Key Words
acute compartment syndrome, fasciotomy
Synopsis
Acute compartment syndrome is a surgical emergency with diverse etiologies. Acute compartment syndrome is classically described clinically with “the 6 P’s”: pain, pallor, paresthesia, paresis, poikilothermia, and pulselessness. Clinical examination along with judgment is the gold standard for diagnosis; however, suspicion of compartment syndrome can be confirmed by measurement of intracompartmental pressures. The definitive treatment of acute compartment syndrome is early fasciotomy. Delayed or inadequate treatment can lead to poor outcomes, including limb amputation, poor motor and sensory nerve function, debilitating contractures, or even multi-organ failure and death. In this chapter, the pathophysiology, etiologies, diagnosis, and treatment of upper-extremity compartment syndrome are reviewed.
Clinical Problem
Compartment syndrome is a surgical emergency with many etiologies that share a distinct clinical picture. In its most basic definition, acute compartment syndrome (ACS) results when there is increased pressure within a fascia-enclosed tissue space that compromises the blood flow to the tissues inside of the compartment. ACS can commonly arise from any number of major traumas (especially those with crush mechanisms), fractures, and burn/electrical injuries, as well as post-surgical revascularization of ischemic limbs. Among other etiologies, it can also be a sequela of internal space-occupying lesions such as tumors, hematomas, abscesses, and extravasation of intravenous fluids or contrast, as well as external causes such as casts and dressings that are placed too tightly. A systematic review of forearm compartment syndrome cases found that the most common cause of ACS of the forearm in children was a supracondylar fracture, whereas in adults the most common cause was distal radius fracture.
Physiologically, a capillary perfusion pressure of approximately 25 mm Hg maintains the oxygen level needed for normal tissue metabolism, which is above the normal interstitial tissue pressure of 4 to 6 mm Hg. The tissue perfusion pressure equals capillary perfusion pressure minus interstitial pressure. Interstitial tissue pressures above 30 mm Hg overwhelm capillary perfusion pressure, causing progressive blood vessel collapse. This, in turn, leads to compromised tissue perfusion pressure, a local tissue oxygen deficit, and an ischemic insult. Early compartment fasciotomy decompression allows tissues under excess pressure to expand, leading to a drop in interstitial pressure, restoration of local blood flow, clearing of toxic anaerobic metabolites, and return of normal cellular function.
Clinically, patients will present with varying symptoms and degrees of severity depending on the etiology of the compartment syndrome. The following section will further elaborate on the physical examination findings to diagnose ACS.
Pre-Operative Management
Physical Examination and Key Anatomy
Given that diagnosis of ACS is best made with a high index of clinical suspicion, physical examination is paramount. Classically, the presentation of ACS is described with “the 6 P’s”: pain, pallor, paresis, paresthesia, pulselessness, and poikilothermia. Pain is considered to be the main clinical symptom of a developing ACS. Specifically, pain out of proportion to examination, pain unresponsive to analgesics, palpable tightness in the affected compartment, and pain worsening with passive stretching of the muscles in the affected compartment are the most accurate signs for early diagnosis. Paresthesia, paresis, and especially pulselessness are usually late signs of an ACS and may indicate potentially irreversible tissue damage. In children or adults with an altered level of consciousness, pain may not be readily appreciated, and the other signs as well as objective measurements play a larger role in making the correct diagnosis. Fullness or distention of the affected compartment from a clinically relevant mechanism in the absence of other “6 P” signs/symptoms should alert providers to the risk of ACS, and these cases warrant close observation with frequent serial re-examinations. In all cases, the mechanism of insult and the overall clinical picture must be accounted for in the physician’s index of suspicion.
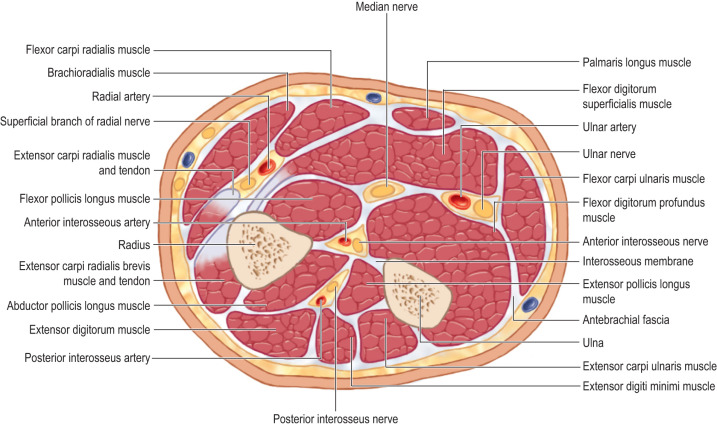
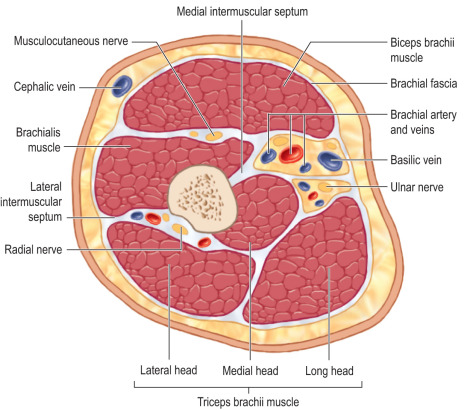
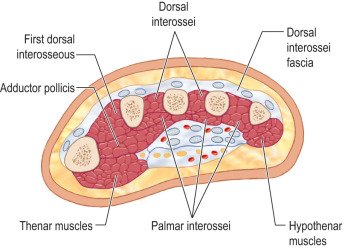
Understanding the relevant anatomy is important to ensure safe, appropriate treatment. The upper extremity is a common site for compartment syndrome with approximately three-fourths of upper-extremity compartment syndromes occurring in the forearm compartments. The forearm comprises three compartments: volar, dorsal, and a mobile wad. The volar compartment contains the superficial and deep flexors. The dorsal compartment contains all the extensors. The mobile wad is composed of extensor carpi radialis longus (ECRL), extensor carpi radialis brevis (ECRB), and brachioradialis (BR) muscles ( Fig. 6.1.1 ). The upper arm consists of three compartments: anterior, posterior, and the deltoid compartment. The anterior compartment comprises the biceps (long and short heads), brachialis, and coracobrachialis. The posterior compartment is composed of the three heads (lateral, medial, and long) of the triceps muscle ( Fig. 6.1.2 ). The hand contains 10 compartments: 4 dorsal interossei, 3 palmar interossei, one thenar musculature, one hypothenar musculature, and one adductor pollicis compartment ( Fig. 6.1.3 ). The upper-extremity compartments with their corresponding contents, blood supply, and innervation are outlined in Table 6.1.1 .
| Compartment | Muscle | Artery | Nerve | |
|---|---|---|---|---|
| Arm | Anterior | Biceps, brachialis, coracobrachialis | Brachial | Musculocutaneous |
| Posterior | Triceps | Profunda brachii | Radial | |
| Deltoid | Deltoid | — | Axillary | |
| Forearm | Volar | Radial and ulnar | Median, ulnar, and anterior interosseous | |
| Superficial | Pronator teres, flexor carpi radialis, palmaris longus, flexor digitorum superficialis, flexor carpi ulnaris | |||
| Deep | Flexor pollicis longus, flexor digitorum profundus, pronator quadratus | |||
| Dorsal | Posterior interosseous | Posterior interosseous | ||
| Superficial | Extensor digitorum communis, extensor digiti minimi, extensor carpi ulnaris | |||
| Deep | Abductor pollicis longus, extensor pollicis brevis, extensor pollicis longus, extensor indicis proprius, supinator | |||
| Mobile wad | Brachioradialis, extensor carpi radialis longus, extensor carpi radialis brevis | — | Radial | |
| Hand | Thenar | Abductor pollicis brevis, opponens pollicis, flexor pollicis brevis | — | Ulnar |
| Hypothenar | Abductor digiti minimi, opponens digiti minimi, flexor digiti minimi | |||
| Adductor | Adductor pollicis | — | Ulnar | |
| Interosseous | 4 dorsal and 3 palmar interosseous muscles | — | Ulnar | |
| Carpal tunnel | Flexor digitorum profundus, flexor digitorum superficialis, flexor pollicis longus | — | Median | |
| Digit | Digital | Digital |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree