia). When present in the bilateral form, the two halves of the face are differentially involved, and the face is asymmetrically affected. ,
The OMENS-Plus classification that evolved from a series of proposed classification schemes by David and Cooter, Vento et al., and Horgan et al. The acronym stands for orbit, mandible, ear, nerve, and soft tissue, with each variable assigned a severity index ( Table 41.2 ). The “plus” indicates the extracranial involvement. The more recent pictorial classification of OMENS by Horgan et al. is an excellent visual tool. Compared with the simpler Pruzansky classification, the more comprehensive classifications are not as clinically practical in guiding treatment planning. However, they have the benefit of ensuring that all of the components of the anomaly are assessed and objectively noted for management.
| Orbit | |
| O0 | Normal orbit—size and position |
| O1 | Abnormal orbit—size |
| O2 | Abnormal orbit—position |
| O3 | Abnormal orbit—size and position |
| Mandible | |
| M0 | Normal mandible |
| M1 | Mandible, body, ramus, condyle, coronoid are present but diminutive |
| M2A | Ramus is present but hypoplastic and in an anatomically acceptable relationship to the glenoid fossa |
| M2B | Ramus is present but hypoplastic and is medially displaced |
| M3 | Ramus—absent or minimally present |
| Ear | |
| E0 | Normal ear |
| E1 | Ear—all structures present, but hypoplastic |
| E2 | Absent external auditory canal with hypoplastic concha |
| E3 | Absent auricle, malpositioned lobule remnant |
| Facial Nerve | |
| N0 | Normal facial nerve function |
| N1 | Upper facial nerve involvement |
| N2 | Lower facial nerve involvement |
| N3 | Upper and lower facial nerve involvement |
| Soft Tissue | |
| S0 | Normal soft tissue and muscle |
| S1 | Minimal soft tissue and muscle deficiency |
| S2 | Moderate soft tissue and muscle deficiency |
| S3 | Severe soft tissue and muscle deficiency |
Even though the extent of the deformity may include the entire hemicraniofacial skeleton, the mandibular deformity is considered the cornerstone. Asymmetrical mandibular growth and development are present in the vast majority as the initial presentation for clinical assessment and management. The mandible plays a pivotal role in progressive distortion of the facial skeleton on the affected side, with secondary compensation on the contralateral side. The hypoplastic mandible results in multiplanar deficiency of the hemimaxilla and obliquity of the occlusal plane by restricting the normal downward vertical growth of the maxilla. Correction of the mandibular–maxillary relationship does not necessarily correct the upper midfacial involvement, and additional procedures may be necessary to achieve facial symmetry.
Unilateral condylar hyperactivity (developmental)
Many authors have used the term unilateral condylar hyperplasia; however, the term unilateral condylar hyperactivity, suggested by Obwegeser, is more appropriate because it more accurately encompasses the various clinical presentations seen.
Idiopathic overgrowth of the mandibular condyle is unilateral, presents itself during pubertal growth as a developing mandibular asymmetry, and is self-limiting by adulthood. It is not evident at birth. The asymmetry becomes increasingly more noticeable in later childhood through adolescence. Often, it is useful to ask the parents to bring annual school photographs to review the progression of the asymmetry, and this helps confirm the diagnosis.
The underlying etiology remains unclear and may be varied, but the final outcome is a dysregulation in growth that occurs within the cartilaginous region of the condylar head. During this active period, technetium-99 scintigraphy can confirm condylar hyperactivity compared with the contralateral unaffected condyle. Although the nuclear scan does not provide insight into the etiology, its value is that a negative result on it confirms that growth is complete, and thus surgical intervention can be initiated.
Idiopathic asymmetry
Many patients present with minor to moderate facial asymmetry without an obvious etiology. These patients may have an extremely mild case of craniofacial microsomia, asymmetry at the extreme of normal variation, or an asymmetry that might be considered normal but bothers the patient. These patients are typical treated with less-invasive procedures to meet their goals.
Traumatic (acquired)
Perhaps the most common cause of dentofacial skeletal asymmetry is trauma. The asymmetry can affect any component, depending on the original fracture pattern, from isolated fractures to panfacial fractures. In the upper midface, posttraumatic nasal asymmetries and residual malar asymmetries are common. In the lower face, traumatic injuries to the mandible, of which nearly 25% involve the condyle, are among the more common causes of facial asymmetry in children and young adults. Complications from either lack of treatment or unsatisfactory outcomes of treatment include skeletal facial asymmetry, occlusal crossbite, lateral gnathism, various degrees of restricted motion to complete ankylosis, and osteoarthritis. In many cases, the early trauma goes unnoticed by the family and medical attention is not sought; and when medical attention is sought, the condylar injury is undiagnosed at the time of the assessment. The hemarthrosis that occurs with condylar compression injuries is often difficult to diagnose and becomes evident with restriction and ankylosis as functional asymmetry progresses. With condylar neck fractures, medial displacement by the lateral pterygoid muscle occurs, affecting the temporomandibular joint (TMJ) kinematics and the posterior mandibular height on the affected site. The condylar head remodeling adapts to maintain TMJ function. The extent to which subsequent facial development can remain symmetrical within an acceptable tolerance depends on the timing of the insult in the growth and development of the child and the extent of the injury. For additional information, the reader is referred to Chapter 42 , which discusses posttraumatic reconstructive strategies in depth.
Parry-Romberg disease (acquired)
Of the facial asymmetries, those caused by Parry-Romberg disease are characterized by a striking “sunken” appearance to the affected side of the face. There is a sharp demarcation from the normal hemiface. Frequently, there is a soft tissue crease in the forehead, a coup de sabre, which is a characteristic hallmark of the disease. The disease is progressive in nature, with atrophy of the skin, subcutaneous tissue, muscle, and dentoosseous framework in its severest forms. Intraoral findings of the atrophic process may involve the alveolar process, the palate, and the tongue on the affected side. In nearly 35% to 40% of the patients, the orbital region and the eyelid adnexal structures are involved, resulting in enophthalmos with loss of periorbital fat, eyelid atrophy with ptosis, and loss of eyelashes and eyebrow hair. Visual acuity may be affected, with involvement of the retina and the optic nerve. ,
The etiology of Parry-Romberg disease remains unknown. It begins insidiously in childhood to midadolescence, with relentless progression until it stabilizes typically in adulthood. The duration of the active phase of the disease process varies significantly, extending from 2 years to up to over a decade. Any orthodontic–skeletal and soft tissue reconstruction must take into account this variability in the duration of the active phase. Although there is little correlation between the severity of the soft tissue involvement and age at onset, the effect on dentoskeletal involvement does correlate with the age of the patient. In an overwhelming 85% of patients with osseous involvement, the disease could have started before age 9 years. With skeletal involvement of the maxilla and the mandible, the dental arch alignments are affected, and there is typically a lateral open bite on the affected side.
History
A thorough history is as critical as the physical examination in evaluating the patient with facial asymmetry. Several aspects of the history are critical in developing a successful treatment plan: When was the asymmetry noticed? Is it stable or progressive? Is the occlusion changing? Is there a history of trauma? Photographs from the patient’s childhood to his or her current age are also helpful in understanding the asymmetry. The answers to these questions can help the clinician narrow the differential diagnosis—congenital, developmental, neoplastic, or traumatic.
Differential diagnosis
Congenital asymmetry, by definition, is present at birth; yet subtle asymmetries may not be obvious, given the abundance of subcutaneous fat in the infant. Craniofacial microsomia is the most common congenital cause of facial asymmetry, and as the child matures, the asymmetry becomes more obvious. Most studies have shown that craniofacial microsomia is not progressive, so the degree of asymmetry should be consistent on the images from the patient’s youth to the current age. Because craniofacial microsomia is congenital, the occlusion should be stable, and an actively changing occlusion is not reported.
Occasionally, the surgeon encounters a patient who reports new onset of asymmetry, but there are no physical signs consistent with a progressive etiology. In these cases, photographs taken through the patient’s life are critical in assessing or ruling out progression of the condition. It is not unusual for a patient with facial asymmetry to subconsciously position the head a certain way to minimize the asymmetry on the photograph. When the patient’s head is level, the asymmetry becomes more obvious. We find that these patients will frequently adopt a head position that minimizes the observed asymmetry, and this position is consistent in serial photographs taken over the patient’s life.
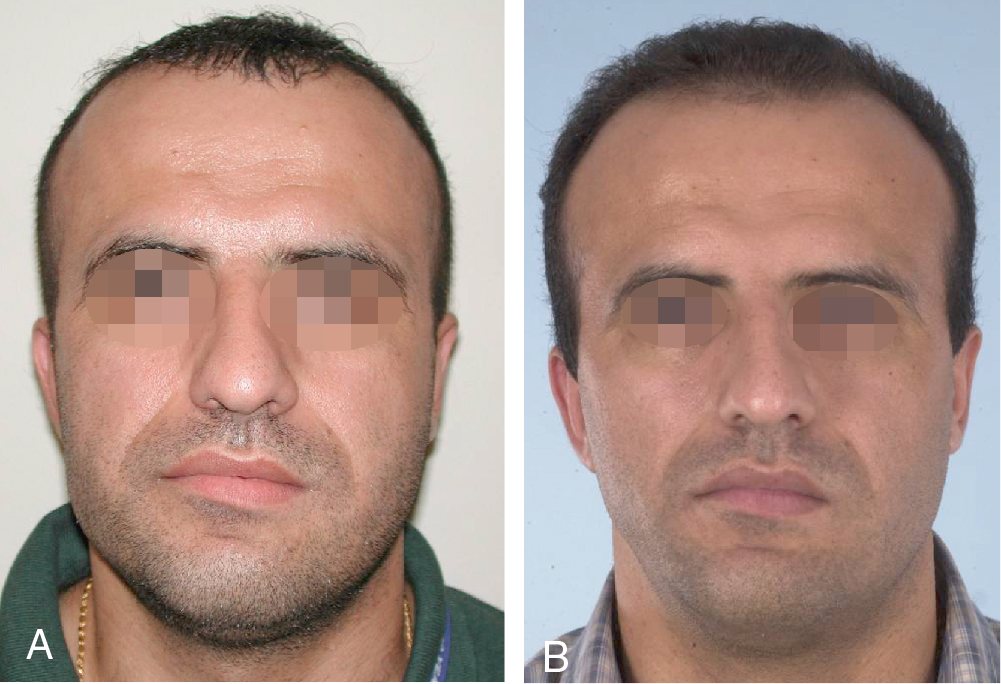
If the degree of asymmetry is progressive or a change in occlusion is reported, the surgeon must determine whether a developmental, traumatic, or neoplastic etiology is present. A change in occlusion occurs in a growing patient when the underlying etiology is causing such a rapid change in the jaw relationship that it exceeds the ability of the opposing jaw/occlusion to stay in a functional relationship. Condylar hyperplasia is an overactive condylar growth center that will cause rapid excessive condylar growth, leading to deviation of the mandible and a change in occlusion ( Fig. 41.1 ). As previously stated, a technetium bone scan is useful in confirming this diagnosis. A neoplastic lesion may also cause rapid jaw growth and can be identified with computed tomography (CT).

A traumatic condylar injury can damage the growth potential of the condyle, leading to lack of growth. This will present as mandibular deviation to the affected side as growth occurs. If the injury occurred at a young age, the growth of the maxilla may follow the pattern set by the mandible, and teeth may be in a functional occlusal relationship. These patients have a presentation very similar to that of patients affected by craniofacial microsomia limited to the jaws.
Identifying the underlying cause, whether traumatic, congenital, neoplastic, progressive, iatrogenic, nonsyndromic, or plagiocephalic, is important for formulating a treatment plan. After a detailed history is obtained, a thorough physical examination of the head and neck region should include observation and palpation of the entire scalp and face, assessing for soft tissue composition and mobility (of skin, fat, muscle, and connective tissue) and underlying bony structures, searching for differences between the two sides of the face.
Physical examination
Objectively assessing the patient who presents with craniofacial asymmetry requires a systematic approach. Each of the components—skeletal, dental, and soft tissue—must be assessed in all three anatomic planes with respect to each other. The natural head position must be noted. Knowing where the head is held in three-dimensional (3D) space is critical to understanding where one begins to establish the planes of symmetry. Many patients with facial asymmetry may exhibit postural compensation to minimize the appearance of the asymmetry. In such cases, correction of asymmetry must begin with an explanation to the patient that the asymmetrical position of the head in 3D space is to be distinguished from the internal asymmetry of the facial components. Whether treatment planning is with respect to the horizon, the interpupillary line, or to an agreed-upon external reference plane, must be clarified.
To determine the internal relationship of the facial components of symmetry, the surgeon must establish the true facial midline, a mirror-image plane of symmetry in which the reflection about the plane can be compared. However, in many patients with facial asymmetry involving the orbital region, defining that plane during surgery is often difficult. Geometrically bisecting the interpupillary line is not always reliable. For example, in patients with pronounced facial asymmetry involving the orbits, the plane that bisects the interpupillary distance does not necessarily match the plane defined by the skull base (crista galli–sella). Thus in more severe forms of facial asymmetry, the plane of symmetry may be difficult to define objectively. The surgeon may need to define the plane on the basis of structures that can be manipulated to establish improved facial symmetry.
In any comprehensive analysis of asymmetry, the face must be anatomically broken down into its “geometric” components—the skeletal masses, the dental arches, the soft tissue envelope, and the individual facial elements. Each of these components then must be defined by its spatial position in space relative to the plane of symmetry and by its individual shape relative to its counterpart.
The skeletal masses are the building blocks that structurally define the framework of the face. These include the frontal bone, the orbital complex, the malar/zygoma, the maxilla, and the mandible. The mandible itself is a composite of the ramus, body, and symphysis. Each of the maxillary and mandibular dental arches need to be assessed independently in terms of the dental midline, arch form, roll, yaw, and pitch. Each is then assessed with respect to its skeletal bases—the maxillary dental arch to the maxilla and the mandibular dental arch to the mandible. Finally, the interrelationship between the dental arches is assessed. The soft tissue envelope of the skeletal framework is assessed in regional subunits , in terms of its thickness measured from the skeletal surface (volume deficiency or excess) and surface topography to achieve the desired symmetry because the correction of the underlying framework does not necessarily correct the soft tissue envelope. Finally, individual facial elements, such as the ears, ocular adnexa, nose, and lips, which ultimately define the face, must also be assessed in terms of both spatial position and individual shape.
Thus when a patient presents with asymmetry regardless of its etiology, every component must be carefully assessed. Only then can a systematic multistaged reconstructive surgical plan be developed (see Indications and Contraindications ).
Image acquisition and virtual surgical planning
Traditionally, surgical planning for maxillofacial surgery was based on clinical examination, two-dimensional (2D) photographs, lateral and frontal cephalometric radiographs, and face-bow mounting of dental casts. Although for half a century this well-established approach provided reliable results in many patients, the outcomes were inconsistent for patients who presented with complex facial asymmetries.
It is only within recent years that accurate surgical planning came within the reach of the surgeon and the orthodontist with our ability to capture surface facial skeletal anatomy three-dimensionally with cone beam computed tomography (CBCT), with its the lower radiation doses; 3D optical and laser surface image capture of the color and texture of the facial appearance; and software that allowed manipulation of data.
The anatomic landmarks can now be more accurately located without the averaging of a 3D projection onto a 2D cephalometric radiograph. Cephalometric analysis no longer needs to be confined to the midsagittal plane. Analysis can now be performed in three dimensions to allow the surgeon and the orthodontist to visualize and address asymmetry in all three planes (see Chapter 17 ).
Today, the software for VSP is capable of simulating surgical procedures with ever-increasing user applicability. , The facial skeleton is treated as a solid 3D object in virtual space that can be digitally manipulated. Osteotomy planes can be defined, and the 3D facial skeletal object can be digitally sectioned into two separate solid objects, and each can now be moved independent of the other. Surgical planning can now be done in 3D space instead of in planar projection 2D cephalometric films. The complex facial skeletal asymmetries can be addressed. The surgeon now has the ability to easily execute various surgical options to optimize the outcome.
Additional tools, such as 3D photographic imaging, may not be as helpful in finalizing a treatment plan, but they are invaluable in counseling the patient about expectations, goals, and limitations before surgery. This imaging modality can be used to mirror the facial halves to each other to illustrate the differences to the patient. Various results can also be predicted to see how the patient feels about different interventions and the predicted outcomes. It is important that the surgeon is realistic about the results he or she can achieve to set and maintain realistic patient expectations.
Indications and contraindications
Forehead: The forehead is primarily a skeletal structure with a relatively thin soft tissue covering. Structural change involves osteotomy, bone grafting, or application of bone cement. Given the thin layer of soft tissue, only minimal deformities should be corrected with soft tissue fillers or fat grafting. The exception is the temporal region. Temporal asymmetry can be successfully treated with autologous fat, dermal fat grafting, or a long-acting filler (e.g., Voluma, Sculptra). Soft tissue augmentation can be used successfully either alone or over an alloplastic implant.
Orbits: Bony and soft tissue orbital symmetry is assessed in all dimensions—sagittal projection, horizontal distance from facial midline, and vertical height. VSP is helpful to evaluate preexisting orbital asymmetry and precisely plan symmetrical orbit position if an orbital osteotomy is indicated (orbital asymmetry is discussed in Chapter 33 ). An orbital osteotomy is a major operation and should not be performed without proper training in orbital–maxillofacial surgery. As an alternative, the surgeon may achieve a very good result with a camouflage procedure. Mild to moderate orbital asymmetry can be treated with an inferior orbital rim implant combined with the overlying placement of autologous fat.
Zygoma: The zygoma is the major bone in the malar region and is covered with the thick soft tissue of the cheek. The zygoma is intimately related to the orbit, and frequently, if asymmetry is noted in one area, it is also present in the other. Reestablishing true zygomatic symmetry requires zygomatic osteotomy, not a small undertaking for some surgeons. If osteotomy is necessary, VSP is a valuable tool in treatment planning. Fortunately, the thick cheek tissue covering bones allows less invasive procedures—such as bone grafting, alloplastic cheek implant, autologous fat grafting, or filler—to give the appearance of symmetry to the zygoma without osteotomy. For pronounced asymmetry, hard tissue replacement is needed. A bone graft requires a donor site and is prone to variable resorption but is autologous and ultimately revascularizes into the recipient site. An alloplastic implant avoids donor site morbidity and is predictable (does not resorb), but it is a foreign body. Regardless of the approach used to restore bony symmetry, fat grafting is a useful adjunct for localized volume additions to create optimal symmetry.
Nose: The nose is a midline structure that is frequently involved in facial asymmetry or, if deviated, may contribute to the perception of facial asymmetry. The nose should always be evaluated and any deviation corrected in a patient seeking correction of facial asymmetry (see Chapters 28 & 29 ).
Maxilla/Mandible: These structures are grouped because of the intimate relationship between their anatomy and treatment. The dental midlines are evaluated to ensure that they are congruent with each other and with the facial midline. If an occlusal cant is noted, it should be corrected to level the occlusal plane and thus the jaws. Orthognathic surgery is recommended to restore the jaws to a symmetrical position (see Chapter 20 , Chapter 21 , Chapter 22 ). However, if the dental midlines are close to or congruent with the facial midline and there is only a minimal occlusal cant, a camouflage procedure may be substituted for orthognathic surgery (see Chapter 25 ). This may meet the patient’s goals, with less morbidity and a faster recovery. Isolated mandibular asymmetry in a patient with class I malocclusion can be treated with a gonial implant and fat grafting. Our preference is to intentionally select an alloplastic polyethylene implant that is about two thirds the ideal size to replace skeletal symmetry. The remaining volume is restored by grafting autologous fat. This technique not only creates visual symmetry but textural symmetry as well. The overlying soft tissue of a hypoplastic mandible is also deficient. Expanding the deficiency with a combination of an implant and grafted fat creates a more symmetrical appearance and feel compared with the result achieved with an alloplastic implant alone (see Chapter 27 ).
Chin: Chin surgery is a powerful tool to correct or alter facial symmetry. The chin can be moved separately from the jaws in orthognathic surgery or can be repositioned as an isolated procedure. (See Chapter 27 for an in-depth review of genioplasty and its impact on facial symmetry.)
Soft tissue envelope: Some patients may have subtle degrees of facial asymmetry but are unwilling to undergo surgery. In these patients, dermal fillers or fat grafting can be employed to improve symmetry in a minimally invasive procedure. There are limits to what can be achieved with fillers, and the patient should be informed before undergoing the procedure given the cost (see Chapter 36 ).
Preoperative planning
Each region of the face is evaluated, and the degree of asymmetry is assessed. 2D photography is the standard to document facial form and to initiate facial analysis. 3D photographic imaging is a very useful tool to document facial asymmetry and to illustrate the asymmetry to the patient. When used to simulate facial change, simulation software can approximate the volume of soft tissue that is required to achieve the desired result.
CT enables the surgeon to see a 3D representation of the face and to determine the contribution of bone and soft tissue to a region of asymmetry. Historically, VSP was used only for complex cases. However, the recent assimilation and scale of VSP into the practice of maxillofacial surgery has allowed it to become a cost-efficient tool for surgical precision in restoring symmetry. When planning osteotomies, VSP is very helpful to determine accurate movements and to fabricate custom implants that can be based on the dimensions of the “normal” side. Even if osteotomies are not being planned, the VSP session can elucidate subtle anatomic findings that contribute to facial asymmetry but may not be clinically obvious to the surgeon without the use of VSP. An in-depth discussion of VSP is found in Chapter 17 .
Primary operative approach
The treatment canons associated with the etiologies of facial asymmetry are well established.
Hemifacial microsomia: This typically involves the upper and lower jaws and is associated with dental midline deviation and an occlusal cant. The only operation that can correct the midline deviation and the occlusal cant is bimaxillary orthognathic surgery. Frequently, the chin will be deviated from the facial midline after repositioning of the jaws, and this will require centering genioplasty. Associated malar or mandibular angle hypoplasia may be treated with bone grafting. Autologous fat grafting is also a useful tool as an adjunct to bone grafting or alone in restoring facial symmetry.
Unilateral condylar hyperactivity: Hyperactive condylar activity typically results in mandibular hyperplasia growing at a rate faster than the maxilla can accommodate. The result is malocclusion, requiring either one or two jaw surgeries to correct it. Centering genioplasty may also be required to restore mandibular symmetry. Because this anomaly is related to condylar hyperactivity, there is no associated soft tissue abnormality unless the condition occurred in childhood and the skeletal anomaly affected the development of functional matrix soft tissue. It is important to ensure cessation of condylar growth before initiating treatment. If treatment is required before the condyle “burns out,” a condylar shave can be performed to surgically remove the growth center of the condyle and thus stop growth.
Traumatic condylar injury: If an injury occurs in the condyle, normal condylar growth can be stunted, resulting in an underdeveloped jaw on the affected side. Depending on age at injury, the trauma may result in an appearance very similar to hemifacial microsomia, with an occlusal cant and midline deviation. Treatment is similar to that for hemifacial microsomia—bimaxillary orthognathic surgery with genioplasty and fat grafting, if indicated.
Parry-Romberg disease: This process affects patients later in life and is associated with primarily soft tissue atrophy, but in severe cases, skeletal trophy occurs as well. Successful treatment of these patients has included microvascular free flaps, but these flaps have largely been replaced by the use of autologous fat grafting due to the excellent results and decreased morbidity.
Idiopathic facial asymmetry: These patients exhibit varying degrees of facial asymmetry without any known etiology. The asymmetry usually is not associated with an occlusal abnormality and is a combination of skeletal and soft tissue components. It is up to the surgeon to determine the optimal approach to treatment based on the physical examination and the patient’s goals.
Alternative approaches
The surgeon’s armamentarium should include a large number of procedures to be able to address each of the components of facial asymmetry involved—skeletal, soft tissue, and functional facial elements. All of the tools at the surgeon’s disposal are discussed thoroughly in separate chapters. The following serves as a brief description of each tool.
Osteotomies: An osteotomy is indicated to make a major structural change in the skeleton. The primary osteotomies employed in the facial skeleton are of the maxilla, the mandible, and the chin. Less frequently, orbital or malar osteotomies are indicated (see Chapter 20 , Chapter 21 , Chapter 22 , 27 , and 33 ).
Bone grafts: Bone grafts are associated with donor site morbidity and undergo variable resorption. However, autologous tissue establishes a blood supply and, over time, is associated with fewer complications compared with alloplastic materials (see Chapter 11 ).
Alloplastic implants: The use of implants avoids donor site morbidity, and once placed, their size and shape remain stable. Because they are foreign bodies, they are susceptible to infection and can cause resorption of underlying bone (see Chapters 12 , 24 , and 26 ).
Free flaps: A useful approach to a large tissue defect is a microvascular free flap. Parascapular flaps are useful in severe facial asymmetry to restore large soft tissue deficits (see Chapter 39 ).
Fat grafts: Structural fat grafting has been a very useful tool to restore large volume deficiencies as well as perfect the soft tissue contour after underlying skeletal change (see Chapter 35 ).
Dermal fillers: Fillers can be used for minor changes in facial form. They allow very precise control of soft tissues and can be reversed, if necessary. The primary disadvantage of dermal fillers is their cost and the fact that the result they create is only temporary (see Chapter 36 ).
Optimizing outcomes
Recent advances in imaging, treatment planning, products, and techniques have given the surgeon a myriad of tools to create structural changes in the human face. There is not one correct solution for every condition. The surgeon must weigh the patient’s health, goals, recovery, and expectations. The surgeon must also be realistic and create a treatment plan with which he or she is comfortable. The described techniques can be applied in a multitude of combinations to treat a patient with facial asymmetry.
Surgical technique
Each of the surgical techniques mentioned in this chapter have been thoroughly described in their respective chapters elsewhere in this text. The clinical cases that follow illustrate the application of various techniques to meet the patient’s goals.
Case 1
In a patient with mild craniofacial microsomia and minimal occlusal cant, facial asymmetry may be managed with the use of an alloplastic implant and structural fat grafting if the patient is not inclined to undergo orthognathic surgery. If the entire asymmetry is corrected with an implant alone, symmetry may be compromised. The hypoplasia involves both hard and soft tissues and thus is ideally corrected with both components. Fig. 41.2 shows a patient whose face was reconstructed only with an alloplastic implant; although skeletal symmetry was achieved, facial symmetry is suboptimal. Our preferred approach in these cases is to select an alloplastic implant slightly smaller than the ideal and to employ structural fat grafting over the area. Theoretically, an implant matched to the opposite side should help achieve a favorable result with fat grafting. However, it is our experience that it may be difficult to predict how the hypoplastic soft tissue will drape over the implant. Using a slightly smaller implant gives the surgeon more freedom in creating ideal symmetry with fat grafts and also produces a supple, natural-feeling result.