This article’s raison d’etre is simple: to deliver a decidedly lucid and sanguinely compelling description of a lower eyelid surgical rejuvenation strategy. By bestowing the surgeon greater control of the lower eyelid, a more esthetic result with fewer complications can be reliably delivered. The pinch blepharoplasty does so by offering 3 unique advantages: First, it respects and preserves both esthetic and functional eyelid posture. Second, it treats the excess eyelid skin and wrinkles comprehensively. And third, it simultaneously addresses the orbital and nasojugal grooves.
Key points
- •
The pinch blepharoplasty procedure offers a confoundingly simple but reliable and safe strategy for lower eyelid rejuvenation.
- •
The pinch blepharoplasty technique must be married to an equally well-executed lateral canthopexy if it is to be maximally harnessed and confidently executed.
- •
The pinch blepharoplasty approach delivers a correction of the aging eyelid that is distinctly comprehensive with its deliberate address of the excess skin, the periorbital/nasojugal grooving, and the eyelid posture.
Video content accompanies this article at http://www.plasticsurgery.theclinics.com .
Introduction
At the risk of sounding hyperbolic, the pinch blepharoplasty has, more than any other strategy, propitiously altered the trajectory of not only my esthetic practice but also my surgical philosophy itself. How you may ask, could one simple twist of technique deliver so profoundly? The answer is that, like so many other technologies, it is usually the ones that appear to be obviously so much better … only after you have experienced their predecessors.
Well that is exactly what happened in my hands with the lower blepharoplasty. The pinch blepharoplasty is a truly transformative strategy that has revolutionized my approach to eyelid surgery, offering unparalleled control and esthetic results. And I am equally as gratified that many others have since adopted this approach. However, it has been my observation that what is being declared as a “pinch blepharoplasty” is not quite. That is, the pinchplasty wounds are still originating far too close to the eyelid margin, the pinchplasty walls are persistently too timid in their girth, and finally, the canthopexy stratagem is not being consistently invoked. So, it is the express purpose of this study to review the arc of the pinch blepharoplasty’s evolution and my accompanying learning curve and then elucidate the exact “specifications” of its present state of the state.
A brief history of the lower pinch blepharoplasty
One can only appreciate the birthing of the modern iteration of the pinch blepharoplasty with an understanding of what came before it. And I purposefully have used the word birthing because its evolution has been decidedly protracted, making it a veritable diorama of fits and starts: from its initial introduction as a simple skin excision in the 1920s , to profound neglect—for almost 50 years—until its resurrection in the early 1970s as a case report with the first description of a proper pinch excision only to suffer another fallow 20 years until the early 1990s with the publication of another “pinch” case report. Then my years-long hum of dissatisfaction with the skin–muscle technique was interrupted by a stroke of serendipity one night, within one presentation slide that revealed the pinching of the excess eyelids. , Inspired, this author went on to apply this tactic on a clinical series of patients, definitively proving its efficacy. ,
My “learning curve” with the pinch blepharoplasty
In the Beginning
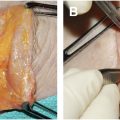
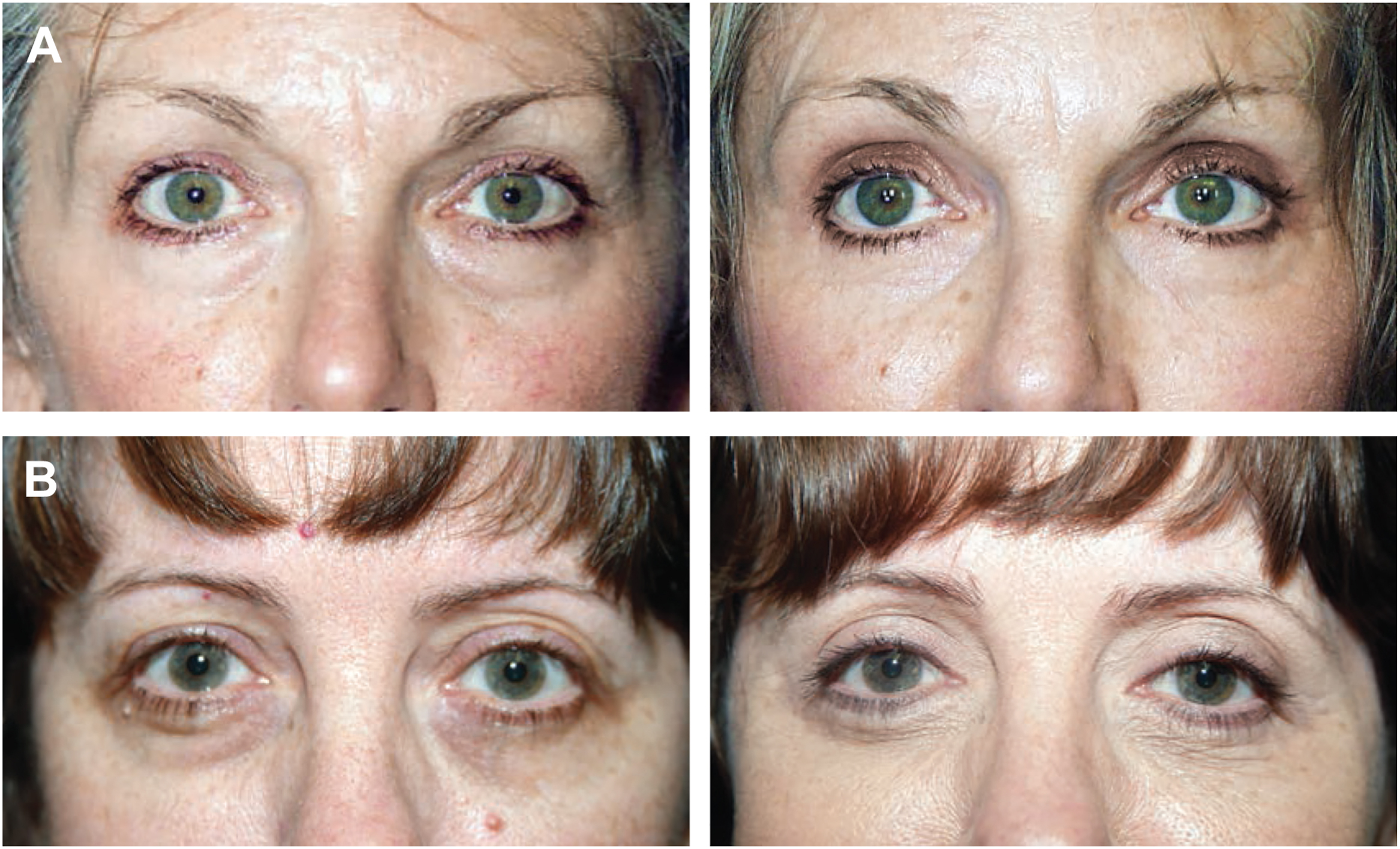
I say “learning curve” because of all the surgeries I have practiced, none has illustrated the concept of iterative improvement more. Reflecting on my early experience with this blepharoplasty, I was inspired, or perhaps it would be more forthright to say, I was chastened by my consistently inconsistent results. I was originally schooled on the reigning gold standard, the skin–muscle flap strategy. And to be fair, it served and still serves up very acceptable outcomes—most of the time. And there is the rub—I witnessed untreated wrinkled eyelid skin and/or compromised eyelid posture. Surgeons invoked heroic offensive strategies for skin flap support, such as the flap to orbital rim, “mother of all stitches,” as dubbed by my partner Gil Gradinger. Others abandoned the skin muscle flap angle altogether and instead combined a transconjunctival approach for treatment of the fat and a CO 2 laser for resurfacing of the skin. But despite my diligent application of these and many other variations on the theme, both scleral show and redundant skin sporadically plagued my results ( Fig. 1 A, B ).
Steal like an Artist
Great ideas are often described by the “inventor” as a classic “in the bathtub” eureka moment. This yarn may sound good at the podium or on the page, but that is not how most advances are actually birthed. Instead, the path to “better” is usually one paved by a labyrinth of uneven but sometimes revelatory steps. And on this journey, one becomes primed to adopt—or rather steal—any better idea that could facilitate a leap. Well, one seminal night in 2000, Dr. Glenn Jelks clicked his next slide to display 2 Brown Adson’s pinching the lower eyelid skin into a standing wall of redundancy, aching to be amputated like an overgrown skin tag. That was my supposed “aha” moment—but what was really the final piece of my dogged puzzle. And this potent strategy had literally been sitting in plain sight since the early 1970s when Parkes and colleagues first published a description of the skin pinch, and Dinner, in the early 1990s, first married the transconjunctival approach for the fat treatment to the pinch technique for skin excision. And I must confess that I also “stole” from myself: or at least from my evolving strategies treating excess tissue in other zones of the body—namely the facelift and the abdominoplasty. Aged tissue, no matter its location, need not be undermined or otherwise mobilized in order to be tightened or excised. This insight became a girding principle in the powerful lateral recruitment and redraping of neck skin in my pinch rhytidoplasty and in the effective discontinuous dissection and advancement of abdominal skin in my high-tension abdominoplasty. , Thus, it was not a giant leap to now reconsider lower eyelid excess/wrinkling as it is nothing more than what may be analogized to a rumpled bed.
Version 1.0
So, I went to work applying the transconjunctival (TC)-Pinch strategy to about a hundred cases in the early 2000s and published my first report in 2005 in plastic reconstructive surgery (PRS).
With this first series, the following surgical principles were evinced:
- 1.
To avoid any distortion of the eyelid skin, local anesthesia was injected either before the patient sterile prep or if under general anesthesia not until after the pinch itself.
- 2.
Originally, the path of the pinch followed the same trajectory as my skin muscle flap incision as a straight line within a few mms of the eyelid margin preserving a lateral wedge of intervening eyelid skin as a bulwark against possible scleral show—a la Gradinger’s personal communication.
- 3.
A canthal tightening, reminiscent of Dr. Fagien’s original description, was employed only if the patient demonstrated obvious scleral show or eyelid laxity.
- 4.
A second stage, “re-pinch,” was invoked, preferably planned, in cases with voluptuous skin excess ( Fig. 2 A–E ).
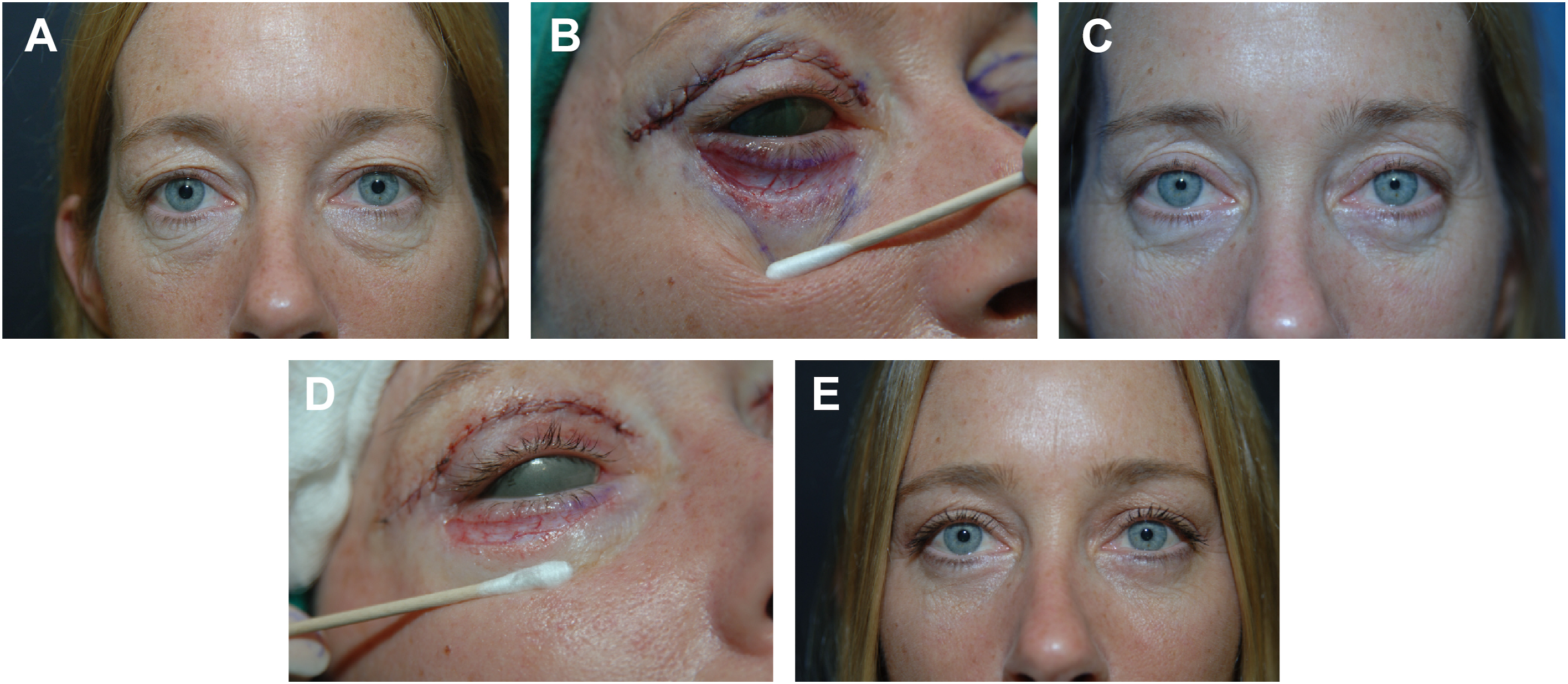
Fig. 2
( A ) 49 year old woman preoperative first pinch. ( B ) Intraoperative first pinch wound. ( C ) Postoperative first pinch 10 months. ( D ) Intraoperative second pinch wound. ( E ) Postoperative second pinch 9 months.
The power of this pinch soon became undeniable: its effect was similar to the making of a rumpled, wrinkled bed. That said, upon my painfully honest assessment, I identified cases of both persistent skin that necessitated an unplanned re-pinch and subtle scleral show despite being initially exempt from the stitch canthopexy.
Version 2.0
I went back to the operating room—our proverbial “drawing board”—and made some edits to the original guiding rules of conduct for this strategy:
- 1.
The latitude of the pinch drifted slightly southward to proffer additional insurance against eyelid posture distortion.
- 2.
Beyond the stitch canthopexy for therapeutic purposes, a “prophylactic” iteration was also adopted. This principle could be compared to the tightening of a clothesline before one hangs the wet clothes. Now all patients enjoyed some form of eyelid tightening and the stigmatizing scleral show was further obviated.
This new and improved iteration of the pinch technique was then reported in aesthetic surgery journal (ASJ).
Version 3.0
And now we come to the centerpiece of this update: the insights, strategies, and outcomes that have evolved over the last 25 years since my original “rediscovery” of the pinch technique’s remarkable promise. Now I can state unequivocally—after well over 3500 cases—that the pinch technique has proven to be a superior strategy to the lower eyelid blepharoplasty.
The present elements of the technique that have been honed to realize ever-improving outcomes are enumerated in the following:
- 1.
As much as the aforementioned “re-pinch” was very effective at cleaning up most of the lingering lower eyelid skin, having to contemplate, even if planned, a second surgery was incentive enough to seek to reduce this predestined revision rate. The only way to do so was to go as Willy Sutton would have declared if he had been asked why venture lower on the eyelid: “Because that is where the excess skin is!” But to do so would mean daring to go beyond the lid margin—our preferred latitude since the beginning of time. Well, a page was taken from my orbital floor fracture playbook of yore—that is, making a point of entry into the eyelid excess at decidedly lower latitude with predictably imperceptible scarring. And so the lower pinch came to pass and my pinches crept ever lower on the eyelid and its full potential unleashed with its brazen placement in the very center of the skin excess, delivering a heretofore unrealized robust, verily comprehensive skin excision. One could envision this antipodal strategy as akin to addressing a roll in a large living room carpet most effectively by moving instead to the same side of the carpet as the roll ( Fig. 3 A–C ).
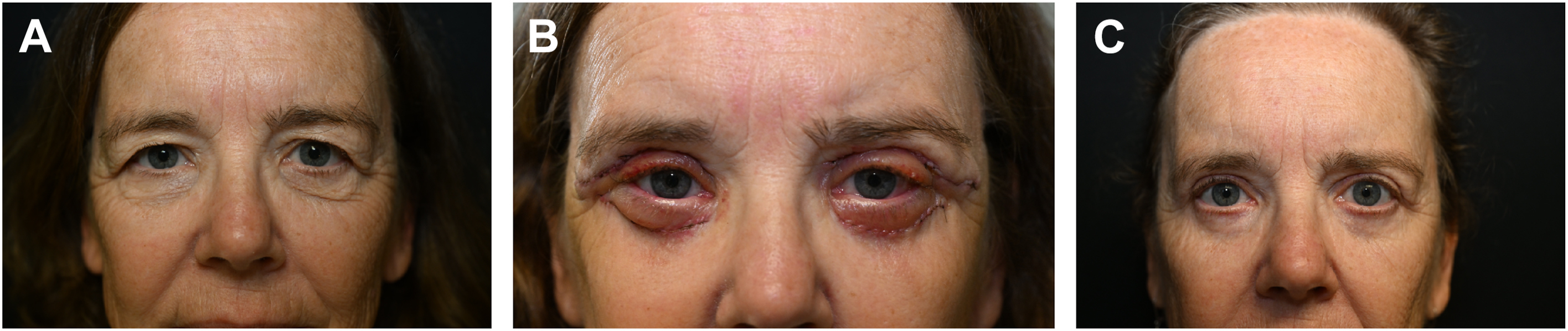
Fig. 3
( A ) 63 year old woman pre-pinch lower and upper blepharoplasty. ( B ) Postoperative day 5. ( C ) Postoperative 12 mo.
- 2.
As my confidence grew in both the efficacy and safety of this hearty pinch, I shifted my focus to the now popular hot topic in the world of blepharoplasty: the periorbital/nasojugal groove. Efforts were being made by our profession to address this “deformity” very directly with autologous fat grafting or infraorbital fat repositioning—with or without orbicularis retaining ligament (ORL) release. Although these strategies can certainly be effective, their unpredictable results and inherent revision rates are simply above, what I call, my complications “boiling point.” , , So I was motivated to review my results up to then and happily noted a definite improvement in the nasojugal/orbital grooves, albeit by indirect means. This effect is akin to the aforementioned making of a messy bed and simultaneously covering a hole in the mattress ( Fig. 4 A, B ).
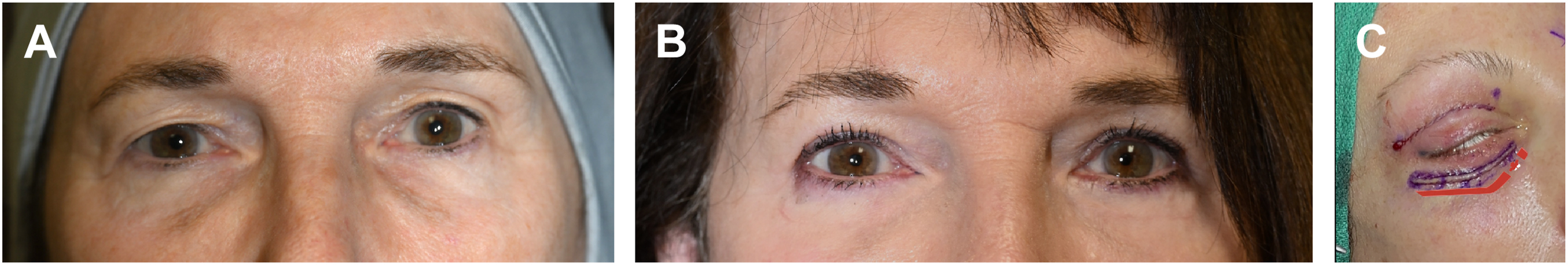
Fig. 4
( A ) 79 year old woman pre-pinch with groove. ( B ) 9 months postoperative with groove correction. ( C ) Intraoperative hockey stick pinch.
- 3.
So now, with my pinch already lower on the eyelid—and ever closer to the groove—an effort was made more deliberately to efface the nasojugal groove by gathering the skin mirroring its trajectory, thus describing a “hockey stick”-shaped wall ( Fig. 4 C).
- 4.
And to facilitate and maximize all of the previous strategies, the addition of hyaluronidase to the local anesthesia delivered a more robust and stable pinch wall ( [CR] pinch w/hyaluronidase).
Present state of the state
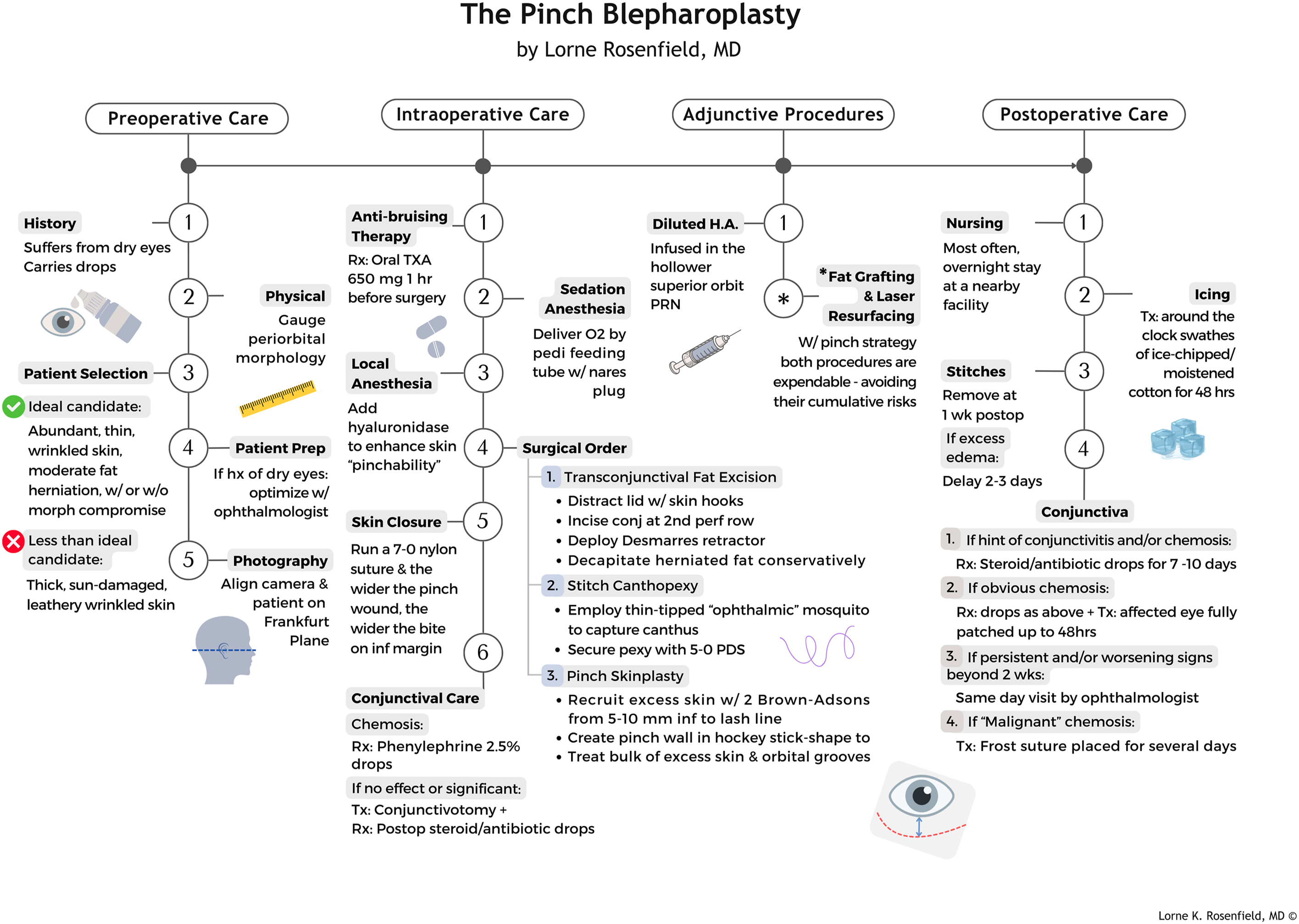
The Pinch Blepharoplasty in 2024
With an experience of well over 3500 cases and counting, the following expository highlights my present working blepharoplasty algorithm.
Preoperative care
- 1.
History : The single most important question to ask is whether the patient suffers from dry eye. And the magnitude of this symptom can be elicited by asking whether the patient presently carries drops in their pocket or purse. If there is indeed a significant history, the patient should be evaluated and “optimized” by an ophthalmologic surgeon prior to surgery.
- 2.
Physical : The most important data point to collect is a measure of the various components of the patient’s periorbital morphology: the size of the globe, the posture and stamina of the eyelid, the projection of the malar, and cant of the palpebral fissure. ,
- 3.
Patient selection : As much as this strategy is efficacious for all comers, like any technique, some patients are particularly better or particularly poorer candidates than others.
That said, the ideal candidates are those with
- •
Not surprisingly, a presentation of an abundance of wrinkled, thin skin coupled with a moderate excess of herniated fat countenances the most accurate and effective pinch possible ( Fig. 5 A, B ).
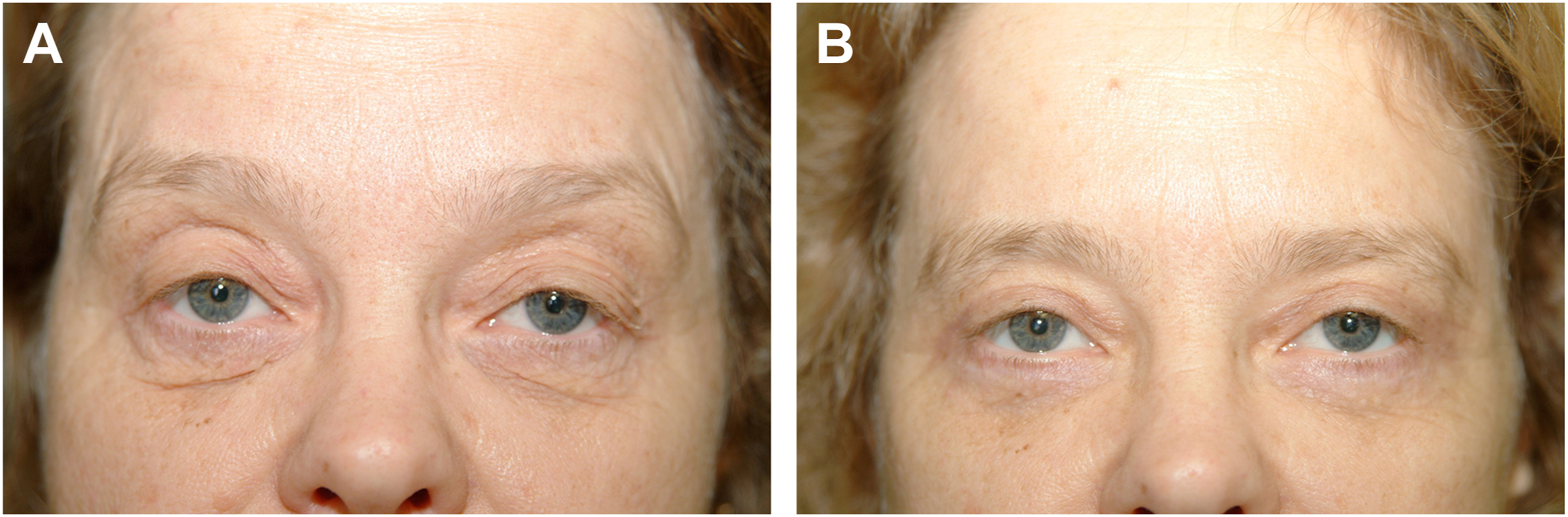
Fig. 5
( A ) 63 year old woman prepinch. ( B ) Post 9 months pinch.
- •
Paradoxically, a morphologically compromised facies, for although normally something to be feared, is now neutralized by the dynamic duo of the pinch and pexy. And one could tout that it is possible to not only prevent worsening of preexisting scleral show but to even improve upon it ( Fig. 6 A, B ).
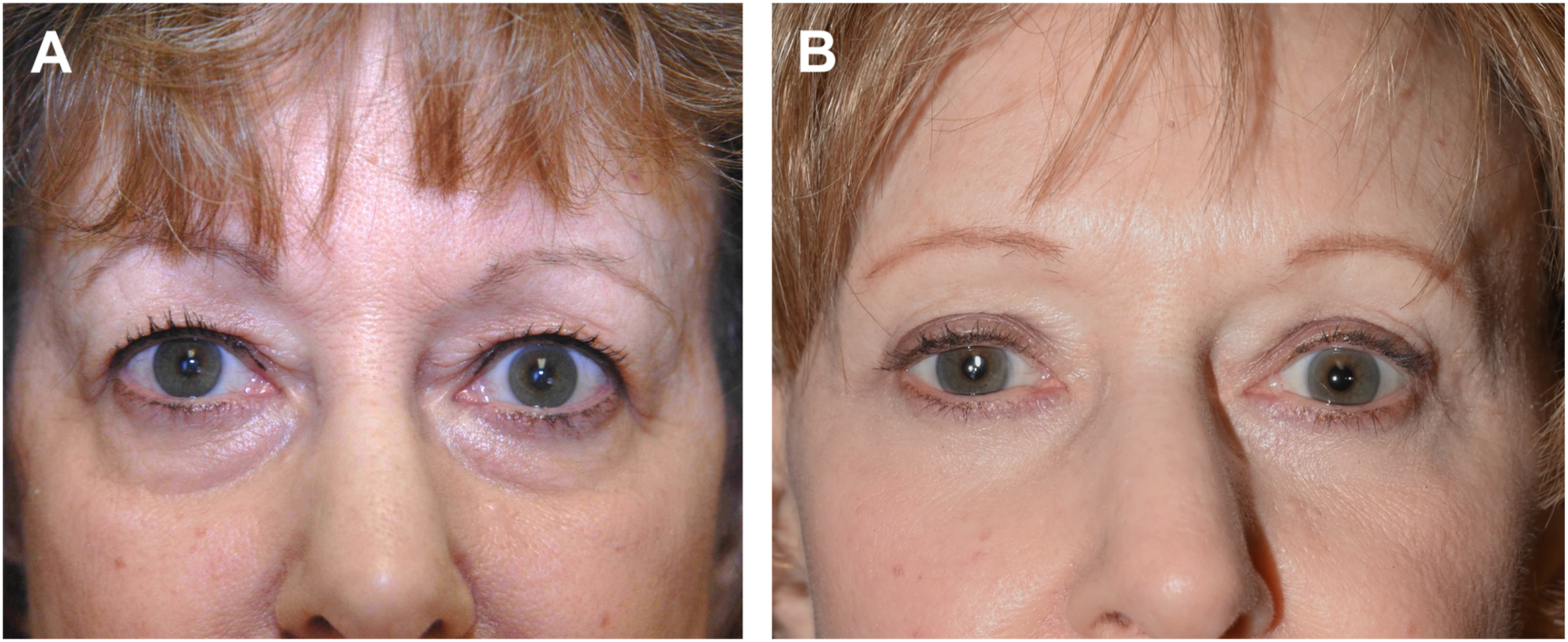
Fig. 6
( A ) 64 year old woman prepinch with scleral show. ( B ) Post 3 years blepharoplasty with corrected posture.
- •
The less-than-ideal candidates present with
- •
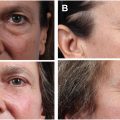
Thick, sun-damaged, leathery wrinkled skin, which inhibits the surgeon’s ability to most accurately and comprehensively pinch this redundancy ( Fig. 7 A, B ).
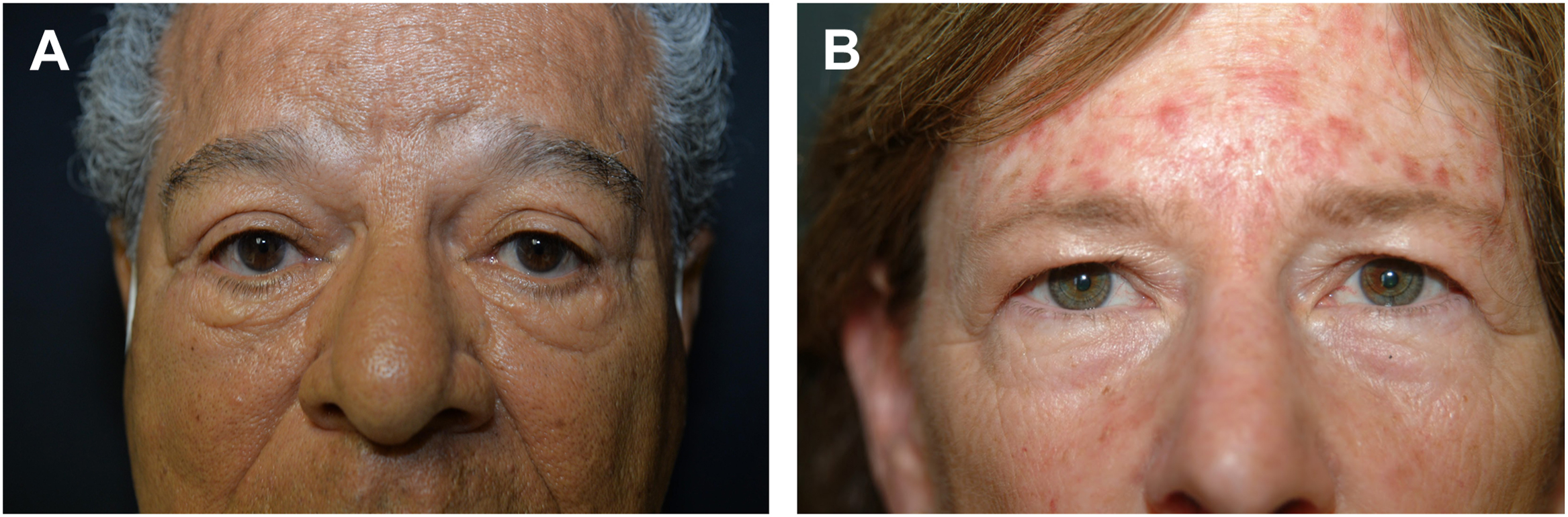
Fig. 7
( A & B ) Thick or sun-damaged skin.
- •
- 4.
Patient Prep : As noted earlier, if there is a history of dry eye, the patient is “optimized” by an ophthalmologist prior to surgery.
- 5.
Photography : The camera and the patient must be studiously aligned on the Frankfurt plane fairly and accurately document the posture of the eyelid margin relative to the globe lest a scleral show may be either concealed or magnified unwittingly.
Intraoperative care
- 1.
Antibruising therapy : An oral dose of tranexamic acid (TXA) 650 mg is now routinely given 1 hour before the surgery.
- 2.
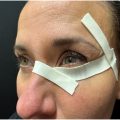
Sedation anesthesia : To negate the risk of O 2 delivery while utilizing a bovie, it is recommended that a trans nasal feeding tube be placed along with of a compressible plug at the opening of the nares ( Fig. 8 A ).
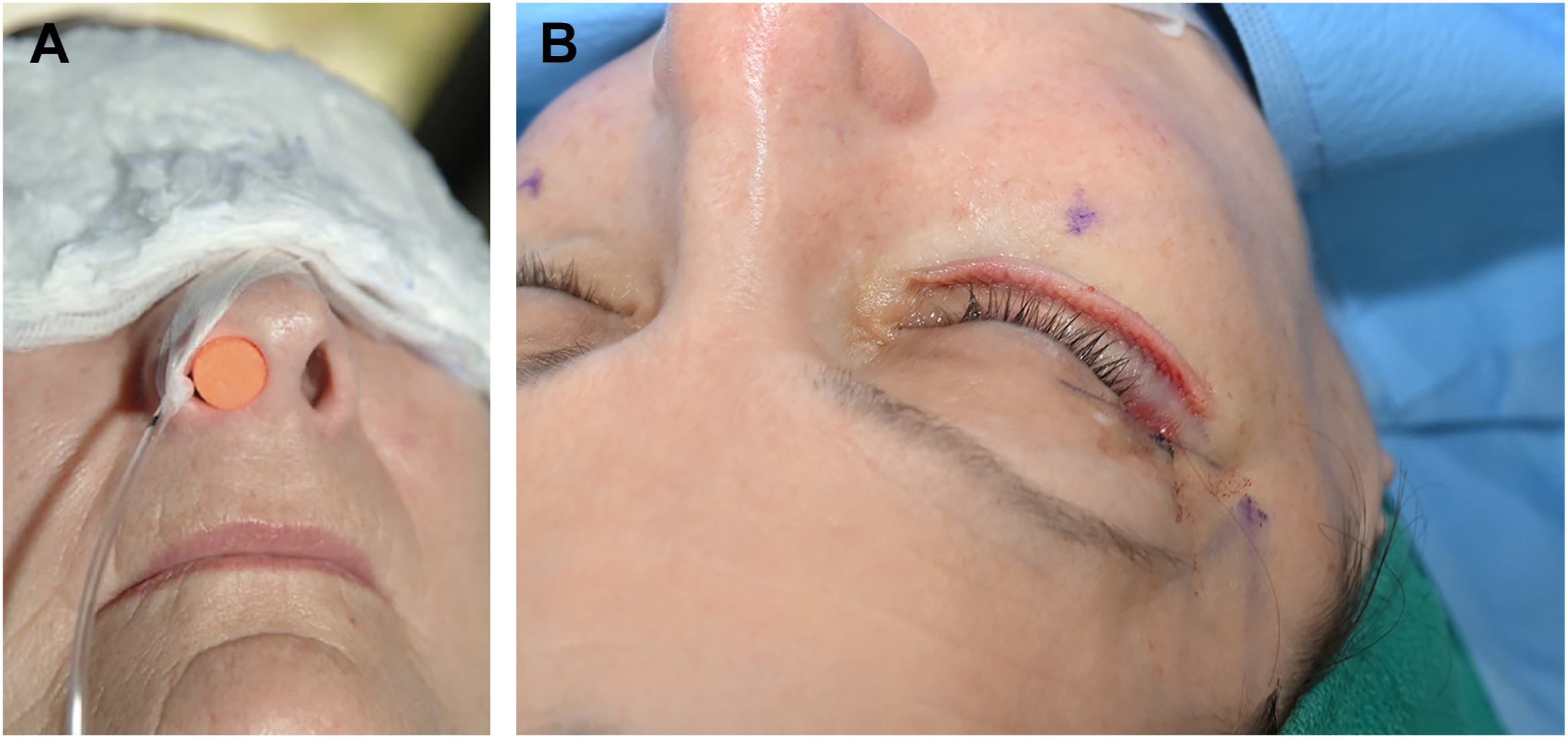
Fig. 8
( A ) Intraoperative nasal plug. ( B ) Intraoperative pinch wall with hyal.
- 3.
Local anesthesia : The local anesthetic is now injected into the lower eyelid at the start of the surgery because of the addition of hyaluronidase, as suggested by a visiting colleague (Dr. Steven Teitelbaum), that dramatically enhances the “pinchability” of the skin: not only can more of the redundancy skin now be recruited but the resultant wall of excess is far more stable, dispelling the prior necessity to conduct the skin excision as soon as possible for fear of its collapse ( Fig. 8 B).
- 4.
Surgical “order” : It is critical that the surgical steps be conducted in an advantageous order:
- •
If a transconjunctival excision of fat is to be conducted, then it is best performed before the canthopexy to take advantage of the facile distraction of the eyelid.
- •
And the pinch should be conducted after the canthopexy and equally so if an upper blepharoplasty is to be performed, since both of these antecedent maneuvers will certainly “pretreat” some fraction of the skin redundancy.
- a.
Transconjunctival fat excision : For the most facile exposure strategy, the lower lid is distracted with a couple of skin hooks, the conjunctiva divided with electrocautery, and a Desmarres retractor deployed, bringing the post-septal fat immediately into clear view, ready for the plucking. Of note, to ensure both a post-septal plane of dissection and ample conjunctival edge for closure, the transconjunctival incision should be conducted in line with the second horizontal row of perforators, usually about 1 cm or more inferior to the lid margin.
- b.
Stitch canthopexy : This now integral step in all blepharoplasties is conducted with a uniquely thin-tipped “ophthalmic” curved mosquito that is meant to capture whatever ensures a visibly definitive translation of tightening of the eyelid. After experiencing issues with visible knots in the thin patient—with clear nylon—and stitch abscesses—with braided suture—I have landed upon the presently most reliable option of a 5-0 polydioxanone (PDS) suture ( [CR] stitch canthopexy).
- c.
Pinch skinplasty : The eponymous seminal step of creating a skin pinch wall of excess skin is now conducted with 2 Brown–Adson forceps. The path of the pinch follows strategic coordinates to recruit the maximum of skin excess while also “treating” the grooves. So the pinch is purposefully placed within the sea of the excess, thus often well below the eyelid margin and parallel to the orbital and nasojugal grooves, and hence, in a hockey stick-shaped fashion ( [CR] big pinch and [CR] j pinch).
- a.
- •
- 5.
Skin closure : A running 7-0 nylon suture is utilized to close the lower eyelid wound. And the wider the pinch wound, the more important it is to take a commensurately wider bite on the inferior margin to successfully preclude a dog ear.
- 6.
Conjunctival care : Should a potentially blossoming chemosis be evident during the surgery, then phenylephrine 2.5% drops are applied. If little effect is noted and/or chemosis is otherwise significant, then a conjunctivotomy is conducted along with a postoperative prescription for steroid/antibiotic drops.
Adjunctive procedures
The “pinch-pexy” strategy does indeed gratifyingly deliver the primary aspirations of a superior esthetic result, but there is one potential adjunctive procedure that rounds out the necessary armamentarium:
- •
Diluted hyaluronic acid : As has been demonstrated, a lower, robust pinch can reliably address, if not entirely, the majority of the periorbital/nasojugal groove. However, in patients presenting with a naturally deep-set but now too hollow superior orbit, then it may be treated with a diluted hyaluronic acid as originally so elegantly described by Lambros. , This strategy, like the pinch, is both simple and effective. And unlike the alternative, autologous fat grafting, it is easily adjustable and reversible. And rarely, should the lower, hardy pinch not fully efface the more advanced periorbital groove, then this author has repurposed the Lambros “dilution solution” elixir filler injection strategy postoperatively to efficaciously clean up the remaining deformity ( Fig. 9 A, B ).
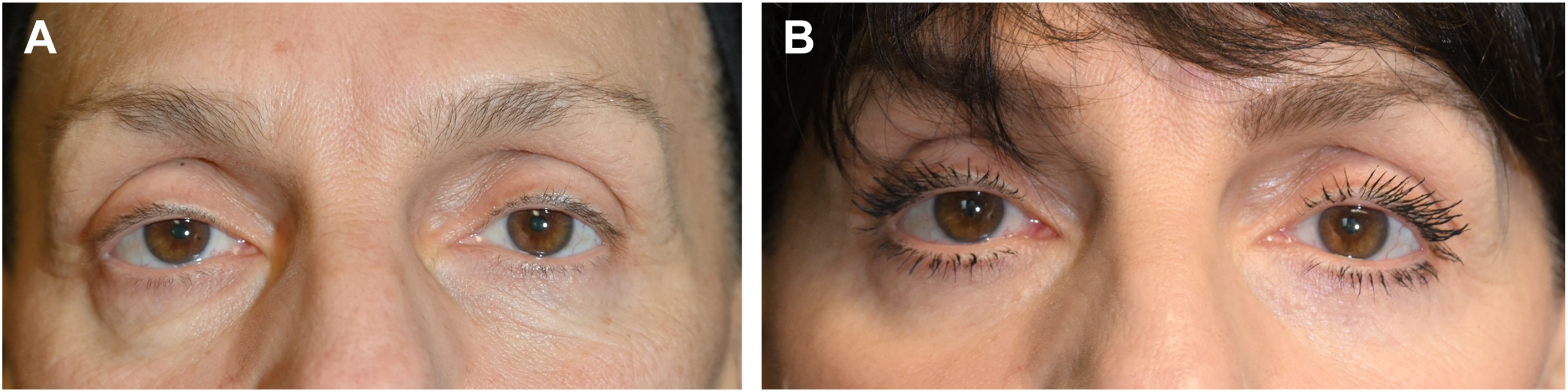
Fig. 9
( A ) 62 year old woman prepinch. ( B ) Postoperative 16 mo and diluted hyaluronic acid filler to lower periorbital.
- •
Note : As for the traditionally applied modality of laser resurfacing/chemical peeling, although once an integral strategic component of the pinch-pexy is mentioned only to declare it as expendable now that the pinch-pexy has so thoroughly addressed the skin itself. And doing so has avoided the additional risks of depigmentation and reduced the additional odds of scleral show.
Postoperative care
- 1.
Nursing : Most often, and always if in conjunction with a facelift, the patient is recovered at least overnight, at a nearby facility with 24 hour nursing care. Beside the immediate and consistent delivery of the best care, it vanquishes any and all anxiety on the part of not only the patient but that of the designated caregiver.
- 2.
Icing : Swathes of iced-chipped cotton are applied to the eyelids around the clock for at least 48 hours along with natural tears throughout the day and lubricating ointment at night.
- 3.
Stitches : At 1 week postoperative, all the sutures are usually removed and otherwise clipped at intervals if there is still significant edema with complete extraction some 3 or 4 days later.
- 4.
Conjunctiva : If there is even a hint of conjunctivitis and/or chemosis, steroid/antibiotic drops are swiftly prescribed and continued for between 7 and 10 days. And if the patient presents with obvious chemosis, beyond the medicinal drops, the affected eye is often fully patched shut for up to 48 hours, a strategy that has been impressively effective. Ultimately, should the patient return with persistent and/or worsening signs beyond 2 weeks or so, they are seen the same day by a local ophthalmologist—at my expense—to ensure that the most efficacious therapeutic strategies are in place. Rarely, if the chemosis is truly “malignant” in character, then a Frost suture is placed for several days, a stratagem that has also been faithfully victorious.
To bring the earlier algorithm alive, it has been transmuted into a visual algorithm to proffer additional clarity ( Fig. 10 ).