Craniofacial clefts are extremely rare. In 1976, Paul Tessier developed a comprehensive numerical classification system to categorize craniofacial clefts based on precise anatomic location. In order to comprehend craniofacial cleft development, it is crucial to understand embryologic development of the face. Craniofacial clefts can be classified into 4 main categories: oral-nasal (number 0–3), oral-ocular (number 4–6), lateral face (number 7–9), and cranial (number 10–14). Treatment goals include restoring oral competence and function, achieving nasal symmetry, establishing separation of anatomically distinct cavities, addressing orbital asymmetries, hypotelorism, or hypertelorism, and reconstructing cranial defects caused from encephaloceles.
Key points
- •
Craniofacial clefts are rare disorders diagnosed by characterization of the bony defect with computed tomography imaging as patients can have variable phenotypic appearances. The designated Tessier location will provide insight into the involved components of the face to guide surgical management.
- •
The goal of surgical repair is to restore anatomic features of the oral, nasal, and ocular compartments of the face. Each surgical plan is individualized to address both function and cosmesis, and will often require complex, staged repairs.
- •
Bony defects may involve structural components requiring grafting, osteotomy, distraction, or cranial resurfacing. Facial bipartition or box osteotomies may be necessary to address hypertelorism.
- •
Soft tissue reconstruction can be approached using the principles of cleft lip repair and flaps described in facial reconstruction. Canthopexy is helpful when the orbit is involved, and attention to the lacrimal system may be needed as in Tessier 3 clefts.
Introduction
Craniofacial clefts are extremely rare, with an estimated incidence of 1.43 to 4.85 cases per 100,000 births and have posed a formidable challenge to surgeons since antiquity. Before the advent of Paul Tessier’s groundbreaking work, classifications were rudimentary, and treatment options were limited. Early classifications relied on descriptive features rather than the precise anatomic delineations we use today. Surgical interventions were fraught with high complication rates and inconsistent outcomes, leaving patients and surgeons alike frustrated with the lack of success in managing these complex anomalies.
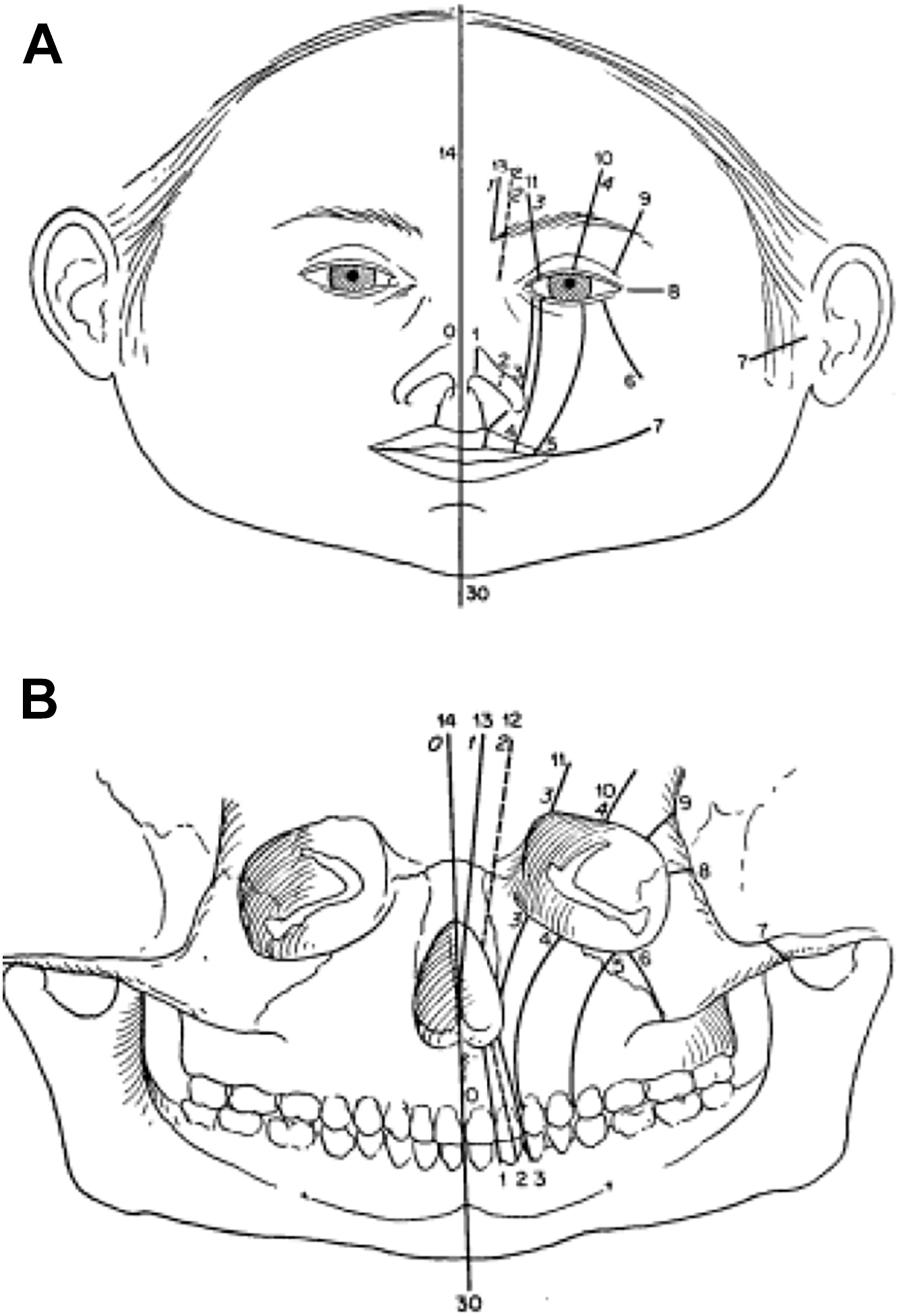
The landscape of craniofacial surgery, however, was revolutionized with the arrival of Paul Tessier. His meticulous anatomic studies and innovative surgical techniques marked a turning point for managing craniofacial anomalies. In 1976, Tessier introduced a comprehensive classification system, numbered 0 to 14 and 30, to categorize craniofacial clefts based on precise anatomic locations ( Fig. 1 ). The cleft is identified by the location of the skeletal defect, using the orbit as the primary reference structure. This framework provided a standardized approach to treatment, laying the foundation for modern craniofacial surgery. Consequently, craniofacial clefts, distinct from cleft lip or palate, are often referred to as “Tessier clefts.”
Background
The anatomic classification of craniofacial clefts is rooted in the location of the bony defect. This is because of an important relationship between the bony and soft tissues purported by Tessier, “a fissure of the soft tissues corresponds with a cleft of the bony structures . ” Prior to his definition, clefting anomalies like those seen in Treacher Collins were historically described and understood as hypoplasia. “Clefting” refers to a failure of fusion between 2 adjacent embryologic structures, which can lead to hypoplasia at the cleft edges and affect the appearance of the surrounding soft tissue. However, the cellular processes of hypoplasia or dysplasia do not in themselves result in the dramatic interruption of the bony tissue seen in clefting. Therefore, the clinical appearance alone cannot classify a craniofacial cleft and care must be taken to preserve the appropriate terminology.
While the Tessier classification remains the most clinically relevant, other classifications systems and theories offer additional insights into the phenotypic variability and underlying pathophysiology. One critique was the lack of explanation for varying soft tissue and bony involvement within his orderly classification. For instance, soft tissue is often more severely affected from the midline to the infraorbital foramen, while bone is typically more severely affected lateral to the infraorbital foramen. In 1983, Van der Meulen introduced his embryological-based classification of clefting, intended as an addition rather than a replacement of Tessier’s description. He believed the classification to be incomplete without a relationship to the underlying embryology to explain the phenomena. This article will integrate Tessier’s anatomic classification with related concepts from the literature to offer a comprehensive understanding of these rare craniofacial malformations.
Facial embryology
An understanding of embryologic events and the facial prominences is essential to this topic. Facial development of the fetus occurs between the third and eighth week of gestation via the convergence of 5 mesenchymal prominences along predictable embryonic lines: the frontonasal prominence, medial and lateral nasal processes, maxillary, and mandibular processes. , ( Fig. 2 ).
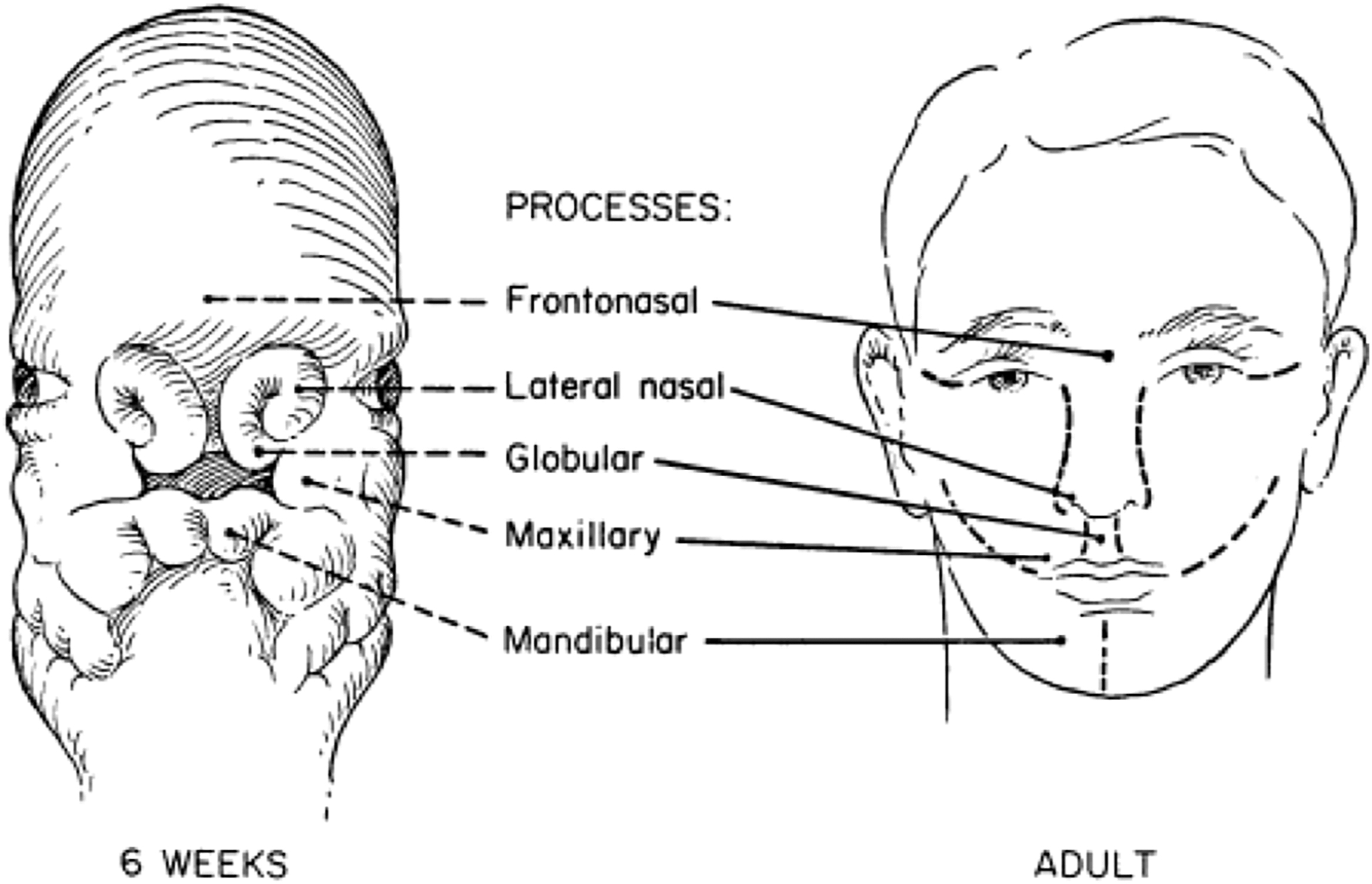
In the third and fourth week, the frontonasal prominence arises from neural crest mesenchyme and forms bilateral ring-like thickenings of nasal placodes, later giving rise to the lateral and medial nasal processes. At 4 weeks, the frontonasal prominence and forebrain comprise the majority of the upper midface. The stomodeal membrane gives way and depresses to create an opening for the mouth above the mandibular arch. The first pharyngeal or mandibular arch bifurcates into the maxillary and mandibular processes and migrates to the midline to form the lower and upper mouth, respectively. , ,
During the fifth week, the medial and lateral nasal processes arise from the placodes and the central placode deepens to form olfactory pits. In week 6, the medial nasal processes merge at the midline to form centralized midface structures (nasal tip, columella, philtrum, premaxilla). This medial nasal process unites with the maxillary processes to form the upper lip. The lateral nasal process gives rise the nasal alae on each side of the face. The nasal dorsum is formed from the frontonasal process. , ,
The mandibular processes merge at the midline by week 6. At the same time, 3 hillocks appear on the caudal border of the mandibular arch which merge with 3 corresponding hillocks on the cephalic border of the hyoid or second brachial arch forming the external ear. By the eighth week of gestation, all 5 facial prominences are typically fused under normal physiology. ,
Cleft pathogenesis
Craniofacial morphogenesis refers to the cellular processes involved in the fusion of the above facial processes. While it is widely understood that clefting results from some type of failed processes during the fusion of facial prominences, there are differing theories regarding the pathogenesis. The “classic” theory, originally described by Dursey in 1869, relies on the assumption of facial processes as free ends with an epithelial lining that coalesces at union. When epithelial contact is made, a remaining ectodermal groove must be obliterated to allow mesodermal elements to merge. If the epithelium between the 2 facial processes fails to degenerate, fusion will not take place. ,
This concept was questioned by Pohlman in 1910 and Veau in 1938, and further challenged by Stark in 1964. And a new theory emerged based on mesodermal migration and penetration. Proponents of this theory do not believe in the presence of free ends to the facial processes. Instead, they propose that the face consists of a bilamellar membrane of ectoderm with epithelial seams delineating the facial processes. Mesenchymal penetration occurs at these epithelial seams, resulting in the smoothing out of the seam. If mesenchymal penetration does not occur, the unsupported epithelial seams will dehisce and a cleft will be formed. Depending on the degree of mesenchymal penetration, an incomplete or less severe cleft may form. ,
In 1939, Hoepke and Maurer supported a combination of these 2 theories regarding the development of craniofacial clefts. They concur that the failure of fusion results in cleft formation, but believed mesenchymal penetration to be the embryo’s attempt to repair the cleft. Similarly, the updated Van der Meulen classification aligns with the classical understanding that failed fusion contributes to the origin of “primary clefts.” They introduce the term “pseudo-clefts” to elucidate phenotypic variations, which they attribute to an event occurring later in development, after fusion is complete. In such cases, there is an inadequate outgrowth of ossification centers from the respective prominence to the site of contact, disrupting normal ossification and behaving like a scar that impedes the expansion of surrounding tissue. While this event occurs at anatomic Tessier cleft locations, the authors feel this represents a dysplastic process rather than a true cleft.
The Tessier classification: presentation and treatment goals
The Tessier classification is an anatomic system to describe craniofacial clefts. Tessier considered the orbit as the landmark transition point between the cranium and underlying facial skeleton, making it the primary reference point. The malformations are named 0 through 14 based on axes in which line 0 is the vertical midline of the midface. Each cleft is described in detail later and summarized in ( Table 1 ).
| Number (Extension) | Oral | Nasal | Orbit | Syndromes |
|---|---|---|---|---|
| Tessier Clefts | ||||
| Oro-nasal | ||||
| 0 (14, 30) | Midline Dental : Between central incisors | Broad, bifid | Hypertelorism | |
| 1 (13) | Cupid’s bow Dental : lateral incisor | Nostril dome Bone: medial piriform rim | Hypertelorism | |
| 2 (12) | Cupid’s bow Dental : lateral incisor | Mid-alar rim Bone : medial piriform rim | Hypertelorism | |
| 3 (11) Nasomaxillary Dysplasia | Cupid’s bow Dental : lateral incisor | Alar base Bone : Lateral piriform rim | Medial lower eyelid coloboma Bone : medial maxillary wall & IOR | |
| Oro-ocular | ||||
| 4 (10) | Between cupid’s bow and oral commissure Dental : Canine | None | Medial third lower eyelid Bone : Medial IOR | |
| 5 (9) | Medial to oral commissure Dental : Lateral to canine | None | Middle third lower eyelid Bone: Middle IOR | |
| 6 Maxillozygomatic Dysplasia | Dental : Maxilla 2nd molar | None | Lateral third lower eyelid Bone : Lateral IOR | Treacher Collins |
| Lateral facial | ||||
| 7 Zygomaticotemporal Oromandibular Dysostosis | Oral commissure Dental : Maxilla 2nd molar, supernumerary teeth Duplicate maxilla | None | None Cheek deformity, external ear | Treacher Collins, Goldenhar, Hemifacial microsomia |
| 8 | None | None | Lateral canthus Bone: Lateral OR | Treacher Collins |
| 9 (5) | None | None | Lateral third upper eyelid/brow Bone : Lateral third SOR | |
| Cranial | ||||
| 10 (4) | None | None | Middle third upper eyelid/brow Bone : Middle third SOR | |
| 11 (3) | None | None | Medial third upper eyelid/brow Bone : Medial third SOR | |
| 12 (2) | None | Bone: Ethmoid labyrinth, frontal process maxilla | Medial eyebrow | |
| 13 (1) | None | Bone: Nasal bone, cribriform plate | Medial eyebrow | |
| 14 (0) | All midline structures, christal galli | All midline structures | All midline structures | |
Craniofacial clefts classified into 4 categories: oral-nasal, oral-ocular, lateral facial, or cranial clefts. Oral-nasal clefts (number 0–3) occur in the midface between the midline and cupids bow, distorting the lip and nose. Oral-ocular clefts (number 4–6) occur lateral to cupids bow and do not affect the nose. They extend through the soft tissue of the cheek and maxilla connecting the oral and ocular cavities. They can also referred to as oblique facial clefts or “meloschisis.” , Lateral facial clefts (number 7–9) extend laterally involving the zygomatic arch or orbit and are often associated with a syndrome. Cranial clefts (number 10–14, 30) extend superiorly from the lateral orbit to the midline and proceed through the frontal bone, and not infrequently the cranial base.
Oral-Nasal Clefts (Number 0–3)
Cleft number 0: medial nasal processes
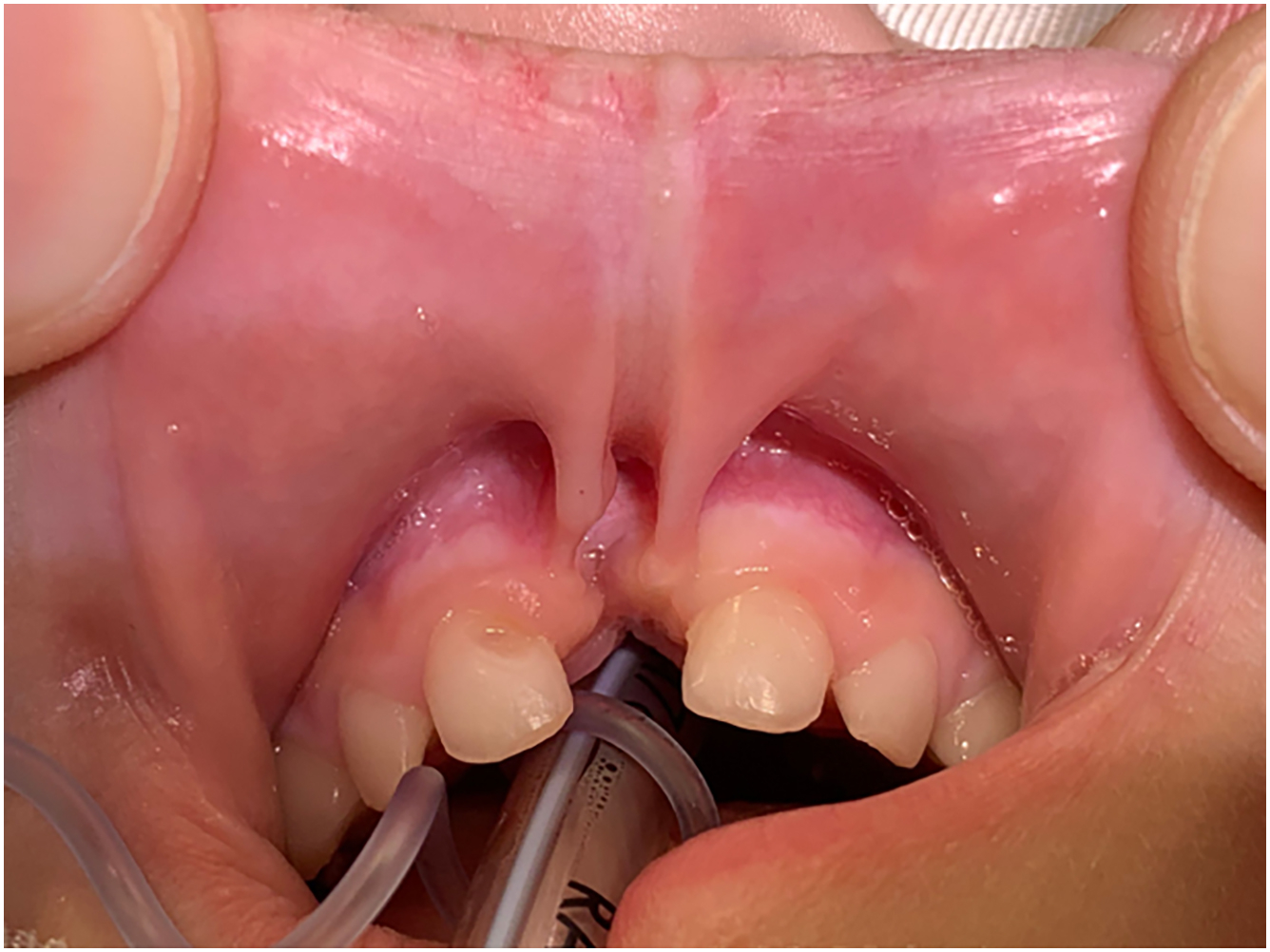
This is a more common craniofacial cleft and results from the failed fusion of the medial nasal processes ( Figs. 3 and 4 ). The medial nasal processes merge at the midline in week 6 to form the centralized midface structures: nasal tip, columella, philtrum, and premaxilla. As such, presentation typically includes a bifid nose with either deficient or excess midline structures. In severe cases, the nasal tip is absent and the nostrils are completely separate, causing significant orbital hypertelorism. This may also appear with absent anterior lip, nasal bones, and premaxilla resulting in cleft palate. When hyperplastic, the nasal septum can be thickened or duplicated with a flat or furrowed nasal dorsum, short and wide columella, and widened forehead with hypertelorism. It may uncommonly present with frontonasal encephalocele, holoprosencephaly, or a range of mental disabilities. A continuation superiorly as a number 14 cleft is also possible.