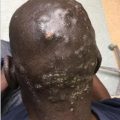
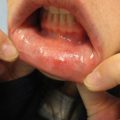
This chapter reviews rashes that present with a primary morphology commonly described as a “bump” by patients. A broad range of conditions is reviewed, including arthropod bites, Grover disease, prurigo nodularis, renal pruritus, keratosis pilaris, lichen nitidus, lichen planus, viral warts, molluscum contagiosum, and granuloma annulare. arthropod bites bug bites Grover disease prurigo nodularis renal pruritus keratosis pilaris lichen nitidus lichen planus viral warts molluscum contagiosum granuloma annulare Campbell Stewart Arthropods are responsible for many dermatologic complaints, including bites, stings, and infestations. They can also be vectors for numerous systemic and life-threatening diseases. The clinical manifestations of arthropod bites vary greatly depending on which arthropod is responsible. Because of the scope of this chapter and book, several arthropod reactions will not be covered, including hymenoptera (bees, wasps, hornets), centipedes, millipedes, caterpillars/moths, scorpions, scabies, chiggers, and lice. Mosquitoes, midges, flies, bed bugs, and fleas are all insects that can cause papular urticaria. These lesions present as discrete, well-demarcated, pink-red, blanching papules at the site of the bite. The usually pruritic papules can last for several days and may not appear until 24 hours after a bite occurred. Occasionally, these lesions can appear papulovesicular or bullous. Often, a central punctum can be identified. Mosquitoes, midges, and flies tend only to bite exposed sites. Flies (such as the horse fly, deer fly, and greenheads) mostly cause painless bites at first, followed by intense pain. The remaining lesions are often more painful than itchy. Fleas jump and therefore commonly affect the lower legs. Bed bugs tend to bite in groups or lines (the so-called “breakfast, lunch, and dinner” sign). Mosquitoes can transmit numerous infections, most commonly malaria, worldwide. In the United States, West Nile, Eastern Equine, and Western Equine encephalitis, as well as Zika and chikungunya, are all relevant mosquito borne diseases. Flies do not tend to transmit disease in the United States but can cause myiasis, filariasis, and onchocerciasis elsewhere in the world. Bed bugs can be a vector for Chagas disease (trypanosomiasis) where the disease is endemic. They may also transmit hepatitis B. Fleas are vectors for murine typhus, tularemia, bubonic plaque, and tungiasis. The differential diagnosis for bites from the aforementioned insects includes allergic contact dermatitis (ACD), scabies infestation, lice infestation, and bullous pemphigoid (BP). Most arthropod bites resolve without intervention. Determining the cause of the bites can be challenging if the practitioner does not ask about outdoor exposure, pet exposures, work, travel, and living arrangements. A thorough history is recommended to identify the most likely cause of the bites. If there is a clear history of outdoor exposure, counsel the patient regarding protective measures. These can include limiting outdoor time at twilight, avoiding stagnant water, and wearing long-sleeve shirts and pants. Insect repellents can be applied directly to skin (DEET or picaridin), and permethrin can be sprayed directly onto clothing and allowed to fully dry (not applied to skin). If there is no clear history of outdoor exposure, then it is essential to take a travel history for the patient and anyone in the home. An infestation of the home by bed bugs or fleas is possible. An exterminator is essential because there is no clear way to determine the type of insect responsible based on the bites alone, unless the patient brings one in to be examined. A mid-potency topical steroid, such as triamcinolone 0.1% cream, should be applied twice daily for up to 7 days. For spider bites, referral to an emergency room may be needed for pain control and if there are systemic signs and symptoms. For brown recluse bites, light compression/immobilization and cooling of the sites may help. Patients may need supportive care and/or administration of antivenom if it is available. A tissue culture may be needed in the setting of necrosis to evaluate for infectious causes. Skin necrosis from brown recluse bites may require debridement and skin grafting. Black widow bites should be treated with pain management, including opioids, antihistamines, and benzodiazepines if needed. If there is suspicion for tick exposure, even if no tick is found, treatment for Lyme disease is recommended in endemic areas. Normally, this includes treatment with oral doxycycline or amoxicillin. If there is a partial, but inadequate response after a 1-week trial of a mid-potency topical corticosteroid monotherapy, a higher potency steroid, such as a clobetasol 0.05% cream or ointment, may be applied twice daily for up to 7 days to the lesions of papular urticaria. If the response continues to be inadequate, reconsider the diagnosis. A biopsy may be indicated. In a patient with lesions that continue to appear in new locations on the body, consider the possibility of an untreated infestation. Topical calcineurin inhibitors, such as tacrolimus and pimecrolimus, may also be used for symptom relief. A common pitfall is not taking an adequate history. Asking specific questions about exposures will yield the correct causative type of arthropod most of the time. Another pitfall is not counseling the patient appropriately about risks and procedures in the setting of home infestations. Many patients are concerned about added costs and are reluctant to pursue veterinary or exterminator appointments as needed. Your skin lesions are small inflammatory reactions to the bite of an insect. These bites are usually very itchy. They can persist for several days or, rarely, weeks. You may not recall being bitten, and bites can take 1 to 2 days to appear. Most insect bites are caused by insects that live outside, such as mosquitoes, flies, or midges. These can be prevented by wearing clothing and applying insect repellent sprays. Most bite more frequently at twilight, so it is best to move indoors at that time. Avoid areas of standing water because these are places where most of them breed. If you do not recall being outside at a time of year when insect bites are common, then you may have been exposed to insects that can live inside. Fleas are common causes of insect bites and can infest pets and humans. They live in your home and are small insects that can be pulled from your involved pet’s coat. They tend to cause bites on the lower legs. Bed bugs can also cause bites. These insects infest homes and are extremely hard to detect except by trained professional exterminators. They live in walls, floorboards, bed frames, and other areas. They can be acquired by staying in an infested home or hotel room and may travel in your luggage. They only feed during a brief period in the night and leave small pinpoint bloodstains on the sheets. Without an exterminator, the infestation will persist. These types of insect bites can be easily treated with topical steroids applied twice daily for 5 to 7 days. If you notice blistering at your bite site, or if there is persistent pain or skin breakdown, you may have been bitten by a spider. You may need to have your home investigated for an infestation. If you have pulled an insect off of you that seemed attached to your skin, it was almost certainly a tick. These bites can cause red target like rashes on the skin. We may need to treat you with an oral antibiotic for several weeks to treat any potential Lyme disease. Shivani Sinha, Gloria Lin, and Katalin Ferenczi Grover disease (GD), also known as “transient acantholytic dermatosis,” is an acquired condition usually seen in middle-aged Caucasian men. The etiology is poorly understood, but GD has been associated with heat, sweating, sun exposure, radiation, and certain medications. Although benign and potentially self-resolving, the rash may become chronic with fluctuating symptoms that can last for several months or even years. The differential diagnoses for GD are folliculitis, including pityrosporum folliculitis, acne, miliaria, morbilliform drug eruption, Darier disease (DD), and pemphigus foliaceus (PF). GD is typically a clinical diagnosis based on the findings of a pruritic papulosquamous eruption on the abdomen and lower back of an older adult. Clues in the patient history, such as symptomatic exacerbation with sweating/overheating, can be helpful in securing the diagnosis. Rarely, a punch biopsy of lesional skin is required to confirm the diagnosis. There are no disease-specific therapies for GD, and treatment is directed toward symptom management. For GD that is refractory to topical steroids and supportive therapies, other treatment options may be considered. If treatment response is inadequate, reconsider the diagnosis and refer the patient to dermatology for further evaluation. You have a condition called Grover disease, which is not dangerous to your health but can be challenging to treat. It is important to avoid any known triggers, such as excessive heat, sweating, and sun exposure, because these can exacerbate the rash. The course of the condition can be unpredictable with fluctuating symptoms, and it may last anywhere between a few weeks to a few years. There is no cure for your condition, but certain over-the-counter (OTC) and prescription medications can help reduce your symptoms. Moisturizers, topical steroids, and antihistamines can help alleviate the itching and may be used as instructed by your physician. Other systemic medications and therapies can be prescribed if your rash is persistent. These medications can be discussed if your symptoms do not improve with the use of creams. The itching you experience may become severe. Let your physician know if it begins to negatively affect your quality of life so that your treatment plan can be adjusted accordingly. Shivani Sinha, Gloria Lin, and Katalin Ferenczi Prurigo nodularis (PN) is a chronic skin condition caused by repetitive scratching, rubbing, or picking (Fig. 6.2). It is more commonly seen in middle-aged women, who often have an underlying condition that may be dermatologic or psychiatric. Less commonly, it can be seen in the pediatric population secondary to concomitant atopic dermatitis (AD). Early recognition is important to halt this cosmetically disfiguring process, which can be extremely distressing for the patient, and to address any underlying conditions that may be contributing to this disease. The differential diagnosis for PN includes keloids, acquired perforating dermatoses, pemphigoid nodularis, nodular scabies, hypertrophic lichen planus (LP), multiple keratoacanthomas, and epidermolysis bullosa pruriginosa. Patients with suspected PN should be referred to a dermatologist for further evaluation and treatment. PN is usually a clinical diagnosis made by the dermatologist based on the patient’s history and physical examination. The most important step in management is to communicate expectations with the patient because PN can be a challenging condition to treat. The patients are often anxious and become easily frustrated by the lack of improvement. Helping to control the pruritus and urge to scratch or pick at the areas is of the utmost importance to stop the repetitive itch-scratch cycle. Based on the complexity and possible reactions to the treatments, a referral to dermatology is advised.
6: Bumpy rashes
Abstract:
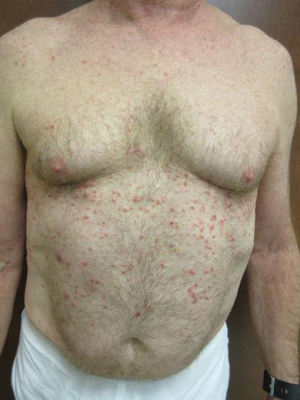
Arthropod bites
Clinical features
Differential diagnosis
Work-up
Initial steps in management
General management comments
Recommended initial regimen
Partial but inadequate response
Continued inadequate response
Other treatment options
Warning signs/common pitfalls
Counseling
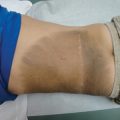
Grover disease
Clinical features
Differential diagnosis
Work-up
Initial steps in management
Inadequate treatment response
Warning signs/common pitfalls
Counseling
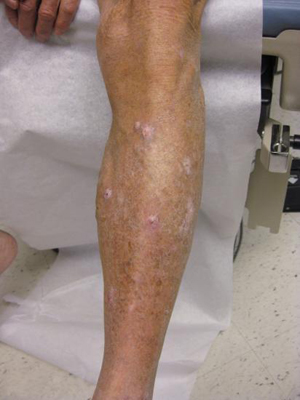
Prurigo nodularis
Clinical features
Differential diagnosis
Work-up
Initial steps in management
Antihistamines
Steroids
Other medications
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine