Every surgical outcome, whether cosmetic or reconstructive, is shaped long before the first incision. Preoperative evaluation in aesthetic surgery and reconstructive procedures represents a structured, multi-domain process that spans medical history review, anatomical analysis, and psychological screening.
While both disciplines demand rigorous clinical workup, their priorities often diverge in meaningful ways. A systematic approach to this assessment phase protects the surgeon and the patient alike, surfacing risk factors that might otherwise complicate the operative setting. It also establishes realistic expectations, aligning what a patient envisions with what surgical intervention can reliably deliver.
Core Components of the Preoperative Workup
A thorough preoperative evaluation draws from several interconnected domains: medical history review, physical examination, laboratory testing, psychological screening, and facial or anatomical analysis. Each domain contributes distinct clinical data, and together they form a comprehensive picture of surgical readiness.
Patient selection begins at the initial consultation, where the surgeon assesses motivations, patient expectations, and overall medical fitness. This early exchange sets the tone for the entire treatment plan, helping distinguish candidates who are well-suited for a procedure from those who may benefit from alternative approaches or further preoperative preparation protocols.
Beyond clinical assessment, accurate documentation and procedural coding support the administrative framework of the surgical evaluation workflow. Clinical support staff responsible for coding surgical consultations and preoperative assessments can access free resources to study for CPC exam to strengthen their procedural coding accuracy. With these foundational components in place, the evaluation process can proceed systematically through each stage of the workup.
Medical History, Lab Testing, and Airway Assessment
A detailed medical history forms the backbone of any preoperative evaluation, serving as the non-negotiable starting point for determining surgical candidacy. This review should capture current medications, known allergies, prior surgical complications, bleeding disorders, and relevant comorbidities such as diabetes or cardiovascular disease. Each of these variables carries direct implications for anesthetic planning, intraoperative hemostasis, and postoperative recovery.
Incomplete histories introduce preventable risk, which is why structured intake protocols that systematically query each domain tend to outperform open-ended questioning alone.
Preoperative Laboratory Protocols
Rather than ordering a blanket panel for every patient, preoperative testing should follow a risk-stratified model. A baseline complete blood count and metabolic panel may be appropriate for most candidates, while coagulation studies, thyroid function panels, or hemoglobin A1c testing are reserved for patients whose medical history warrants them.
This targeted approach reduces unnecessary cost and avoids delays without sacrificing clinical thoroughness. When findings fall outside acceptable parameters, they guide further workup or prompt a referral before the patient reaches the operating room. A deeper look at comprehensive patient evaluation strategies can help clinicians refine their testing protocols based on published evidence.
Mallampati Classification and Anesthesia Risk
The Mallampati assessment evaluates oropharyngeal visibility by grading the structures visible when a patient opens the mouth and protrudes the tongue. The four-class system ranges from Class I, where the soft palate, uvula, and tonsillar pillars are fully visible, to Class IV, where only the hard palate is visible. Higher Mallampati classes correlate with reduced pharyngeal space and increased likelihood of difficult intubation, making this a standard screening step in anesthesia evaluation.
For procedures requiring general anesthesia, this classification directly influences airway management planning and equipment selection. Integrating Mallampati classification with findings from the medical history and laboratory results allows the care team to synthesize a composite risk profile. This synthesis, rather than any single data point, ultimately informs the clearance decision and determines the safest anesthetic strategy for each patient.
Psychological Screening and Patient Selection

Medical clearance and laboratory data address physical readiness, but they leave a significant dimension unexamined. Psychological screening evaluates patient motivations, emotional stability, and the degree to which expectations align with achievable surgical outcomes.
Certain patient profiles warrant particular caution during this phase. Individuals seeking surgery in the midst of acute life crises, those presenting with vague or frequently shifting aesthetic goals, and patients reporting dissatisfaction across multiple prior procedures all represent elevated risk for postoperative regret. Identifying these patterns early allows the surgeon to slow the process, request further evaluation, or redirect the conversation toward non-surgical alternatives before committing to an operative plan.
Body Dysmorphic Disorder in Surgical Candidates
Among the psychological considerations that complicate patient selection, body dysmorphic disorder stands out for its prevalence and clinical impact. Research suggests that BDD affects roughly 7–8% of cosmetic surgery populations, a rate significantly higher than the general population. Patients with BDD fixate on perceived flaws that are minimal or unobservable to others, and this fixation persists regardless of objective outcome quality.
The result is a cycle of dissatisfaction that surgery alone cannot resolve. Validated screening instruments, including the Body Dysmorphic Disorder Questionnaire, can flag at-risk individuals before a surgical commitment is made. Incorporating these tools into standard intake protocols strengthens the patient selection process and reduces the likelihood of operating on someone whose distress is psychological rather than anatomical in origin.
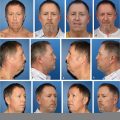
Facial Analysis and Photographic Documentation
Systematic facial analysis translates subjective aesthetic concerns into objective, measurable data. Using standardized landmarks and proportional frameworks, the surgeon evaluates symmetry, skin quality, soft tissue volume, and the structural relationships between facial thirds.
These measurements provide the anatomical foundation for surgical planning, identifying asymmetries or disproportions that may not be immediately apparent to the patient. Communicating these findings during the consultation helps align patient expectations with what the anatomy will realistically allow, reducing the gap between desired and achievable outcomes.
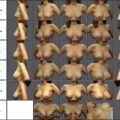
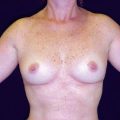
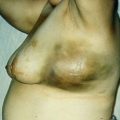
Photographic documentation complements this clinical assessment by creating a visual baseline. Standardized views, including frontal, lateral, oblique, and basal perspectives, serve as intraoperative references and postoperative comparison tools. They also function as medicolegal records, preserving the preoperative state in a format that is reproducible and defensible.
Both aesthetic and reconstructive cases in facial plastic surgery require consistent photographic protocols, though reconstructive documentation often extends beyond cosmetic baselines to capture functional deficits. Regardless of the indication, the combination of facial analysis and photographic records ensures that surgical planning is grounded in reproducible, patient-specific data rather than subjective recall alone.
From Evaluation to Operative Readiness
Preoperative evaluation functions not as a static checklist but as an integrated clinical judgment process. Medical findings, psychological screening results, and anatomical data feed into one another, and a red flag in one domain often triggers deeper investigation in the next.
This iterative quality distinguishes a thorough preoperative evaluation from a procedural formality. Reconstructive and aesthetic cases, despite their differing indications, converge on the same principle: operative readiness is earned through systematic assessment across every relevant domain, never assumed on the basis of a single favorable finding.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree