I. EMBRYOLOGY
A. Ectoderm: Epidermis, pilosebaceous glands, apocrine glands, eccrine sweat glands, nails
B. Mesoderm: Langerhans cells, macrophages, mast cells, Merkel cells, fibroblasts, blood vessels, lymph vessels, fat cells
C. Neuro-ectoderm: *Melanocytes, nerves, specialized sensory receptors
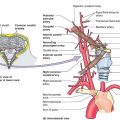
II. ANATOMY
A. Epidermis—outer layer
1. Cell types: Keratinocytes, melanocytes, Langerhans cells, Merkel cells
2. Superficial to deep: Stratum corneum, lucidum, granulosum, spinosum, basale
B. Dermis
1. Cell types: Collagen, elastin, ground substance
2. Nerves, blood vessels, lymphatics, muscle fibers, pilosebaceous/apocrine/ eccrine glands
3. Two layers superficial to deep
a. Papillary—fibroblasts, mast cells, histiocytes, Langerhans cells, lymphocytes
b. Reticular—thicker than papillary dermis
i. Extends to underlying fat
ii. Contains elastin with interspersed large collagen fibers.
III. BENIGN LESIONS
A. Epidermal lesions
1. Epidermal nevus (linear nevus)
a. May be associated with developmental abnormalities. Ocular, central nervous, skeletal cardiovascular, urogenital systems
b. Present at birth or early childhood.
c. Clinical presentation: Tan or brown warty papules
d. Anatomic location: Extremities
e. Treatment: Excision, laser therapy(CO2), dermabrasion, or cryotherapy
2. Inflammatory linear verrucous epidermal nevus
a. Present at birth or early childhood.
b. Clinical presentation: Erythematous, rough, scaly papules in linear array, extremely pruritic
c. Anatomic location: Extremities
d. Treatment: Excision or laser therapy (intense pulsed light)
3. Seborrheic keratosis
a. Derived from basal layer of epidermis. Cystic inclusions of keratinous material
b. Present in middle age around fifth decade.
c. Clinical presentation: Waxy, stuck-on appearance; warty papule or plaque May be yellow, light brown, dark brown, or black in color
d. Anatomic location: Head, neck, and trunk
e. Treatment: Dermabrasion, cryotherapy, shaving, and excision
______________
*Denotes common in-service examination topics
a. Occurs on sunlight-exposed skin
b. Most common pre-malignant skin lesion
i. *Approximately 5% to 20% will develop into squamous cell carcinoma
ii. May be present in transplant patients
iii. Require aggressive treatment due to high risk of malignant transformation.
c. Clinical presentation: Erythematous, rough, or scaly macules or papules
d. Anatomic location: Most commonly located on sunlight-exposed areas (scalp, ears, face, and hands)
i. Actinic chelitis (aggressive form involving lips)
ii. Histologically characterized by dyskeratosis, atypia in basal layer of epidermis
e. Treatment: Imiquimod 5% (Aldara) or 5-fluorouracil, cryotherapy, topical tretinoin
5. Verruca vulgaris
a. Common wart: Caused by human papillomavirus (HPV)
b. Clinical presentation: Scaly, rough appearance with a cap of friable keratotic material
c. Anatomic location: Variable. Lesions arise from stratum granulosum
d. Treatment: Cryotherapy, chemical ablation, or excision
6. Cutaneous horn
a. Clinical presentation: Well-circumscribed cone with hyperkeratotic features.
i. Resemble actinic keratoses
ii. Must be distinguished from squamous cell carcinoma
b. Anatomic location: Variable
c. Treatment: Excisional biopsy with careful evaluation of lesion base
7. Leukoplakia
a. Associated with chronic inflammation/irritation (Alcohol or tobacco)
b. *May degenerate into SCC
c. Clinical presentation: Mucosal lesion
i. White plaque exists on stratified squamous epithelium
ii. Cannot be wiped away
d. Anatomic location: Mucosal surface
e. Treatment: Removal of irritant, biopsy may be warranted
8. Keratoacanthoma
a. *Rapid growth phase followed by spontaneous regression
b. Clinical presentation: Firm, dome-shaped nodule
i. Prominent horn-filled central depression
ii. Keratin with thick epidermis
c. Difficult to distinguish from SCC
d. Treatment: Simple excision; may consider 5-fluorouracil for patients with multiple lesions.
B. Melanocytic lesions
1. Nevus of Ota
a. Found in patients with Asian ancestry
b. Appears at birth
c. Clinical presentation: Appears as large, blue-gray patch
d. Anatomic location: Areas innervated by first and second branches of trigeminal nerve
e. Treatment: Laser therapy (Q-switched Nd:YAG)
2. Nevus of Ito
a. Found in patients with Asian ancestry
b. Appears at birth
c. Clinical presentation: Appears as large, blue-gray patch
d. Anatomic location: Posterior shoulder and areas innervated by posterior supraclavicular and lateral cutaneous brachial nerves
e. Treatment: Laser therapy (Q-switched Nd:YAG)
a. Appears at birth
b. Clinical presentation: Tan patch with speckled hyperpigmented macules and papules
c. Anatomic location: Commonly on trunk
d. Treatment: Observation, laser therapy (intense pulsed light), or simple excision
4. Spitz nevus (benign juvenile melanoma)
a. Appears in childhood or early adulthood
b. Clinical presentation: Pink or tan, dome-shaped, smooth plaque
c. Anatomic location: Commonly located on face
d. Treatment: Excision with margins to decrease recurrence risk (range from 1 to 2 mm to 1 to 2 cm depending on concern for melanoma)
e. May be difficult to distinguish histologically from malignant melanoma
5. Junctional nevus
a. Nevus cells located at epidermal-dermal junction
b. Appears in childhood or early adulthood
c. Clinical presentation: Brown, evenly pigmented macule with well-defined borders
d. May be difficult to differentiate from melanoma
e. Anatomic location: Most commonly on trunk
f. Treatment: Simple excision
6. Compound nevus
a. Contains both junctional and intradermal components.
b. Appears in childhood or early adulthood.
c. Clinical presentation: Appears a dark-brown papule with regular borders
d. Anatomic location: Most commonly on trunk
e. Treatment: Simple excision
7. Intradermal nevus
a. Located entirely within the dermis.
b. Appears in the second or third decade of life
c. Clinical presentation: Appears as a flesh-colored or light tan papule
d. Anatomic location: Face or neck
e. Treatment: Simple excision
8. Common blue nevus
a. Appears during adolescence
b. Clinical presentation: Blue or blue-black papule
c. Anatomic location: Head, neck, and dorsum of hands/feet
d. Treatment: Simple excision
e. Cutaneous metastasis of malignant melanoma can resemble blue nevus
9. Cellular blue nevus
a. Appears after second decade of life
b. Clinical presentation: Blue-black papule
c. Anatomic location: Most commonly on buttocks
d. Treatment: Simple excision
10. Atypical (dysplastic) nevus
a. Patients with dysplastic nevi and a family history of melanoma in a first-degree relative are at a high risk of melanoma.
b. Regular skin examination
c. Appear after puberty
d. Clinical presentation: Appears as a central brown macule with irregular pink rim.
e. More irregular pigmentation and borders compared with typical nevi.
f. Anatomic location: Trunk
g. Treatment: Excision with margins to prevent recurrence
i. Total body skin examination to rule out other lesions
ii. Sunscreen and avoidance of sunburning/tanning
C. Adnexal tumors
1. Background
a. Excised for aesthetic reasons
b. Normal relationship between epithelial and stromal components of skin altered
c. May be classified as nevus, adenoma, or epithelioma
d. May include sebaceous glands, hair follicles, apocrine, or eccrine sweat glands
2. Hair follicle tumors
a. Located in lower dermis and subcutaneous fat
b. Pilomatrixoma (calcifying epithelioma of Malherbe)
i. Typically seen in younger patients (<20 years old)
ii. Clinical presentation: Single, solid subdermal nodule
a) Positive tent sign—stretching of overlying skin yields multiple peaks
b) Difficult to distinguish from calcified masses or carcinoma.
c) On pathology shows epidermoid cells with basophilic and eosinophilic cells
iii. Anatomic location: Involves face and upper extremities
iv. Treatment: Excision (with up to 1 to 2 cm margins) with up to 10% recurrence rate
c. Trichofolliculoma (hair follicle nevus)
i. Clinical presentation: <1 cm and skin-colored
ii. Anatomic location: On face with thin pale hairs
iii. Treatment: Excisional biopsy for management
d. Trichoepithelioma
i. Involves patients after puberty
ii. Rasmussen syndrome is an autosomal dominant disorder that is a triad of multiple trichoepitheliomas, cylindromas, and milia.
iii. Clinical presentation: Appears pink or flesh-colored
iv. May be difficult to distinguish clinically and histologically from basal cell carcinoma
v. Anatomic location: Multiple trichoepitheliomas may have symmetric distribution around face and eyes
vi. Treatment: Electrodesiccation
e. Trichilemmoma
i. Cowden disease (multiple hamartoma syndrome) should be suspected if patients have multiple such tumors
ii. Glycogen-rich epithelial cells surrounded by sheaths of cells resembling hair follicles on histology
iii. Clinical presentation: Smooth papule
iv. Anatomic location: Found on scalp or other hair-bearing regions. Association with nevus of Jadassohn if on scalp. Warrants biopsy
v. Treatment: Laser therapy (CO2), electrodessication with curettage, or simple excision due to similar appearance with BCC and trichilemmal carcinoma
3. Eccrine tumors
a. Cylindroma (turban tumor or tomato tumor)
i. Appears in early adulthood
ii. Multiple cylindromas may indicate autosomal dominant cylindroma syndrome.
iii. Clinical presentation: Appears as firm, smooth pink nodules
iv. Anatomic location: Often located on scalp
v. Treatment: Laser therapy (CO2), electrodessication/curettage, cryotherapy, or simple excision
b. Eccrine poroma
i. Clinical presentation: Firm, papular or nodular lesions surrounded by rim of hyperkeratosis; may appear pedunculated
ii. May resemble amelanotic melanoma and pyogenic granuloma
iii. Anatomic location: Found on palms and soles of feet
iv. Treatment: Simple excision
c. Syringoma
i. Appears in early adulthood
ii. May have increased incidence with Down’s syndrome
iii. Clinical presentation: Small papules ranging from yellow to pink in color. May be confused with xanthelasma or trichoepithelioma
iv. Anatomic location: Most commonly appears in the periocular region (eyelids, upper cheek) but may involve trunk, neck, or extremities
v. Treatment: Laser (CO2) or electrodesiccation
d. Eccrine spiradenoma
i. Appears in young adults
ii. Clinical presentation: Tenderness or pain with manipulation
iii. May be mistaken for glomus tumor
iv. Anatomic location: Appears as a single nodule on ventral upper half of body
v. Treatment: Simple excision if symptomatic
e. Eccrine hidrocystoma
i. Dilated and obstructed sweat ducts histologically
ii. Clinical presentation: Translucent vesicles
iii. Swell in heat/humidity; regress in cooler/dry climate
iv. Anatomic location: Appears on lower eyelids and upper cheeks
v. Treatment: Puncture to release pressure
4. Sebaceous tumors
a. Sebaceous nevus of Jadassohn
i. Appears at birth
ii. *After puberty, 10% to 15% degenerate into BCC. May also develop SCC or keratoacanthoma
iii. Clinical presentation: Appears as yellow/orange, waxy, smooth plaques prior to puberty
iv. Appear as rough, verrucous, orange plaques after puberty
v. Anatomic location: Most commonly found on scalp
vi. Treatment: Excision
b. Sebaceous hyperplasia
i. Appears in middle or late age
ii. Clinical presentation: Appears as shiny, small umbilicated, yellow-white papules
iii. May be covered with telengiectasia
iv. Anatomic location: Most common on face
v. Treatment: Cryotherapy, electrodesiccation, or laser (intense pulsed light or CO2)
vi. May be excised due to similar appearance with BCC.
c. Sebaceous adenoma
i. Appears in middle age
ii. *May be associated with Muir-Torre syndrome—an autosomal dominant syndrome associated with multiple keratoacanthomas, marked increase in visceral neoplasm
iii. Clinical presentation: Yellow nodules
iv. Anatomic location: Located primarily in head and neck
v. Treatment: Simple excision
5. Apocrine tumors
a. Apocrine cystadenoma
i. Contains brown or blue tinged fluid
ii. Clinical presentation: Appears as a single translucent nodule
iii. Anatomic location: Most common on face
b. Chondroid syringoma
i. Composed of sweat gland (epithelial) and cartilaginous elements (mesenchymal) on histology
ii. Treatment: Excisional biopsy
c. Syringocystadenoma papilliferum
i. Appears during childhood
ii. Clinical presentation: May be associated with nevus sebaceous
iii. Nearly 10% will harbor BCC
iv. Anatomic location: Most commonly found on scalp
v. Treatment: Excision
1. Leiomyoma
a. Abnormal proliferation of smooth muscle
b. May become symptomatic with pain on exposure to cold/pressure
c. Clinical presentation: Appears as firm, pale intradermal nodules with brown hue
d. Treatment: Excisional biopsy
e. Local recurrence may occur
f. Malignant degeneration to leiomyosarcoma is rare
E. Cysts
1. Epidermal inclusion cyst (epidermoid cyst)
a. May be incorrectly called a sebaceous cyst; however, not sebaceous in origin
b. Appears in adulthood
c. Clinical presentation: Fluctuant, flesh-colored, well-circumscribed nodules
i. Punctum may be visible
ii. Contains foul-smelling keratinous debris
d. Anatomic location: Commonly found on face, neck, and trunk
e. Treatment: Simple excision if uninfected; if infected, perform incision and drainage with interval excision
2. Dermoid cyst
a. Appears at birth or early childhood
b. Clinical presentation: Similar to epidermal inclusion cysts. Lined with epidermal skin appendages
c. *Anatomic location: Most commonly found along supraorbital ridge, lateral brow, or nasal midline
d. Treatment: Excision
e. *Midline nasal mass differential diagnosis
i. Dermoid cyst, glioma, meningocele/encephalocele
ii. CT or MRI prior to excision to determine intracranial extension
3. Trichilemmal cyst
a. Pilar cyst
b. Appear in adulthood
c. Clinical presentation: Similar to an epidermal inclusion cyst
d. Anatomic location: Most commonly found on scalp
e. Treatment: Excision if uninfected; if infected, incision and drainage with interval excision
F. Fibrous Lesions
1. Dermatofibroma
a. Appears in adulthood
b. Clinical presentation: Brown-red indurated papule or nodule Positive dimple sign—when squeezed it sinks
c. Anatomic location: Most common lower extremities
d. Treatment: Simple excision
2. Angiofibroma
a. Clinical presentation: Pale, firm papule. May have telengiectasia or erythema
b. Anatomic location: Most commonly on lower third of face
c. Treatment: Simple excision for cosmesis
d. May be associated with tuberous sclerosis if multiple
3. Lipoma
a. May be present at any age
b. Clinical presentation: Painless, soft, flesh-colored nodule
c. Anatomic location: Commonly found in the trunk and extremities
d. Treatment: Simple excision
4. Dermatofibrosarcoma protuberans
a. Appears in middle age
b. Clinical presentation: As a reddish-brown, firm, nodular plaque
c. Anatomic location: More commonly found on trunk, extremities
d. *Treatment is radical excision due to locally aggressive behavior. Margins >3 cm if possible
e. Local recurrence is common; however, metastasis is rare.
5. Neurofibroma
a. Composed of Schwann cells and endoneurial fibroblasts.
b. May appear at any age
c. Clinical presentation: Soft, compressible, flesh-colored or pink nodules; button-hole sign (can be pushed deeper into dermis)
d. Anatomic location: More common on the trunk and extremities
e. Treatment: Excision
f. Multiple neurofibromas may be associated with neurofibromatosis type I or II
i. *Type I—Cafe-au-lait spots, Lisch nodules (iris hamartomas), and optic nerve glioma
ii. Type II—bilateral acoustic neuroma
IV. OTHER DISORDERS
A. Calciphylaxis
1. Metastatic calcification resulting in calcification of blood vessels and necrosis of surrounding tissue.
2. Associated with renal failure
3. May appear at any age; more common in women
4. Clinical presentation: As necrotic ulcerations with red-blue mottling of skin (livedo reticularis)
5. Anatomic location: Common trunk and extremities
6. Treatment: Supportive care, phosphate-binding agents, parathyroidectomy, intravenous sodium thiosulfate, or excision
7. Excision often results in progressive calcification
B. Hidradenitis suppuritiva
1. Clinical presentation: Chronic inflammation and infection of the apocrine sweat glands. May result in chronic draining sinus tracts and abscesses.
2. Anatomic location: Most commonly affects axillae, breasts, perineum, and buttocks.
3. Treatment: Topical clindamycin, oral or IV antibiotics, excision of involved tissue. Following excision, reconstruction can occur via healing by secondary intention or by placement of a skin graft.
C. Xeroderma pigmentosum
1. Autosomal recessive disorder affecting DNA repair
2. High risk for SCC, BCC, and melanoma
3. Treatment: Avoidance of sunlight, isotretinoin, 5-fluorouracil, or excision of malignant lesions
D. Dystrophic epidermolysis bullosa
1. Hereditary disease with bulla formation of skin/mucosa following minor trauma
2. May result in encasement of digits with scar tissue
3. Treatment: Scar release/Z-plasty, topical steroids, avoidance of trauma
E. Cutis laxa
1. Defect in elastic fibers
2. Skin hangs loose from folds
3. Premature aging
4. Wound healing unaffected
5. Blepharoplasty and face lift can be beneficial
F. Pseudoxanthoma elasticum
1. Affects elastic fibers and collagen
2. Skin thickens and appears cobblestoned with mechanical stress
3. Wound healing is normal
G. Ehlers-Danlos syndrome (cutis hyperelastica)
1. Autosomal recessive or x-linked
2. Hyperextensible skin, severe joint laxity
3. Blood vessels are delicate
4. *Wound healing is abnormal: Approach surgery with caution
H. Acne vulgaris
1. Appears in younger patients
2. Clinical presentation: Comedones, inflammatory cysts, seborrheic plaques
3. Anatomic location: Face
4. Treatment: Topical retinoic acid, oral antibiotics, antibiotic pads, and oral isotretinoin (accutane). Isotretinoin—risk of birth defects; patients must have two forms of contraception. Avoid if planning aesthetic facial rejuvenation with lasers or peels.
I. Acne rosacea
1. Clinical presentation
a. Facial flushing (increased vascularity)
b. Thickened skin erythema, telangiectasia
c. Acne rosacea (papules and pustules)
d. Rhinophyma—nasal skin becomes erythematous with telangiectatic changes
2. Anatomic location: Affects forehead glabella, malar region, nose, chin
3. Treatment: Oral antibiotics, retinoic acid, dermabrasion, cryotherapy, laser (CO2), tangential excision (for Rhinophyma)
4. Reconstruct with secondary contraction versus skin graft
J. Pyoderma gangrenosum
1. Clinical presentation: Multiple superficial abscesses with significant ulceration and skin necrosis.
2. Should get a dermatology consult and biopsy to evaluate, though this is a diagnosis of exclusion.
3. Treatment: Broad spectrum antibiotics
4. Approach surgery with caution given chances that this could create a flare and spreading of the disease.
5. Harvesting STSG can also create a flare of the disease at the donor site.
6. Associated with ulcerative colitis
PEARLS
1. Keratoacanthomas are characterized by rapid growth and spontaneous regression; they are difficult to distinguish from squamous cell carcinomas although they are not malignant.
2. Nevus sebaceous has a 10% to 15% risk of malignant degeneration into BCC. Excision is warranted.
3. Patients with cutis laxa do not have impaired wound healing and can be candidates for surgery, while those with cutis hyperelastica have wound healing difficulties and may not tolerate surgery.
4. 5-Fluorouracil is a DNA synthesis inhibitor; imiquimod (Aldara) is an immunomodulator.
5. Excision is generally appropriate when definitive pathology and/or margins are required.
6. Keep in mind the amount of local anesthetic which can be used (e.g., 1% lidocaine vs. 1% lidocaine with epinephrine).
7. When drawing up lidocaine for excision, avoid displaying needle.
8. Identify lesion and its observable borders prior to injection with lidocaine to avoid obscuring the lesion boundaries.
9. Design excisions as ellipses with sharp corners to facilitate closure and avoid dog-earing.
10. Nylon stitches from the face should be removed in 5 days to avoid railroad tracks. Stitches on back should be left in for 2 weeks to allow for more robust healing and to avoid splitting apart.
QUESTIONS YOU WILL BE ASKED
1. What is the recommended treatment of a nevus sebaceous?
Excision with clear margins.
2. What is the risk of malignant transformation of an actinic keratosis, and what type of skin cancer can it progress to?
Rates of AK progression to SCC were calculated at 0.6 percent at one year and 2.6 percent at four years. Of these SCCs, 75 percent were considered invasive and the remainder were in situ.
3. Patients with which of the following disorders should be approached with caution when considering surgical intervention: Cutis laxa? Pseudoxanthoma elasticum? Ehlers-Danlos?
Patients with Ehlers-Danlos syndrome may suffer from excessive postoperative bleeding and poor wound healing and therefore surgery is generally contraindicated.
4. What is the most common location of dermoid cysts?
Periocular region.
5. What malignancy can Spitz nevi appear histologically similar to?
Melanoma.
Recommended Readings
Lee EH, Nehal KS, Disa JJ. Benign and premalignant skin lesions. Plast Reconstr Surg. 2010;125:188e–198e. PMID: 20440130.
< div class='tao-gold-member'>