In the first part of this 2 part series, we describe the comprehensive evaluation of the overhead throwing athlete’s shoulder. The physical examination of the throwing shoulder requires a comprehensive knowledge and familiarity with anatomy, kinesiology, pathology, and unique sporting demands. The history, systematic basic examination, and special testing of the rotator cuff, biceps and superior labrum anterior and posterior lesions, instability and labral pathology, and scapular dyskinesia will be covered in this review.
Key points
- •
The examination of the shoulder in throwing athletes is integral to narrow the differential diagnosis, pinpoint patient symptoms, and build patient rapport.
- •
The physical examination of the rotator cuff is separated into impingement tests (external and internal) and testing for tears (partial and full thickness).
- •
There are a multitude of superior labrum anterior and posterior tests, with those that recreate the peel-back mechanism of the superior labrum-biceps anchor complex providing the lowest rate of false negatives.
- •
Testing for shoulder instability can include both quantitative testing for laxity and binary result tests for instability.
- •
The scapula and scapulothoracic kinematics are essential to shoulder function in throwing athletes and should always be included as part of the physical examination of the overhead thrower’s shoulder.
Introduction
The physical examination (PE) of the throwing shoulder requires a comprehensive knowledge of anatomy, pathology, and unique sporting demands. Although advanced imaging has revolutionized musculoskeletal diagnosis, the PE continues to provide invaluable information, patient rapport, and relevance of pathologic findings that cannot be replaced, and physicians of the throwing athlete should always begin with a thorough examination of the shoulder after a detailed history. In this review, we discuss the comprehensive PE of the thrower’s shoulder.
The basics
Inspection and Palpation
The examination of the shoulder should proceed in a systematic order. Inspection should be performed with the patient’s chest up exposed, with modesty maintained in female individuals. Symmetric contours of the patient’s shoulders should be compared. Any isolated atrophy of the supraspinatus or infraspinatus provides a clue toward suprascapular neuropathy. Deltoid or teres minor atrophy indicates axillary nerve pathology (ie, quadrilateral space syndrome) and scapular winging indicates either long thoracic (medal winging) or spinal accessory neuropathy (lateral winging). Asymmetry between the pectoralis major or biceps brachii can indicate tendon rupture. , The shoulder should then be palpated for pain generators, including the acromioclavicular (AC) joint, Codman’s point indicating supraspinatus insertion pathology (just distal to the anterolateral corner of the acromion with the shoulder extended and internally rotated), bicipital groove, scapular spine and acromion, and posterior glenohumeral joint. ,
Range of Motion Testing
Consistent and accurate range of motion testing should be performed systematically. Forward elevation (FE) in the plane of the scapula, forward flexion (FF) in the sagittal plane, abduction in the coronal plane, external rotation (ER) with the shoulder adducted by the side and abducted to 90°, and internal rotation (IR) both behind the back and with the shoulders abducted to 90° should be examined for asymmetric differences with the patient upright. Throwers, in particular, will often have increased ER and decreased IR of the throwing extremity compared to the contralateral, which is often physiologic. If an IR difference of 20° exists compared to the contralateral arm, or the total arc of motion is decreased greater than 10°, glenohumeral internal rotation deficit is considered. Our preference is to view the patient from behind, for the additional ability to view both scapulae simultaneously. Rotation testing should lastly be performed with the patient supine, with a small bolster under the humerus to prevent posterior sag of the upper extremity. This was a particular point of emphasis from Silliman and Hawkins, as the most accurate assessment of true glenohumeral rotation could be obtained by placing a finger on the coracoid during ER and IR testing, documenting rotation until coracoid movement, and eliminating scapulothoracic contribution to overall shoulder rotation.
Neurovascular Testing
The examination of the joints above and below is essential, which for the shoulder involves a thorough cervical spine examination, including strength and sensation testing of C5 to T1. Although the rich anastomoses of vasculature about the shoulder often prevent any vascular abnormalities until late in disease courses, symptoms of arm heaviness, decreased endurance, or cold intolerance should raise suspicion for vascular disorders such as arterial/venous thoracic outlet syndrome or axillary artery compression. Overhead athletes are particularly at risk given the frequency of exacerbating position of shoulder hyperabduction and ER, hypertrophied pectoralis minor, or subclinical anterior humeral head subluxation that can compress the axillary artery, and an Adson test should be performed in all athletes with these complaints. Lastly, special testing of specific pathologies within the examining surgeons’ differential diagnosis should be performed, as described in the following sections.
Rotator cuff
Impingement Tests
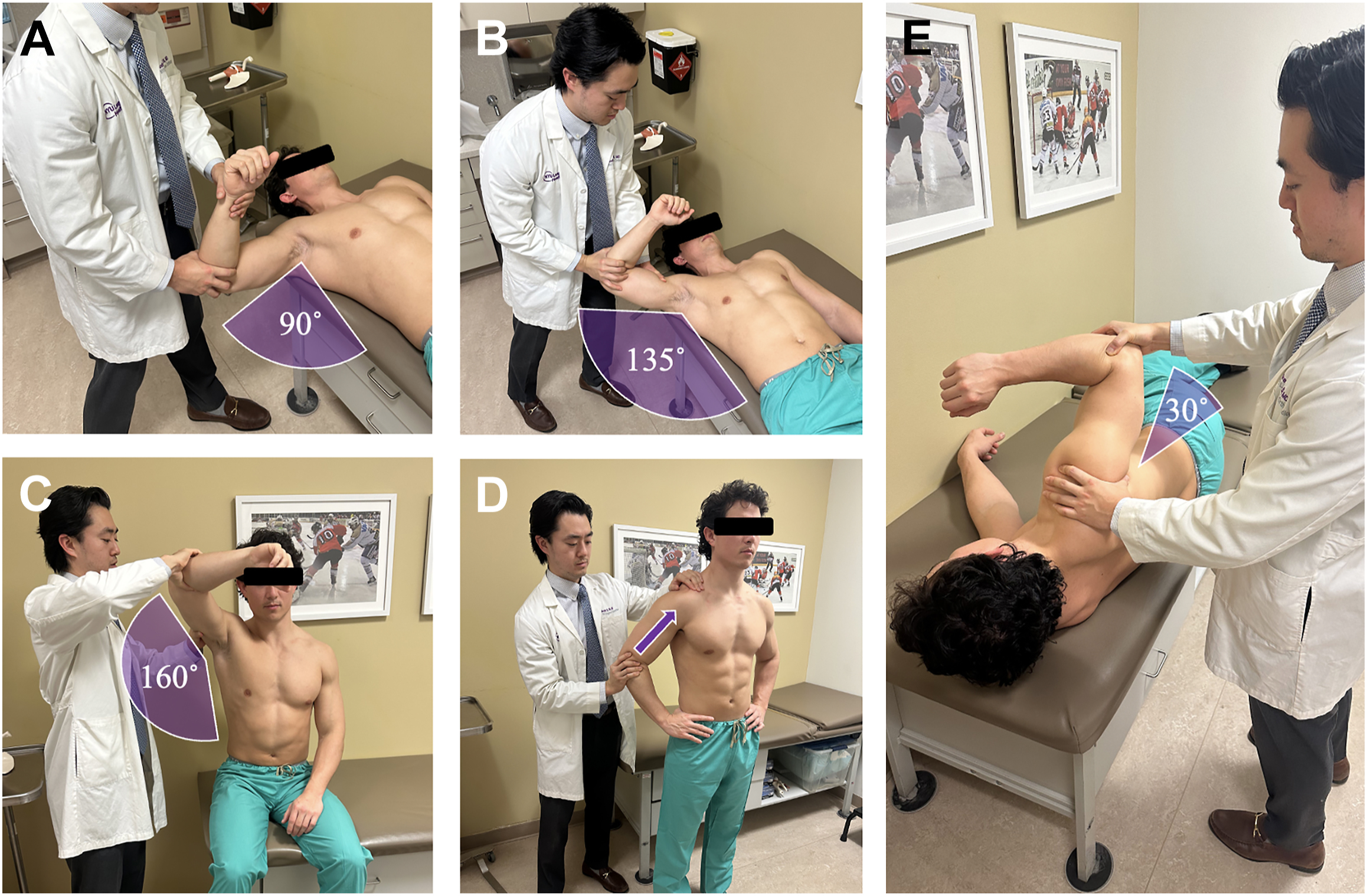
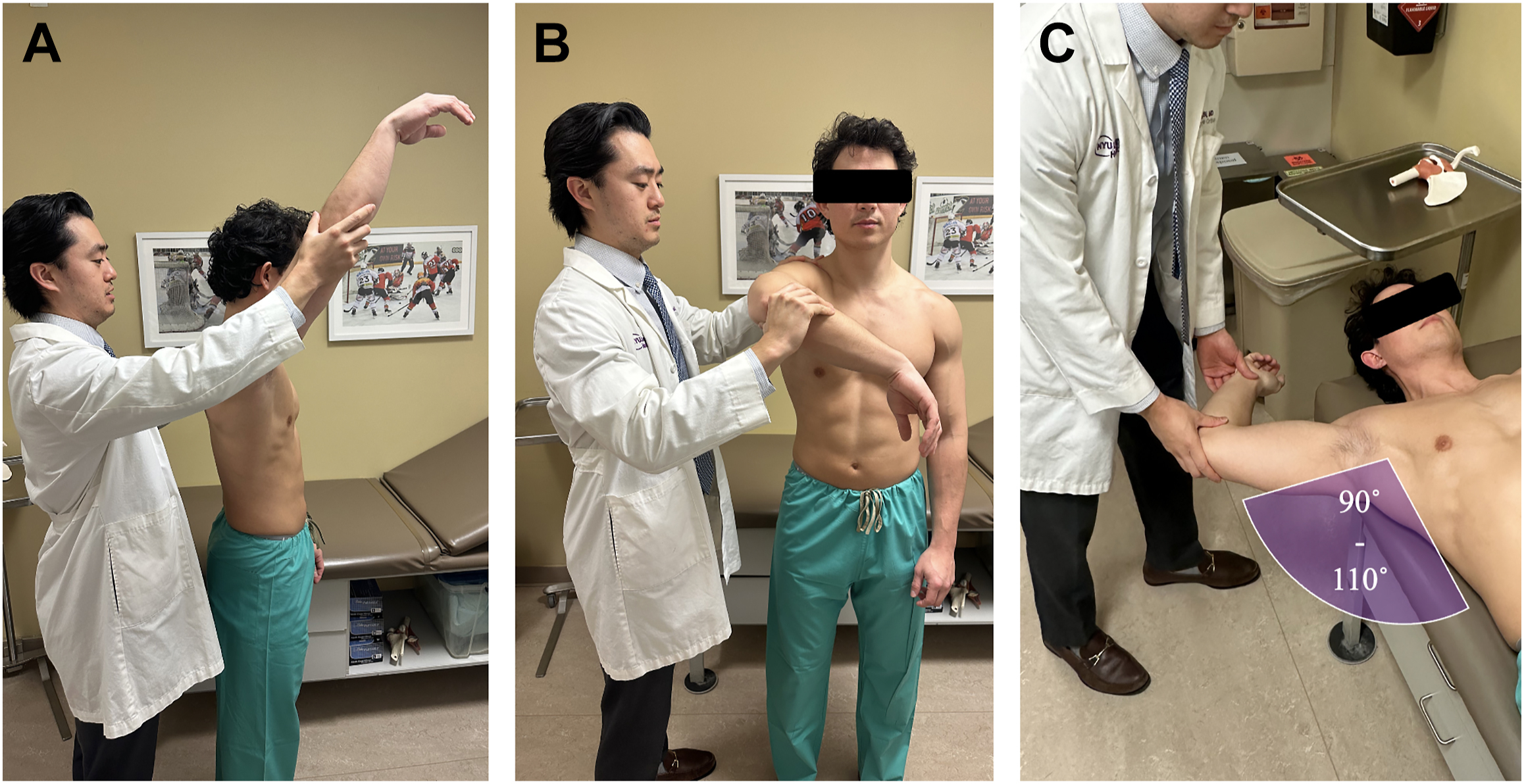
The PE of the rotator cuff has been shown to have a wide range of sensitivity (SN) and specificity (SP) for the ability to differentiate impingement, tendinosis, partial-thickness rotator cuff tears (PTRCTs), and full-thickness rotator cuff tears (FTRCTs). Impingement testing begins with Neer’s landmark publication in 1983, with descriptions as early as 1972. , The Neer Impingement Sign is elicited with the patient seated and the examiner behind, with one hand preventing scapular rotation while the other raises the patient’s arm in forced FE, causing the greater tuberosity to impinge against the acromion ( Fig. 1 A ). Neer proclaimed in this study the nonspecific nature of the testing and suggested further performance of the Neer Impingement Test , in which a 10 cc injection of 1.0% xylocaine is given in the subacromial space anteriorly, and the test is repeated, which increases the SP for external impingement. The Hawkins–Kennedy impingement test, described in 1980 as “another less reliable method of demonstrating this [external] impingement involves forward flexing the humerus to 90 degrees and forcibly internally rotating the shoulder, impaling the supraspinatus tendon against the anterior surface of the coracoacromial ligament,” and reported it more useful in the younger patient population or when considering when to resect the coracoacromial ligament ( Fig. 1 B). Hegedus and colleagues demonstrated in a meta-analysis the SN of the Neer and Hawkins–Kennedy tests to be 72% and 79%, with SP of 60% and 59%, respectively. Tests for internal impingement of the shoulder should be of particular focus in throwers given a high incidence of posterior capsular tightness, internal impingement, partial-articular rotator cuff tears, and IR deficits. These focus mostly around the Meister posterior impingement sign, described in 2004 by eliciting posterior pain , not apprehension, with bringing the shoulder into 90° to 110° abduction, slight extension, and maximum ER to impinge the posterior greater tuberosity/posterior labrum against the articular surface of the posterosuperior rotator cuff, describing an overall SN 75.5% and SP 85% ( Fig. 1 C). In vivo demonstration of internal impingement was first described by Paley and colleagues in 41 professional overhead throwing athletes, demonstrating arthroscopically contact between the rotator cuff articular surface and posterosuperior glenoid rim or greater tuberosity in 100% of subjects.
Supraspinatus, Infraspinatus, and Teres Minor Testing
The PE for PTRCTs and FTRCTs should focus on pain and/or strength deficits, although torn cuffs can be masked by normal strength and intact cuffs can be weak and painful. The Whipple test was described by Savoie in 2001 with the patient holding their shoulder FF 90°, partially adducted, palm down, and resisting a downward force by the examiner as a maneuver to test for PTRCTs of the supraspinatus ( Fig. 2 A ). Jobe and Moynes described the “empty can” (EC) test in 1982, isolating the supraspinatus maximally using electromyography (EMG) in a position of “90° abduction, 30° horizontal flexion, and full internal rotation,” while Kelly and colleagues reported modifications of 45° lateral humeral rotation (“full can” [FC]), best isolated the supraspinatus on EMG ( Fig. 2 B, C). , Ackmann and colleagues demonstrated SNs of 88.6%, 88.6%, and 75.0% and SPs of 29.4%, 58.8%, and 47.1%, for the Whipple test, EC, and FC test, respectively, while Sgroi and colleagues reported similar discrepancies between SN and SP, with superior positive predictive values (PPV; 0.88–0.93) compared to negative predictive values (NPV; 0.17–0.21). , The contributions of the deltoid remain a confounding factor in both EC and FC testing, and Chalmers and colleagues described the “Champagne toast test” to best isolate the supraspinatus from the deltoid on EMG testing, with the shoulder held in 30° abduction, mild ER, 30˚ FF, and 90° elbow flexion ( Fig. 2 D).
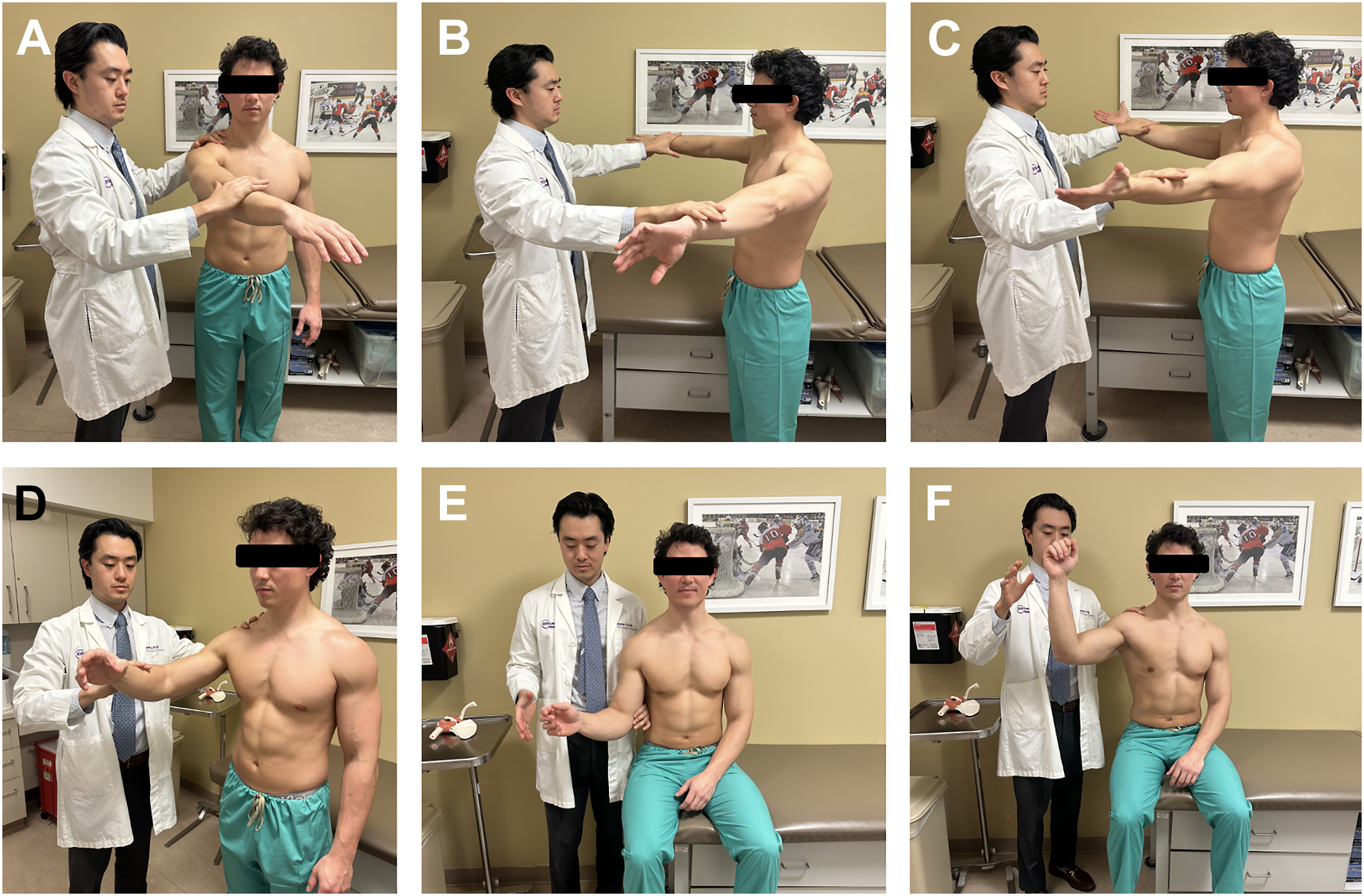
Infraspinatus integrity is best tested with ER strength against an examiner with the arm adducted 0° and IR 45°, as demonstrated by Kelly and colleagues’ EMG testing. Hertel and Gerber described the ER lag sign in 1996 (in addition to the drop arm test and IR lag sign) with the patient seated, examiner behind the patient, and the arm held in 0° adduction, 90° elbow flexion, 20˚ FE, near maximal ER (minus 5° to avoid elastic recoil) and then released, asking the patient to maintain the arm position ( Fig. 2 E). , The teres minor is similarly tested with the arm abducted to 90°. ER strength in this position best isolates the teres minor from the infraspinatus and posterior deltoid, and the inability to maintain this position with a lag indicates a positive Hornblower sign, which has been attributed to both Patte (and thus known as the Patte sign) and Arthuis, which demonstrated to have similar accuracy ( Fig. 2 F).
Subscapularis Testing
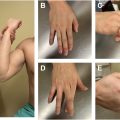
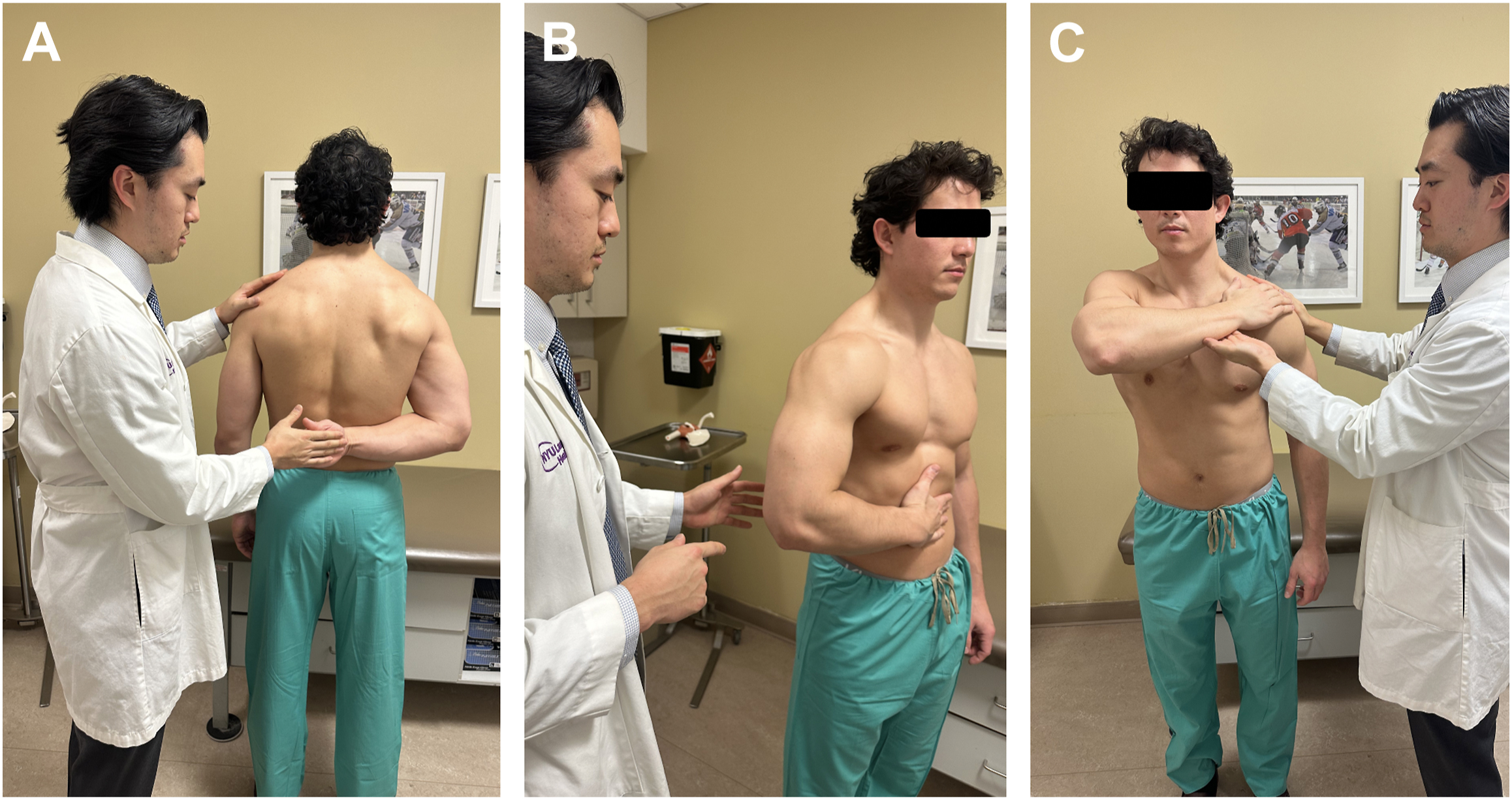
The subscapularis is a powerful internal rotator and stabilizer of the shoulder and should be tested for strength in 0° adduction, 90° elbow flexion, and neutral rotation. Several special tests can be divided into tests anterior to the body, which relatively isolates the upper fibers, and posterior, which relatively isolates the lower fibers. Gerber has been the primary pioneer behind subscapularis testing, describing his lift-off test in 1991 in 16 patients, with the dorsum of the hand at the mid-lumbar spine and then maximally IR. An inability due to pain or weakness was described as a positive test ( Fig. 3 A ). Gerber then moved anterior and described the belly-press test in 1996 for patients without the shoulder IR necessary for the lift-off test. The hand is instead pressed flat on the abdomen and attempts to keep the arm in maximal IR, and a positive test demonstrates the elbow sagging posteriorly ( Fig. 3 B). Modifications grading for wrist flexion to keep the elbow anterior have been coined the “Napoleon sign” for the position Napoleon would pose for portraits. Burkhart and De Beer later described the bear-hug test in 2006, in which the palm is held on the opposite shoulder like the cross-body adduction while resisting an ER force by the examiner on the volar forearm, and demonstrated the highest SN of the 4 (60% vs 40% belly-press, 25% Napoleon, and 17.6% lift-off) with excellent SP for all ( Fig. 3 C). Of note, the bear-hug test is notable, but negative, if pain is present, but positive only with the presence of IR weakness. Tokish and colleagues confirmed using EMG testing the isolation of the upper subscapularis with belly-press testing and lower subscapularis with lift-off tests, and Yoon and colleagues demonstrated highest SN with belly-press and highest SP with lift-off testing (96.9%–100%). ,
Biceps and superior labral pathology
Biceps Pathology
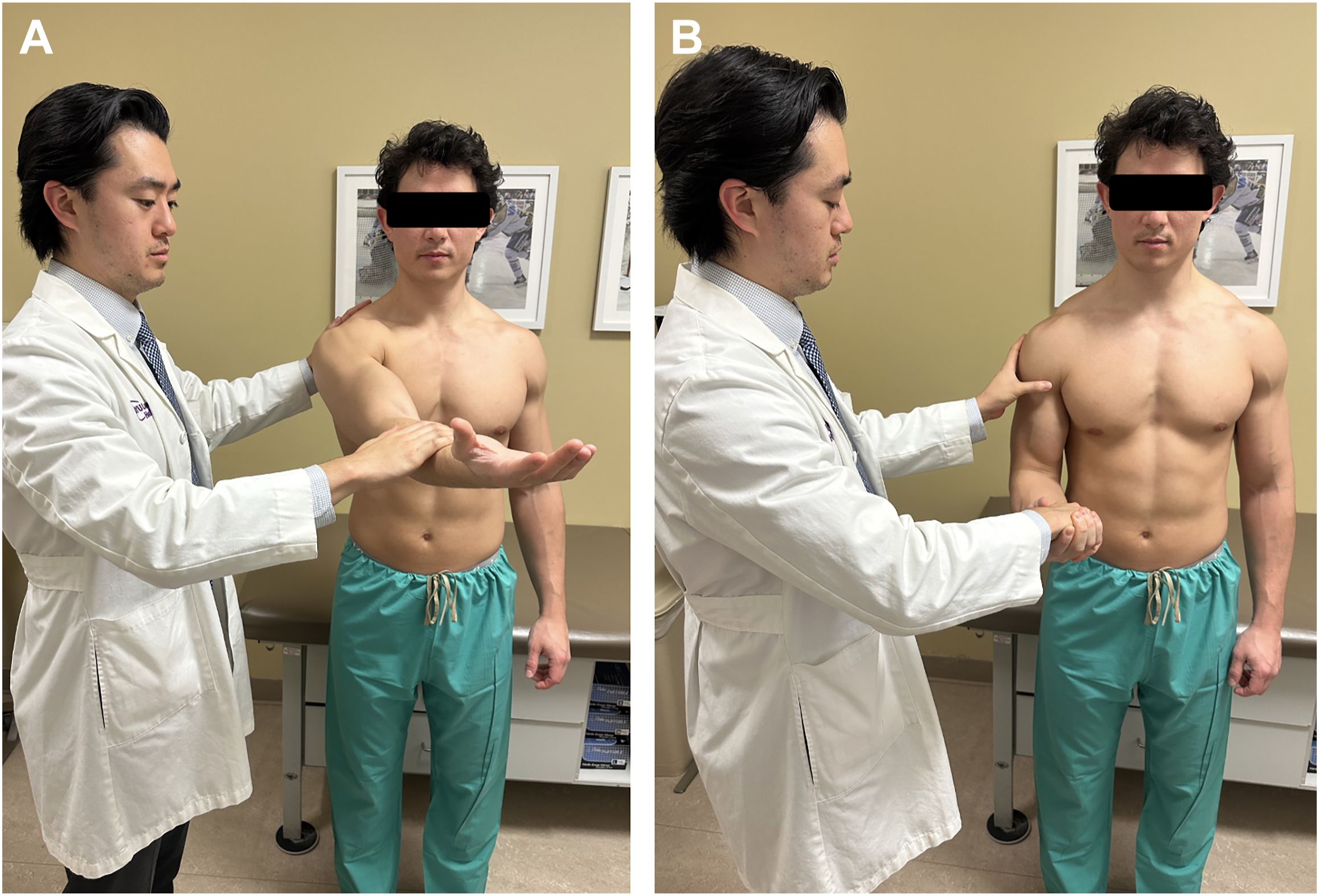
The long head of the biceps tendon (LHBT) can contribute to pain in the overhead athlete in the bicipital groove under the sheath contributions of the coracohumeral and transverse humeral ligaments, intra-articular portion, or at its attachment at the superior labrum. Bicipital groove pain can be evident on palpation and proximal ruptures can present with Popeye deformities on inspection. Speed’s test is an evaluation for both LHB tendinitis and its anchor for superior labrum anterior and posterior (SLAP) lesions. The position of the arm is that which James Spencer Speed, Chief of Orthopedics at the Campbell Clinic, himself had bicipital groove pain while lifting his patients’ legs for straight leg raise testing—hand supination, elbow extension, and shoulder flexion—and was actually described by his colleagues Crenshaw and Kilgore in 1966 at the Campbell Clinic ( Fig. 4 A ). , Yergason described his “Supination Sign” in 1931 in a woman with suspected bicipital tendinitis due to handwashing a large amount of clothes that resolved after purchasing a washing machine. , He performed his test with resisted wrist supination with the shoulder adducted and elbow flexed 90° and considered bicipital groove pain a positive examination ( Fig. 4 B). Studies using arthroscopic confirmation report superior SN and NPV, while others report opposing superior SP and PPV for the Speed’s and Yergason’s tests. , Taylor and colleagues reported improved SN (73%–98%) and moderate SP (46%–79%) with the grouping of the PE into a “3 pack” of O’Brien active compression test, throwing test, and biceps groove palpation, which has later been modified to include a lidocaine injection into the bicipital groove for a “4 pack” test.
Superior Labrum Anterior and Posterior Lesions
SLAP lesions affect a high proportion of overhead throwers and can be difficult to isolate from other diagnoses due to its high rate of concomitant pathology, with a 22% to 73% incidence of Bankart lesions to PTRCTs. , Special tests can be roughly divided into general tests, designed simply to trap torn labrum between the humeral head and glenoid, and those that mimic the peel-back mechanism that occurs during the throwing position of shoulder abduction and maximum ER. From Snyder’s compression-rotation test in 1990 (supine patient, shoulder abducted 90°, elbow flexed 90°, with axial load and rotation of the humerus), Andrews’ clunk test (supine patient, shoulder abducted 135°, with anterior translation of one examiner hand, and axial load and rotation of the humerus with the other hand grasping the elbow), Liu and colleagues’ crank test (patient upright, shoulder FE 160°, with axial load and rotation of the humerus), Kibler’s anterior slide test (patient upright with their hands on hips and thumbs posterior, one examiner hand stabilizing the patient’s AC joint, and the other hand axial loading at the elbow anterior and superior), or Kim and colleagues passive compression test (patient lateral decubitus with affected shoulder up at 30° abduction, stabilize AC joint and scapula, and axial load and ER through the elbow), these “mortar and pestle” tests have been described with a variety of modifications ( Fig. 5 ). , O’Brien described his active compression test in 1998, holding the patient’s arm in 90˚ FF, 10° to 15° adduction from behind, full elbow extension, and providing a downward force with the patient’s hand in maximal pronation and supination, with a positive test indicated with “internal pain” or clicking with pronation, and either relieved by supination, or transfer of pain to the AC joint area.