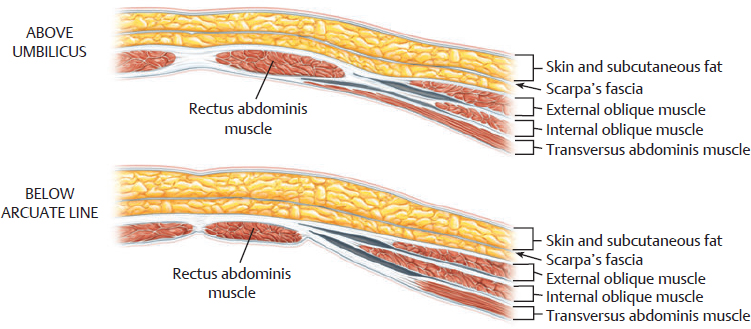
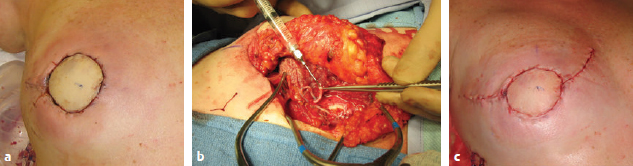
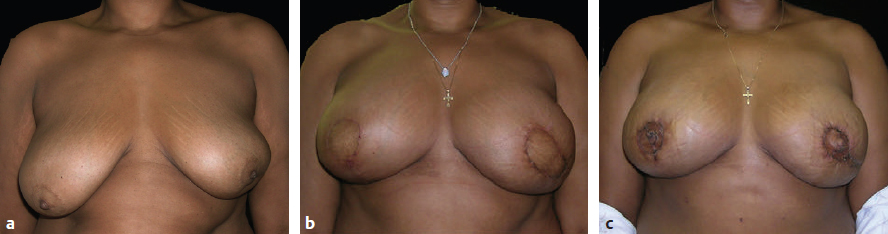
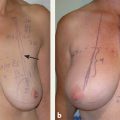
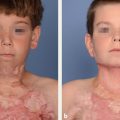
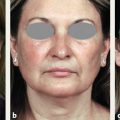
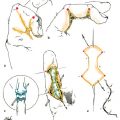
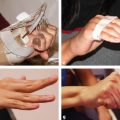
CHAPTER Breast cancer affects 1 in 8 women, and mastectomy for treatment has become increasingly common.1 Breast reconstruction offers an opportunity to restore a significant portion of what is lost both mentally and physically.2,3 Women often face a decision between implants and autologous options for reconstruction. Although the expander and implant reconstruction remains the most common form of reconstruction in the United States, autologous reconstruction in the form of free tissue transfer has become increasingly common in major centers.4 Free flap breast reconstruction offers some significant advantages over implant reconstruction in that the reconstruction replaces like with like and creates by far a more natural aesthetic result that evolves with the patient over time and requires no maintenance. This leads to long-term higher satisfaction compared with implant reconstruction.5 Although not all patients are candidates for autologous reconstruction, most women of typical breast cancer age have enough redundancy in the lower abdomen to provide for at least one flap. Because the abdomen has become the workhorse for autologous breast reconstruction, this chapter focuses on these approaches, including the muscle-sparing free transverse rectus abdominis myocutaneous (MSFTRAM), deep inferior epigastric perforator (DIEP), and superficial inferior epigastric artery (SIEA) flaps. The concepts discussed here can be used to avoid and manage similar complications with other forms of autologous reconstruction. Summary Box Most Common Complications of Breast Reconstruction with Autologous Tissue • Flap thrombosis and flap loss • Fat necrosis • Asymmetry • Delayed wound healing • Hernia/bulge • Patient dissatisfaction No chapter on autologous reconstruction would be complete without a discussion of flap thrombosis. Flap thrombosis is a dreaded complication of all microsurgeons, because it is the only complication that can lead to complete failure of the reconstructive effort while still putting the patient through the difficult recovery process. Managing a thrombosis is addressed later in this chapter, but avoiding the complication is always preferable. Various publications have placed flap thrombosis rates for breast reconstruction from less than 1 to 5%.6–8 Our experience has been less than 1%, making free flap breast reconstruction very successful. The first thing to consider in avoiding this complication is patient selection and taking an appropriate history and physical. The surgeon should take a moment to specifically ask questions targeted at identifying hypercoagulability such as previous deep vein thrombosis (DVT), pulmonary embolism (PE), stroke, or multiple miscarriages in the patient or first-degree relatives, because 5 to 10% of the population is estimated to be hypercoagulable.9,10 In our practice, any unusual history prompts a referral to hematology for a hypercoagulable workup to look for genetic conditions such as factor V Leiden, prothrombin gene mutation, antithrombin III deficiency, protein C or S deficiency, or acquired conditions such as lupus anticoagulant, antiphospholipid, or anticardiolipin antibodies, to name a few. That being said, a negative screening does not mean the patient is not hypercoagulable; it is estimated that more than 40% of patients who are clinically hypercoagulable have no identifiable cause.11 Identifying a cause, or at the least a history, allows for proper patient counseling preoperatively; however, this is not to say that hypercoagulable patients are not candidates for free flap reconstruction. Hypercoagulable patients are at higher risk, with flap failure as high as 20%.12 This risk can be mollified by the use of intraoperative and postoperative anticoagulation. A regimented use of anticoagulation can lead to very successful outcomes. Nelson et al13 have had early success with a protocol including a 2,000-unit bolus of heparin before anastomosis followed by a therapeutic heparin drip postoperatively, then anticoagulation with warfarin for 1 month. Not surprisingly, this does lead to higher transfusion and hematoma rates, which patients should be counseled on.13 Regardless of the use of anticoagulation, flap thrombosis in a known hypercoagulable patient, in our experience, has had zero chance of salvage with takeback. Previous history of radiation should be discussed. Radiation has been shown to lead to a higher rate of intraoperative vascular complications requiring anastomotic revision and the use of intraoperative anticoagulation.14 This appears to be limited to an intraoperative phenomenon and in our experience does not connote a higher incidence of postoperative thrombosis or flap loss. We do not specifically change our approach knowing that radiation was received; however, radiated vessels may be less ideal for teaching purposes, and the surgeon should have a low threshold for redoing an anastomosis if it does not look perfect.14 Finally, previous surgery should be considered. The internal mammary vessels are our preferred site for use as a recipient. Previous mediastinal surgery may make these vessels more scarred and less healthy, and the surgeon should not be afraid to look for an alternative recipient site if need be. Our second choice is almost always the thoracodorsal vessels, but both have comparable results.15 Abdominal surgery can affect the quality of the pedicle as well. If the quality of the pedicle does not appear to be normal, the free flap can be converted into a standard pedicled transverse rectus abdominis myocutaneous (TRAM) in most circumstances. Fat necrosis is characterized by areas of a flap that are no longer soft and supple, but rather are palpable masses or nodules that can be quite concerning to patients who have been treated for breast cancer. Usually, areas are small and treatable by simple excision, but occasionally fat necrosis can be more extensive. The cause of fat necrosis is fairly straightforward—small areas of underperfusion of a flap. This can result from arterial underperfusion or venous congestion. Risk factors from a medical history perspective have been difficult to consistently identify, but several studies have shown that radiation therapy increases the likelihood of fat necrosis. Obesity increases the likelihood in pedicled TRAM reconstruction but is less convincingly a problem in free flap reconstruction. Smoking was consistently shown to adversely affect results in pedicled TRAM reconstruction, but this has been less convincing in free tissue techniques, likely because of the more robust blood supply.16 The most important factor in avoiding this complication is maintaining a diffusely well-perfused flap. Studies have consistently shown a higher rate of fat necrosis in DIEP flaps compared with free TRAM flaps.16,17 Regarding perfusion, there are likely several factors worth discussing. Perforasomes refer to the innate vascular territory supplied by any given perforator. Unfortunately, predicting the territory of a perforasome is challenging. Generally speaking, the further tissue is from a perforator, the less reliable the blood flow. For that reason, we routinely discard the most lateral abdominal tissue when using an abdominal flap. We serially resect tissue until normal bleeding (usually not congested) edges are identified. The quality and location of the perforators are factors that should always be assessed when performing a free flap. Breast free flaps are generally large in volume and fatty tissue, which is sensitive to underperfusion; thus harvesting a big flap on one small perforator is generally not a good idea. We sometimes do single vessel perforator flaps from the abdomen, but the perforator should be easily palpable and fairly centrally located. Despite being a large perforator, if it enters the very edge of a flap, the distal perfusion will likely be inadequate. This is particularly true when using medial perforators in bilateral free flaps where the abdominal tissue was split in the midline. Therefore centrally located lateral-row perforators are likely more appropriate for bilateral free flaps, whereas medial row perforators are more centrally located in a unilateral flap that incorporates volume from zones 1, 2, and 3. Whenever possible, we recommend using several perforators per flap to broaden the location of perfusion. Having multiple perforators also creates redundancy in the perfusion in case perforator injury occurs during dissection or transfer. Fat necrosis rates have been well studied, and there is ample literature to support that fat necrosis rates go up as the number of perforators goes down.18 In summary, it is clear that a true DIEP is more likely to result in fat necrosis than a MSFTRAM. Debate has lingered about the improved abdominal wall function with a true DIEP or SIEA; however, the results on abdominal wall function may be less pronounced than previously believed. In general, women have a hard time recognizing the effects of free flap reconstruction on abdominal wall function regardless of type of flap.19–21 In the end, women want and deserve a soft and supple reconstruction without areas of fat necrosis that remind them of cancer. For this reason, we recommend erring on the side of sacrificing a little muscle to maximize perfusion if necessary. This is particularly true in higher-risk patients who have other risk factors such as smoking, previous scar, or impending postoperative radiation therapy. When in doubt, the surgeon can temporarily place micro–bulldog clamps on each perforator and assess any effects on perfusion before ligation. The SIEA appears to have a perforasome more confined to a hemiabdominal location. The arterial perfusion of the SIEA does not reliably cross the midline.22,23 Therefore we rarely incorporate a large amount of volume from the contralateral abdomen when a unilateral SIEA is performed. The superficial venous outflow is sometimes necessary to prevent congestion. Some flaps appear to be inherently drained by the superficial vessels. We preserve a length of the superficial inferior epigastric vein (SIEV) whenever possible to allow for a secondary venous anastomosis if congestion is noted. If a flap appears congested on the abdomen after anastomosis of the deep system or if the superficial vein appears incredibly engorged, we often connect this vein to either a second internal mammary vein (IMV), a perforating vein, or the retrograde IMV for additional outflow. The improved outflow is often immediately evident clinically. Finally, the surgeon should avoid the use of too many insetting sutures to secure the flap. It is tempting to spend a considerable amount of effort shaping the flap and smoothing the contour with sutures; however, every bend placed in the flap or suture tied down decreases perfusion to the area. These small areas can lead to fat necrosis down the road. It is easier to smooth the contour and reshape later than it is to remove large areas of fat necrosis. Asymmetry is much more common after unilateral reconstruction than bilateral reconstruction. Although matching a contralateral native breast is much easier with a free flap than with an implant, some asymmetry is unavoidable. Thus, correcting the problem is likely a bigger topic than avoiding it. Nevertheless, there are some factors that are incredibly important to help minimize asymmetry. Asymmetry can be from positional, skin envelope, shape, or volumetric causes. From a positional standpoint, the best way to avoid a problem is to make sure the mastectomy pocket is properly defined before insetting the flap. Often, the mastectomy extends beyond the natural boundaries of the breast. It is a fundamental error to inset the flap before reestab lishing those boundaries first. This may require suturing of the mastectomy skin flaps down along the inframammary fold or out laterally. Scattered simple sutures are more than adequate to prevent further compromise of the blood flow within the skin flaps. Skin envelope issues are best avoided by making similar changes bilaterally or paying attention to differences in asymmetry to begin with. Shape asymmetries are difficult to avoid. Again, the surgeon should resist the temptation to do too much shaping with sutures to avoid fat necrosis. Shape is best addressed once everything has healed. The one area that should be addressed specifically if possible is the tail of the breast mound. Fitting the lateral extent of the flap into the tail helps avoid a divot over the superolateral pectoralis, which is hard to correct in later stages. Volume asymmetry is best avoided by assessing the patient in a supine and upright position and trimming as needed. Finally, sometimes the abdominal donor site is asymmetrical, and the surgeon must account for this during flap harvest and inset. Free flap breast reconstruction can be plagued by delayed wound healing of either the chest or abdomen. Both can be a result of patient factors or surgical factors. Preoperative assessment may help avoid some of this, but at the very least, identifying risk factors helps the surgeon to properly counsel patients preoperatively and prepare them for a potentially long road ahead. In multiple studies, diabetes, smoking, and morbid obesity have been identified as the biggest risk factors for wound-healing complications.6,8,24,25 This is true for most surgical procedures in general, but it is particularly true in free flap breast reconstruction, which creates large wounds to heal. In the setting of cancer, there may not be time for a patient to quit before surgery; however, in prophylactic cases, smoking cessation for 30 days prior and at least 4 to 6 weeks postoperatively will significantly improve results.26–28 In addition, checking the hemoglobin A1C of patients with diabetes is mandatory as a screening measure to know how effective their long-term glucose management strategy is. The surgeon should have a low threshold to consult an endocrinologist to help maintain tight glucose control postoperatively. Although it must be balanced with the need for a second surgery, delayed reconstruction may be the most appropriate option for patients of poor health with multiple risk factors for delayed wound healing. Aside from generalized wound-healing risk factors, intraoperative issues contribute to delayed wound healing as well. The biggest impact on the healing process of the chest is the perfusion of the mastectomy skin flaps. Poor wound healing of the chest is incredibly rare in delayed reconstruction, because these skin flaps are smaller, are delayed, and can be made as thick as possible. In immediate reconstruction, the reconstructive surgeon is reliant on the breast surgeon’s contribution, who has a different focus in mind—to get the cancer out. This can put the reconstructive and extirpative surgeon at odds, but ultimately it is the reconstructive surgeon’s responsibility to recognize and excise underperfused skin if necessary. Although a larger skin paddle is less aesthetically appealing in the long term, it is better than having to deal with dressing changes for months and an ugly tethered scar as a result of leaving underperfused breast skin at the time of surgery. Several centers have adopted the use of the SPY System (NOVADAQ Technologies), which uses indocyanine green (ICG) and a laser angiography to assess for perfusion of the mastectomy skin. This technology can be very useful not only in assessing mastectomy skin flap perfusion, but flap perfusion as well.29 Unfortunately, this technology is expensive and not universally available. Thus many surgeons resort to clinical judgment and simple techniques such as bleeding skin edges and capillary refill to assess for tissue perfusion. As for the abdomen, tension and perfusion are the biggest risk factors for poor outcomes that can sometimes be modified. If patients have previous scars, such as a cesarean-section scar, the surgeon should try to place new incisions in the same position to avoid parallel scars. This may require shifting the planned flap up or down on the abdomen depending on the location of scars. When dissecting up to free the upper abdominal tissue for closure, the surgeon should only dissect the minimum amount necessary to allow for closure. In large patients, this may require very little dissection. If full upper dissection is necessary, the surgeon should at least try to avoid sacrificing perforators in the upper outer quadrants of the abdomen to maintain perfusion. In addition, only the amount of tissue necessary to reconstruct the breasts should be removed. Most women do not require a very wide flap. The width of the breast mound usually correlates to the height of the tissue taken from the abdomen in standard reconstruction, in which a contralateral flap is rotated 90 degrees and connected to the internal mammary vessels. Taking no more than is necessary will help alleviate closure under tension. Postoperatively, these wounds should be followed closely. The surgeon should avoid the temptation to remove drains prematurely, because fluid collections can lead to wound dehiscence. Infection should also be treated aggressively, because the combination of infection and tension usually has poor outcomes. Perhaps most importantly, patients must be instructed to eat well. Many patients lack appetite or have a sudden urge to “eat healthy” postoperatively. This is not the time to eat salad and toast. A high-protein diet maximizes the body’s ability to heal, and we actively encourage our patients to increase protein intake. Aside from an SIEA, all other abdominal free flaps inherently have the potential to affect the integrity and function of the abdominal wall long term. Studies have shown measureable functional differences between an SIEA, DIEP, and MSFTRAM, most notably in bilateral reconstruction; however, these differences are imperceptible to patient functioning and have no apparent effect on quality of life.19,20 That being said, to minimize the risk of bulge and weakness, the surgeon should try to preserve as much functional muscle as possible. The lateral innervation of the rectus muscle should be left intact if possible, and if a well-perfused DIEP can be performed, this should be chosen over a MSFTRAM. A hernia is an unfortunate complication that occurs after 3 to 5% of free flap harvests from the abdomen, with the exception of the SIEA, which carries no risk. When it occurs, surgical correction is usually necessary and can be challenging; therefore attention to detail to prevent a hernia is necessary. Prophylactic mesh has been shown to reduce the risk of hernia or bulge but mesh is likely more important in bilateral cases where muscle has been sacrificed.30 Because this is a clean procedure, permanent mesh offers the strongest closure with the lowest risk of bulge. We therefore recommend prophylactic mesh within the rectus sheath with complete fascial coverage for a two-layered closure with permanent suture when muscle has been taken with the flap31 (Fig. 39.1). The greatest risk of hernia is below the arcuate line where all of the strength layers have been violated; therefore meticulous closure and proper mesh fixation is required to create the strongest closure. Postoperatively, patients should be told to refrain from heavy lifting for 6 weeks. Fig. 39.1 Cross-sectional anatomy of the abdominal wall above and below the arcuate line. (Reproduced from Jones GE. Bostwick’s Plastic and Reconstructive Surgery. 3rd ed. New York: Thieme Publishing; 2010.) Autologous breast reconstruction has a fairly high rate of postoperative satisfaction; however, dissatisfied patients are unavoidable. Although good outcomes certainly minimize the likelihood of dissatisfaction, there are dissatisfied patients with good outcomes and happy patients with bad outcomes. In the end, the most important step is to choose patients wisely and manage expectations well. This translates into spending a considerable amount of time with the patient preoperatively and educating him or her on the overall process including the good, the bad, and the ugly. If the surgeon has told them about the risks adequately in the beginning, most patients understand when they happen. An experienced microsurgeon or surgical team can instantly recognize a complete arterial thrombosis characterized by loss of a Doppler signal, capillary refill, and warmth (Fig. 39.2). Likewise, a complete venous thrombosis is easily diagnosed by an enlarged, congested flap with a blue to purple appearance (Fig. 39.3). One of the keys to maximizing clinical outcomes, however, is recognizing an impending problem. Early recognition is important because the faster the surgeon is able to correct a problem, the more likely the chance of flap salvage.32 Impending arterial thrombosis can be characterized by a changing quality of a Doppler signal. A bounding signal may change to an intermittent one as small thrombi form and clear. Capillary refill may become less brisk. If there is concern, a pinprick or scratch can be used to assess for bleeding. This should be brisk—any concern for decreased bleeding should prompt exploration. An early venous problem is sometimes only noted by “quick” capillary refill. Sometimes, the skin paddle may appear tense or glistening well before purple or blue discoloration settle in. Regardless, any hint of thrombotic issues should prompt surgical evaluation. While waiting, a bolus of heparin is indicated. Fig. 39.2 (a) Postoperative arterial thrombosis characterized by a typical pale skin paddle. (b) The anastomosis is resected, flushed, and reperformed to reestablish flow. (c) The skin island subsequently has greatly improved color and capillary refill. Fig. 39.3 The typical appearance of a venous thrombosis characterized by increased size and dark discoloration. Upon exploration, the pocket is reopened through the same incisions and the insetting sutures are removed to allow for complete mobilization out of the pocket and good exposure. The surgeon can get a better sense of perfusion by looking at the muscle included in the flap and the pedicle itself. An isolated arterial thrombosis with intact vein is repaired by placing a proximal bulldog clamp and resecting the entire anastomosis. The surgeon should inspect the suture line for technical causes to explain the problem. Both ends should be trimmed back to healthy tissue. Inflow should be rechecked and, if insufficient, either cut back further or converted to an alternative recipient artery. If a significant gap exists, either the artery and vein will need to be both redone to ensure equal length, or an interposition vein graft will be needed. The success rate of vein grafts is quite high, so surgeons should have a low threshold for their use.33 The flap should flush easily with heparinized saline. If there is no flow distally, thrombolytics or mechanical thrombectomy can be used. A venous thrombosis can be more challenging to correct. If there is still arterial inflow, the venous anastomosis is resected and the vein is milked of its clot. This is done without clamping the arterial inflow to avoid increasing the risk of a subsequent arterial clot. If good outflow flows from the pedicle, then the recipient vein is flushed to confirm distal outflow as well. After trimming for healthy tissue, the anastomosis is performed again. Again, if an interposition graft is needed, one should be performed. A more common occurrence is an inability to restore outflow in a “no reflow” phenomenon. In this case, a small butterfly needle can be placed into the artery and a thrombolytic (2 to 4 mg of tissue plasminogen activator in 50 mL 5% dextrose) slowly instilled into the flap over 10 to 20 minutes. If outflow is reestablished, the anastomosis is reperformed. If a secondary vein such as a superficial inferior epigastric vein is available, this should be connected if possible as well. If the recipient vein is clotted or unhealthy after distal resection, then an alternative site should be used. Postoperatively, more aggressive anticoagulation should be used over the standard subcutaneous heparin dosing, unless a clear technical problem is found such as twisting or backwalling. If there is no clear reason, the surgeon should assume a hypercoagulable state exists and the patient should be fully anticoagulated postoperatively. This may require outpatient conversion to warfarin as well. If the flap cannot be salvaged, it should be removed in the acute setting. Before a return to the operating room, the surgeon should inform the patient of the possibility of an inability to fix the problem and discuss alternatives. Although a secondary free flap is not indicated at this time, a tissue expander can be placed if two-stage reconstruction is an option. If previous radiation therapy eliminates this option, then closing the wound and readdressing reconstruction at a later date is the best course of action. On a rare occasion, a patient presents with a delayed venous thrombosis after leaving the hospital. If caught early, surgical intervention as described previously may be warranted; however, if the vein has been thrombosed for a prolonged time, as is often the case, then anticoagulation is the only option. Leach therapy has been tried and largely abandoned because of its complications.34 Small areas of fat necrosis can be treated with excision; however, larger volumes or areas in the far upper pole can be difficult to treat with excision without creating obvious contour deformities or new visible scars. Contour deformities from excision can be treated with fat grafting, but this may commit patients to multiple surgeries. An alternative technique can use liposuction, ultrasonic liposuction, or a power dissector.35 In this technique, a small cannula is used to drill holes in multiple directions in the area of fat necrosis. This technique is similar to aerating a green on a golf course. These small holes often soften the feel of the necrotic area and may allow for tissue ingrowth, which leads to improvement with time. It is useful to categorize deformities based on patient and surgeon observations. First, volume asymmetry is one of the biggest drivers of patient dissatisfaction because bra fitting is a challenge. In unilateral reconstruction, the free flap may be smaller or larger than anticipated; however, even in bilateral reconstruction, volume asymmetry occurs. Treatment of volume differences greatly depends upon patient wishes. Small reductions in a flap can be easily performed with liposuction, whereas large reductions may require a more formal approach with resection. Conversely, augmentation of the contralateral side can be performed with fat grafting or implants. Which side to modify greatly depends on patient goals. Contour irregularities are common after free flap reconstruction. The cause is multifactorial, but the most common factor is a baseline mismatch in size or shape between the breast tissue removed and the free flap inset. This can be most notable in the upper pole or tail of the reconstructed breast mound, where a tapered effect is difficult to achieve primarily. Small areas of fat necrosis can lead to hollowing or frank masses, which may require revision. In addition, lack of central projection relative to a natural breast is a common complaint. This is generally caused by an inability to completely cone the central mound in a manner similar to a native youthful breast. A free flap (particularly a DIEP without muscle) is often fairly uniform in depth, which can lead to a flat-appearing breast mound. All of these issues can be addressed with fat grafting, although on occasion a small implant centrally can work very well to add central projection. Many women choose autologous reconstruction to avoid the issues associated with implants, however, in which case staged fat grafting may be a better choice. Patients with grade I ptosis are rarely subject to problems with flap position in the postoperative period as long as the mastectomy pocket remains confined to the breast tissue. Simple changes may be amenable to liposuction, but generally speaking, major changes require re-creation of the pocket, movement of the flap, and redefining of the pocket. Because this is not a minor revision, every attempt should be made to avoid this problem to begin with. More likely, positional problems arise in patients with preexisting ptosis when skin envelope changes are being made in an immediate reconstruction or in delayed reconstruction when the envelope is being re-created. A common issue is a vertical discrepancy, either related to uneven skin resection from side to side or in a unilateral reconstruction in which a contralateral balancing procedure is needed. Assessing symmetry and patient satisfaction should be approached similarly to how a surgeon would assess any breast consultation. Similar techniques also can be used to improve vertical positioning, such as the vertical mastopexy. Usually, however, these are skin-only procedures as opposed to formal parenchymal and pillar procedures. In all cases, but delayed reconstruction in particular, it is important to ensure enough time has passed to allow the envelope to relax and drop before revision. The use of fat grafting is possibly the most important technique available to revise the reconstructed breast (Fig. 39.4). Fat grafting techniques are addressed in detail in Chapter 19; however, some technical points are worth discussing here. First, the donor site may play a role in graft take; some studies have shown the lower abdomen and inner thighs to be higher in adipose-derived stem cells.36 These cells are believed to aid in survival; however, other studies have failed to highlight major differences in donor site value.36–39 The donor site of choice is injected with 1% lidocaine with epinephrine. Fat can be procured using manual aspiration or a formal liposuction device. Larger cannula diameters may yield healthier fat cells.40 If a lipo suction device is used, it is likely that lower aspiration pressures aid in cell survival, but further research is needed in this area. The fat must be prepared before use to remove fluid, debris, and free oil. This can be done using filtration, sedimentation, or a centrifugation system that spins the fat down. Centrifugation is more practical for larger volumes; however, no one method of preparation has been shown to be most effective.41 Several procurement and processing systems are now marketed to make the process more efficient and hopefully offer better results, but their efficacy has not been proven. Research on the quality of the fat based on site of harvest and method of procurement is constantly evolving and at this time is not convincing that one method far surpasses another.41 What is likely the most important factor contributing to long-term survival is the environment in which the fat is placed. Fortunately, a previously transferred free flap is usually very well perfused. Fat should be placed in small aliquots (no more than 0.5 cc per pass) using a multipass technique as described by Coleman.42 The fat should be placed in multiple planes even if the defect feels superficial. Superficial and deep planes allow for placement of each pass into its own space. Injection can be made directly into the pectoralis muscle, because it serves as an excellent recipient site for fat survival. Fat should be injected in multiple directions as well. This technique requires multiple access points. Because this can be done through 1-mm access points, scarring should not be a concern. A three-dimensional crosshatch network of lines should be the goal, not simply injecting through convenient locations. When larger volumes are necessary, the surgeon must avoid the temptation to try to achieve perfection in one setting. Overfilling leads to lower retention rates and most patients, if educated properly, will understand why staged surgical procedures are necessary and beneficial.43 A radiated bed can still receive fat grafts; however, retention rates are likely lower.44 Therefore the surgeon should inform the patient that fat grafting may require more stages or even be ultimately less successful after radiation therapy.
39
Breast Reconstruction with Autologous Tissue
Avoiding Unfavorable Results and Complications in Breast Reconstruction with Autologous Tissue
Thrombosis and Flap Loss
Fat Necrosis
Asymmetry
Delayed Wound Healing
Hernia/Bulge
The Dissatisfied Patient
Managing Unfavorable Results and Complications in Breast Reconstruction with Autologous Tissue
Thrombosis and Flap Loss
Fat Necrosis
Asymmetry
Assessing the Problem
Volume
Contour/Shape
Position
Fat Grafting
Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine