Physiologic differences
• Children seem more susceptible to symptomatic bronchospasm than adults
• Young infants may have a less mature renal concentrating ability than adults
• Young children seem to handle fluid overload poorly in comparison to adults
• Children resuscitated with hypotonic fluid may develop cerebral edema and seizures
• Young children have a higher metabolic rate and energy requirements per unit body weight and will lose lean body mass more rapidly if fasted
• Young children have a higher surface area to body weight ratio which makes hypothermia more likely to occur
• Young children may form hypertrophic scar more readily than older adults
Anatomic differences
• Child’s upper airway is narrower and therefore more susceptible to occlusion by soft-tissue swelling
• Child’s trachea is shorter and therefore more susceptible to mainstem intubation
• Young children have thinner skin than older children and adults which makes burn healing and donor harvesting more problematic
• Young children have smaller blood vessels than adults which makes vascular access more challenging
• Young children grow, often outgrow, with an initially good surgical result and require revision
Psychologic differences
• Pain and anxiety assessment is more difficult in children than adults
• Family and school issues have a major impact on physical and emotional recovery in children
• Major changes in psychologic needs with developmental stage are predictable
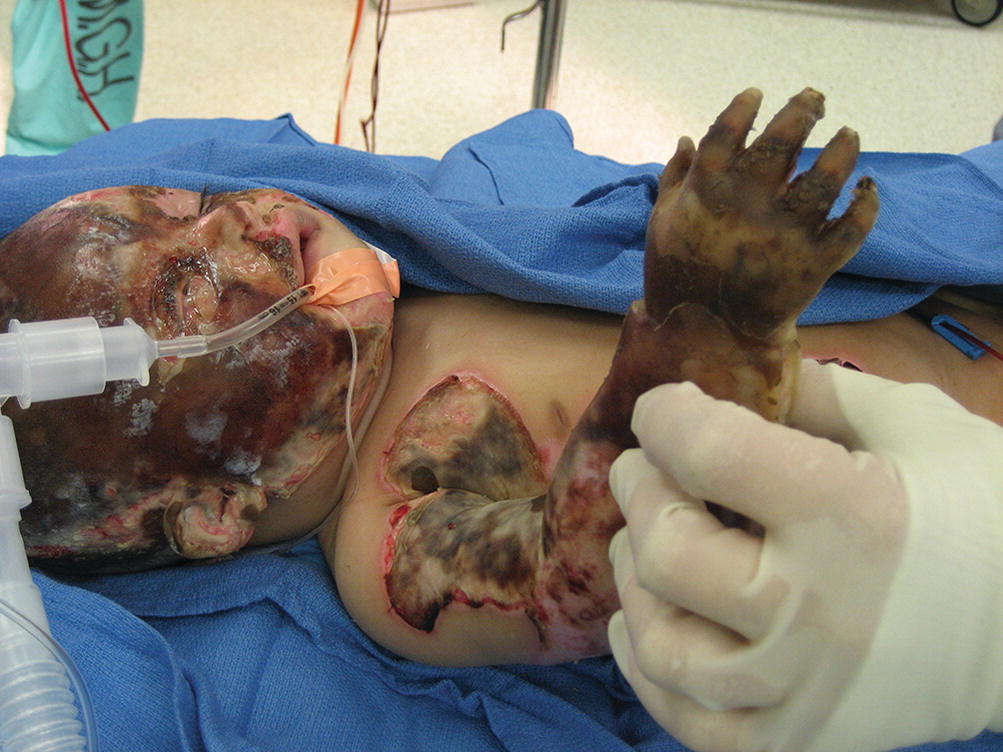
Young children have a high surface area to mass ratio and often minimal subcutaneous fat, making them extremely prone to hypothermia
Important anatomic differences also exist. The child’s upper airway is narrow and more prone to occlusion from resuscitation-associated edema. The trachea is shorter in infants, and more susceptible to mainstem intubation. Young children have small caliber blood vessels, making vascular access more challenging. Children will often outgrow an initial good surgical result, requiring more frequent reconstructive interventions. Anecdotally, young children more vigorously form hypertrophic scar than the elderly. Young children, like the elderly, have a much thinner skin, making burn healing and donor procurement more challenging.
Important emotional and psychologic differences also exist. Pain and anxiety are more difficult to assess in young children and adults. Emotional pitfalls and needs vary with development, with the middle school years being particularly difficult. Family and school issues have a major impact on the well-being of a recovering child.
29.3 Epidemiology and Mechanism Differences
The etiology and incidence of burns varies most with socioeconomic status and age [3]. In the developing world, legislative safety mandates are less frequently enforced resulting in both a higher incidence of injury and differing mechanisms. Electrical injuries are far more common in developing countries as are related cooking injuries. In the developed world, scald injuries predominate in infants and toddlers.
Safety and prevention are laudable efforts in this age group. Safety mandates are variably enforced and include legislation regarding fire retardant sleepwear, fire safe cigarettes, and hot water heater temperature set points. Prevention efforts focused on family education have been successful [4]. Constant repetition is essential.
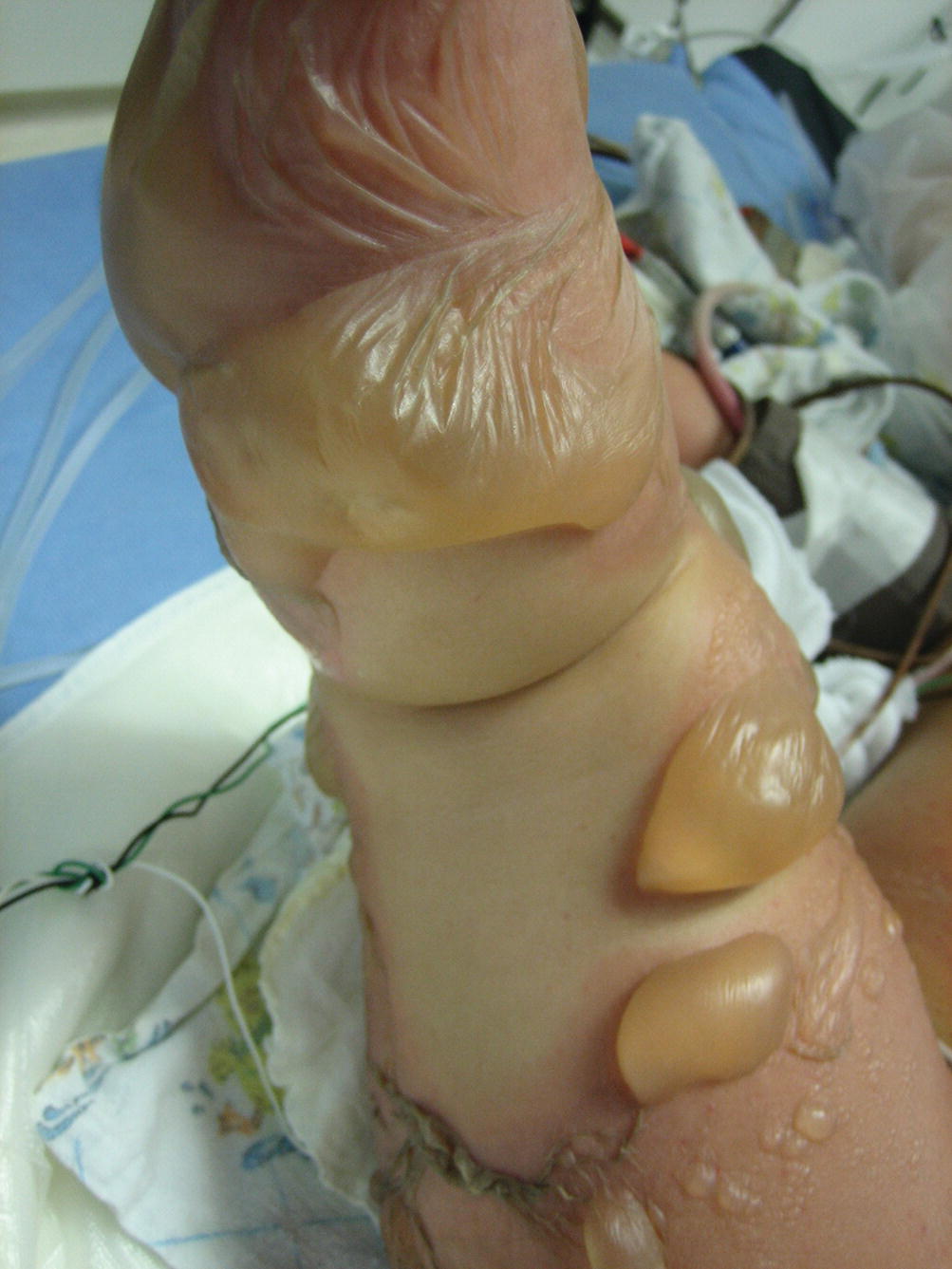
When caring for children in whom abuse or neglect is suspected, detailed and non-judgmental documentation, careful wound diagrams, and quality wound photography are extremely important
29.4 Outpatient Care Differences
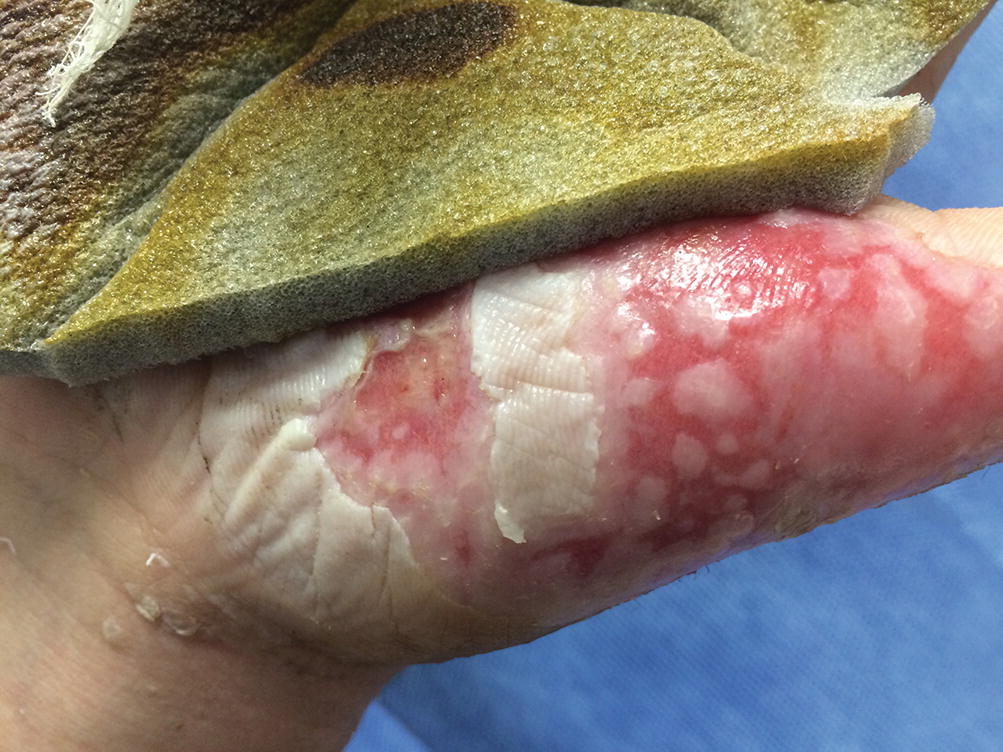
As in adult outpatient care, membrane dressings of a variety of types have proven efficacious in extending the ability to provide comfortable outpatient burn care. This membrane dressing absorbs moisture while releasing silver ion. Many partial thickness wounds will epithelialize under such membranes, but monitoring for submembrane infection is important
29.5 Inpatient Care Differences
The general management strategy for children with large burns based on the early excision paradigm is not conceptually different than that for adult patients [8]. These principles are well outlined elsewhere in this book. However, some subtle but important differences in execution do exist. Engaging the family throughout the care process is important. Time should be budgeted in the busy provider’s day to review progress and plans with the family frequently. Having the family as an ally is extremely helpful both short and long term.
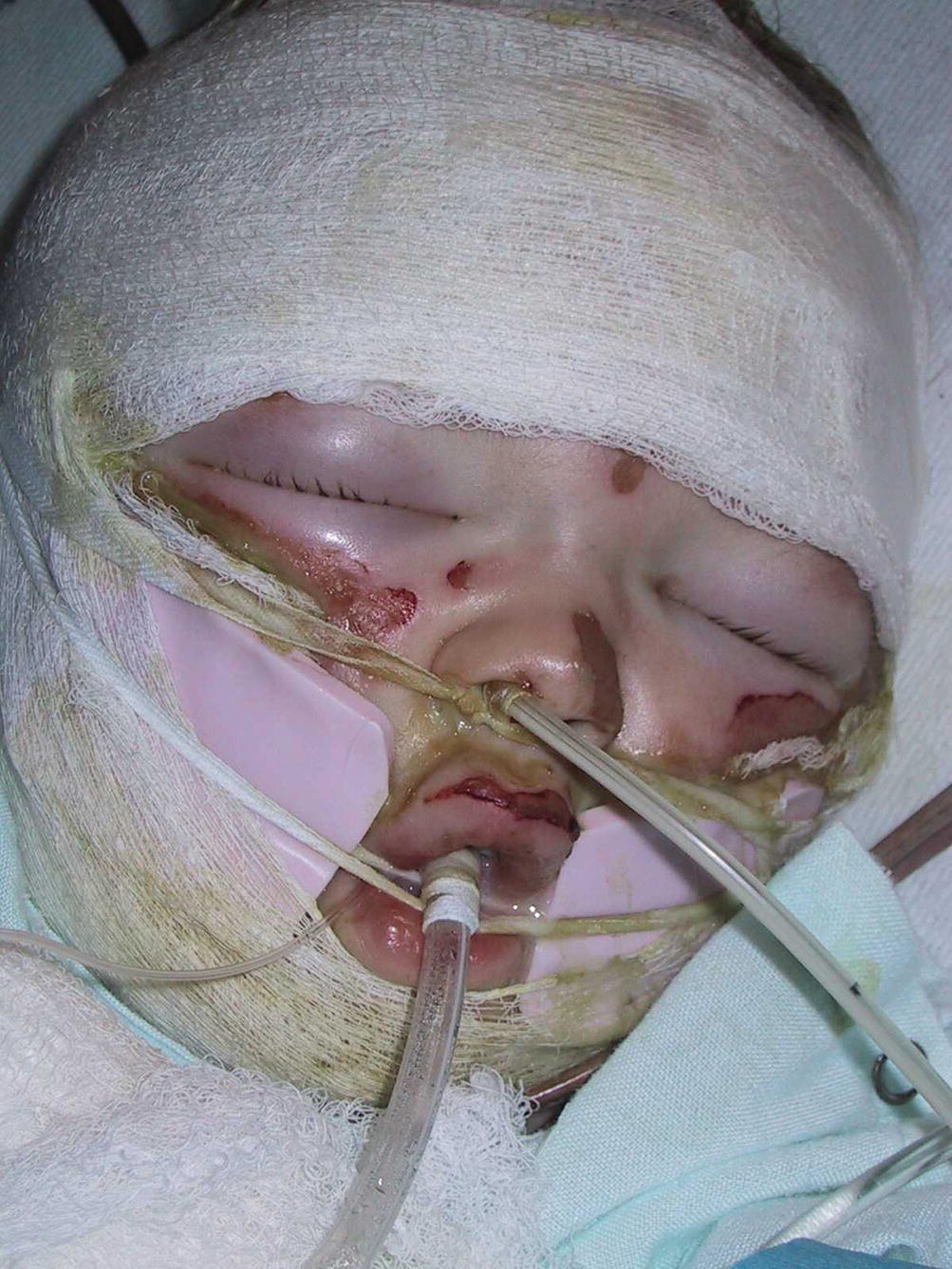
Reintubating children after unplanned extubation can be quite challenging and is best avoided through adequate sedation and mechanical tube security, one of which is a tube–tie harness system as illustrated here
The hypermetabolic catabolic state is poorly tolerated by young children. Early tube feedings are advocated, generally beginning during resuscitation. Short-term parenteral nutrition is well tolerated and can be useful during periods of sepsis or hemodynamic instability [15]. Nutritional targets should include 2–2.5 g per kilogram of ideal body weight per day of protein and a caloric target of 1.5–1.7 times a basal metabolic rate [16]. The use of anabolic agents remains an area of some controversy in the field with good outcomes documented on both sides [17, 18].
Differentiating benign fever from sepsis in children can be challenging. Many young children have a propensity to manifest high fever in the absence of infection. In the current era of antibiotic stewardship, if a child looks toxic with a fever, drawing blood cultures and starting antibiotics with a plan to stop them if the blood cultures are negative at 72 h is reasonable [19]. Children with inhalation injury and respiratory failure are ideally managed with lung protective strategies of mechanical ventilation, pulmonary toilet, and focused treatment for infection [20]. It was not that long ago that young age was an independent predictor of mortality in burns. However, that is no longer the case largely secondary to the evolution of pediatric critical care techniques with early wound excision, accurate individualized fluid resuscitation, lung protective strategies of ventilation, and focused treatment of infection [21].
29.6 Fluid Resuscitation Differences
Basic principles of burn resuscitation are similar in adults and children. Here again, this section will only present differences that have practical clinical consequences. Children with burns less than about 15% of the body surface generally need no formal resuscitation. Providing them fluid at about 150% of a maintenance rate via combined oral and intravenous route is generally sufficient. Adequacy of hydration can be monitored by urine output (weighing diapers and physical exam looking at mucous membranes and peripheral pulse quality).
Suggested resuscitation endpoints in children
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








