41 Burns
Summary
Reconstruction of pediatric burns have improved recently. Management is based on the principles of wound healing and scar maturation. Tissue can be manipulated with topical and intralesional modalities, local tissue rearrangements, grafts, and photomedicine.
41.1 Introduction
There has never been a more exciting and optimistic time in the history of pediatric burn therapy than that exists today in the developed world. Current therapeutic options to treat children who sustain burn injuries of all varieties have now reached a state of effectiveness that was unimaginable only a few short decades ago. Progress in the understanding of wound healing, improved diagnosis through technological advances, vastly superior critical care, as well as new and refined techniques of reconstructive surgery make the care of pediatric burns and restoration of the patients’ quality of life an exciting and rewarding field of pediatric plastic surgery. Because burns can involve all areas of the body and vary in size from the very small to almost the entire body surface area, they require a completely competent and caring plastic surgeon to treat the whole patient, the whole family, and the whole range of deformities that can be encountered. A few salient strategic concepts, however, are worth emphasizing at the beginning of this chapter.
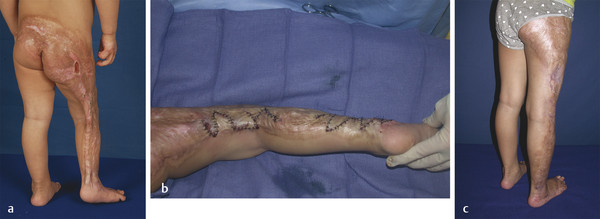
Acute burn injuries that are not life-threatening should be cared for with the most conservative burn wound management possible. Early excision and grafting commits a patient to a donor site and a grafted outcome that is iatrogenic and permanent (Fig. 41‑1). When necessary, to prevent serious complications, such early surgical intervention is essential. When not necessary, it is harmful for the patient. Improved diagnostic techniques such as laser Doppler imaging have been validated in multiple large studies and should be incorporated in the care of all pediatric burn injuries if at all possible. The overwhelming consensus from recent literature reports originated in the United Kingdom and Belgium has demonstrated that following the adaptation of laser Doppler imaging, the incidence of early excision and grafting in pediatric plastic surgery units has significantly decreased. Early excision and grafting has been advocated in smaller burns because of an alleged superior outcome and prevention of hypertrophic scarring. Profound advances in our ability to prevent and treat hypertrophic scarring as well as combining local plastic surgery techniques and the use of lasers and other photomedicine have allowed us to regenerate scars in ways that were inconceivable as recently as the 1990s. Today, a patient’s hypertrophic, contracted scars are often their most valuable reconstructive donor sites. The reason for that is that nothing beats “original equipment,” and their own scarred tissue is potential reconstructive material in the right location with the best possible color and texture match. It also does not require the creation of an iatrogenic donor site deformity on an uninjured part of the patient’s body (Fig. 41‑2). The ability to help scars to regenerate themselves is an essential part of pediatric burn care and reconstruction.

41.2 Diagnosis
Burn deformities present unique and complex reconstructive challenges for the pediatric plastic and reconstructive surgeon. A thorough understanding of the burn wound and its evolution is critical to successful treatment outcomes and is part of sound surgical judgment and expertise. Burn care can be considered as one of the most challenging areas of medicine because it involves multiple medical and surgical treatment modalities implemented over the course of time, frequently many years. It is beyond the scope of this chapter to discuss acute burn care, but suffice to say that well-described methods for recognizing burn injury from a number of modalities are replete within the literature. Thermal, electrical, and chemical injuries form the basis of the majority of the causative factors for acute burn injuries.
Burns, in general, constrict and deform and in doing so alter contour, proportions, features, form, and function. Burn care should strive to restore the injured patient as much as possible to their preburn condition and as close to “normal” as is possible with minimal morbidity (Fig. 41‑3). A return to normal, that is, the way in which the patient existed prior to the burn, is not possible. This must be clearly communicated to the patient and his or her loved ones so that they understand that the journey of burn care and reconstruction is one that sets realistic expectations and goals in treatment and offers the hope that we can get such patients to “near-normal.” Such an approach is realistic, responsible, and still offers optimism and hope to the patient, and family, that he or she can look forward to a return as close to the preburn injury condition as is possible, save for what the future may hold with regenerative medicine or technological advancements on the horizon.

The ultimate goal of burn reconstruction should be the restoration of an aesthetically pleasing and absolutely tension-free appearance to allow for appropriate form and function. The keys to achieving that goal are to appropriately diagnose the burn scar deformity, understand what issues are preventing that goal, and then provide a sound plan to address the problems. In concept, this sounds simple, but in practice it requires expertise and resources to make this goal a reality. Controversy still exists on what the optimum treatment is for moderate to severe burns. The vast majority of burns treated conservatively with topical antibiosis should heal in approximately 3 weeks. Burns that are obviously full thickness are best treated by early, tangential excision and grafting within 7 to 10 days. Even for controversial areas, the majority of burns can and are treated expectantly in most pediatric burn centers with a combination of modalities, which will be addressed later in this chapter.
Several useful generalizations regarding diagnosis and correct characterization of burns are important to mention and keep in mind. Superficial second-degree burns typically heal without scarring or pigmentary changes to the skin. Deeper or medium-thickness second-degree burns that epithelialize in 10 to 14 days will often heal without scarring although long-term changes in skin pigmentation and texture are frequent occurrences. Deep second-degree burns that epithelialize in 14 to 28 days or longer require careful observation; they are prone to develop severe late hypertrophic scarring. These patients, in particular, require close and continuous follow-up after the initial healing phase and must be managed via all available ancillary modalities, including appropriately timed surgical intervention when indicated.
41.3 Nonoperative Management
Whether we are considering nonoperative or operative treatment of burns, both modalities are based on an overall strategy and understanding of the specific problem at hand. This was briefly mentioned already in the “Diagnosis” section. Many techniques, including a plethora of surgical ones, have been described in the literature to address burns of many varieties and depths. What is most important is that in all cases, fundamental principles are recognized and followed such that the goals of management and treatment are arrived at in a predictable fashion. Therefore, developing a strategic concept of burn treatment is paramount and will help avoid unfortunate results.
Deep second- and third-degree burns heal by contraction and epithelialization and the deeper the injury, the more healing takes place by contraction. This category of burn depth will be expanded upon in the operative treatment section to follow as these typically do not do well without operative management. More superficial burns, as mentioned previously, require patience, observation, and providing the wounded area a milieu to allow for rapid, infection-free re-epithelialization. This is typically accomplished by good hygiene of the area, judicious pain control, and local wound care with a combination of modalities that include antibiotic topical creams or gels to more sophisticated wound dressings that are applied and changed daily or every several days while awaiting wound re-epithelialization. Typically, these burns wounds are those which heal within days to less than 2 weeks. Once the wound is re-epithelialized and risk of infection has passed, other well-described modalities exist for adjunctive therapy. Pressure garments have long been demonstrated to be effective in suppressing and reversing hypertrophic scarring. The addition of silicone to pressure therapy has also been a significant advance. Judicious use of sunscreen on immature and newly re-epithelialized burn scars is mandatory and typically should last a year as the scar undergoes maturation and is prone to hyperpigmentation from ultraviolet (UV) radiation. Sunscreen, in general, should be encouraged and recommended as part of a daily program of skin protection and treatment, regardless of burn depth and as part of normal pediatric skin care and skin maintenance.
41.4 Operative Treatment
As discussed earlier, a clear understanding of the pathophysiology responsible for a chronic open burn wound or burn scar contracture is essential to be able to devise an operative strategy to treat it. Several fundamental concepts and techniques are important to discuss prior to describing specific operative interventions: contractures, contour and proportion, tension, donor site availability, aesthetic units, Z-plasty, grafts, flaps, and lasers. These nine basic treatment strategies must be understood in order to have a comprehensive overview of operative pediatric burn wound management and treatment.
41.4.1 Contractures
Burn injury leads to tissue loss and the resultant wounds heal with contraction, which results in contractures. Contractures are either “intrinsic” or “extrinsic.” Intrinsic contractures are those that result from loss of tissue in the area of the contracture with subsequent distortion of the part affected. Extrinsic contractures include those in which the tissue loss is at a distance from the affected area, but the distorted structures are themselves not injured. It is critical to recognize these differences given that they are often overlooked in burn scar and burn injury treatment. Not only must corrective measures be directed at the cause of the contracture to prevent iatrogenic deformities, but it is also essential to minimize the amount of skin and scar that are excised when dealing with contractures. Minimizing excision decreases the amount of new skin that must be provided. In fact, due to the beneficial effects of releasing tension, most scars will mature favorably once a release has been carried out (Fig. 41‑2 and Fig. 41‑3). It is important to understand that scars are living things, not static entities, and that they will respond to a change in their environment.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








