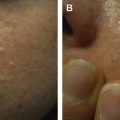
Acne vulgaris, a disorder of the pilosebaceous unit, is one of the most commonly encountered conditions in dermatology practice. Effective treatment of acne vulgaris is important in that it can prevent psychosocial distress and physical scarring. Systemic therapeutic options are available for moderate to severe acne. It is imperative that the safe and effective treatment revolves around the health care provider’s familiarity of side effects of various treatments. In this article, the side effects and monitoring guide for the most commonly prescribed systemic agents for acne vulgaris are reviewed.
Key points
- •
Minocycline-induced autoimmunity and hypersensitivity reactions have been increasingly reported in the last few decades.
- •
Doxycycline is rarely associated with serious adverse effects over more recent years.
- •
There is literature to support that routine monitoring of serum potassium levels in healthy young women taking spironolactone for acne is not necessary.
- •
Ocular adverse effects of isotretinoin may need to be communicated to the patients more actively for better safety monitoring.
- •
Low-dose intermittent isotretinoin regimen has been reported effective.
Introduction
Acne vulgaris is one of the most commonly encountered conditions in dermatology practice. It is a disorder of the pilosebaceous unit and affects about 33% of individuals between the ages 15 and 44 years, primarily adolescents. Effective treatment of acne vulgaris is important in that it can prevent psychosocial distress and physical scarring. Various therapeutic options are available according to the severity of the disease. Although a broad proportion of patients with acne can be successfully treated using topical agents such as benzoyl peroxide, topical antibiotics, and topical retinoids, patients with moderate to severe inflammatory acne require systemic therapy. This article is a concise review of side effects and monitoring guide for the most commonly prescribed systemic agents for acne vulgaris.
Introduction
Acne vulgaris is one of the most commonly encountered conditions in dermatology practice. It is a disorder of the pilosebaceous unit and affects about 33% of individuals between the ages 15 and 44 years, primarily adolescents. Effective treatment of acne vulgaris is important in that it can prevent psychosocial distress and physical scarring. Various therapeutic options are available according to the severity of the disease. Although a broad proportion of patients with acne can be successfully treated using topical agents such as benzoyl peroxide, topical antibiotics, and topical retinoids, patients with moderate to severe inflammatory acne require systemic therapy. This article is a concise review of side effects and monitoring guide for the most commonly prescribed systemic agents for acne vulgaris.
Tetracyclines
Tetracyclines are the most commonly prescribed antibiotics for the treatment of acne. Compared with the original tetracycline, the second-generation synthetic molecules, doxycycline and minocycline, offer easier dosing schedules and are more readily absorbed when taken with food. They are bacteriostatic and work on inhibition of bacterial protein synthesis. Serious side effects associated with tetracyclines are rare in its use for acne, but as an antibiotic class, more common side effects of doxycycline and minocycline include gastrointestinal symptoms with nausea, vomiting, and diarrhea; pediatric teeth discoloration; central nervous system effects such as dizziness and light headedness; and candidiasis. Photosensitivity and photo-onycholysis are also seen, however, sun protection with daily sunscreen wear may help prevent treatment-related sunburns. Doxycycline and minocycline offer similar efficacy for management of acne, but they differ in their side-effect profiles. Recent literature reviews have compared the safety profiles of doxycycline and minocycline.
In their systematic review of safety of doxycycline and minocycline, Smith and and Leyden noted that there were more than 3 times as many new prescriptions for doxycycline than for minocycline in the United States from 1998 to 2003. And the adverse event rates for the same period were 5 times greater for minocycline than doxycycline based on the US Food and Drug Administration’s MedWatch Adverse Event reporting program data. Analysis by Smith and Leyden also found that gastrointestinal effects were the most common adverse effects related to doxycycline use, whereas central nervous system and gastrointestinal effects were most common with minocycline. In this 2005 article, Smith and Leyden made an observation regarding the kinds of adverse effects that differed from clinical trials and published case reports. For doxycycline, the types of adverse effects in published case reports were similar to those reported in clinical trials. However, those for minocycline were significantly different, with events that range from minocycline-induced drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome with persistent myocarditis to minocycline-induced autoimmunity (MIA). The authors noted that case reports represent something of clinical interest to the medical community and generally reflect less frequent but more serious adverse effects. However, taken collectively, the patterns of reported adverse events can suggest a causal relationship between the drug and event, justifying further investigation.
According to Kircik in his 2010 article, data indicate that MIA may lead to chronic symptoms, persisting from 13 to 48 months. Pathogenesis of MIA has not yet been established, although it is suspected to be similar to other drug-induced autoimmunity. Female patients are more commonly affected than male patients. The average age of onset of MIA was between 13 and 18 years with mean duration of minocycline therapy of 13 months for those with transient MIA, 14.6 months for those with intermediate, and 11.8 for those with chronic MIA. The median estimated cumulative minocycline dose in each of the 3 groups was 72 g, and most patients had a positive family history of autoimmune disorder.
Minocycline is also associated with potentially fatal hypersensitivity syndrome or DRESS. Predictive factors are not well defined, but recent evidence suggests that minocycline-induced DRESS occurs mainly in patients with Fitzpatrick skin phototypes V and VI. Although the incidence of minocycline-induced DRESS is rare, its widespread use necessitates awareness among physicians who are initiating systemic antiacne therapy in patients, especially those with skin types V and VI.
Doxycycline, however is viewed as the safest within the tetracycline class, with fewer reported cases of side effects. It is available in 2 different formulations: doxycycline hyclate and doxycycline monohydrate. Doxycycline hyclate is more acidic than doxycycline monohydrate and may be associated with a higher risk of esophageal ulceration if the drug is taken without sufficient water. The development of enteric-coated doxycycline hyclate has been linked to a decrease in gastrointestinal side effects. Also, taking it with adequate amount of water is found to significantly decrease the risk of esophageal ulceration. Studies support the benefit of enteric-coated doxycycline to decrease nausea, vomiting, and abdominal pain compared with both conventional doxycycline hyclate capsule and doxycycline monohydrate. Despite its favorable safety record, several serious doxycycline-induced adverse reactions have emerged over the last few years. There are several case reports of doxycycline-induced pseudotumor cerebri in acne patients and DRESS syndrome after doxycycline treatment. One case of doxycycline-induced cutaneous inflammation with systemic symptoms was also reported in a 15-year-old patient taking doxycycline for 2 years. A brief summary of adverse reactions to minocycline and doxycycline is outlined in Table 1 .
| Antibiotic | Adverse Reaction | Studies |
|---|---|---|
| Minocycline | Vomiting/abdominal pain/diarrhea | Smith & Leyden, Kircik |
| Vertigo/dizziness/light headedness/ataxia | Smith & Leyden, Kircik, Meynadier & Alirezai | |
| Candidiasis | Smith & Leyden, Kircik | |
| Photosensitivity/photo-onycholysis | Sloan & Scheinfeld | |
| Bluish discoloration of the skin | Tan | |
| DRESS | Shaughnessy et al, Eshki et al, Maubec et al | |
| MIA—lupus, autoimmune hepatitis, serum sickness, vasculitis | Elkayam et al, El-Hallak et al, Matsuura et al, Sturkenboom et al, Schlienger et al, Seaman et al | |
| Pneumonitis | Christodoulou et al | |
| Doxycycline | Vomiting/abdominal pain/diarrhea | Smith & Leyden, Kircik, Story et al, Jarvinen |
| Dizziness/light headedness | Smith & Leyden, Kircik | |
| Candidiasis | Smith & Leyden, Kircik | |
| Photosensitivity/photo-onycholysis | Sloan & Scheinfeld, Edwards | |
| Acute generalized exanthematous pustulosis | Trueb & Burg | |
| Esophageal ulceration | Kircik, Sloan & Scheinfeld, Berger | |
| Pseudotumor cerebri | Tabibian & Gutierrez, Friedman et al | |
| DRESS (data very limited) | Robles et al, Mailhol et al | |
| Cutaneous inflammation with systemic symptoms (15 y-old patient taking doxycycline daily for 2 y) | Weinstein et al |
Spironolactone
Although not approved by the US Food and Drug Administration for the treatment of acne, spironolactone, a medicine that blocks androgen receptors, is found to be effective in treating acne vulgaris, at daily dosage of 100 to 200 mg, in most women and adolescent girls, especially those with worsening acne associated with menstrual cycle. The incidence of side effects at this dose may be high, ranging from 75% to 91%, but the severity is generally mild with good tolerance by most women. Reported side effects included menstrual irregularities and central nervous system side effects such as headache and dizziness. More recent data support the efficacy of lower doses of spironolactone at 50 to 100 mg daily, which were much better tolerated. The main side effect reported at this dose was mild, clinically insignificant elevation of serum potassium levels. Plovanich and colleagues most recently report the results on the monitoring of serum potassium level for this potential hyperkalemia among healthy young women taking spironolactone for acne in their electronically published article in March 2015. Based on their data from a retrospective study of 974 healthy young women taking spironolactone from 2000 to 2014, they noted 13 abnormal serum potassium measurements in 1802 measurements obtained. This finding yielded a rate of 0.72% for hyperkalemia compared with 0.76% baseline rate of hyperkalemia in this population. Furthermore, the repeat testing in 6 of 13 patients found normal values, suggesting that the findings might have been erroneous. Considering this new establishment of hyperkalemia incidence, which is equivalent to the baseline rate in this population, Plovanich and colleagues concluded that routine potassium monitoring is unnecessary in healthy young women taking spironolactone for acne. A list of reported adverse reactions associated with spironolactone is outlined in Table 2 .
| Reaction Pattern | Studies |
|---|---|
| Menstrual irregularities | Shaw, Shaw, Hughes & Cunliffe, Shaw, Yemisci et al, Lubbos et al |
| Breast tenderness or enlargement | Shaw, Cunliffe & Simpson |
| Headache | Shaw, Lubbos et al |
| Fatigue | Shaw, Shaw |
| Dizziness | Shaw, Yemisci et al |
| Drowsiness | Shaw |
| Nausea/vomiting/diarrhea/anorexia | Shaw, Shaw |
| Decreased libido | Shaw |
| Hyperkalemia | Shaw, Plovanich et al |
| Melasma | Shaw |
| Facial swelling | Lubbos et al |
Isotretinoin
The clinical adverse effects of isotretinoin can be grouped into 2 categories: mucocutaneous and systemic. Of the adverse effects reported, those that occur with highest incidence are mucocutaneous in nature and usually noticeable within the first week of therapy. This effect is caused by changes in mucosal surfaces and skin that have been altered in the barrier function from the reduction in sebum production leading to thinning of the stratum corneum.
Most patients have dryness and fissures on the lips, skin, and mucosa. Lip dryness occurs in 100% of the cases and cheilitis in 95% of the cases. This dose-related cheilitis is so common that some elucidate it is a marker of the action of the isotretinoin. On the other hand, complete absence of cheilitis may suggest noncompliance or malabsorption of the drug. Dryness of the nasal and oral mucosa have been reported in 50% and 40%, respectively. Dry eyes and blepharoconjunctivitis develop in 25% of the patients and are controlled with eye lubricants.
The ocular side effects tend to be less emphasized despite their frequent report along with lip dryness. Neudorfer and colleagues looked at the study population of 14,682 adolescents and young adults who were new users of isotretinoin for acne and 2 age- and sex-matched comparison groups. They described the most common adverse effects and evaluated the period of highest risk. The most common adverse effects in Neudorfer’s study included conjunctivitis, hordeolum, chalazion, blepharitis, eye pain, and dry eye, which is in agreement with findings from previous studies. Development of these ocular adverse effects took place with the peak increased risk at 4 months after the first dispensed isotretinoin prescription, advocating for a follow-up visit to the ophthalmologist around that time. The results of this study underscore the importance of proper prevention and management measures and the most optimal timeframe to detect any significant ocular adverse effects. Ocular lubricants such as preservative-free artificial tears can be prescribed, but in more severe cases, topical ophthalmologic antibiotics may be needed. The health care provider must be aware of these potential side effects when educating patients, because some events are reported to be irreversible, even during periods of acute exposure to isotretinoin.
In 2010, Brito and colleagues published a study in which they evaluated the clinical adverse effects and laboratory alterations in patients with acne treated with oral isotretinoin. Of the 150 patients, the frequency of the mucocutaneous adverse effects was similar to that found in the literature. Cheilitis (94%) was the most common followed by xeroderma and dryness of mucous membranes (47%). Despite this high rate of mucocutaneous effects, symptoms were managed with lip balm and body moisturizers, eye drops, and ophthalmologic evaluation, and none of the effects served as a reason to suspend the drug in Brito’s study. They also noted the incident of pyogenic granuloma in 13% of the cases but without any case resulting in the suspension of isotretinoin. There was a report of 3 cases of granulomalike reactions in 66 patients (4.5%) treated with isotretinoin for nodulocystic acne. Pyogenic granulomalike reactions developed in previous acne lesions and led to discontinuation of the drug in 2 of them. The exact incidence of pyogenic granuloma or granulomalike reactions secondary to the use of isotretinoin is unknown.
Mucocutaneous effects usually persist throughout the treatment course but have been documented to be reversible at the time of dosage reduction or discontinuation of the drug. Most of these effects can be efficiently managed through the use of mild soaps, facial washing limited to once a day, avoidance of concurrent use of other acne medications, use of hydrating moisturizers, use of sunscreen, and frequent lip lubrication with a petroleum product. Patients should be instructed to avoid cosmetic procedures such as dermabrasion, waxing, and laser treatment for up to 6 months after isotretinoin therapy because of complications including potential keloid formation and delayed wound healing.
The systemic toxicity of retinoid may affect bones, muscles, gastrointestinal tract, central nervous system, lungs, ears, and kidneys. Isotretinoin use by patients with acne usually does not cause serious bone changes. Although hyperostosis are considered irreversible, they are generally asymptomatic and insignificant even with long-term use. In addition to hyperostosis, case reports of premature epiphyseal closures have been described with high doses of isotretinoin, but it may be reversible. Myalgia can occur, especially in patients who exhibit vigorous physical activity. In general, however, elevation in creatine phosphokinase level is relatively uncommon and usually reversible. Myalgia can usually be controlled with nonsteroidal anti-inflammatory drugs. Adverse gastrointestinal effects related to isotretinoin therapy seem to be reversible after therapy cessation and range from nausea and other nonspecific gastrointestinal effects to pancreatitis, hepatitis, appendicitis, esophagitis, and colitis. There are conflicting reports regarding the possibility of isotretinoin causing or exacerbating the symptoms of inflammatory bowel disease ; however history of inflammatory bowel disease does not seem to be an absolute contraindication for isotretinoin use for nodulocystic or recalcitrant acne among current practitioners. Neurologic reactions reported to occur with isotretinoin use are rare. They include idiopathic increases in intracranial pressure, confusion, dizziness, drowsiness, seizures, lethargy, malaise, nervousness, syncope, weakness, paresthesias, stroke, and pseudotumor cerebri presenting with headache, nausea, vomiting, and visual disturbances. Such symptoms should be carefully discussed, and a referral to a neurologist may be warranted. Despite the adverse pulmonary effects associated with isotretinoin therapy, specific pulmonary events such as bronchospasm and asthma exacerbation have been noted. Monitoring of the pulmonary function may be required in individuals with this response for proper reduction of dose or termination of therapy. Among other uncommon events that are reported in the literature, hearing impairment is significant to recognize, as it does not disappear after the suspension of isotretinoin. The mechanism that causes this deterioration in hearing is unknown, and patients must be evaluated by otorhinolaryngologist. Besides hearing impairment, tinnitus has also been described. Other nonspecific hearing problems were identified by Brito and colleagues in 2010, which did not lead to suspension of the drug. Adverse renal effects related to isotretinoin use are rare, with a few cases of glomerulonephritis, urethritis, and proteinuria. These renal abnormalities resolve after discontinuation of isotretinoin therapy.
With regard to psychiatric effects attributed to isotretinoin, controversies exist over a causal relationship between treatment with isotretinoin and psychiatric symptoms with the reports of depression, psychoses, suicidal thoughts, and suicide attempts. However, there are doubts about this association. A 2001 cohort study conducted in Canada looked at 7535 patients treated with isotretinoin and 14,376 patients treated with oral antibiotics. The study compared the relative estimated risk of suicide among patients with acne treated with isotretinoin or oral antibiotics, but an association between isotretinoin use and an increased risk of suicide was not found. Physicians’ concerns for the psychiatric adverse effects have not subsided, and continuing efforts with educating patients, especially those with a history of depression, to immediately report changes in moods or behavior, suicidal thoughts, or feelings need to be regularly practiced.
Among the adverse side effects of isotretinoin, teratogenicity is considered the most serious. Specific teratogenic effects involve craniofacial, cardiac, thymic, and central nervous system structures. These findings have resulted in a stringent management of the medication with birth control policy, which includes 2 pregnancy tests before initiation of therapy, 2 forms of contraception to be used throughout the therapy, contraception education, and the required informed consent for patients. All patients should re-review the information in the informed consent form at each monthly follow-up visit. It is imperative that only 1-month supply of isotretinoin be prescribed at any office visit after documentation of the absence of pregnancy. Patients must be counseled that pregnancy prevention should continue 1 month after discontinuation of therapy. It is a standard practice at some dermatologists’ offices to formulate these into a checklist and use as protocol for initial and follow-up appointments.
In addition to monthly pregnancy testing, review of any laboratory alterations are necessary before continuing isotretinoin therapy. Of the laboratory abnormalities, liver functions tests and lipid abnormalities are most critical to assess. Despite the fact that 5% to 25% of patients treated with isotretinoin show some abnormalities in the liver function tests, most of these cases are without any histologic liver changes, and the elevated levels of hepatic enzymes return to normal after discontinuing isotretinoin therapy or with dose reduction. As a general rule, dose reduction should be considered when the liver function results are 2- to 3-fold their normal value, and if they do not decrease with dose reduction after 2 weeks, discontinuation of isotretinoin may be necessary. Elevations of transaminase levels greater than 3 times the upper normal value warrant immediate cessation of therapy. Monitoring of liver function is especially critical in patients with underlying liver disease or history of hepatitis. It is recommended that health care providers also educate patients on the concomitant use of hepatotoxins, such as alcohol and other drugs, which may contribute to hepatic function test abnormalities. Evaluation of liver function tests at baseline before isotretinoin therapy and at follow-up appointment at each month is a standard safety practice in this regard. Lipid abnormalities are another well-documented adverse effect of isotretinoin therapy requiring a sound monitoring. These effects include decreased serum levels of high-density lipoprotein cholesterol, increased serum levels of very low-density lipoprotein cholesterol and low-density lipoprotein cholesterol, and increased serum total cholesterol levels. Increased triglyceride levels are seen in 25% to 45% of patients on isotretinoin. Although significant variations of serum lipid and lipoprotein levels do not affect the overall risk of atherosclerosis in young and healthy patients on short courses of isotretinoin, continuous isotretinoin use in patients with underlying lipid disorders may lead to an increased risk of cardiovascular event. Although rare, cases of isotretinoin-induced pancreatitis secondary to hypertriglyceridemia have also been reported. For this reason, if pancreatitis is suspected, or if hyperlipidemia is not controlled with antihyperlipidemic medicines, it is important to suspend isotretinoin use. In general, dose reduction or the introduction of antihyperlipidemic agent is considered when triglyceride level exceeds 500 to 600 mg/dL in an otherwise asymptomatic patient. Other reversible and dose-dependent laboratory abnormalities reported in the literature are decreased white blood cell and neutrophil counts, increased platelet counts, thrombocytopenia, and increased erythrocyte sedimentation rates.
Other adverse effects that are less common but worthwhile to note are photosensitivity, pruritus, hair loss, and skin infections. Photosensitivity appears in 40% of the cases. Pruritus, scaly skin, and worsening of atopic dermatitis occur in 25%. Telogen effluvium may be found in up to 25% of the patients, resolving after discontinuation of the isotretinoin treatment. Skin infections caused by Staphylococcus aureus may develop because of an increase in its colonization resulting from a reduction in sebum production.
The aforementioned use of oral isotretinoin in conventional dose administration has been limited by its reported side effects including mucocutaneous adverse effects, teratogenicity, depression with suicidal ideation, and biochemical abnormalities, such as impaired liver function and hyperlipidemia. The low-dose intermittent isotretinoin regimen was devised as a low-cost alternative to the conventional dose regimen, also in effort to reduce the occurrences of adverse effects of isotretinoin. The low-dose intermittent regimen consists of isotretinoin, 0.5 mg/kg/d for 1 week in every 4 weeks for a total period of 6 months. The efficacy of this regimen for mild to severe acne has been established by different studies. Various fixed low-dose isotretinoin regimens have also been emerged, and one such regimen with fixed low-dose isotretinoin, 20 mg/d and 20 mg on alternate days for a total period of 6 months, is found to be effective in moderate acne. Previous data exist to support that the frequency and severity of mucocutaneous side effects were lower with this low-dose intermittent regimen than with conventional isotretinoin therapy. In an uncontrolled, open-label observational study, Kumar and Kumar evaluated hematologic, biochemical, and radiologic abnormalities associated with low-dose intermittent isotretinoin therapy at 0.5 mg/kg/d for 1 week every 4 weeks for a duration of 6 months. In their study, liver function results, including total bilirubin levels and transaminase levels, remained within normal limits in all cases. Increase in cholesterol to borderline-high levels (200–239 mg/dL) was observed in 8.3% cases, whereas increase to high levels (≥240 mg/dL) was observed in only 5% of cases after low-dose intermittent isotretinoin. Compared with 30% elevation in cholesterol levels after conventional dose of isotretinoin, the results added to the safety data of low-dose intermittent isotretinoin therapy favorably. Elevation in triglycerides and low-density lipoprotein levels revealed similar outcomes. Furthermore, neither the radiologic changes consistent with diffuse interskeletal hyperostosis of the spine nor the hematologic changes such as leukopenia and increased platelet counts were observed in any case in the Kumar study.
Throughout the last 20 years, the frequency of rigorous laboratory monitoring has decreased, and some of the recent studies show that there is no need for laboratory follow-up in patients taking isotretinoin. Although there remains a resistance to the use of isotretinoin, especially for milder cases of acne that are irresponsive to conventional therapies, isotretinoin can now be viewed as a reasonably safe drug in relation to adverse effects when the patient is well monitored.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree