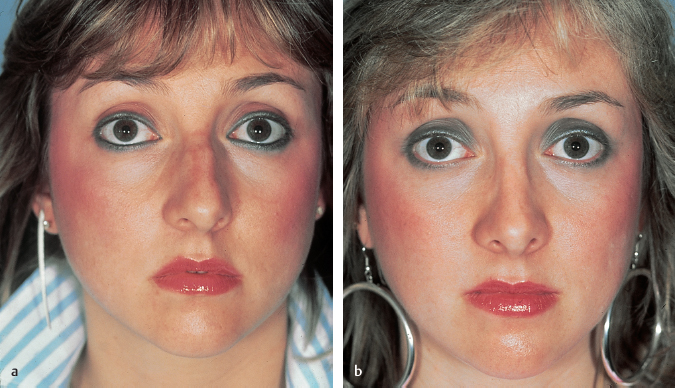
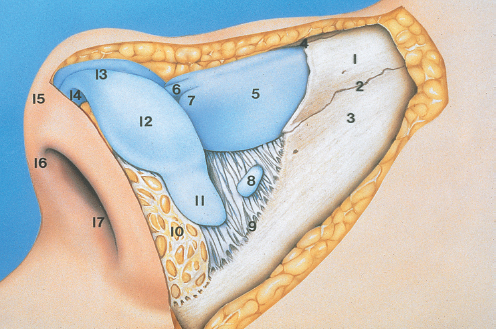
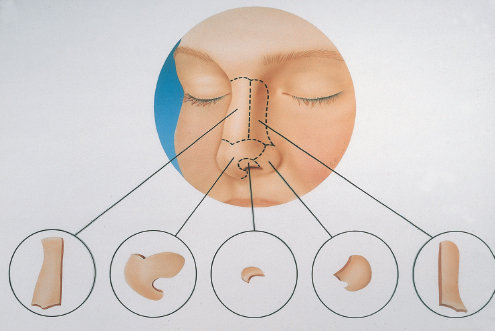
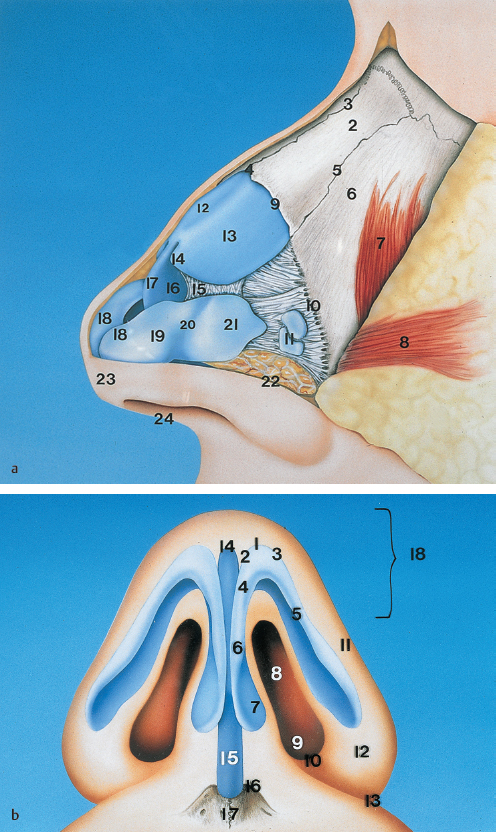
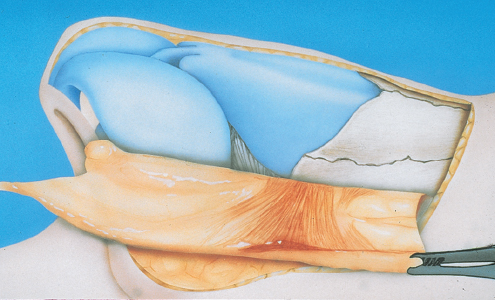
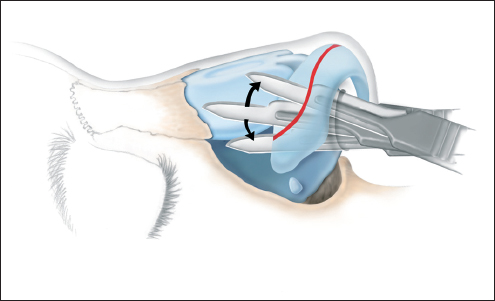
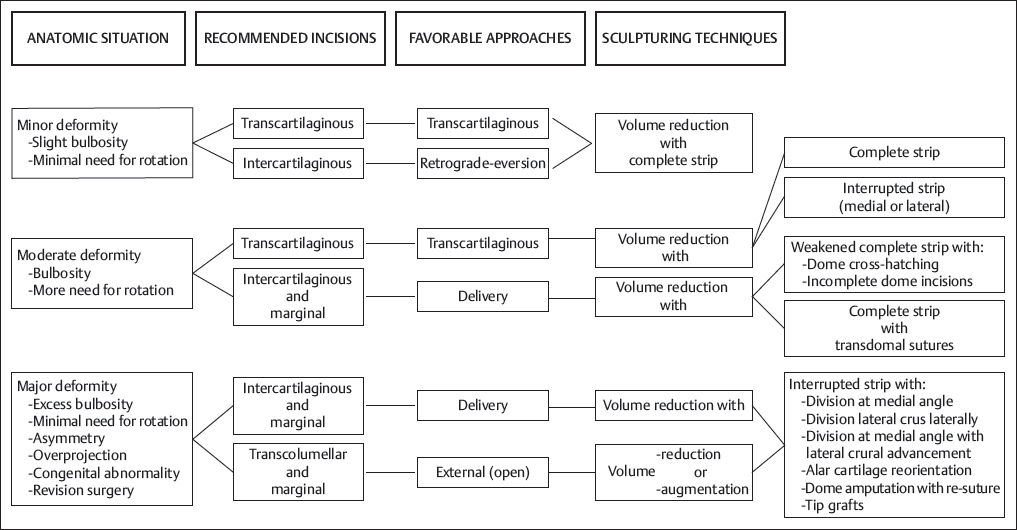
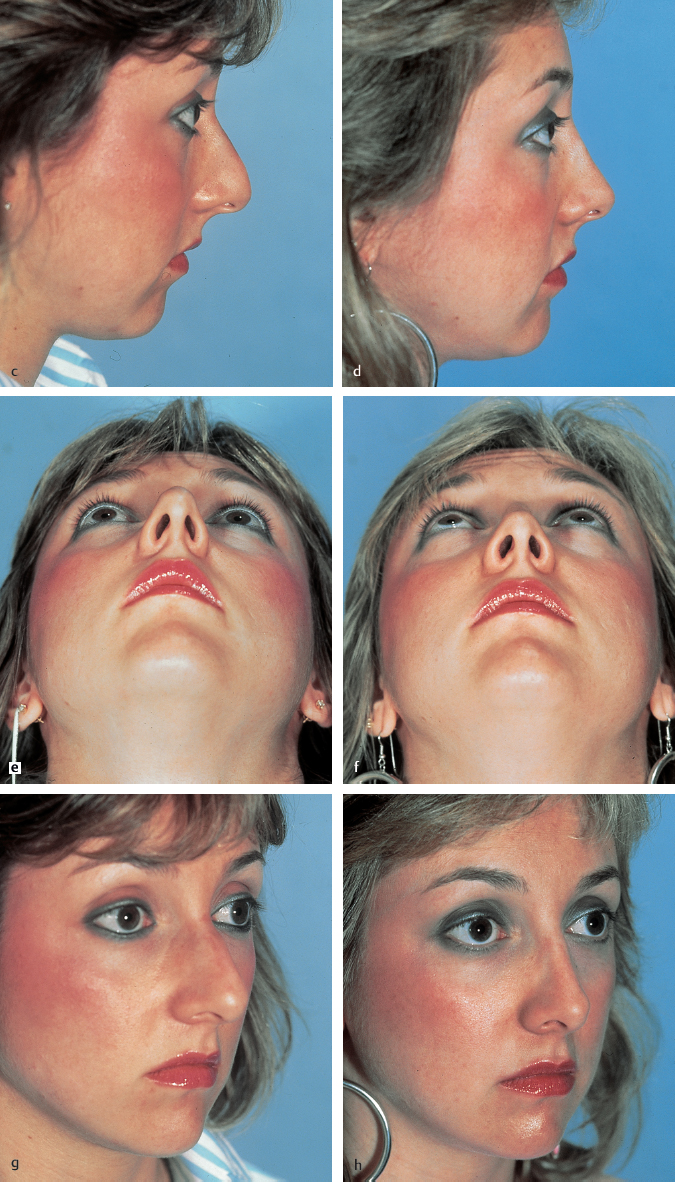
Chapter 2 2.1 Introduction and Personal Philosophy 2.5 Preoperative Considerations 2.6 Special Surgical Requirements Although the history of modern rhinoplasty surgery extends back only one century, typical, traditional reduction rhinoplasty is now commonly associated with a nasal reconstructive procedure characterized by tissue preservation, reconstruction, augmentation, and reorientation. The most significant advances in rhinoplasty in the past two decades have been characterized by a stronger emphasis on exacting anatomical analysis. Although techniques have certainly been refined and improved, the final result of any rhinoplastic procedure develops as the consequence of the patient’s unique anatomy coupled with the surgeon’s skill in accurately diagnosing the exact anatomy and variants of anatomical components. Fundamental knowledge of the universal principles and canons of rhinoplasty, coupled with an understanding of the dynamics of the operation itself and the healing changes that inevitably evolve over time, equips the contemporary surgeon best to achieve uniformly excellent results. The surgeon must initially judge, by inspection and palpation, the character and texture of the skin and subcutaneous tissues as they vary from nasal region to region, the influences of facial mimetic musculature, the relative strength and support of the cartilaginous and bony framework and substructure, and the limitations imposed by the interrelationship of all these structures on the ultimate favorable result. Concomitant creation or preservation of normal airway function is essential. All this must be balanced with the individual surgeon’s aesthetic judgment, factoring in the surrounding facial features and overall stature of the patient. No single surgical technique will suffice to refine every nose to an ideal state. Thus, a wide repertoire of surgical skills must be employed to manage the plethora of abnormalities encountered. Most importantly, the wishes of the patient create a critical factor in fashioning the ultimate surgical outcome. Rhinoplasty continues to be increasingly characterized by a global, multicultural desire for improvement in appearance and nasal function. Thus, the racial variations in nasal form and function assume more importance, and patients increasingly request nasal modifications that improve appearance but preserve cultural and racial characteristics. The objective of aesthetic nasal plastic surgery is to create a nose that draws no attention to itself but enhances the beauty of the eyes, allows for comfortable nasal function, and is in harmony with the other features of the face. This simple statement belies a complex problem. The universal concept of what is “beautiful” or “ideal” remains an age-old question, and the solution involves a multiplicity of emotional reactions and prejudices. In addition, values and assessments of beauty vary within different age groups and social structures. To evaluate what is beautiful entails a study of physical and cultural anthropology, ethnology, psychology, and aesthetics. Beauty of the human face is neither abstract nor absolute; it varies among different ethnic groups and is subject to interpretation by each individual. This attitude is based on a multiplicity of factors varying according to the body image and cultural values of individual conditioning, particularly during the formative years, when it often becomes part of the unconscious mind. Contemporary rhinoplasty fortunately is characterized by the strong, appropriate concern for conservative and subtle anatomical changes (Fig. 2.1). Rather than excisional sacrifice of large segments of cartilage or bone, a philosophy of preservation and reorientation of tissues has developed that largely eliminates the creation of unnecessary tissue voids that too often contract and scar unpredictably. Conservation surgery thereby further extends the surgeon’s control over the healing surgical result, as an appropriate equilibrium between the corrected nasal skeleton and investing soft-tissue covering is more reliably achieved. Effective methods of autogenous tissue grafting extend the surgeon’s control over the final outcome and its long-term stability. Finally, thoughtful nasal surgeons, through accurate anatomical diagnosis, discern which portions of the nasal anatomy are pleasing and satisfactory, striving to avoid disturbing these structures and areas when correcting (or gaining access to) anatomical components in need of correction. Fig. 2.1 (a–h) Favorable surgical outcome in patient shown 3 years after conservative and balanced septorhinoplasty surgery. An artistic anatomical concept must be developed by the rhinoplastic surgeon when approaching the study of nasal anatomy (Fig. 2.2). The surgeon visualizes the nasal structure not only as static bone and cartilage, but also as muscle and cartilage tension, skin texture, interconnected relationships with surrounding structures, and the effect of related and interrelated structures on the shape of the nose. He or she must develop a personal sense of the “ideal normal,” altering abnormal nasal anatomical components based on this artistic concept, coupled with the patient’s clearly defined expectations. Rhinoplasty is traditionally undertaken as the result of a patient’s request to surgically correct perceived anatomical nasal abnormalities. A didactic list of surgical indications might include the following: • Nasal aesthetic deformity. • Nasal functional deformity with airway blockade. • Nasal traumatic deformities, both acute and preexisting. • Abnormalities from previous nasal operations (revision rhinoplasty). 1. Nasal bone 2. Nasomaxillary suture line 3. Ascending process of maxilla 4. Osseocartilaginous junction (rhinion) 5. Upper lateral cartilage 6. Anterior septal angle 7. Caudal free edge of upper lateral cartilage 8. Sesamoid cartilage 9. Pyriform margin 10. Alar lobule 11. Lateral crus of alar cartilage—lateral portion 12. Lateral crus of alar cartilage—central portion 13. Tip-defining point 14. Transitional segment of alar cartilage (intermediate crus) 15. Infratip lobule 16. Columella 17. Medial crural footplate Absolute as well as relative contraindications to rhinoplasty exist. Absolute Contraindications • Bleeding and coagulation disorders which are uncorrectable. • Pregnancy. • Any systemic illness that might be worsened by rhinoplasty surgery. • Significant psychiatric disorder. Relative Contraindications • Temporary or correctable coagulopathies. • Severe nasal sunburn. • Severe nasal acne. • Psychological and psychiatric disorders that cannot be corrected or stabilized. • Active relapsing polychondritis and similar autoimmune illnesses. Although closed reduction of nasal fractures is not uncommon in acute and subacute nasal fractures, no other true alternatives to elective rhinoplasty presently exist. Whether septorhinoplasty is to be performed as a hospital inpatient or an office (or hospital) outpatient procedure depends on several factors. Although traditionally this operation involved overnight hospitalization, increasingly rhinoplasties deemed to be straightforward may be accomplished safely as outpatient or office procedures, provided that no additional compromise to patient safety and well-being is involved. Regardless of the surgical setting, the preoperative evaluation and preparation remain the same, and must be exacting. Education of the patient by the surgeon and his staff is preeminent. It is essential to guide patients and the family gently through a form of self-analysis and awareness of the interdependent structures of the nose and face, an exercise that catalyzes the patient’s understanding of the scope of the deformity and operation, and the limitations imposed on the procedures by the imperfect existent anatomy. Using a three-way mirror supplemented by accurate preoperative photographs aids in the patient and surgeon arriving at a joint understanding about the nature and goals of the operation. It is absolutely essential that the patient be able to characterize exactly what outcome is desired. Even a result judged by the surgeon to be superb may fall short of the patient’s expectations without this knowledge. If, in the surgeon’s judgment, realistic motivation and understanding is present, plans are made to schedule the desired operation. If any doubt exists, it is propitious to allow a period of reflection and contemplation on the part of the patient, scheduling a second interview and consultation before any firm decision for surgery. The following is a necessarily incomplete list of characteristics of potential problem patients: • Unrealistic expectations. • Obsessive-compulsiveness, perfectionism. • Sudden whims. • Indecisiveness. • Rudeness. • Unkemptness. • Uncooperativeness. • Depression. Questionable candidates may also be: • Overly flattering. • Overly familiar. • Possessed of a minimal or imagined deformity. • A careless or poor historian. • Obsessed with being a “very important person.” • Overly talkative. • A “surgeon shopper.” • A “plasti-surgiholic.” • A price haggler. • Involved in litigation. • Disliked by the surgeon or his staff. Surgeons should be alert to the above characteristics and evaluate such patients more carefully before accepting them for appearance-changing surgery. The wise admonition “the surgeon makes his living from the patients he operates, but secures his reputation from those he refuses to operate” should be heeded. Standard classical rhinoplasty instrument sets are ubiquitous in operating theaters throughout the world. In addition, a personal preference is strongly held for the following: 1. The Dunning semisharp septal perichondrial elevator. 2. Long nasal speculum. 3. Rubin guarded osteotomes. 4. Osteotomes: 2 and 3 mm. 5. Sharpening stone (hone). 6. Tardy microsurgical RHINOBUR (Medtronic, Jacksonville, Florida, United States). An exacting preoperative analysis and diagnosis of the unique nasal deformity presenting in each patient is arguably more important than surgical skill. Skillful surgeons who fail to accurately understand (and thus correct) the many nasal variants encountered in a rhinoplasty practice stand little opportunity of achieving an excellent long-term outcome. Detailed anatomical descriptions of the nasal anatomy exist in several excellent anatomy textbooks. The following description, unlike traditional anatomy discussions, will review the specific features of nasal anatomy that directly influence the rhinoplasty operation, with emphasis on the philosophy of surgical conservatism and reorientation of the interrelated nasal anatomical components. The commonly accepted anatomical terms in rhinoplasty are illustrated in Figs. 2.2–2.5 and will prevail throughout this chapter. The nose itself represents an aesthetic unit located centrally within the other aesthetic regional units of the face. On the nasal surface, one can identify several distinct anatomical topographical subunits (Fig. 2.3).1 Individual inherited characteristics render these subunits prominent or unobtrusive. In the reconstruction of external nasal defects, it is often preferable to resect and replace an entire topographical subunit with skin of like color, character, and texture rather than simply fill the existing primary defect with a skin graft or pedicle flap. In similar fashion, during rhinoplasty the surgeon must avoid a sharp, unnatural overemphasis of any one subunit in comparison to a surrounding subunit; each should ideally blend into the other with a gracefulness that draws no attention to the nasal repair. Nasal subunits consist of the nasal dorsum, the nasal sidewalls, the nasal tip (including the infratip lobule and columella), the alar lobules, and the depressions of the supra-alar facets (Fig. 2.3). Fig. 2.3 The fundamental anatomical topographical subunits of the nose, isolated in an exploded illustration for more critical aesthetic evaluation. Both nasal reconstructive procedures and rhinoplasty techniques should incorporate an appreciation for and an understanding of the importance of restoring and rendering symmetrical these subunits. The quality and thickness of the skin and supportive subcutaneous tissues investing the nose exert a major influence on the surgical dissection in rhinoplasty and the ultimate natural appearance of the final healed result. By inspection and palpation, one can judge the character, thickness, elasticity, and overall quality of the skin to accurately estimate how much and what form of surgical correction is possible. Surgeons often prefer patients with thin, delicate skin, as they invariably develop less postoperative edema and heal more quickly. Markedly thin skin with sparse subcutaneous tissue, however, poorly camouflages even minor irregularities in the nasal supporting structures, potentially unveiling bony or cartilaginous highlights, asymmetries, offsets, or irregularities during the early postoperative healing period. Conversely, thick skin, which heals and contracts less quickly, tends toward greater postoperative edema, healing and contracting less quickly. Since subcutaneous scar formation generally is more abundant, the unwary surgeon is exposed to the possibility of one form of postoperative pollybeak deformity; this is particularly true when excessive nasal skeleton is needlessly sacrificed. Smooth draping of skin is less easily accomplished when thick skin exists; therefore, efforts aimed at surgical creation of accentuated definition, particularly at the nasal tip, are largely limited. Excision of excessive subcutaneous tissue in the nasal tip, commonly necessary in thick skin, is usually contraindicated in thin skin, since the maintenance of a pleasing, natural contour demands preservation of interposed soft tissue between skeletal structures and delicate overlying skin. Nasal skin is considerably thinner, more mobile, and more easily repositioned in the cephalic three-fifths of the nose, where it is relatively devoid of subcutaneous tissue and sebaceous glands. Progressing caudally toward the nasal tip, the skin assumes a thicker, more glandular sebaceous quality (Fig. 2.2). An ideal skin type does in fact exist for favorable results in rhinoplasty. Neither too thick nor too thin, this ideal epithelium possesses a minimum of sebaceous glands and wide pores and redrapes well after conservative undermining and elevation. Sufficient subcutaneous tissue is present to cushion the epithelium from underlying osseocartilaginous structures, but a minimum of fat is present. Gentle palpation and rolling of the nasal skin during the physical examination identify this favorable skin condition for the surgeon. The varying thickness of the skin-subcutaneous tissue sleeve plays a vital role in profile planning in rhinoplasty. The skin covering is usually thin at the rhinion and thick at the nasion and supratip area (Fig. 2.4); a slight skeletal hump at the rhinion exists even when the external epithelial profile line is relatively straight and devoid of an external humped appearance. Straight-line removal of the nasal hump (consisting of cartilage and bone) will generally result in an unacceptable profile line. The more abundant and subcutaneous tissue covering the cartilaginous dorsum creates a need for a quantitatively differential profile alignment (as opposed to bony dorsum alignment) to achieve desirable profile contouring. Whereas excessive soft tissue may require reduction in thick-skinned patients, ordinarily every effort must be made to preserve the subcutaneous soft tissues to ensure the most favorable long-term result. There are definitive tissue dissection planes in the nose and these should be exploited during primary rhinoplasty; in revisional rhinoplasty, favorable dissection planes are commonly obliterated by scar tissue. By sharp knife and scissor dissection in the immediate supraperichondrial plane over the upper and lower lateral cartilages and subperiosteal elevation over the bony dorsum, ideal soft-tissue preservation for potential cushioning and camouflage of possible slight irregularities that may develop postoperatively along the nasal profile is maintained (Fig. 2.5). Elevation of the soft tissues in this favorable plane not only creates less eventual scarring but also facilitates access to the supportive skeletal substructures of the nose and avoids the vascular and neural structures lying more superficially. Fig. 2.4 (a,b) Additional anatomical landmarks and standard terminology. 1. Nasofrontal suture line 2. Nasal bone 3. Internasal suture line 4. Osseocartilaginous junction (rhinion) 5. Nasomaxillary suture line 6. Ascending process of maxilla 7. Levator labii superioris muscle 8. Transverse nasalis muscle 9. Cephalic portion of upper lateral cartilage (articulates with undersurface of nasal bone) 10. Pyriform margin 11. Sesamoid cartilages 12. Cartilaginous dorsum 13. Upper lateral cartilage 14. Caudal free margin of upper lateral cartilage 15. Intercartilaginous tissue condensation 16. Quadrangular cartilage 17. Anterior septal angle 18. Tip-defining point alar cartilage 19. Lateral crus of alar cartilage 20. Concavity (“hinge”) of lateral crus 21. Lateral aspect of lateral crus 22. Alar lobule 23. Infratip lobule 24. Columella. 1. Apex of alar cartilage 2. Medial angle of dome 3. Lateral angle of dome 4. Alar cartilage transitional segment (intermediate crus) 5. Lateral crus alar cartilage 6. Medial crus alar cartilage 7. Medial crural footplate 8. Nostril aperture 9. Nostril floor 10. Nostril sill 11. Lateral alar sidewall 12. Alar lobule 13. Alar–facial junction 14. Anterior septal angle 15. Caudal septum 16. Maxillary crest 17. Nasal spine 18. Infratip lobule Too much emphasis cannot be placed on this all-important concept of proper nasal dissection planes. Ideally, anesthetic infiltration should be placed precisely in this supraperichondrial (superficial musculoaponeurotic system) plane in the lower half of the nose to aid in avascular dissection. The ideal base view and the terminology applied to the anatomical components are depicted in Fig. 2.6. As a bilateral and often difficult operation, rhinoplasty remains the most challenging of all aesthetic facial operations because no two procedures are ever identical. Equally importantly, total control of the healing process by the surgeon is not possible. Each patient’s nasal configuration and structure require individual and unique operative planning and surgical reconstruction. Therefore, no single technique, even when mastered, will prepare the surgeon for the varied anatomical patterns encountered. It is essential to regard rhinoplasty as an operation planned to reconstitute and shape the anatomical features of the nose into a new, more pleasing relationship with one another and the surrounding facial features. Rhinoplasty should be approached as an anatomical dissection and exposure of the nasal structures requiring alteration, conservatively shaping, repositioning, and often augmenting these anatomical elements. Excision should be kept to a minimum, and cartilage grafting should be employed when indicated. Many more problems and complications arise from overcorrection of nasal abnormalities than from conservative correction. An inappropriate technique applied persistently without regard for existing anatomy creates frequent complications. One truism, namely that “it is not what is removed in rhinoplasty that is important but what is left behind,” remains valid. Furthermore, one must comprehend clearly the dynamic aspects of operative rhinoplasty because all surgical steps are interrelated and interdependent, most maneuvers leading to a temporary deformity to be corrected progressively by the steps that follow (the “dynamics” of rhinoplasty). Sculpture of the nasal tip is regarded, and properly so, as the most exacting aspect of nasal plastic surgery.2,3 The surgeon is challenged by the bilateral, animate, and mobile nasal anatomical components. Because no single surgical technique may be used successfully in correction of the endless anatomical tip variations encountered, the surgeon must analyze each anatomical situation and make a reasoned judgment about which approaches and tip modifications are indicated and which techniques will result in a predictably natural appearance. Factored into this decision must be consideration of, among other things, the following: 1., 2. The strength, thickness, and attitude of the alar cartilages. 3. The degree of tip projection. 4. The texture and quality of tip skin and subcutaneous thickness. 5. The columellar length. 6. The length of the nose. 7. The width of the tip. 8. The interdomal distance and domal angles. 9. The tip–lip complex angulation. 10. Anatomic tension forces within the tip structures. One fundamental principle of tip surgery is that normal or ideal anatomical features of the tip should be preserved and, if possible, remain undisturbed by surgical dissection, and abnormal features must be analyzed, exposed, reanalyzed, and corrected by reduction, augmentation, or reorientation and shape modification.3 Surgeons have gradually come to understand that radical excision and extensive sacrifice of alar cartilage and other tip support mechanisms all too frequently result in eventual unnatural or “surgical” tips. What appears pleasant and natural in the early postoperative period may heal poorly because of overaggressive attempts to modify the anatomy more extensively than the tissues allow. Cross-cutting or morselization of the lateral crura may provide an excellent early appearance, but commonly results in asymmetry, bossae, and distortion or loss of tip support as the soft tissues “shrink-wrap” around the weakened cartilages over time. Rhinoplasty is, after all, a compromise operation, in which tissue sacrifices and reorientation are made to achieve a more favorable appearance. It is thus judicious to develop a reasoned, planned approach to the nasal tip based entirely on the anatomy encountered coupled with the final result intended. A philosophy of a systematic incremental anatomical approach to tip surgery is highly useful in achieving a consistently natural result (Fig. 2.7). Fig. 2.6 Favorable tissue plane over nasal skeleton is ideally entered with sharp knife elevation of the overlying skin-subcutaneous canopy during rhinoplasty. Conservative reduction of the volume of the cephalic margin of the lateral crus, preserving a substantially complete, undisturbed strip of residual alar cartilage, is a preferred operation in individuals in whom nasal tip changes are intended to be modest. As the tip deformity or asymmetry encountered becomes more profound, more aggressive techniques are required, from weakened and complete strip techniques to significant vertical interruption of the residual complete strip with profound alteration in the alar cartilage size, attitude, and anatomy. Cartilage structural grafts (tip shield grafts, columellar struts, onlay grafts, alar batten grafts, and alar sidewall grafts) to influence the size, shape, projection, and support of the tip are often invaluable. Tip sculpture cannot be successfully undertaken, let alone mastered, until the major and minor tip support mechanisms are appreciated, respected, and preserved or, when indicated, reconstructed (Table 2.1). Loss of tip support and projection in the postoperative healing period is one of the most common surgical errors in rhinoplasty. This tip “ptosis” is usually the inevitable result of sacrificing nasal tip support mechanisms. In the majority of patients, the major tip support mechanisms consist of the following: • The size, shape, and resiliency of the medial and lateral crura. • The wraparound attachment of the medial crural footplates to the caudal end of the quadrangular cartilage. • The soft-tissue attachment of the caudal margin of the upper lateral cartilage to the cephalic margin of the alar cartilage. Compensatory reestablishment of major tip support by suture repair, columellar struts, application of tip grafts, etc., should be considered if, during the operation, any or all of these major tip support mechanisms are compromised in any fashion. The minor tip mechanisms that, in certain anatomical configurations, may assume major support importance include the following: • The dorsal cartilaginous septum. • The interdomal ligament. • The membranous septum. • The nasal spine. • The surrounding skin and soft tissues. • The alar sidewalls.4 Tip projection in every rhinoplasty operation is inevitably enhanced, reduced, or preserved in its original state (Fig. 2.8). Anatomical situations in which each of these outcomes is desirable and intended are regularly encountered in a diverse rhinoplasty practice.5 The desirable surgical goal in every operation is preservation of the projection already existent, if, as is true in the majority of rhinoplasty patients, preoperative projection of the tip is satisfactory. Other patients require an increase in the projection of the tip relative to the intended new profile line. A predictable variety of reliable operative methods exist for creating or augmenting tip projection, which are discussed later in the chapter. Finally, in a limited but clearly definable group of patients with overprojecting tips, a calculated, intentional reduction of excessive tip projection is desirable to effect intentional retroprojection. Successfully achieving these diverse surgical results requires an understanding of and a healthy respect for the major and minor tip support mechanisms, seasoned by the recognition of the intraoperative surgical tip dynamic principles that interact in every tip operation.6 It clearly follows that the appropriate tip incisions and approaches should be planned to preserve as many tip supports as possible. Alar cartilage sculpturing should similarly respect this principle by conserving the volume and integrity of the lateral crus and avoiding, in all but the most extreme anatomical situations, radical excision and sacrifice of tip cartilage.
Contemporary Rhinoplasty: Personal Principles and Philosophy
2 Contemporary Rhinoplasty: Personal Principles and Philosophy
2.1 Introduction and Personal Philosophy
2.2 Indications
2.3 Contraindications
2.4 Alternative Techniques
2.5 Preoperative Considerations
2.6 Special Surgical Requirements
2.7 Preoperative Analysis
2.8 Surgical Techniques
2.8.1 Surgery of the Nasal Tip
Plastic Surgery Key
Fastest Plastic Surgery & Dermatology Insight Engine