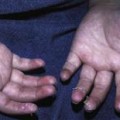
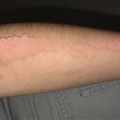
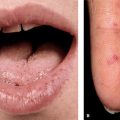
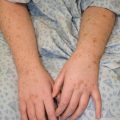
Extensor versus flexor skin surfaces: skin over the extensor surface is thicker and darker in color. This is designed to withstand trauma which is more likely to occur with extension movements than with flexion movements.
• Skin in the back of your arm and upper body (extensor surface) is thicker and darker than skin in the front of your upper body or arm.
• Skin in the front part of your leg is thicker and darker than in the back of your leg.
Intertriginous area (skin fold) is where skin touches skin frequently (e.g., groin and axilla). These areas are more likely to get infection with Candida, scabies, hidradenitis suppurativa, etc.
Rash variations: we included few classic pictures of various rashes, but in your free time try to look for other variations online. This can help you on exam. Just as humans, of the same Homo sapiens species, look different from one another, rashes of the same condition can look different too. If you Google search for atopic dermatitis or lichen planus, you will be amazed at how many variations you can find.
Terminology to describe skin lesions
Patcha | ||
Fluid-filled blisters b | ||
aPatches that are palpable, or with corrugated, elevated surface are called plaques. | ||
bIf the fluid inside blister/bullae is yellow, then it is called a pustule. | ||
cSimilar to this principle, gastric erosion affects only mucosa, if there is involvement of submucosa, it is called an ulcer. | ||
13.1 Skin Infections (Folliculitis, Furuncles, Carbuncles, Skin Abscess, Paronychia, and Hidradenitis Suppurativa)
13.1.1 Folliculitis
Definition: Superficial infection around a hair follicle, most commonly due to Staphylococcus aureus.
Exam: Pinpoint erythema or pustules around follicles. It can be tender.
Rx: Depends on the area of involvement and severity.
Differential dx: Bathtub folliculitis due to Pseudomonas. The lesions typically start below the neck (bathtub water submersion pattern). Treatment is avoidance or chlorination of hot tub. In severe cases use ciprofloxacin.
13.1.2 Furuncles, Carbuncles, Skin Abscess, and Paronychia
Microbiology: Most common (MC) organism is S. aureus.
Physical Exam: As opposed to folliculitis which might not be tender, these are usually tender. A small collection or fluctuant mass is felt, with surrounding erythema and swelling.
13.1.3 Hidradenitis Suppurativa
Predisposing factors: Obesity, smoking, genetic susceptibility, and postpuberty. Occurs in intertriginous areas (arm pits, inguinal, genital, and perianal area).
Rx: Lifestyle modification (e.g., maintaining hygiene) and, depending on severity, topical or systemic antibiotics and/or surgery (punch debridement or unroofing).
13.2 Other Bacterial Infections Involving Skin
13.3 Viral Skin Infections-HSV-1, HSV-2 and Herpes Zoster
13.3.1 Herpes Simplex Virus (HSV) Infection
13.3.2 Herpetic Whitlow
Background: Cutaneous herpes simplex virus (HSV-1 or -2) can be acquired through contact with infected herpes genitalia or cold sores (e.g., dentist gets exposed to patient’s oral lesions). It can occur as a result of self-infection, too.
Presentation: Clear fluid-filled vesicles or pustules in fingers or hands. It is usually tender and can be recurrent.
Dx: Clinical, but when in doubt, we can do viral culture, viral PCR, direct fluorescent testing on sample, or Tzanck smear (to look for multinucleated giant cells).
Rx: Conservative management in most patients. In significant cases, consider antiviral valacyclovir, famciclovir, or acyclovir.
13.3.3 Herpes Zoster a.k.a. Shingles
Background: After getting chicken pox (primary varicella zoster virus infection), the virus can remain dormant in sensory nerve ganglia for years. Precipitating factors such as immunosuppression can lead to reactivation of virus and eruption of rash along a sensory nerve root distribution.
Vesicles are in classical dermatomal distribution and unilateral (i.e., does not cross the mid-line). The rash is painful and itchy.
Some patient can present only with neuropathic pain in dermatomal distribution (preherpetic neuralgia). Pain can precede rash for days to weeks!
Severe postherpetic neuralgia (after onset of rash) can also occur.
Rx: Antiviral valacyclovir, acyclovir, or famciclovir (+clovir). In immunocompromised patients consider varicella zoster immune globulin.
Type of precaution in a health care setting (e.g., hospitals) | Indication for postexposure prophylaxis in patients who lack immunitya | |
|---|---|---|
Primary infection (chicken pox), disseminated zoster (when zoster involves more than 1 dermatome), and immunocompromised patient with dermatomal zoster | Airborneb + contact precautions | |
Only for close contacts of patients with open, weepy lesions. NOTE: crusted zoster lesions are not infectious. | ||
aIndividuals with no immunity to VZV (varicella zoster virus) are: | ||
bRequires negative-pressure room. Same type of precaution is used for active tuberculosis. | ||
Postexposure prophylaxis is recommended with two doses of zoster vaccine. Since it is a live vaccine, it is contraindicated in newborns, pregnant, or immunocompromised individuals. In these patients, use varicella zoster immune globulin instead.
Unique presentations of Varicella Zoster (aka Herpes Zoster) virus reactivation
13.4 Parasitic Skin Infections
13.4.1 Scabies
Background: Skin infection due to Sarcoptes scabiei, which is transmitted by close contact.
Presentation: Scattered papules and/or pustules ± underlying erythema found particularly in digital webs (interdigital space of hands or feet), palms, and intertriginous areas. These are very itchy. Look for history of exposure to patients with similar symptoms. Patients with HIV can develop extensive scabies with severe crusting, known as Norwegian scabies.
NSIDx: Find parasite in skin scrapings.
Rx: Topical permethrin or oral ivermectin. With crusted scabies, combine both oral and topical treatment.
Complication: Secondary bacterial skin infection can develop (e.g., impetigo, cellulitis).
13.4.2 Pediculosis (Head Lice)
Background: Infestation by lice can occur in hair-bearing areas; usually in head, but can occur in genital or axillary area.
Presentation: Prominent itching and skin excoriations. Secondary bacterial infection can develop.
NSIDx: Direct examination of hair-bearing areas.
13.5 Intertrigo
Definition: Intertrigo is an umbrella term for inflammatory conditions located in skinfolds (intertriginous areas). It can develop due to mechanical skin-on-skin friction/irritation alone or become complicated by superimposed fungal or bacterial infection.
Risk factor: Diabetes, obesity, advancing age, and other forms of immunosuppression.
Presentation: Erythematous lesions that can be painful and pruritic. Secondary spongiosis can occur (formation of vesicles and pustules which can weep, ooze, and crust). Intertrigo can also present as diaper rash in children.
General treatment: Minimize friction (barrier creams) and prevent moisture buildup (absorptive powders such as corn starch).
Look for Secondary infection with dermatophytes, Candida, Corynebacterium (erythrasma), staphylococcus and streptococcus.
Papules or plaques that can be of various colors. Rash can have overlying white lacy to net-like lines. | Lichen planusa | ||
Initial oval or round herald patch (looks like rash of tinea corporis), followed by development of maculopapular eruptions that occur in a Christmas-tree-pattern | If rash is atypical do VRDL or RPR test to screen for syphilis (palms and soles’ involvement points toward secondary syphilis) | Benign condition that usually resolves on its own. | |
Get Clinical Tree app for offline access 
|