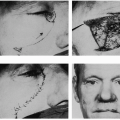
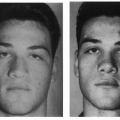
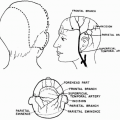
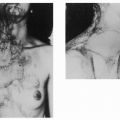
Transposed (Mcgregor) Flap in Eyelid Reconstruction
I. A. McGREGOR
EDITORIAL COMMENT
In the editor’s view, this flap, which is simpler and less involved, has supplanted the more extensive Mustardé-type flap, which was the standard for lower lid reconstruction.
This flap consists of an inferiorly based transposed flap raised on the skin area below and lateral to the outer canthus, and it is moved medially to close V-shaped full-thickness defects of the lower eyelid. Transfer of the flap leaves a triangular secondary defect laterally, and this is closed using a Z-plasty.
INDICATIONS
The reconstruction that uses this flap is primarily applicable to full-thickness defects of the lower eyelid that can be created in the form of a V, although, as discussed later, the principle also can be applied to comparable defects of the upper eyelid (1, 2). This flap can be used for defects of up to two-thirds of the breadth of the lower lid, canthus to canthus, but defects greater in breadth are unsuitable. The technique is one of the triad of reconstructions used to treat full-thickness V-shaped defects of increasing breadth (Fig. 12.1). With the narrow V, the defect can be closed directly; where the defect is broader and direct closure would be under tension, reduction of tension can be provided by dividing the slip of the lateral canthal ligament to the lower eyelid—lateral canthotomy. It is when the defect is still too broad for lateral canthotomy alone that the transposed flap has to be advanced medially to bring together the two limbs of the V and close the defect.
The method is easiest to carry out technically when an element of tarsal plate is present on both sides of the defect. The presence of the plate provides a good base for suturing the two margins of the V together, and while the method can be used for defects that abut on one or the other canthus, the absence of tarsal plate on one side of the defect makes secure closure of the defect more difficult.
FLAP DESIGN AND DIMENSIONS
Before raising the flap, the lines along which the various incisions will be made are drawn out on the skin. With the V-shaped defect outlined on the eyelid, the line that indicates the upper border of the transposed flap extends laterally from the outer canthus, continuing the upward curve of the margin of the lower eyelid, to just short of the temple hairline. The upward curve is required to provide an adequate vertical height of the reconstructed eyelid segment and to avoid ectropion.
From the lateral extremity of this line, a further line is drawn in a generally downward direction parallel to the lateral limb of the V on the eyelid, the angle between the two lines being approximately 60°. The effect is to outline a flap with the overall shape of a parallelogram. As already indicated, transfer of the flap medially leaves a triangular defect that is closed by a Z-plasty. This is designed at this stage, before any skin incisions are made, constructed around the lateral part of the line representing the upper margin of the flap. This acts as the common limb of the Z, it and the line representing the lateral margin of the flap together forming one of the Z-plasty flaps. Design of the Z-plasty is completed with the drawing of a line that runs upward and laterally from the upper margin of the flap, outlining the second Z-plasty flap.
OPERATIVE TECHNIQUE: LOWER EYELID DEFECTS
With the V excision of the full thickness of the eyelid completed, the flap, as outlined, is raised at the face lift level lateral to the orbicularis oculi. When the orbicularis is reached, the plane of elevation becomes deep to the muscle, the muscle being advanced as part of the flap. In the process of elevating the flap, the slip of the lateral canthal ligament to the lower eyelid is divided. This division can be carried out as a formal step, but the ligament can just as effectively be felt as a resistance to medial flap advancement and be divided.
With a skin hook to gently pull the flap medially, sites of resistance to advancement can be identified with the finger and divided with scissors. In the process, much of the lower border of orbicularis is divided, as well as the orbital septum, neither structure being divided as a formal, visualized step, but rather felt as a focus of resistance to medial advancement. The amount of tissue that must be divided in this way depends very much on the breadth of the V and the amount of flap advancement required to
approximate its two limbs. A broad V necessitates more extensive soft-tissue division; a narrow V, less. Division must be continued until the flap can be advanced to close the defect with a minimum of tension. The extent of mobilization required also depends to some extent on the preexisting laxity of the eyelids and local tissues generally. When the amount of soft-tissue division is considerable, the flap may ultimately appear to be attached inferiorly by little more than the skin and immediately subcutaneous tissues superficially and the conjunctiva deeply. There should be no particular concern about this. In contrast to the cheek rotation flap used in lower eyelid reconstruction, with its recognized vulnerability to necrosis, the ratio of length to breadth and the relative smallness of the transposed flap make it safe.
approximate its two limbs. A broad V necessitates more extensive soft-tissue division; a narrow V, less. Division must be continued until the flap can be advanced to close the defect with a minimum of tension. The extent of mobilization required also depends to some extent on the preexisting laxity of the eyelids and local tissues generally. When the amount of soft-tissue division is considerable, the flap may ultimately appear to be attached inferiorly by little more than the skin and immediately subcutaneous tissues superficially and the conjunctiva deeply. There should be no particular concern about this. In contrast to the cheek rotation flap used in lower eyelid reconstruction, with its recognized vulnerability to necrosis, the ratio of length to breadth and the relative smallness of the transposed flap make it safe.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree