Combination therapies capitalize on and allow for synergistic benefits from different treatment modalities.
Platelet-rich plasma is easily combined with microneedling or laser resurfacing, leading to more effective results and shorter downtime.
Microneedling, through its simple and rapid mechanical penetration of the stratum corneum, holds promise for transdermal delivery of drugs.
The increased strength of combination therapies should be routinely weighed against possible increases in adverse events.
9.1 PRP with Laser Resurfacing
Platelet-rich plasma (PRP) is an autologous solution and concentrated reservoir of numerous growth factors, including platelet-derived growth factor (PDGF), vascular endothelial growth factor (VEGF), transforming growth factor (TGF), epidermal growth factor (EGF), and insulin-like growth factor (IGF). 1 Isolated from whole blood after venipuncture, PRP can be easily prepared in the office setting just prior to a planned procedure. Peripheral whole blood undergoes centrifugation to separate the desired platelet and plasma (also known as PRP) components, with a resultant 5 mL of PRP typically concentrated to contain a platelet count of at least 1,000,000/µL (note that blood draw volume, preparation techniques, and final concentration vary by system and can substantially impact the final concentration and composition; Chapter 1). 2 Importantly, the facility of PRP procurement and delivery allows it to be readily used in conjunction with other treatment modalities.
One important application of PRP is with laser resurfacing procedures. This combination applies the regenerative properties of PRP to the microthermal treatment zones created during resurfacing. Several studies have compared the use of laser resurfacing alone versus in combination with PRP ( ▶ Table 9.1).
Authors | Study design | N | Mean age, year (range) | Comparison | Treatment protocol | Results | Adverse effects |
Shin et al. (2012) | Facial rejuvenation; control group and experimental group | 22 | 43.7 (30–56) | 1,550-nm fractional erbium glass laser + topical PRP vs. 1,550-nm fractional erbium glass laser alone | Three treatments at 4-week intervals | Non-ablative fractional laser + topical PRP led to scar improvement in 73% of patients vs. 45% with laser alone. Combination therapy also led to larger increases in collagen and fibroblasts | No long-term adverse effects |
Lee et al. (2011) | Acne scars; split-face design | 14 | 28.1 (21–38) | Fractional CO2 laser + intradermal PRP vs. fractional CO2 laser + intradermal NS | Two treatments at 1-month interval | CO2 laser + intradermal PRP led to greater scar improvement and faster resolution of laser-damaged skin vs. CO2 laser + intradermal NS | No long-term adverse effects |
Na et al. (2011) | Healthy skin on the bilateral inner arms; split-body design | 25 | Not listed | Fractional CO2 laser + topical PRP vs. fractional CO2 laser + topical NS | One treatment | CO2 laser + topical PRP led to reduced erythema and trasnspeidermal water loss in the recovery period vs. CO2 laser + topical NS. PRP treatment was also associated with thicker collagen bundles at 1-month follow-up | No long-term adverse effect |
Gawdat et al. (2014) | Acne scars; two groups, each with split-face design | 30 | 24.8 (19–35) | Fractional CO2 laser + topical PRP vs. fractional CO2 laser + intradermal PRP vs. fractional CO2 laser + intradermal NS | Three treatments at 1-month intervals | A grade of >75% improvement was seen in 67% of areas treated by CO2 laser + intradermal PRP vs. 60% of areas treated by CO2 laser + intradermal PRP vs. 27% of areas treated by CO2 laser + intradermal NS. Topical PRP application yielded reduced pain vs. intradermal | PIH on the sides of two patients treated with CO2 laser + intradermal NS |
Abbreviations: PRP, platelet-rich plasma; CO2, carbon dioxide; NS, normal saline; PIH, postinflammatory hyperpigmentation. | |||||||
Shin et al 3 examined the value of dual therapy in 22 patients undergoing facial rejuvenation. Half of the patients received topical application of PRP (unspecified concentration) combined with fractional laser resurfacing, while the other half received fractional laser resurfacing alone. Subjects underwent three treatments with a non-ablative 1,550-nm fractional erbium glass laser, each separated by 4 weeks. In the combination treatment group, topical PRP was applied under occlusion for 20 minutes immediately after laser therapy. Patient-reported improvements in skin texture, elasticity, and fine wrinkles were all higher in the combination treatment group. Blinded evaluators noted clinical improvement in 73% of patients in the combination group versus 45% in the monotherapy group, although the difference between groups was not statistically significant. Biopsies performed before and 1 month after the final treatment showed that combination therapy lead to significantly greater increases in the length of the dermal–epidermal junction, the volume of collagen, and the number of fibroblasts (p < 0.05). There were no significant differences in adverse events between the two groups.
Lee et al 4 investigated the combination of PRP with ablative carbon dioxide (CO2) fractional resurfacing in the treatment of acne scars. In a split-face study of 14 patients, all subjects first received full-face treatment with the fractional CO2 laser, then intradermal injections of PRP (unspecified concentration) on one side of the face versus intradermal injections of saline on the other side. The procedure was repeated 1 month later for a total of two treatment sessions spaced 1 month apart. Results confirmed an expedited recovery time after combination therapy compared to the saline control, with the mean duration of posttreatment erythema shortened by 1.8 days, duration of edema shortened by 1 day, and the duration of crusting shortened by 0.9 days (all p < 0.05 between treatment groups). The investigators also graded patients’ clinical improvement according to a quartile scale from 0 (no improvement) to 4 (>75% improvement). Four months following the second treatment session, the sides of the face receiving combination therapy showed greater improvement in acne scars than the control (mean quartile improvement of 2.7 vs. 2.3; p = 0.03). Similarly, Na et al 5 found greater wound healing and reduced transient adverse effects when fractional CO2 resurfacing was followed by the application of PRP. In this study, thicker collagen bundles were also noted on histological examination of PRP-treated sides relative to controls.
Expanding on such results, Gawdat et al 6 compared differential effects seen with topical versus intradermal PRP in conjunction with ablative resurfacing for management of acne scars. Thirty subjects were enrolled in the split-face study and separated into two groups. In the first group, one side of the face underwent fractional CO2 laser resurfacing followed by intradermal injections of PRP (unspecified concentration), and the other received laser treatment followed by intradermal injections of saline. In the second group, one side of the face underwent fractional CO2 laser resurfacing followed by intradermal injections of PRP; the other side received laser treatments followed by topical PRP application under occlusion for 15 minutes. Patients completed three sessions at monthly intervals. Results at 3 months after the final session showed that the combination of laser with PRP (regardless of whether topical or intradermal) yielded greater scar improvement than the laser control group. In addition, adverse events such as erythema, edema, and crusting resolved more quickly on the combination-treated areas. The total downtime was statistically significantly shorter in the combined topical PRP and laser group (2.8 days) and the intradermal PRP and laser group (2.3 days) relative to the laser control group (4.4 days; p = 0.02). Notably, there were no significant differences between the intradermal and topical applications of PRP, with the lone exception of reduced pain scores in the topical PRP group. These findings support the notion that when used concurrently with laser resurfacing, the topical route of PRP administration allows for maximized patient comfort without compromising efficacy.
9.2 Platelet-Rich Plasma with Ultrasound
Ultrasound is another energy-based modality employed to increase the penetration of PRP. In one study of striae distensae, Suh et al 7 combined topical PRP (4.5 times concentration) with ultrasound after the application of fractional radiofrequency. Eighteen patients were treated every 2 weeks for four sessions. Two months after the final treatment, the mean width of the widest striae decreased from 0.75 to 0.27 mm. About 70% of patients reported being “very satisfied” or “extremely satisfied” with the degree of improvement. Lack of control groups receiving radiofrequency, PRP plus ultrasound, or no therapy was a major limitation to this study; however, results are encouraging and warrant further investigation, especially considering striae are a common yet challenging to treat condition.
9.3 Platelet-Rich Plasma with Microneedling
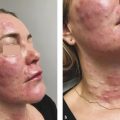
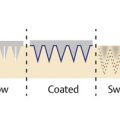
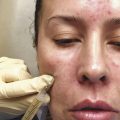
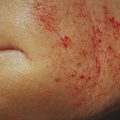
Microneedling therapy uses small gauge needles to injury deliberately and mechanically the epidermis and dermis and thereby, encourage skin rejuvenation ( ▶ Fig. 9.1a–c). Puncture wounds created by microneedles promote growth factor release and wound healing cascades. Histological examinations following microneedling therapy demonstrate increases in collagen and elastic fiber formation, leading to a thicker dermis with normal-appearing architecture rather than scar-type dermal changes that occur after more extensive trauma. 8, 9 The clinical applications of microneedling are wide ranging, with the largest body of literature in skin rejuvenation and the treatment of acne scars ( ▶ Fig. 9.2a–c and ▶ Fig. 9.3a, b) (Chapter 6). 10, 11, 12, 13 In addition, there are encouraging results observed in the management of hypertrophic burn scars and melasma. 14, 15, 16 The possible indications for microneedling continue to expand. These investigational applications include androgenic alopecia, hyperhidrosis, striae rubra, and transdermal delivery of drugs ( ▶ Fig. 9.4a,b and ▶ Fig. 9.5, ▶ Fig. 9.6, ▶ Fig. 9.7, ▶ Fig. 9.8). 17, 18, 19, 20
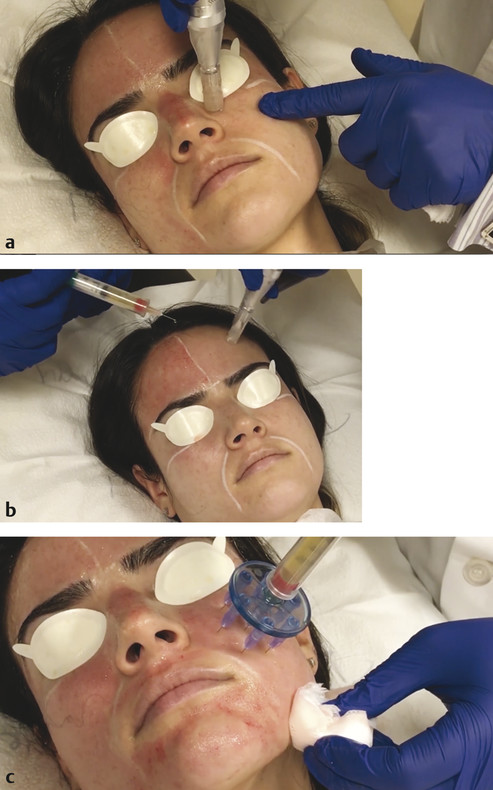
Fig. 9.1 Microneedling with PRP. (a) The microneedling device is first used to create minute puncture wounds. (b) Topical PRP is then applied to the skin using a syringe. (c) Alternatively, PRP can be injected intradermally following microneedling. (© 2017 Cutis (https://www.mdedge.com/cutis) and Gary Goldenberg.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree