Lower eyelid function and appearance depend on the complex anatomic relationship between the soft tissue lamellae, supportive tarsoligamentous sling, and bone. Aging in the lower lid area may be caused by changes in the anterior lamella (skin and orbicularis oculi muscle), middle lamella (orbital septum and lower lid fat pads), posterior lamella (tarsus, lower eyelid retractors, and conjunctiva), tarsoligamentous sling (lateral retinaculum), or any combination of the previously described.
Key points
- •
Both the lateral and medial canthal regions contain critical anatomy implicated in lower blepharoplasty surgery.
- •
The arcus marginalis and orbicularis retaining ligament are distinct structures with separate, functional implications in lower blepharoplasty surgery.
- •
The lateral retinaulum is a complex structure with contributions from the lateral horn of levator aponeurosis, the lateral canthal tendon, the tarsal strap, Lockwood suspensory ligament, Whitnall ligament, and check ligaments of the lateral rectus muscle.
Introduction
The purpose of this article is to review basic soft tissue anatomic concepts that should help plastic surgeons better understand the complex dynamics of lower eyelid. A nuanced understanding of the orbital and periorbital 3-dimensional anatomy will translate into accurate and targeted pathoanatomic examinations, appropriate lower blepharoplasty decision making, technical finesse, and predictable lower blepharoplasty outcomes with minimized risk.
Discussion
Skin, Orbicularis Muscle, Orbicularis Retaining Ligament, and Arcus Marginalis
The lower eyelid skin is elastic and thin. It adheres tightly to the underlying sphincter-like orbicularis oculi muscle, which is divided into its pretarsal, preseptal, and preorbital anatomic portions. Together, skin and orbicularis oculi muscle make up the eyelid’s anterior lamella.
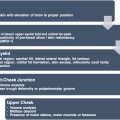
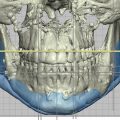
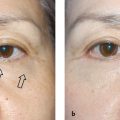
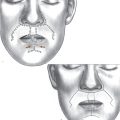
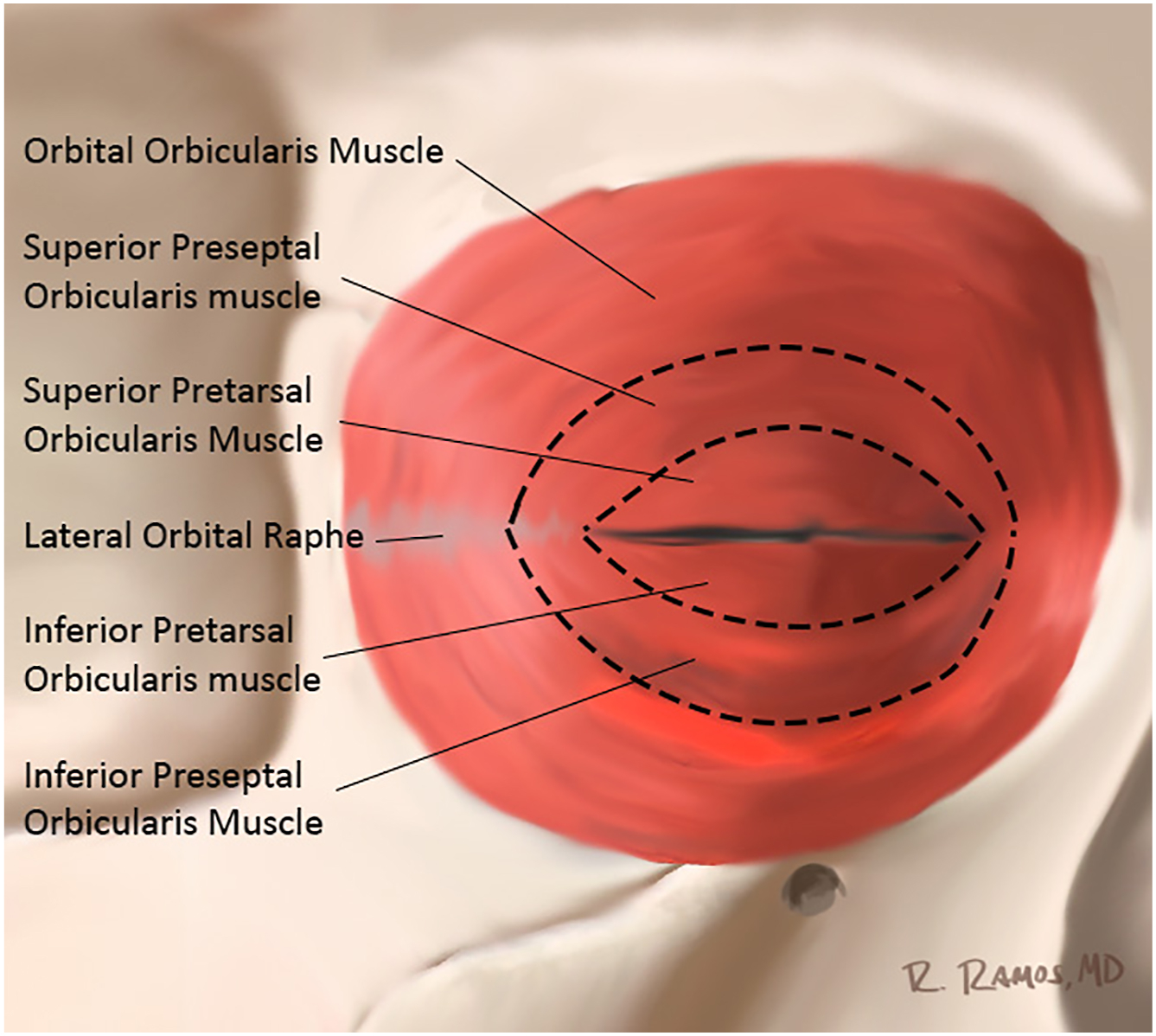
The orbicularis retaining ligament (ORL) separates the eyelid from the malar cheek at the lid-cheek junction. The orbicularis retaining ligament, also known as the orbitomalar ligament, traverses the periosteum of the lower orbital rim to the fascia of the deep surface of the orbicularis oculi and skin, providing an attachment between the 2 structures ( Fig. 1 ). With aging, laxity in these 2 structures can lead to nasojugal and palpebromalar grooves. In doing so, the ORL demarcates the prezygomatic space from the preseptal space. This prezygomatic space is bound superiorly by the ORL, inferiorly by the zygomatic cutaneous ligaments, posteriorly by preperiosteal fat and bone, and anteriorly by the suborbicularis oculi fat and orbicularis muscle ( Fig. 2 ). It also distinguishes the preseptal orbicularis from the orbital orbicularis ( Fig. 3 ). Medial to the medial corneal limbus, the ORL is commonly referred to as the tear trough ligament. In this area the orbicularis oculi is tightly adherent to the medial infraorbital rim and therefore hidden. Lateral to the medial cortical limbus, the ORL takes on a bilamellar structure that increases in length until it reaches the arcuate expansion. It then shortens again, and eventually fuses with the lateral orbital thickening. In lower lid blepharoplasty, the ORL may be released to mobilize the preseptal orbicularis and achieve tightening and suspension as an orbicularis muscle flap, sewing it to the lateral orbital rim. The ORL is most prominent centrally and diminishes medially and laterally to the lateral canthal region.
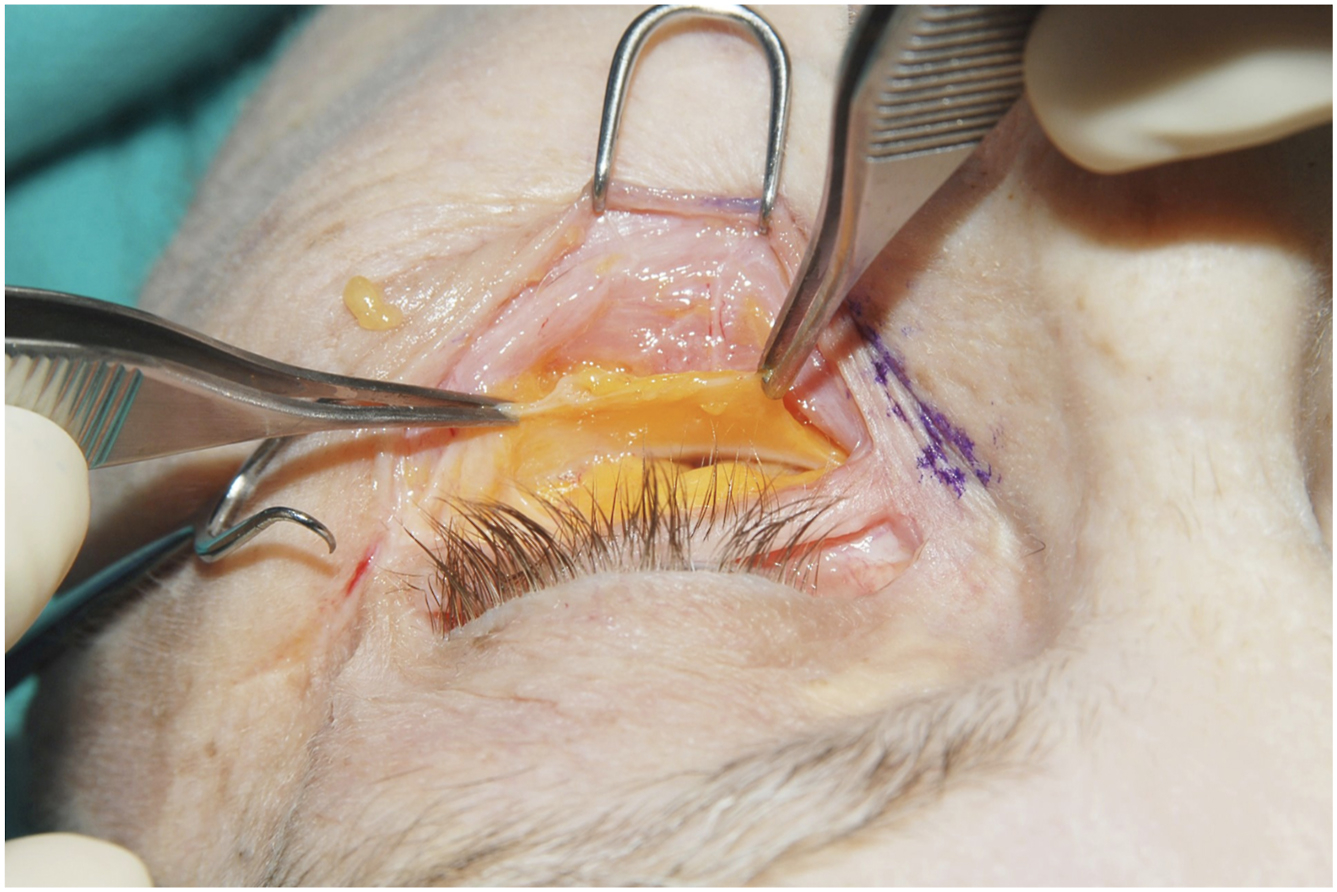
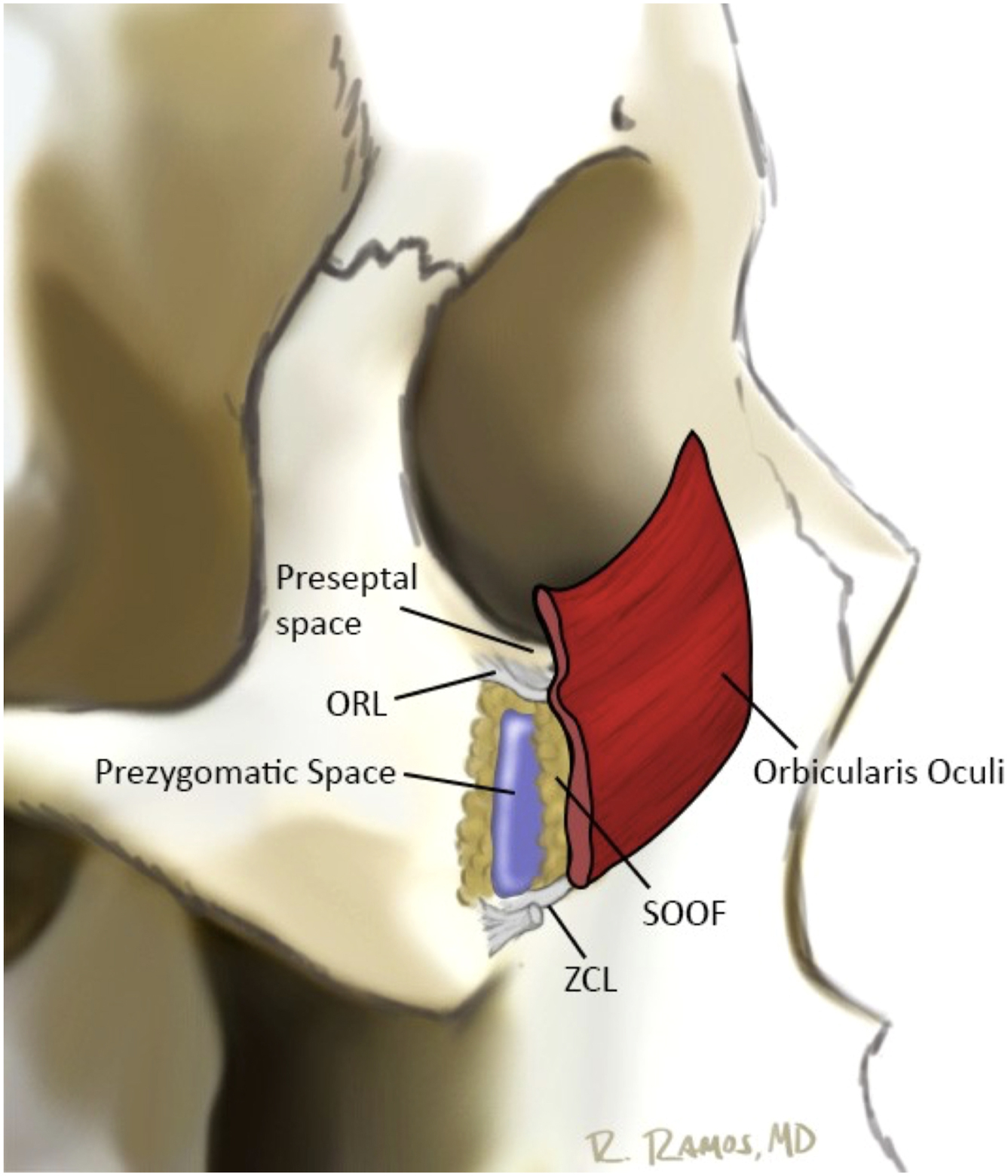
The arcus marginalis is an entirely distinct periorbital structure. It differs from the orbicularis retaining ligament in composition, location, attachment, function, and clinical relevance. The orbicularis retaining ligament is ligamentous in nature and spans the orbital periosteum to the deep surface of the orbicularis oculi. The arcus marginalis, on the other hand, is a fibrous structure formed by the fusion of the orbital rim periosteum with the orbital septum. The arcus marginalis is located at the orbital rim while the ORL attaches to the periosteum of the orbital rim approximately 2 to 3 mm superior to the arcus marginalis. Functionally the arcus marginalis serves as an attachment point for the lower septum while the ORL acts to function as an attachment point for the orbicularis.
Release of the arcus marginalis allows one to connect the orbital fat with the preperiosteal or subperiosteal plane while avoiding insult to the septum. In patients who have pseudoherniation of orbital fat, and specifically in those with tear trough deformities or palpebral malar groove, release of the ORL allows access to the anterior orbital rim. As an alternative to orbital fat excision, fat can then be repositioned onto the anterior orbital rim obliterating the tear trough. Hamra modified this technique to involve incising the arcus marginalis and repositioning septum and fat onto the anterior orbital rim. He coined this the septal reset.
Orbital Septum
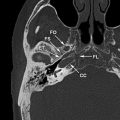
The orbital septum forms the middle lamella of the lower eyelid ( Fig. 4 ). Its inelastic fibrous composition contributes to its ability to confer structural support to the orbital contents. It retains some elasticity consistent with the mobility of the lower lid. The septum is of variable thickness, with the lateral tissues thicker than the medial aspect and composed of layers of thin membranous tissues.
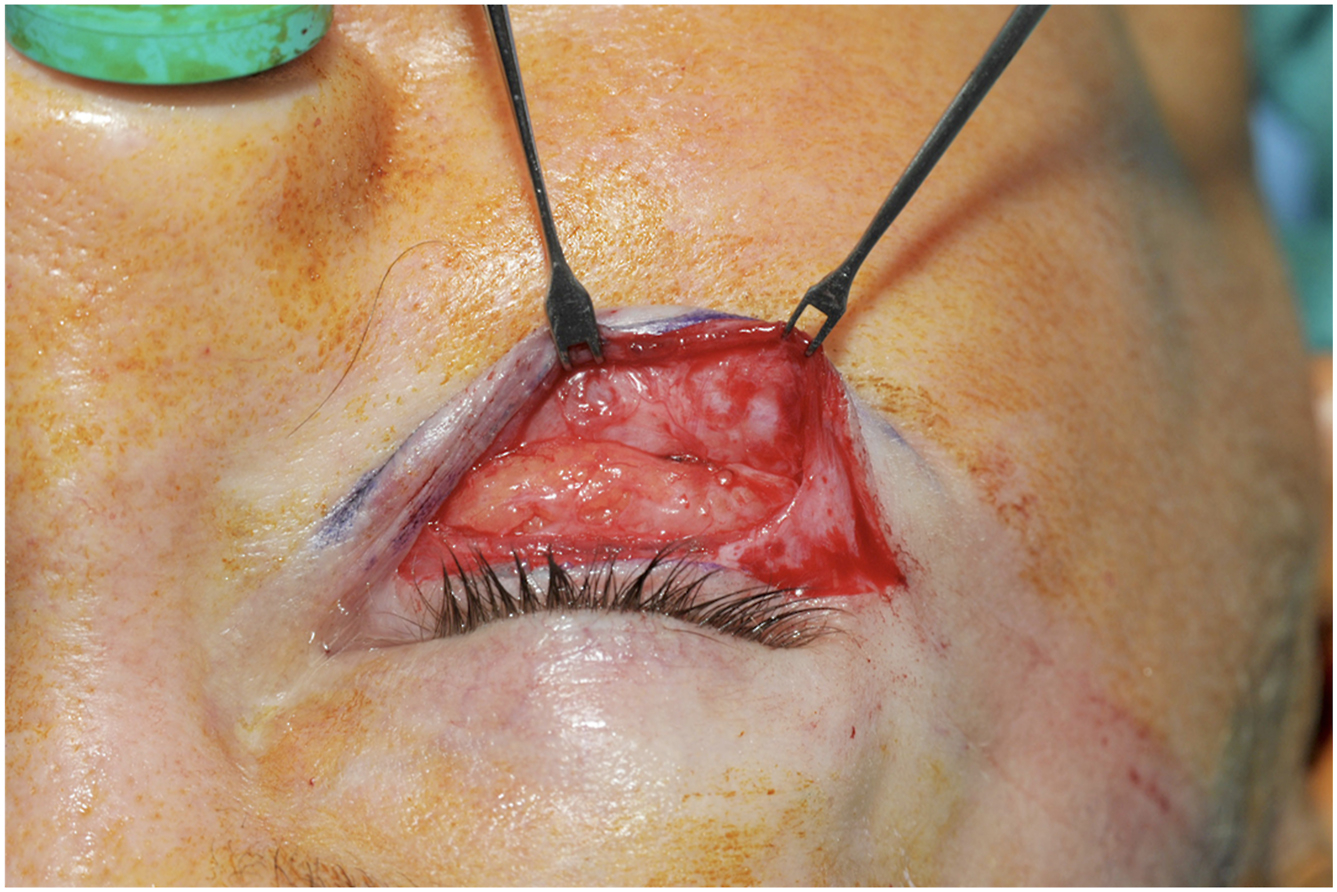
The lower lid septum originates from the arcus marginalis. In Caucasian individuals, the septum meets the lower lid retractors approximately 5 to 6 mm inferior to the lower margin of the tarsus, while in Asian individuals, it joins the lower lid retractors approximately 3 mm inferior to the lower tarsal margin. The attachment of the capsulopalpebral fascia (CPF) with the septum divides the lower lid septum into 2 clinically relevant components: a superior orbital septum and an inferior septum.
The anterior surface of the lower lid orbital septum, as well as the capsulopalpebral fascia inferior to the tarsus, is covered with the suborbicularis oculi fascia, which consists of relatively lax fibrous connective tissue. , , The corresponding tissue of the upper eyelid, the suborbicularis adipose layer, consists of higher adipose content and has less fibrous quality. There exists the recess of Eisler at the inferolateral aspect of the orbital septum toward the zygoma. This space, along with the structural qualities of the septum, allows for lower periorbital fat to exist beyond the boundaries of the inferolateral orbital rim. , By contrast, periorbital fat at the medial lower lid lies millimeters superior to the inferior orbital rim because of the support of the arcus marginalis and lower septum. This underscores the deepened appearance of the nasojugal fold seen with aging as the medial periorbital fat herniates anteriorly rather than inferomedially.
Lower Tarsus, Lower Eyelid Retractors, and Conjunctiva
The lower tarsus, lower eyelid retractors, and conjunctiva make up the posterior lamella of the lower eyelid. Posterior lamellar structures of the lower eyelid are largely analogous to those of the upper eyelid. Of note, the average lower tarsal plate height in Caucasian patients is notably smaller than that of the upper tarsal plate, measuring approximately 4 to 5 mm versus 10 to 12 mm, respectively. In the lower eyelid, the orbital septum inserts to the inferior edge of the tarsus. By comparison, the septum inserts approximately 2 to 3 mm superior to the tarsus at the levator in the upper eyelid. The CPF, which arises from the inferior rectus and inferior oblique muscles, extends anteriorly to blend with Lockwood ligament, then merges with the deep surface of the lower lid orbital septum. The conjoined tissue formed by the fusion of the CPF with the septum extends superiorly approximately 3 to 7 mm to the inferior border of the tarsus. The superior aspect of the septum (tarsal-facing septum) is reinforced by its fusion with the CPF. By contrast, the inferior aspect of the septum lacks such CPF reinforcement, and, as a result, is prone to having a relative bulge, even in youthful anatomy. As aging commences or in the congenitally attenuated lower eyelid, orbital fat may herniate through this less-reinforced, weaker inferior aspect of the septum. The lower eyelid’s capsulopalpebral fascia and inferior tarsal muscle are analagous to the upper eyelid’s Muller muscle and levator palpebrae superioris.
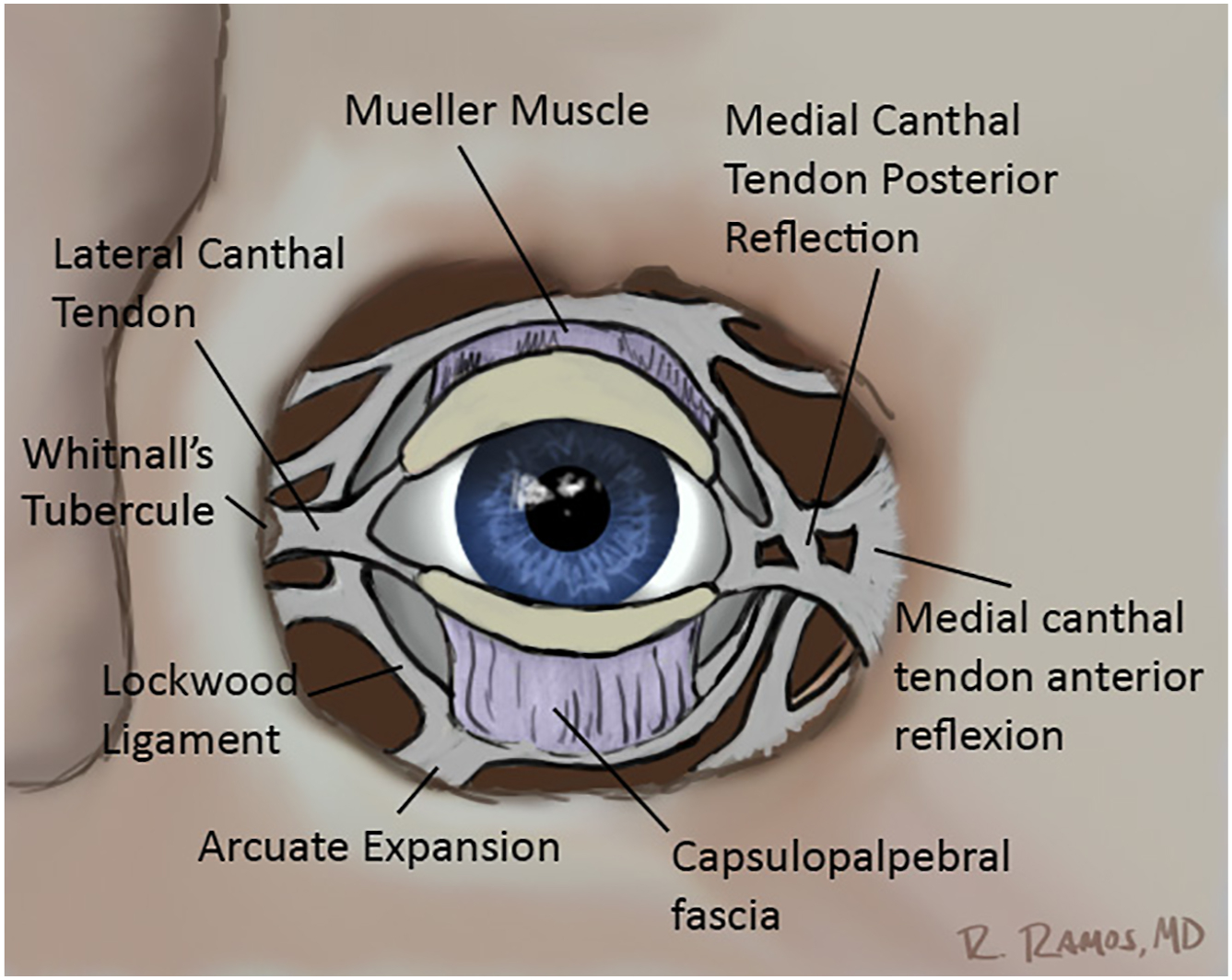
Lateral Retinaculum
Various distinct soft tissue structures converge and anchor to the lateral orbit to maintain the structure and support of the globe and eyelid. These structures are collectively called the lateral retinaculum ( Fig. 5 ). The attachments that comprise the lateral retinaculum consist of the lateral horn of levator aponeurosis, the lateral canthal tendon, the tarsal strap, Lockwood suspensory ligament, Whitnall ligament, and check ligaments of the lateral rectus. These structures insert directly or indirectly onto the periosteal thickening of Whitnall tubercle (lateral orbital tubercle), which is found on the inner aspect of the medial orbital rim approximately 10 mm inferior to the zygomaticofrontal suture.