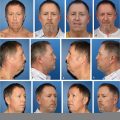
In modern clinical practice, PRIVATE AESTHETIC CENTER by PUNIN relies on a simple idea: understanding how the skin responds to factors such as environmental stress, UV exposure, and biological aging. Based on this scientific foundation, specialists develop structured programs for skin recovery by combining advanced aesthetic medicine with proven modalities like biorevitalization and injection-based hydration. These programs are designed to reinforce epidermal integrity and help the skin return to a resilient, functional baseline.
What’s interesting to note is that the global market for this practice is growing at a rate that catches the eye. According to Strategic Market Research, the sector was valued at approximately USD 9.7 billion in 2024 and is projected to reach a whooping USD 16.4 billion by 2030. That’s an 8.5% CAGR growth. What does that translate to? A clear sign that demand for clinical treatments is becoming mainstream around the globe.
Molecular Mechanisms of Skin Barrier Restoration
Let’s start with the skin barrier. The scientific way of saying it is that it’s a dynamic biological system led by lipid architecture, protein scaffolding, and tightly regulated hydration gradients. When this system is compromised through exogenous factors such as chronic sun exposure or age-related lipid depletion, the result is tissue homeostasis is disrupted, and the skin loses its ability to self-regulate effectively. Clinical protocols targeting restoration must therefore address the molecular disruptions that allow them to occur, not just surface symptoms.
Let’s start with the skin barrier. Scientifically, it is a dynamic biological system shaped by lipid architecture, protein scaffolding, and tightly regulated hydration gradients. When this system is compromised by exogenous factors such as chronic sun exposure or age-related lipid depletion, tissue homeostasis is disrupted and the skin loses its ability to self-regulate effectively. This is why clinical protocols focused on restoration must address the molecular mechanisms of dermal recovery, rather than only visible surface symptoms.
Two of the most significant mechanisms in barrier repair are:
- The prevention of transepidermal water loss.
- The enzymatic regulation of epidermal lipid synthesis.
Both are measurable, treatable, and key to any evidence-based skin recovery protocol.
Preventing Transepidermal Water Loss
Transepidermal water loss (TEWL) is defined as the rate at which water passively diffuses through the stratum corneum and evaporates from the skin surface. In healthy skin, a tightly organized lamellar lipid matrix, composed primarily of ceramides, free fatty acids, and cholesterol, keeps TEWL at clinically low levels. When barrier function deteriorates, TEWL rises, creating a diagnostic marker that clinicians use to assess dermal integrity and monitor the effectiveness of treatment protocols.
Elevated TEWL is associated with a range of conditions such as:
- Atopic dermatitis
- Post-procedure sensitivity
- Photoaging
Clinically validated interventions, including ceramide-enriched topicals, occlusive barrier creams, and prescription emollients, have showcased the ability to reduce TEWL and restore the stratum corneum’s functional architecture. According to a 2026 review, TEWL is now recognized as a critical objective parameter for measuring clinical wound healing endpoints, particularly for evaluating functional barrier restoration.
Role of Niacinamide in Lipid Synthesis
Niacinamide (vitamin B3) has risen to prominence as one of the most evidence-backed active ingredients in barrier-repair clinical aesthetics. Its mechanism is enzymatic: niacinamide replenishes NAD⁺/NADP⁺ pools in keratinocytes and upregulates serine palmitoyltransferase (SPT), the rate-limiting enzyme in sphingolipid synthesis. The result is measurable upregulation of ceramide, free fatty acid, and cholesterol production within the stratum corneum, directly supporting barrier restoration from within.
In a landmark study published in Skin Pharmacology and Applied Skin Physiology, topical nicotinamide application increased ceramide synthesis alongside free fatty acid production by 2.3-fold and cholesterol synthesis by 1.5-fold. In vivo, this translated to reduced TEWL in subjects with dry skin, a clinically meaningful finding for protocols targeting oxidative damage and chronic barrier insufficiency. When paired with ceramide-enriched formulations, niacinamide delivers additive gains in hydration, irritation tolerance, and long-term epidermal lipid density.
Advanced Strategies for Managing Oxidative Stress
One of the main contributors to the aging of the skin and weakening of the skin’s barrier is oxidative stress. Oxidative stress occurs when the reactive oxygen species (ROS), which are produced by UV exposure, pollution, and metabolism, damage the cell membranes, break down collagen proteins, and disrupt cell repair processes. In the absence of sufficient antioxidants and medical intervention, the gradual build-up of ROS damage causes changes to the skin’s connective tissue, which is seen as uneven skin texture, dark spots, and skin sagging.
Most of the clinical protocols treating oxidative stress use a combination of topical antioxidant treatments (vitamins C and E resveratrol glutathione) and the procedures that can lead the skin’s collagen production and vascular support to a natural level. The idea is to interrupt the chain reaction of ROS by various ways such as eliminating free radicals on the skin surface and enhancing the cell’s natural recovery mechanism.
Biorevitalization for Intense Dermal Hydration
Biorevitalization is about the intradermal or subdermal introduction of bioactive compounds, usually hyaluronic acid (HA), amino acids, vitamins, and minerals, intended to replenish physiological hydration and maintain tissue homeostasis deep down. Whilst skin surface moisturizers only act superficially, biorevitalization returns to the dermis, the layer where the HA fragments latch onto water molecules forming a hydration reservoir that cannot be matched by surface treatments.
Clinical evidence supports its efficacy. A systematic review published in Aesthetic Surgery Journal found that more than 80% of participants across multiple injectable HA studies showed significant improvement in skin hydration, elasticity, and overall quality following microinjection protocols. In one randomized study, intradermal HA-glycerol injections significantly increased skin hydration for up to 16 weeks, with hydration effects lasting up to 9 months after the final session, particularly in subjects with dry or environmentally stressed skin.
Clinical Approaches to Photoaging Management
Photoaging management is one of the most active areas in clinical aesthetics. It results from the cumulative damage in the dermis caused by chronic exposure to the ultraviolet rays of the sun. Overall, intrinsic aging happens to a large extent due to the genes, whereas photoaging leads to mechanisms that rapidly break down collagen, cause higher levels of matrix metalloproteinase (MMP), and make pigment irregularities more pronounced through oxidative pathways. From a clinical point of view, managing photoaging needs several different methods combined: dealing with the discoloration of the skin, replenishing the volume of skin and enhancing the repair of cells at the fibroblast level.
Most protocols share the feature of mixing fractional laser resurfacing, chemical peeling, and injectable treatments. This multisite approach targets various layers of photoaged skin simultaneously. For example, energy-based devices promote neocollagenesis in the reticular dermis, while topical retinoids act on the epidermal level to normalize keratinocyte differentiation and increase cell turnover. Multiple controlled clinical studies have shown that these combined protocols noticeably improve skin texture, tone, and elasticity.
The Efficacy of Injectable Protocols in Aesthetic Medicine
Injectable treatments play a major role in evidence-led skin healing in clinical aesthetics. They include dermal fillers, skin boosters, polynucleotides (PDRN), and platelet-rich plasma (PRP). Every method focuses on a different part however they all have one fundamental goal: to restore the natural conditions of the skin that enable it to upkeep and repair itself. The table below shows a clinical summary of the most recognized injectable methods and their key mechanisms:
| Injectable Protocol | Primary Mechanism | Key Benefit | Typical Sessions |
| Hyaluronic Acid Skin Boosters | Intradermal hydration depot | Injectable hydration, tissue homeostasis | 3 sessions, 4 weeks apart |
| Polynucleotides (PDRN) | DNA repair, fibroblast stimulation | Cellular repair, collagen synthesis | 4–6 sessions |
| Platelet-Rich Plasma (PRP) | Growth factor cascade activation | Dermal regeneration, barrier restoration | 3–4 sessions |
| Profhilo (HA remodelling) | Bioremodelling of dermis and epidermis | Epidermal integrity, skin laxity | 2 sessions, 4 weeks apart |
| Mesotherapy (vitamin cocktails) | Micronutrient delivery to dermis | Oxidative damage recovery, radiance | Monthly maintenance |
Injectable hydration is not just about skin aesthetics; it is a therapeutic rationale. As the dermis is depleted of HA with age or environmental damage, it suffers loss of structural support and a decrease in hydration capacity at the same time. This double deficit cannot be altogether compensated by topical products alone.
Injectable setups replenish both, providing instant hydration and at the same time activating fibroblasts that contribute to the molecular recovery process over time. The injection procedures combined with skin barrier repair via topical application and skin molecular diagnostics form the perfect model of clinical skin restoration that is available today. This approach is gaining popularity as the global market for these products and services is growing at a pace of almost 9% per year.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree