Key Words
cerebral palsy, thumb-in-palm deformity, EPL tendon rerouting, wrist flexion contracture, adductor release
Synopsis
Cerebral palsy is a disorder of the central nervous system affecting body movement and muscle coordination. It is the most common of all childhood disabilities, affecting roughly 2 to 3 children out of every 1000. Cerebral palsy is found all over the world, including in developing countries. A spectrum of spastic upper-extremity disorders is associated with pediatric cerebral palsy. One such condition is a thumb-in-palm deformity, caused by muscle imbalance and resulting in an impaired ability to grasp objects. Surgical treatment aims to strengthen underactive muscles while weakening those that are overactive. One of the primary surgical treatment options for children with a thumb-in-palm deformity is extensor pollicis longus rerouting and adductor release. This chapter will examine the presentation of thumb-in-palm deformity and give step-by-step details of the treatment option described earlier. Further, flexor carpi ulnaris transfer to extensor carpi radialis brevis will be discussed as an adjunct treatment for associated wrist flexion deformity. Post-operative care and management of common complications also will be reviewed.
Clinical Problem
Cerebral palsy (CP) in children is caused by abnormal brain development or brain damage. Congenital CP is defined as CP secondary to brain injury before the time of birth, often the result of brain hypoxia. CP affects roughly 2 to 3 children out of every 1000. The prevalence of CP increases to 100 per 1000 live births in low-birth-weight babies. The incidence is higher in developing countries, where prepartum monitoring and obstetrical care resources are not as available. Children present with poor muscle control, poor muscle tone, and subsequent impaired balance and diminished posture. Other associated impairments include behavioral and intellectual disability as well as sensory and visual disability. Some children experience more significant muscle contractures and are confined to a wheelchair. Additionally, many CP patients have poor bowel and bladder control.
The clinical presentation of CP can be classified using the Surveillance of Cerebral Palsy in Europe (SCPE) system. SCPE divides CP into three major categories: spastic, dyskinetic, and ataxic. Spastic CP is further subdivided into unilateral and bilateral limb involvement. Patients are then classified as hemiplegic, diplegic, or quadriplegic.
The potential diagnosis of CP is generally done before 2 years of age and is based on the aforementioned clinical assessment tool without relying on neuroimaging or laboratory tests. However, imaging modalities can be used to confirm the diagnosis; these include MRI and cranial ultrasound of the brain. MRI findings consistent with CP include periventricular leukomalacia and post-hemorrhagic porencephaly. On ultrasound, periventricular echolucency and ventricular enlargement often correlate to a diagnosis of CP. Laboratory tests, including TSH, ammonia levels, lactate, pyruvate, and chromosomal analysis, can rule out other causes with similar clinical presentations. These tests may or may not be available in the developing world.
Rehabilitation for children with CP requires a team approach. The involvement of physical and occupational therapists is imperative. Additionally, many children with CP have auditory and visual disabilities. Auditory therapists, otolaryngologists, speech therapists, and optometrists often contribute to the care and rehabilitation of the patient.
Rather than review a comprehensive list of all the possible reconstructive procedures that may be performed in patients with CP, this chapter will focus on a few that commonly may be performed in settings around the world with limited resources. Thumb-in-palm deformity is a common upper-extremity finding in CP. The condition is the result of spasticity of the thumb adductor and flexor muscles. Enhanced thumb mobility is achievable with the use of muscle releases and tendon transfers. A wrist flexion deformity is commonly in association with thumb-in-palm deformity. It is caused by hyperactive wrist flexors and weak wrist extensors. Flexor carpi ulnaris (FCU) to extensor carpi radialis brevis (ECRB) tendon transfer, or FCU-to-ECRB, can improve wrist mobility and overall function of the spastic hand.
Pre-Operative Management
Determination of surgical candidacy is based primarily on the child having volitional control of the hand. Surgical intervention is not recommended in a child with a functionally discounted limb. Patient age should also be considered in the pre-operative assessment. Many surgeons maintain that early intervention in children is ideal because it minimizes the effects of joint contracture. This in turn may improve physical therapy and overall surgical prognosis. The literature has not established an optimal age for surgical intervention. In developing countries, patients may present later with fixed contractures. However, it is widely accepted that children should not undergo surgery until they are old enough to understand and participate in post-operative rehabilitation. Another concern is deformity recurrence, a common complication in growing children. It occurs most prevalently in patients between the ages of 7 and 10 and often requires secondary surgery.
Physical examination of the child should include size measurements of the arm and hand, documentation of passive and active ranges of motion for all upper-extremity joints, strength testing, sensibility testing, and specific functional capacity with regard to grasp and pinch. The Manual Ability Classification System (MACS), detailed in Table 5.9.1 , is a well-accepted way to define the functional capacity of children with CP. MACS divides CP children into five primary levels. Level I children are able to perform manual tasks and handle objects easily, while Level V children have poor manual ability and are completely dependent. MACS serves as a useful communication tool between medical care teams. The system is also useful for goal setting for patient rehabilitation.
| MACS Level | |
|---|---|
| I | Handles objects easily and successfully. |
| II | Handles most objects with somewhat reduced quality and/or speed of achievement. |
| III | Handles objects with difficulty; needs help to prepare and/or modify activities. |
| IV | Handles a limited selection of easily managed objects in adapted situations. |
| V | Does not handle objects and has severely limited ability to perform even simple actions. |
* From www.macs.nu .
Common CP Problems
Thumb-in-Palm Deformity
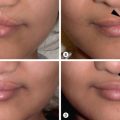
Thumb-in-palm deformity is the result of complex anatomical imbalances. It can include muscle contractures and first web space skin contractures as well as ligamentous and capsular instability. The designation of a thumb-in-palm deformity specifically refers to adduction-flexion of the metacarpal and proximal phalanges of the thumb, and extension or hyperextension of the interphalangeal (IP) joint of the thumb during digital extension.
To determine whether a thumb-in-palm deformity is present, the surgeon must maximally flex the wrist, at which point the thumb will adduct and rest in the palm with limited ability to actively extend. Due to the normal route of the extensor pollicis longus (EPL), ulnar to Lister’s tubercle, a thumb adduction deformity may be worsened by the pull of the EPL. Therefore EPL rerouting can reduce symptoms.
Anatomical localization of the specific pathologies involved is essential to the selection of the most appropriate surgical intervention. Thumb-in-palm deformity is classified into three major types: intrinsic deformity (type 1), extrinsic deformity (type 2), and combined deformity (type 3). Intrinsic deformity is due to spasticity of the intrinsic thumb muscles, causing adduction of the thumb metacarpal, flexion of the metacarpophalangeal (MCP) joint, and extension of the IP joint. Extrinsic deformity has a lesser degree of metacarpal adduction, and is characterized by spasticity of the extrinsic flexor pollicis longus, causing flexion of the MCP and IP joints. Combined deformity is adduction of the first metacarpal with MCP joint hyperextension. Surgical correction seeks to weaken the deforming force while strengthening opposing forces to improve joint stability and maximize function.
Wrist Hyperflexion
There is an association between thumb-in-palm deformity and concomitant wrist hyperextension in children with CP. If finger extension relies on wrist flexion and finger flexion relies on wrist extension, this is called a tenodesis grasp. Special attention should be directed toward observing this in a potential surgical patient. The surgeon should confirm that surgical correction of wrist hyperflexion will not impair that patient’s ability to extend the fingers.
Zancolli et al. described three primary patterns of hand function, classified into four groups. Pattern III hand function is associated with poor surgical prognosis ( Table 5.9.2 ). Patients who demonstrate pattern I and II have a better chance of favorable surgical outcome.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree