Thinking about bariatric surgery? In Colorado, everything starts with one number—your Body Mass Index (BMI). Yet hospitals, insurers, and Reddit threads toss out competing cut-offs, leaving you guessing.
We’ll clear that up in one read. Below you’ll see exactly where Colorado’s leading programs draw the line, how Medicaid and private insurers layer on their own BMI rules, and what to do if you sit just outside them. First, jot down your BMI with this quick BMI calculator. Got it? Good—let’s see whether you already meet the 40-or-35-with-conditions benchmark and what comes next.
The national baseline: why the 40 and 35 numbers still matter
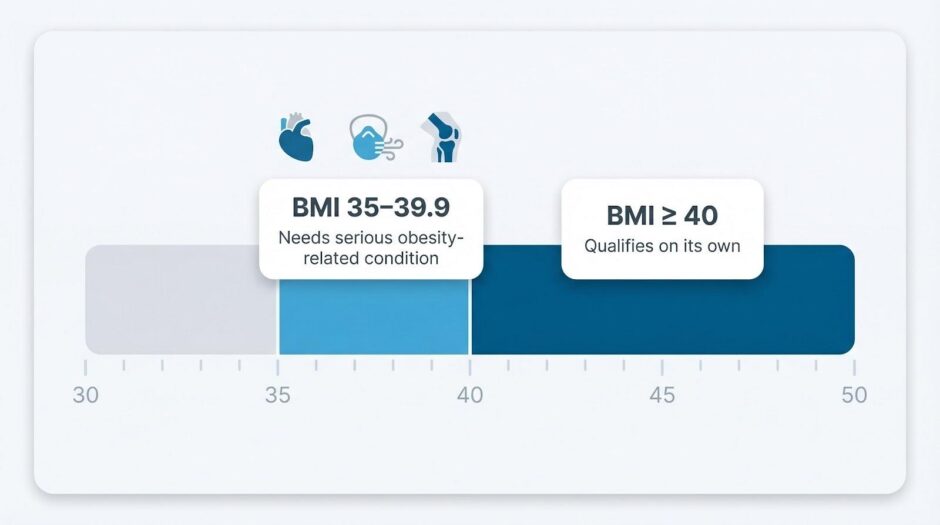
A BMI of 40 or higher qualifies for bariatric surgery on its own. A BMI of 35–39.9 still meets the mark when at least one serious obesity-related condition is present—type 2 diabetes, obstructive sleep apnea, resistant hypertension, or severe joint damage.
Most programs accept adults aged 18–65 because surgical risk climbs after the mid-60s and insurers want extra clearance.
Remember, BMI is simply a height-and-weight shortcut that helps clinics and insurers speak the same language. Surgeons still confirm readiness with lab work, cardiac testing, and a mental-health review before scheduling the operating room.
Those checks matter, yet the two numbers—40 and 35—remain the gatekeepers. Every later conversation with an insurance reviewer, HR rep, or curious family member circles back to this baseline.
With the national yardstick set, let’s see how Colorado programs adapt it for teens, very high BMIs, and the new Medicaid expansion.
UCHealth: straight-up standards, big-system resources
UCHealth anchors Colorado’s academic medical scene, so it follows the classic playbook. A BMI of 40, or 35–39.9 with a serious condition such as type 2 diabetes or sleep apnea, unlocks surgery. Below that range, the team shifts to medication or supervised weight loss first.
Step one is a free online orientation where surgeons outline procedure options and lifestyle changes. Next come a psychological evaluation, dietitian visits, and six months of weight-management records if your insurer requests them. UCHealth flags those paperwork hoops early, so no one is surprised later.
High-risk candidates are not turned away. Anesthesia and cardiology review every chart, and the team often asks patients with very high BMIs to drop a few pounds pre-op for safety.
Because UCHealth stretches from Denver’s Anschutz campus to northern Colorado, rural patients can finish most dietitian and psychology appointments by telehealth, then drive in only for key milestones—useful when winter closes I-25.
If you prefer every specialty under one roof, UCHealth delivers. Just plan to follow their detailed checklist; academic centers keep a tight schedule, and that structure starts on day one.
Denver Health: wide BMI window and a path for teens
Denver Health is the city’s safety-net hospital, yet its bariatric unit runs like a top-tier specialty center. Adults with a BMI of 40–65 qualify outright. Those at 35–39.9 need one serious obesity-related condition to proceed.
The 65 ceiling is uncommon. Surgeons accept patients other programs ask to slim first, then set a short pre-op plan to shrink the liver and reduce anesthesia risk. If your BMI is above 65, they coach you to dip just under that mark before scheduling surgery.
Denver Health also holds full accreditation for adolescent surgery. Teens aged sixteen and up follow the same 40 or 35-plus-condition rules, but must show maturity, family support, and completion of the Healthy Lifestyles clinic. Most consults, dietitian visits, and support groups happen on secure video, which helps when school calendars clash with medical appointments.
Cost concerns? The center offers Sliding Fee and Financial Assistance programs for uninsured residents, and staff keep appeal letters ready when commercial insurers hesitate. Medical need comes first, and Denver Health works to keep the door open.
HealthONE / HCA: hinting at the future with a 30-plus option
Walk into any HealthONE hospital—Rose, Swedish, or Presbyterian/St. Luke’s—and the familiar rule appears: BMI 40 qualifies outright, while 35–39.9 needs a major comorbidity.
The twist is in the low-thirty range. Public guides note that surgeons will review charts for patients with stubborn diabetes at BMI 30–34.9, signaling that Colorado’s largest private network is inching toward the 2022 metabolic-surgery guidelines.
Practical takeaway: if you are 5 ft 6 in and 206 lb with an A1c that refuses to improve, book a consult instead of assuming the door is closed. Expect nutrition classes, a psychologist’s clearance, and proof of prior medical therapy, yet the invitation itself shows how fast eligibility is moving.
For most applicants, the classic playbook still applies. Complete an online seminar, log six months of supervised weight-loss visits, stop nicotine use, and line up social support. Coordinators walk you through each step and handle insurance appeals when needed.
Bottom line: HCA programs respect the traditional thresholds, but the data suggest earlier intervention beats waiting for a BMI of 40. If you fall in the grey zone, ask anyway.
BMCC at Parker Adventist: full-service care and Medicaid’s new gate opener

Walk into the Bariatric & Metabolic Center of Colorado and the vibe shifts from institutional to boutique. Dr. Joshua Long’s team follows the standard rule—BMI 40 qualifies, and 35–39.9 needs a serious health issue—yet participation in Health First Colorado now lets the clinic accept adults at BMI 30–34.9 who have uncontrolled diabetes, fatty-liver disease, or severe hypertension.
The team now asks patients to run their numbers through its online weight loss calculators, a one-page tool set for BMI, basal-metabolic-rate and target-heart-rate that confirms eligibility in seconds.
This policy change saves patients from the old “gain ten pounds, then call us” loop. Staff screen every Medicaid referral for medical necessity, then assemble the six-month packet Medicaid requires: dietitian notes, supervised weight-loss logs, a psychologist’s clearance, and physician attestations. You focus on lifestyle prep while the paperwork moves behind the scenes.
Self-pay clients get transparent package pricing with financing options when employer plans exclude bariatric coverage. Because Parker Adventist holds full accreditation, Medicare patients also satisfy the Center of Excellence rule without traveling elsewhere.
Telehealth nutrition visits, Saturday support groups, and a quick-response insurance team remove barriers. Meet the criteria, commit to the plan, and the path stays clear—whether your BMI begins with a three or a six.
Colorado Bariatric Surgery Institute: classic criteria, concierge feel
Colorado Bariatric Surgery Institute, led by Dr. Thomas Brown, keeps its BMI markers simple: 40 qualifies on its own, while 35–39.9 requires a major comorbidity such as diabetes or severe sleep apnea.
From there, the service turns boutique. A coordinator verifies your insurance benefits within 48 hours, then emails a clear roadmap: seminar date, dietitian appointments, psychology referral, and target labs. Because CBSI schedules only a few cases per day, patients often move from consult to operating room faster than at larger systems.
Cash-pay packages help when employer plans exclude bariatric surgery. Prices and financing options appear openly on the website, and revisional or robotic procedures carry upfront quotes.
For BMIs above 60, surgeons offer a staged plan—first a sleeve to lower risk, then a second procedure if needed. That willingness to manage complex cases, paired with small-office attention, draws patients from across the country.
If you meet the classic BMI rule and want white-glove guidance, CBSI delivers.
Insurance guidelines in Colorado: will your plan cover you?
A surgeon’s “yes” is only step one. Your insurance policy applies its own BMI limits and paperwork requirements on top of the medical rules. We will review the major payers—starting with the public program that recently opened access for thousands of Coloradans.

Colorado Medicaid: a new floor at BMI 30
Health First Colorado once followed the 40 / 35-plus-condition rule. In late 2025 the state lowered the bar: adults with BMI 30–34.9 qualify when a serious obesity-related illness is present—usually uncontrolled type 2 diabetes, aggressive fatty-liver disease, or severe hypertension.
What Medicaid still expects
- Six consecutive physician-supervised weight-loss visits
- Documented nutrition counseling
- A clean psychological evaluation
- Surgery at a Center of Excellence
Meet those boxes and Medicaid covers the operation at 100 percent.
Demand spiked the moment the rule changed, so orientation classes and dietitian slots can book out weeks in advance. Register early, keep every appointment, and you will hold your place while the paperwork moves forward.
Medicare: classic criteria, fewer hoops
Medicare follows the NIH baseline: BMI 35 or higher plus at least one significant comorbidity such as type 2 diabetes, coronary artery disease, or disabling arthritis.
The process is lighter. Medicare does not require a six-month supervised diet or attendance logs, although surgeons still recommend those habits to shrink the liver and improve long-term results.
One rule is firm: your surgery must take place at an accredited Center of Excellence, a box every Colorado program in this guide already checks. Older adults face extra medical clearance, including cardiology and pulmonary reviews, yet once those specialists sign off, Medicare pays under the standard deductible and coinsurance schedule.
If you are 65 with a BMI of 37 and sleep apnea, Medicare is likely an ally. Gather your records, let the surgical team handle authorization, and focus on pre-op preparation instead of insurance paperwork.
Anthem Blue Cross Blue Shield: six months to yes
Anthem covers more Coloradans than any other private carrier. It mirrors the NIH standard—BMI 40 alone or 35–39.9 with one major comorbidity—but adds one clear process step: six consecutive physician-supervised weight-management visits.
Each monthly check-in can be with a primary-care doctor or a registered dietitian. Anthem expects documentation of nutrition coaching, exercise goals, weight, and blood pressure. Miss a month and the calendar restarts, so schedule those visits early.
After visit six, your surgeon’s office bundles the diet notes with a psychology clearance, a medical-necessity letter, and two years of weight history. When every item matches the checklist, approvals usually arrive within two weeks.
Good news: if pre-op preparation drops your BMI below 40, Anthem still honors the approval. Stay on the program, arrive on surgery day, and coverage remains intact.
Bottom line: Anthem is predictable. The steps take time, but thousands of Colorado patients clear them by treating those six visits as non-negotiable.
UnitedHealthcare: strict on documentation
United mirrors Anthem on paper—BMI 40 alone or 35–39.9 with one major comorbidity—yet the company demands meticulous proof.
Plan on six consecutive supervised weight-management visits. Each note must list your weight, blood pressure, and the counseling provided. Miss a month and United restarts the calendar; clinics call this the “United reset.”
United also asks for a five-year weight history to show long-standing obesity. Pull those data early from primary-care charts, OB-GYN visits, or even old sports physicals to avoid delays.
When the packet is complete, approvals usually arrive within two weeks. Denials almost always trace back to missing pages, not BMI, so scan every note and keep receipts.
Good news: once United approves, it does not revoke coverage if pre-op weight loss drops your BMI below the threshold. Shrink the liver, arrive fitter, and your green light remains.
Cigna: three months, then the green flag
Cigna trimmed its pre-op program to three monthly weight-management visits, making it the quickest major insurer in Colorado. The BMI gates stay classic—40 alone or 35–39.9 with diabetes, sleep apnea, or another serious condition—but the timeline to approval can be as short as 90 days.
During each visit you meet a dietitian, keep food journals, and set activity goals. Reviewers look for documented “intensive behavioral therapy.” Complete all three sessions, add a psychologist’s clearance, and most authorizations land within ten business days.
Because the window is tight, documentation discipline matters. Reschedule a session and the calendar may slip into a fourth month, flagging the file for extra scrutiny.
Cigna also approves BMI 30–34.9 cases with uncontrolled diabetes. Surgeons win these exceptions by citing the 2022 metabolic-surgery guidelines and providing continuous-glucose-monitor data. If that sounds like you, mention it during the first consult.
Aetna: opening the door at BMI 30 with extra homework
Aetna was the first big carrier to adopt the 2022 metabolic-surgery guidelines. It still honors the classic thresholds—BMI 40 alone or 35–39.9 with a major comorbidity—yet adds a third lane: BMI 30–34.9 plus poorly controlled type 2 diabetes.
The opportunity is real, but preparation is strict. Aetna requires an intensive, multi-component behavioral program totaling twelve sessions. Most Colorado centers bundle these into a three-month sprint of weekly dietitian calls, exercise coaching, and progress check-ins. Miss a visit and reviewers pause the file until all twelve notes are complete.
Once you finish the program, surgeons add a psychologist’s letter and recent lab work that proves diabetes remains uncontrolled. Approvals often arrive within ten days because the request aligns with Aetna’s published policy.
Cost sharing follows your plan’s standard rules: deductible first, then coinsurance. If surgery pushes you past your out-of-pocket cap, future medical bills drop to zero for the rest of the year—a financial perk worth noting.
Key takeaway: Aetna rewards documentation. Show the twelve visits, present current diabetes data, and even a BMI in the low thirties earns a smooth approval path.
When the numbers don’t line up: smart moves at BMI 33 or 63
We hear two questions every week.
BMI 33 and health is sliding.
If your BMI sits at 33 with uncontrolled diabetes, do not gain weight just to reach 35. Instead, use newer pathways:
- Health First Colorado and Aetna approve BMI 30–34.9 when a serious disease is documented.
- HealthONE surgeons review similar cases for self-pay or clinical-trial spots.
- Any program can file an exception appeal when records show urgent need.
Bring recent lab results, an endocrinologist’s letter, and the 2022 metabolic-surgery guidelines. Surgeons upload that packet to the insurer’s appeal portal, and approvals often follow quickly.
BMI above 60 and safety questions.
Surgery remains possible, but expect a short pre-op plan:
- Denver Health accepts up to BMI 65 but requests a five-to-ten percent weight loss to shrink the liver.
- Other centers stage care: a sleeve first, then a second procedure after the initial weight drop.
- Insurers stay supportive; the loss target comes from surgeons, not payers.
The goal is risk reduction, not a test of willpower. Work with a dietitian, consider weight-loss medication, and meet the modest target. Each pound reduces anesthesia time and improves recovery odds.
Beyond BMI: the other boxes you must check
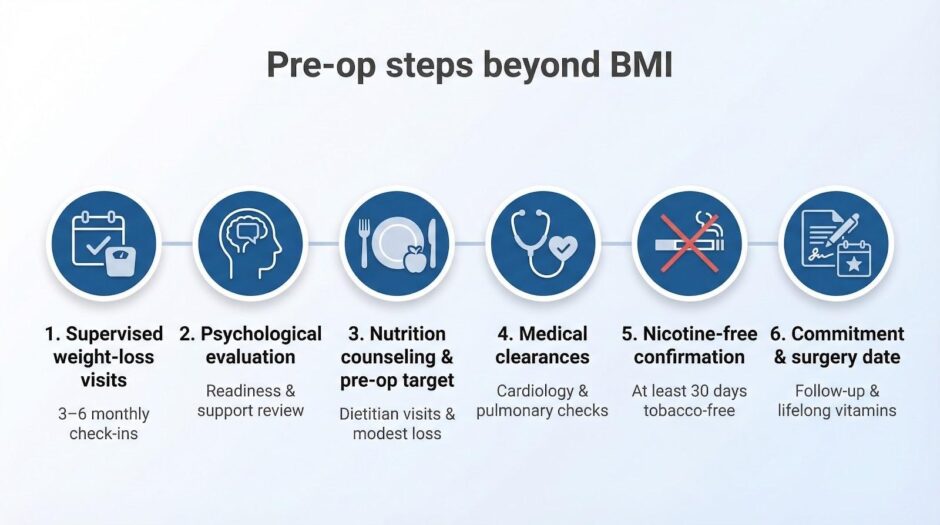
Documented weight-loss attempts
Insurers want proof you tried structured weight management first. Most plans require three to six consecutive visits with a physician or registered dietitian. Each note must list:
- Current weight and blood pressure
- Nutrition or exercise counseling provided
- A follow-up goal for the next visit
Reschedule a session and some carriers restart the clock, so lock these dates early and treat them as non-negotiable.
Psychological green light
Every insurer and surgical team requires a licensed psychologist or psychiatrist to confirm you are mentally ready for the lifestyle shift. During a one-hour conversation you will review:
- Eating triggers and stress patterns
- Substance use or past addiction treatment
- Support network at home and work
Conditions such as depression or anxiety are acceptable when treated and stable. Unmanaged binge-eating disorder or substance abuse pauses the process until therapy begins. Bring a brief weight-loss history, medication list, and names of key supporters—the evaluator includes these details in the report that lands in your insurance file exactly as written.
Nutrition counseling and pre-op weight targets
Most insurers will not approve surgery until your chart shows dietitian work. Plans typically need at least two dietitian notes; Medicaid and Aetna often ask for four or more. Each note must include your weight, a specific goal for the next visit, and any questions you raised. Keep copies—these pages prove you completed the “intensive behavioral therapy” step if an appeal arises.
During the first consult the dietitian maps your usual meals. Then you rehearse surgery-style eating: lean protein first, small bites, thirty slow chews. Portion practice shrinks liver fat, giving surgeons better visibility and faster operating times.
Surgeons may add a modest pre-op target, usually five to ten pounds for average-size patients or five percent of body weight when BMI exceeds sixty. The goal softens the liver so instruments fit safely; it is not a test of discipline.
Once the dietitian signs off and the scale shows progress, medical clearance and a surgery date follow quickly. Your next job is gathering the final paperwork so insurance cannot delay the big day.
Medical clearance and lifestyle commitments
Your surgery date appears only after a final safety check.
- Specialist approvals
- Cardiology evaluates heart function under stress.
- Pulmonology reviews sleep-apnea treatment.
- Anesthesia studies airway notes and current medications.
- Nicotine screen
Programs require a negative result for at least 30 days because tobacco constricts blood vessels and slows healing. - Commitment contract
You sign a document that lists follow-up visits, vitamin schedules, and routine bloodwork for life. Surgeons frame it as a clear handshake: they rebuild anatomy, you protect the investment.
Complete these steps and every requirement—BMI, paperwork, and medical safety—locks in. Insurance issues the authorization, the OR schedule opens, and your focus shifts to packing that first-day protein shake.
Conclusion
Colorado often claims the “fittest state” title, yet severe obesity continues to rise. The good news: policymakers and health systems now treat bariatric surgery as essential care rather than a last resort.

Proof arrived when Health First Colorado dropped its BMI floor to 30. Private insurers are following close behind; Aetna already wrote the lower threshold into its policy, and Cigna grants exceptions when diabetes stays uncontrolled.
Lawmakers are pushing too. Senate Bill 24-054, the Diabetes Prevention and Obesity Treatment Act, would require all commercial plans to cover bariatric surgery and anti-obesity medications. The bill stalled in committee but is expected to return next session with broad bipartisan support.
Hospitals are preparing for higher demand. Denver Health doubled its support-group calendar, UCHealth expanded telehealth slots for rural patients, and Centura added weekend nutrition classes at Parker Adventist. These moves create capacity for a younger, more medically complex patient pool.
Bottom line: Colorado now sits ahead of most states—broader Medicaid coverage, private insurers racing to match new science, and hospital systems scaling up. If your BMI and health history point toward surgery, the path to approval has never been clearer.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree