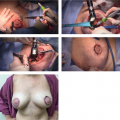
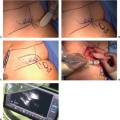
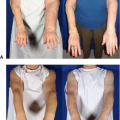
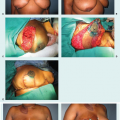
Avoiding Pitfalls in Symmetry Procedures Following Unilateral Autologous Versus Implant-Based Reconstruction
Michele A. Shermak
History
Breast reconstruction is performed in women post lumpectomy or mastectomy for breast cancer treatment. Over 100,000 breast reconstruction procedures are performed annually (1). Unilateral acquired defects are more common than bilateral presentations, and initial reconstruction is focused on creating an aesthetic breast post partial or total mastectomy, in an immediate, delayed, or staged fashion. To achieve symmetry with the reconstructed breast, plastic surgical procedures are often necessary for the contralateral, otherwise unaffected breast, particularly with implant reconstruction. In 1998 President Clinton mandated that insurance companies cover reconstructive surgery on both breasts in breast cancer patients, even with unilateral cancer, so more women are able to pursue contralateral symmetry surgery since insurance covers it. This mandate also came at a time when breast reconstruction outcomes were providing more superb aesthetic results not only in clothing but undressed and more women were opting to undergo reconstruction, encouraged by other cancer survivors and their treating physicians. Breast reconstruction prevalence has increased almost 30% since 2000 (1). Pedicled TRAMs were routine in the 1990s, and perforator flaps were starting to join the mainstream. Over time, less-invasive mastectomy approaches have allowed improved aesthetic outcomes, such as skin-sparing patterns, ultimately followed by nipple-sparing techniques (2,3). Women are experiencing greater aesthetic results of their reconstructed breast, often surpassing their preoperative appearance, so the need for the opposite breast to match and look as good as the reconstructed breast became increasingly accepted and expected.
The best option for the best match is undergoing contralateral prophylactic mastectomy (CPM) with symmetrical mastectomy and reconstructive procedures. This practice is controversial in that the risk of contralateral cancer has proven to be low while the risk of complications associated with contralateral mastectomy and reconstruction are considerable (4,5). It has been demonstrated that the 10-year cumulative risk of developing a contralateral breast cancer in women who were initially diagnosed with unilateral disease is 6% to 7%, and that the 20-year incidence is 9% (6,7). While CPM is recommended for patients with genetic or treatment-based (Mantle radiation) predisposition for breast cancer, the application of CPM to achieve symmetry is a standard some centers follow, but not most (8).
As CPM is not universally accepted, symmetry procedures after unilateral mastectomy reconstruction have become the necessary challenge to meet. Contralateral procedures for symmetry are more necessary after implant-based reconstruction relative to autologous techniques, as the main goal of autologous breast reconstruction is to maintain the volume, shape, and dimensions of the breast undergoing mastectomy (9). With microsurgical techniques gaining greater prevalence over pedicled reconstructions, greater volumes of tissue may be more safely transferred, and skin-sparing mastectomy approaches have also resulted in reduced need for contralateral symmetry procedures (2,6). Despite improved outcomes in autologous reconstruction, implant reconstruction rates are growing due to acceptance of nipple-sparing mastectomy (NSM), acellular dermal matrices, and greater implant options (10). With the shift in higher utilization of implant reconstruction, there is an even greater need currently for contralateral symmetry procedures.
It is understood that contralateral breast surgery should not impair screening for breast cancer, and this is supported by data. It has been determined that mammographic accuracy, sensitivity, and specificity are not affected by the glandular rearrangement (11).
While contralateral surgery may be performed immediately at the time of cancer resection and reconstruction, when performed at a second stage, symmetry is better guaranteed, allowing the breast reconstruction to
fully heal and settle. The best long-term result is the one that settles least, and breast implant reconstruction has resulted in the best outcomes through objective testing. Breast lift and breast reduction techniques change most over time with age, weight changes, and medications necessary for cancer treatment, with increasing ptosis and size, leading to less predictability over the long term relative to implant reconstruction. Over time, the literature has focused greater interest on the “if” over the “what” with regard to contralateral symmetry procedure: patient satisfaction versus what procedure to do. Symmetry is the key to long-term successful outcome and patient satisfaction after breast cancer treatment (12,13).
fully heal and settle. The best long-term result is the one that settles least, and breast implant reconstruction has resulted in the best outcomes through objective testing. Breast lift and breast reduction techniques change most over time with age, weight changes, and medications necessary for cancer treatment, with increasing ptosis and size, leading to less predictability over the long term relative to implant reconstruction. Over time, the literature has focused greater interest on the “if” over the “what” with regard to contralateral symmetry procedure: patient satisfaction versus what procedure to do. Symmetry is the key to long-term successful outcome and patient satisfaction after breast cancer treatment (12,13).
The toolbox for contralateral breast symmetry surgery includes implants and/or breast lift, or breast reduction. Fat transfer also may be incorporated in the reconstructive strategy.
Indications
Implants
Implant placement in the contralateral breast may be performed when the woman undergoing mastectomy and reconstruction decides she wants to aim for a higher volume, fuller breast post mastectomy reconstruction. This is common for women who are younger, thinner, postpartum, and/or have deflated breasts without significant ptosis. Optimal patients for contralateral implant procedures include those who undergo NSM with immediate prepectoral reconstruction, non-NSM with expander reconstruction above or below the pectoralis major with later conversion to a breast implant, or autologous reconstruction.
In women who hope to achieve a final breast volume comparable to baseline, reconstruction with shaped textured implants particularly in the prepectoral position may achieve acceptable symmetry to the contralateral breast; however, due to the greater documented risk of BIA-ALCL with textured implants, more implant-based reconstructions include smooth round implants which provide more upper pole volume, and a need to match this with an implant or fat on the uninvolved breast (14).
Breast Lift
Breast lift of the contralateral breast is performed in women with ptosis who have satisfactory volume match, or in women whose contralateral breast becomes relatively more ptotic after radiation treatment which results in more fibrosis, scarring, and a tighter breast envelope on the cancer side. Breast lift may be performed with an implant and/or fat transfer to achieve better volume symmetry and to obtain more optimal upper pole fullness which better matches the upper pole on the reconstructed side, more common with implant reconstruction. It is important for the patient to understand that breast lift may not provide symmetry over the long term and future adjustments may be necessary for breast changes secondary to weight gain, aging, and decreased tissue strength leading to future ptosis.
Breast Reduction
Contralateral breast reduction more often applies to women who are older, have a larger BMI and/or a large breast size with ptosis, or in women who have undergone lumpectomy and radiation for breast conservation which does not conserve symmetry. Breast reduction pairs well with a staged implant reconstruction associated with total mastectomy in which the nipple cannot be spared; autologous reconstruction with a volume reduced from baseline; or lumpectomy and oncoplastic reconstruction followed by radiation therapy. Breast reduction helps achieve three-dimensional symmetry, including width, length, contour, and volume of the mastectomy reconstruction. As with breast lift, patients need to be informed of changes anticipated in the reduced breast over time that may require revision surgery to restore symmetry, particularly with implant reconstruction of the cancer side.
Fat Transfer
While fat transfer is a useful tool for reconstruction post mastectomy, filling in defects left unfilled by implants, camouflaging rippling under thin skin flaps, or smoothing transition of the reconstructive border with flaps or implants, fat is also an ideal adjunct to enhancing the contralateral breast, improving volume and size, as well as creating upper pole fullness, with autologous tissue properties that avoid the need for foreign material. Fat transfer optimization is an active area of study that will continue to evolve to allow greater success with larger volumes of fat and improvement of survival with reduction of absorption.
Contraindications
Contraindications to symmetry procedures hinge on the cancer status, personal preference, and medical comorbidities of women undergoing breast cancer treatment. Women might not opt for contralateral surgery due to aversion to noncritical surgical procedures, relying on special bras and prosthetic inserts to achieve a more symmetrical appearance in clothing. Women with aggressive breast cancer requiring adjuvant therapies and particularly poor prognosis should delay contralateral surgery, but these issues, which previously were total contraindications, have become relative contraindications. Women with medical issues such as severe cardiopulmonary diseases are not candidates for elective symmetry surgical procedures. High BMI, dependence on blood thinners, and tobacco use present relative contraindications to any surgical procedure. Scarring and prior surgery on the contralateral breast may limit options regarding techniques used for symmetry.
Preoperative Planning
Reconstructive planning accounting for the goal of symmetrical breasts may take place at the time of initial consultation, even if staging is necessary. Plans must be made in conjunction with the breast oncologic surgeon. Decisions impacting reconstructive planning depend on whether the nipple areolar complex (NAC) may be spared; if lumpectomy or mastectomy is mandated; if oncoplastic approach is possible; if there are plans for adjuvant chemo- or radiation therapy, either before or after mastectomy; and the prognosis of the patient. Reconstructive planning for contralateral surgery depends on patient acceptance of contralateral surgery versus attempting to create the best match to the native breast, most possible with autologous reconstruction. Surgical plans for the contralateral breast may evolve after mastectomy and reconstruction, depending on the degree of asymmetry and patient acceptance of this. There is no specific time surgery must be done on the opposite breast: contralateral breast surgery may be performed immediately at the time of mastectomy; delayed 4 to 6 months after mastectomy and reconstruction; or beyond that if the patient needs more time to recover from adjuvant treatments or does not feel ready for contralateral surgery.
Reconstructing the contralateral breast in a later stage is beneficial for optimizing aesthetic outcome and symmetry. Delaying contralateral surgery to a second stage allows for healing and settling of the reconstructed breast; and dealing with any wound-healing complications or scarring fibrosis after mastectomy and reconstruction. The patient also may be stronger for second-stage surgery over performing single-stage surgery. If there is a need for additional contralateral volume, women may be sized with implants or with three-dimensional imaging to best plan for a matching implant. Measurements are also more reliable in considering delayed contralateral breast reduction or lift, depending on how the reconstructed breast settles after mastectomy/reconstruction. Radiation therapy may be required in treatment, and allowing for contraction of breast dimensions will afford better contralateral symmetry as well.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree