31 Management of Facial Filler Injection Complications
Pearls
Skin thickness varies across different anatomic regions. Since the eyelids, periorbital area, and nasal dorsum are known to have a very thin dermis, special care should be taken while injecting into these regions not to create lumpiness, nodules, or granulomas.
The glabellar and nasolabial regions are regarded as high-risk facial units in which surgery can lead to serious vascular complications.
Fillers should be placed in the appropriate layer of skin. Too superficially injected fillers can result in unevenness and visibility. Too deeply injected fillers can be under effective at changing shapes.
Given that most faces are slightly asymmetric, it is important to visually check whether the two sides of the face are symmetric during injection.
Massage is generally sufficient to flatten and disperse excessive, superficial, or unaesthetically placed filler causing visibility.
Bilateral compression and releasing of the superior nasal corner of the orbital rims during injection is a new maneuver that can reduce orbital complications by increasing intraluminal pressure.
Severe pain and blanching of the skin are warning signs of intravascular injection of filler and require emergent measures. These include stopping injection, aspirating as much injected filler as possible, and injecting a high dose of hyaluronidase in case of hyaluronic acid filler.
Low-molecular-weight heparin, hot packs and soft massage, 2% nitroglycerin paste patch, and injection of prostaglandin E1 are additional measures to enhance vasodilation and inhibition of platelet aggregation in case of vascular occlusion by filler.
Once eschar has formed, appropriate wet dressing is required with antibiotics to prevent secondary infection. Starting hyperbaric oxygen therapy also helps to improve healing.
When addressing an intervention to complicated cases such as skin necrosis, more conservative and less invasive treatment should be attempted before recommending a radical solution.
Introduction
A filler is any material that can augment volume when injected into the body, and is usually available in an injectable form. Well-known fillers include hyaluronic acid products, collagen, paraffin, and liquid silicone. Although most of the fillers in the market are known to have a good safety profile, complications can occur occasionally since they are artificial implants that can induce a foreign-body reaction. Because injection is a blind procedure, the physician is unable to see exactly where the filler is placed. According to a study of 286 patients injected with hyaluronic acid gel, there was a complication rate of ~ 5%.1 However, most complications can be prevented by selecting safe products and performing the procedure in an appropriate manner. Although fillers can be injected into any region of the body theoretically, each filler has a specific niche in terms of its purpose. For instance, human collagens and the medium hyaluronic acid products such as Restylane (Galderma) and Juvederm Ultra (Allergan) are appropriate for correcting fine rhytides in thin-skin areas while heavier fillers such as calcium hydroxyapatite and poly-Llactic acid are excellent for their volumetric effect.2
An understanding of facial anatomy, especially skin thickness and vessels, is also crucial to reduce complications. Skin thickness varies among different anatomic regions, and requires different techniques depending on filler type. Generally, human collagen should be placed in the middermis, and medium-length hyaluronic acid products should be placed in the deep dermis. Calcium hydroxyapatite is injected at the dermal subcutaneous border, while poly-Llactic acid and fat are injected into the subcutis.2 Since the eyelids, periorbita, and nasal dorsum are known to have a very thin dermis, special care should be taken when injecting into these regions not to introduce lumpiness, nodules, or potential granulomas. For the novice, sometimes it is better to err on the side of filler placement that is too deep rather than too superficial even though the augmentation effect may not be as apparent.2,3
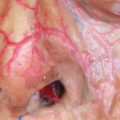
The rich network of blood vessel in the face is by and large a blessing, but it can increase the chances of bruising, hematoma, or embolism-related complications. The glabellar and nasolabial regions are regarded as high-risk facial units that can be associated with serious complications, including emboli and resulting necrosis because their main arteries, the supratrochlear artery and the angular lateral nasal artery, respectively, are vulnerable to embolism by filler (Fig. 31.1).2,3,4 Augmenting the chin with heavy fillers can potentially lead to vascular compromise if too much of the product is injected at once by compressing the blood vessels.
It is not clear which type of injection technique, the multiple serial puncture or the linear threading technique, causes fewer complications. The multiple puncture technique makes it easier to control placement but can lead to unevenness. The linear threading technique tends to require more experience, and can result in over-injection to a given area. The fanning technique has been reported to increase the likelihood of bleeding even in experienced hands.2,5 Ultimately, the practitioner can utilize these techniques to supplement the weaknesses of one another.
Patient Evaluation
The patient with complications after filler injection should be interviewed thoroughly about previous medical procedures. If the patient is in an immunosuppressed state, it is not a contraindication, but the higher risk of infection should be discussed. In those patients with immunologic diseases such as lupus or scleroderma, it is best to consult with the dermatologist or rheumatologist before proceeding with any additive procedures. Previous filler-related issues, including type and dose of fillers, number of injections, and injected areas, should be evaluated.
If a patient is dissatisfied with a previous filler type, the physician should not re-administer that product. In this situation, it is best to attempt an alternative treatment or product, or simply not to treat at all. To set up an accurate treatment plan, the physician should ask about the onset and progress of symptoms and signs. Generally, transient swelling or tenderness can be seen 24 to 72 hours after injection because of the physical imposition and subsequent volume displacement on the skin from an implant.2 These adverse effects will diminish over a relatively short period of time. But if there is an irregularity due to a semipermanent or permanent filler, it will require some form of intervention. When the physician determines it is necessary to do some kind of intervention, the patient needs to be informed that the treatment plan may require multiple sessions, whether it is a small complication or a devastating one. A discussion regarding the potential for any permanent scars from these interventions should be included in the initial consultation. This step is really important in maintaining a good doctor-patient relationship since the patient is usually in a very anxious state. More conservative and less invasive treatment is often recommended as a first attempt for a complicated patient rather than a radical solution.
Complications and Their Management
The best way to manage complications is to prevent them by choosing the appropriate technique and filler type. Attaining a consistently excellent outcome and avoiding poor results begin before the actual injection. Marking the injection points prior to the actual injections considering adjacent anatomy is helpful to reach these goals.
Early Onset
Minor Form
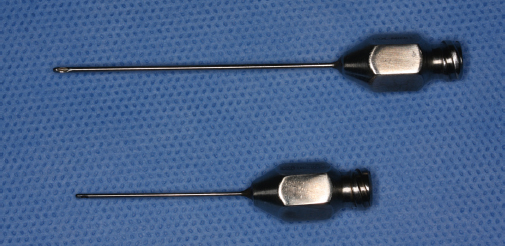
Bruising is a common complication of filler injections, and it is caused by vascular damage from a needle. All patients should be informed not to take blood thinners such as aspirin 1 week before the procedure. During the procedure, piercing of muscular layers must be minimized. The injection site should be cleaned with an alcohol swab, and the procedure should be performed in a room with adequate lighting. Immediately applying an ice pack to the injection site may help to minimize bruising. Special needles or cannulae can be used to minimize vascular injury as well (Fig. 31.2). If bleeding occurs during the procedure, the injection site should be covered with gauze and pressed for several minutes to prevent hematoma formation. Usually bruising is only temporary and does not affect the final therapeutic effect. It can darken in the days following the injection, but will gradually disappear after 10 days in most cases.6
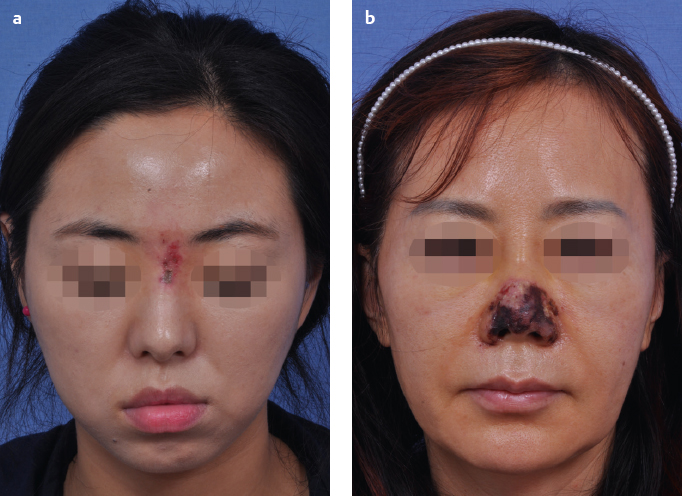
Occasionally, there may be hypersensitivity to the filler ingredients. The main symptoms are pain and erythema, accompanied by pruritus and fever.7 In the vast majority of patients, fortunately, these symptoms resolve in 2 to 3 days as the causative substance disappears. In severe cases, administering corticosteroid products and warm compression may help alleviate the symptoms. V-beam laser treatment can be used for persistent erythema.8
Major Form
The serious complications that occur after filler injection are blindness and dermal necrosis. Vascular compromise can be largely divided into intra- and extravascular causes. Intra-arterial injection of filler is rare but can be disastrous. Extravascular causes include external venous compression due to excessive volume of injection, and edema and inflammatory response caused by a component of the filler.
Intra-arterial Embolism
Intra-arterial embolism has a relatively low incidence, but its consequences are devastating. Blindness following cosmetic filler injection is the most serious complication. Most cases of ocular complications occur during multiplesite injections, but some facial units distinguished by the fat compartments and the retaining ligaments may have a higher risk compared with others.9,10,11 The nasolabial and the frontotemporal units are known to be danger zones due to large-core cutaneous arteries susceptible to accidental cannulation, the facial and the superficial temporal arteries.12 Young patients may have higher risk of blindness because healthy skin has abundant cutaneous arterial anastomoses.
The facial artery takes a tortuous course along the nasolabial crease (Fig. 31.3), where it becomes endangered by an injection intended to soften and reduce the prominent nasolabial fold. The frontal branch of the superficial temporal artery gives off descending branches to anastomoses with the supraorbital and the supratrochlear arteries from the ophthalmic artery. To prevent complications, a smallbore needle tip is recommended with smaller syringes, preferably 0.5 to 1 mL, so that less pressure is required on the plunger. The needle tip should be moved back and forth continuously during injection since most complications occur while injecting filler materials in the static state with high pressure. Previously traumatized areas, such as a blunt trauma site or blepharoplasty site, should be avoided. During filler injection at the temple area, the needle tip can be deviated superficially from the deep injection plane by a bony curve of the frontal bone and encounter the frontal branch of the superficial temporal artery. Thus, special care should be taken not to lose the appropriate plane. Recently, evidence has emerged of persistent anastomoses between the ophthalmic artery and the facial arterial system at the superior nasal corner of the orbital rim.12 Based on this knowledge, the author has introduced an effective safety maneuver that bilaterally compresses the superior nasal corners of the orbital rims during the injection moment and releases them soon afterward. This technique creates a temporary collapse of the anastomotic pathways using the hand of an assistant (Fig. 31.4).
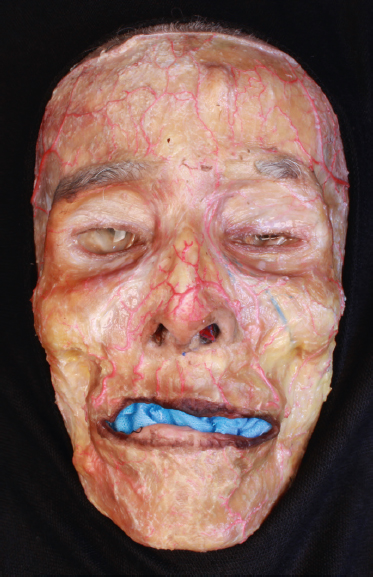
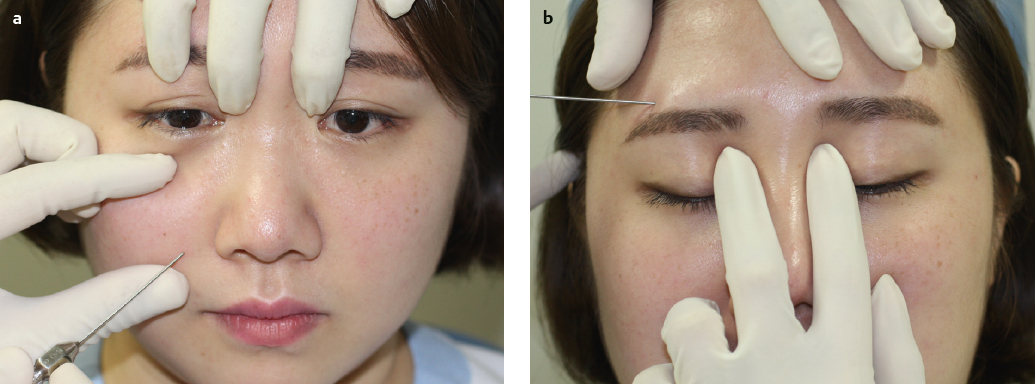
When an assistant is unavailable, an alternative method is to compress the tissue on the course of the core artery between the injection site and the eye while stretching the skin for an injection procedure using the nondominant hand. This method could increase the luminal pressure enough to block any filler that was accidentally injected into the main artery underneath from traveling to the globe. The target areas for compression are the oral commissure, upper nasolabial fold, alar crease, side of the nose, medial canthus, superior nasal orbital rim, and glabella. With the index and long fingers counteracting with the thumb, the injection areas can be stretched and immobilized.
If the patient complains of sudden ocular pain or visual loss, however, injection must cease immediately. An ophthalmologist should be contacted for measurement of visual acuity and fundoscopy.
The goal of treatment is rapid restoration of perfusion to the retina and optic nerve head. Retrobulbar injection of 2 to 4 mL (150 to 200 U/mL) of hyaluronidase is recommended within 60 to 90 minutes.13 This might be the single most effective option to dissolve the intraorbital intravascular hyaluronan in a time-sensitive manner.14 Ocular massage (repeated, increasing pressure applied to the globe for 10- to 15-second intervals over 3 to 5 minutes) may lower intraocular pressure and increase arteriolar flow, potentially moving the retinal vascular embolus peripherally.15 Intravenous mannitol and diuretics (500 mg of acetazolamide) may increase retinal blood flow and rapidly reduce intraocular pressure. Topical and intravenous antibiotics and subsequent administration of high-dose corticosteroid (methylprednisolone 1 g/day intravenously for 3 days, and dose tapering with oral administration) can be attempted.15,16 In fact, no safe, feasible, and reliable treatment exists for iatrogenic retinal embolism. Nonetheless, therapy should theoretically be applied as soon as possible to increase the chance of recovery.
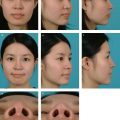
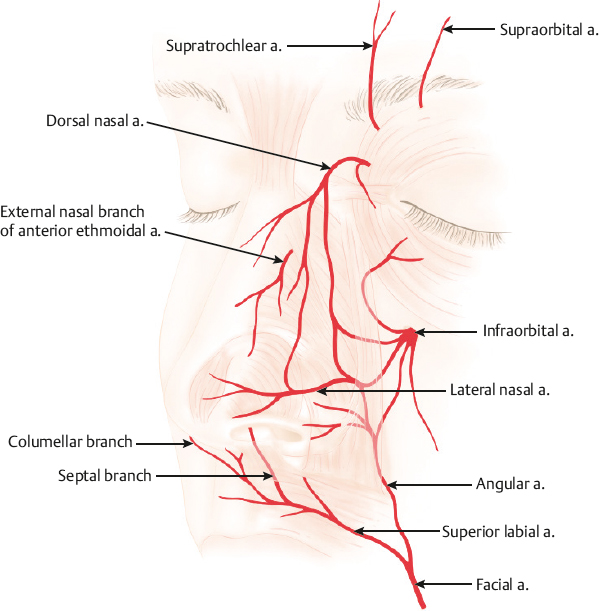
Injection rhinoplasty is also the main procedure that can induce intra-arterial embolism by injecting the dorsal nasal artery directly. The dorsal nasal artery, as its name suggests, runs along the dorsum of the nose, ~ 3 mm away from the midline (Fig. 31.5). It is a fairly immobile blood vessel fixed to the surrounding tissue, and the needle tip can be inserted safely if it is inserted in parallel with the blood vessel. The dorsal nasal artery anastomoses with the ophthalmic, infratrochlear, and angular arteries, and a widespread embolism through the connected blood vessels manifests as skin necrosis in a geographic pattern.
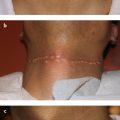
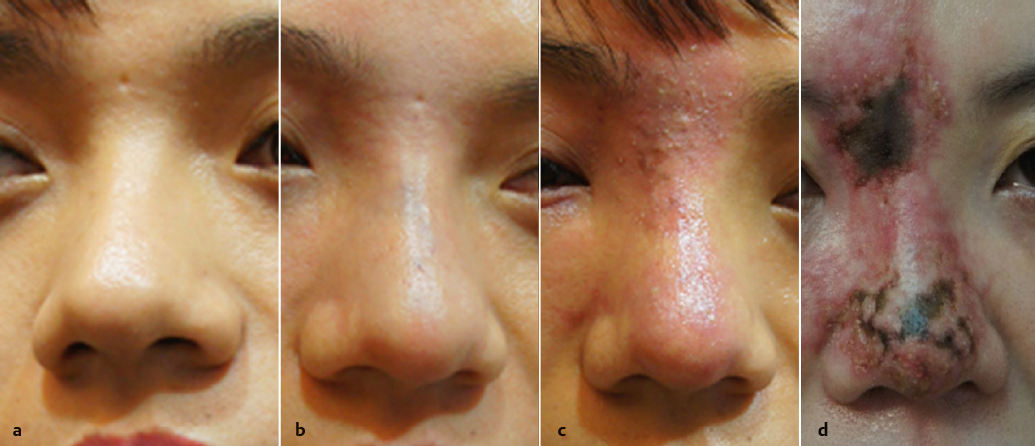
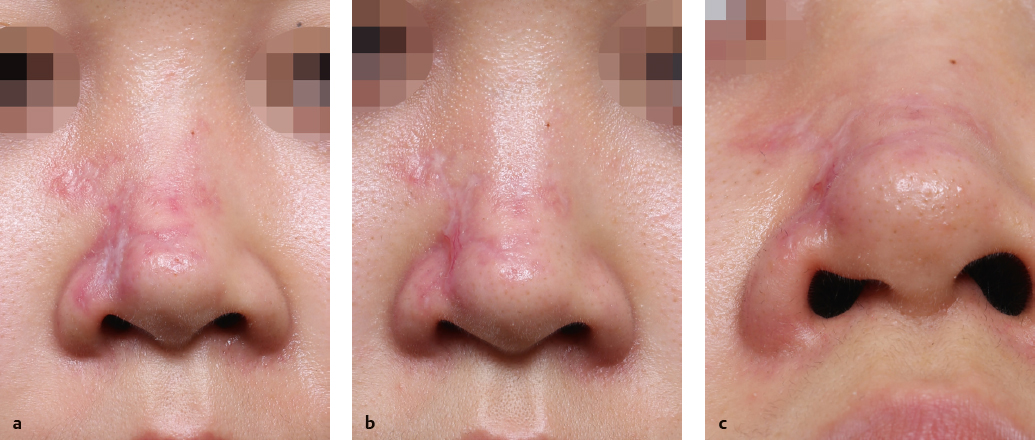
If arterial injection is suspected, however, prompt management should be done according to the treatment protocol of intra-arterial embolism. Once filler is injected into the arterial bloodstream, the patient experiences severe pain immediately, and may complain of a sensation of something spreading out from the injection site. The area supplied by the blood vessel where filler embolism has occurred becomes pale due to ischemia. The ischemic area develops edema within several hours, and soon appears mottled and purplish due to venous congestion as a rebound phenomenon. After ~ 24 hours, multiple ulcerative lesions accompanied by eschar and erythema, worsening over time, result in desquamation of the tissue within several days (Fig. 31.6).3,4 These large areas of necrosis heal and reduce over time, eventually leading to scar formation with contraction of tissue (Fig. 31.7).
To prevent this complication during nasal augmentation with fillers, the needle tip must always be located in the midline to avoid injecting into the dorsal nasal artery. If filler has to be injected into the side of the nasal dorsum, for example, for correction of a deviated nose, the needle should never move in parallel with the direction of the blood vessel. After inserting the needle into the midline, the needle tip should move to the side. Because the dorsal nasal artery is located in the superficial fatty layer and SMAS, the injection should be into the deep fatty layer to prevent embolization to the dorsal nasal artery. Aspirating the needle before injection and injecting filler while withdrawing the needle are tips for safe injection. Using a blunt cannula also helps to prevent incidental puncture of the vessel and is recommended to physicians who are not familiar with the injection technique.
If the patient complains of severe pain and blanching of the skin is observed along the area of the blood vessel during the filler procedure, the injection should immediately stop and as much filler should be aspirated as possible. If hyaluronic filler has been injected, injection of hyaluronidase to the lesion is recommended (Fig. 31.8). The optimal time of hyaluronidase injection in case of vascular complications has not been determined yet, but it is wise to use high doses of hyaluronidase (at least 200 U) as early as possible. Some experts recommend dilution with saline to increase dispersion or lidocaine to aid vasodilation. Additional hyaluronidase should be injected if improvement is not seen within 60 minutes.17 According to an experimental study, the degradation ratio of cross-linked HA with 100 IU of hyaluronidase after 24 hours was 50%, and it depended on the amount of hyaluronidase.18,19 Recently, there has been some evidence that if hyaluronidase is injected subcutaneously, it will diffuse into the obstructed vessels and degrade the HA filler to prevent impending necrosis caused by intra-arterially injected HA filler.17 Low-molecular-weight heparin therapy can decrease thrombosis and embolism, but it may be difficult to obtain and administer in an outpatient clinic setting. It is very important to supply enough oxygen to the area of ischemia. For this purpose, hot packs, soft massage, and 2% nitroglycerin paste can be applied for vasodilation. Injection of prostaglandin E1 is effective by the action of vasodilation and inhibition of platelet aggregation. A regimen of 10 mg a day for 3 to 7 days is recommended. Appropriate dressing should be applied once desquamation and pustule formation occur after a day. The physician should administer appropriate antibiotics to prevent secondary infection, apply wet dressing for faster wound healing, and continue to administer antibiotics.2,3,4
Starting hyperbaric oxygen therapy is also helpful. It is known to improve neovascularization and postischemic tissue survival by elevating cellular oxygen levels. The protocol differs among practitioners, but the authors recommend 90 minutes of treatment twice per day for 7 to 30 days with 100% oxygen at 0.2 MPa. This yields a more than 20% increase in arterial blood oxygen content.20
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree