Rotator cuff and biceps tendon injuries are a common source of pain and dysfunction among overhead athletes. The stress across the glenohumeral joint and its dynamic stabilizers in high level throwing leads to adaptive anatomic changes that must be recognized and respected. Nonoperative treatment is recommended for partial rotator cuff tears and biceps tendinitis and tendinosis. Surgical treatment is indicated for persistent symptoms despite conservative treatment. For rotator cuff repairs, it is critical to avoid over-tensioning as this will lead to the loss of range of motion and lower rates for return to play.
Key points
- •
Nonoperative management is effective for the majority of rotator cuff and biceps pathology in the thrower’s shoulder.
- •
Arthroscopic rotator cuff repair should respect adaptive changes incurred in the throwing athlete.
- •
Avoid over-tensioning the rotator cuff repair to maintain range of motion and exacerbating internal impingement.
- •
Biceps tenodesis is an option for biceps tendon tears, extreme tendinitis, subluxation, and incarceration that failed conservative treatment.
Video content accompanies this article at http://www.sportsmed.theclinics.com .
Introduction
The repetitive forceful dynamics of throwing a baseball creates shoulder injury risk. Shoulder injury risk is further propagated by deficiencies of the shoulder girdle or imbalanced mechanics in the kinetic chain. Rotator cuff injury is a common source of pain and dysfunction in the baseball athlete due to the tremendous stresses imparted on the dynamic stabilizers of the shoulder with repetitive acceleration, deceleration, and overhead motion during throwing. , The long head of the biceps (LHB) tendon is another common source of pathology in overhead athletes, representing the fourth most common injury among professional baseball players. Successful management of rotator cuff and biceps injuries requires a comprehensive understanding of the underlying pathoanatomy, symptoms, treatment options along with a thorough evaluation of the shoulder girdle, scapula, kinetic chain, and throwing motion.
This article describes the pathoanatomy of throwing athletes, theories for rotator cuff involvement in throwers, evaluation of rotator cuff tears, the role of the biceps in the shoulder and reviews current treatment options for rotator cuff and biceps tendon pathology in baseball players.
Pathoanatomy
The rotator cuff consists of 4 muscles about the shoulder girdle: the subscapularis, supraspinatus, infraspinatus, and teres minor. Through the phases of throwing, the rotator cuff incurs both concentric and eccentric stresses. During windup, rotator cuff activity is largely absent; however, as the thrower progresses from early to late cocking, the posterosuperior rotator cuff concentrically contracts bringing the arm into external rotation. Next, the acceleration phase concentrically activates the subscapularis and other shoulder internal rotators to contract. In the internally rotated position, the thrower completes their follow-through phase, decelerating their arm through eccentrically contracting the posterosuperior rotator cuff. Electromyography (EMG) activity in the posterosuperior cuff has been shown to be highest during the follow-through phase. Andrews and colleagues theorized tearing of the posterosuperior rotator cuff could represent a tension phenomenon experienced from the eccentric stress during follow-through.
There are several theories as to how rotator cuff injuries occur in the throwing athlete. These include internal impingement, posterior capsular contracture, and adaptive changes. The throwing shoulder has unique adaptive capacity that leads to altered biomechanics compared to the contralateral non-throwing shoulder. For example, professional pitchers have increased humeral retroversion (average of 17°) compared to contralateral non-throwing shoulder. The anterior capsule had developed increased laxity. The posterior capsular thickening or contracture limits internal rotation and is referred to as glenohumeral internal rotation deficit (GIRD). Moreover, biomechanical data indicate that posterior capsular contracture increases force between the coracoacromial ligament and the rotator cuff.
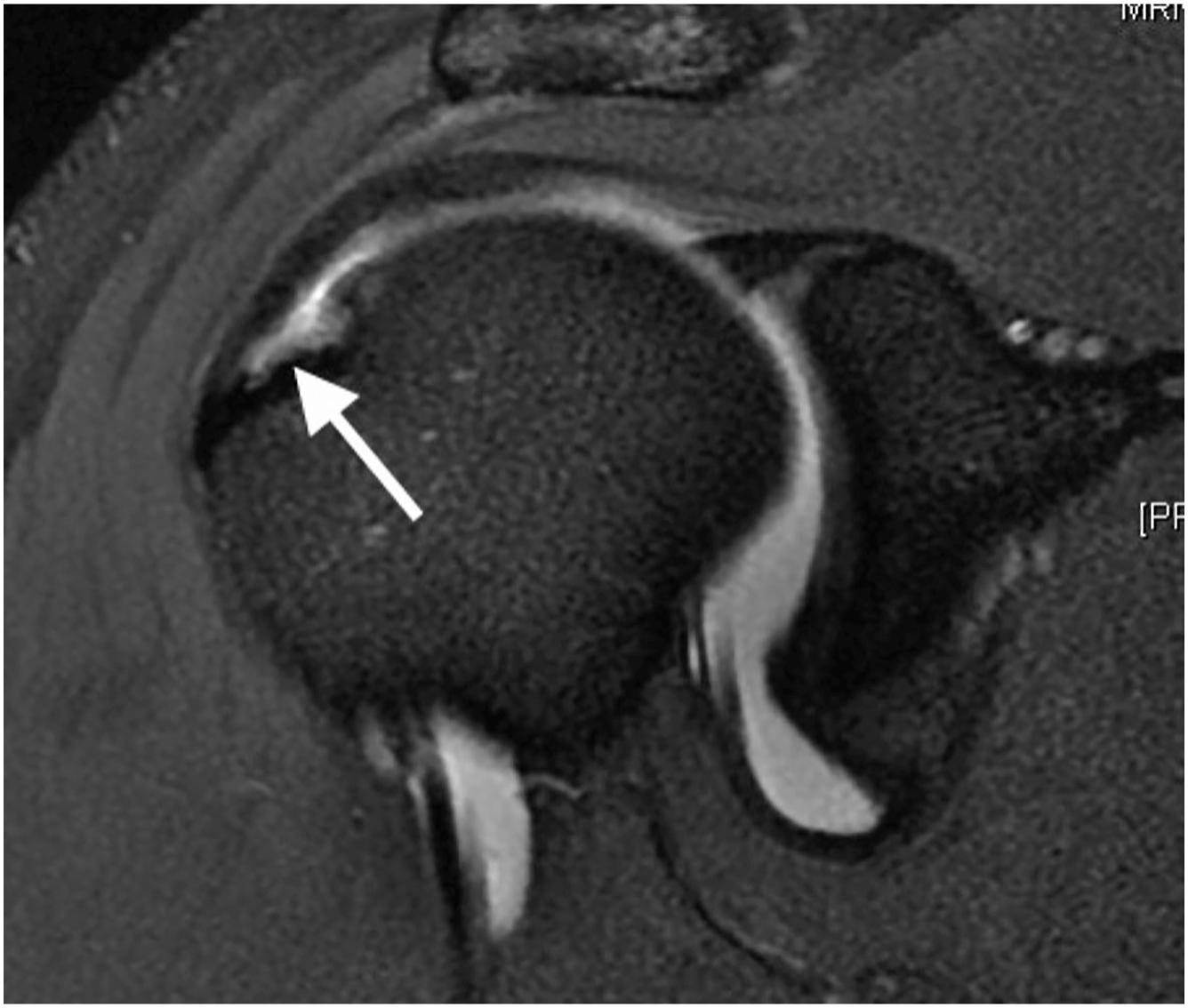
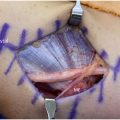
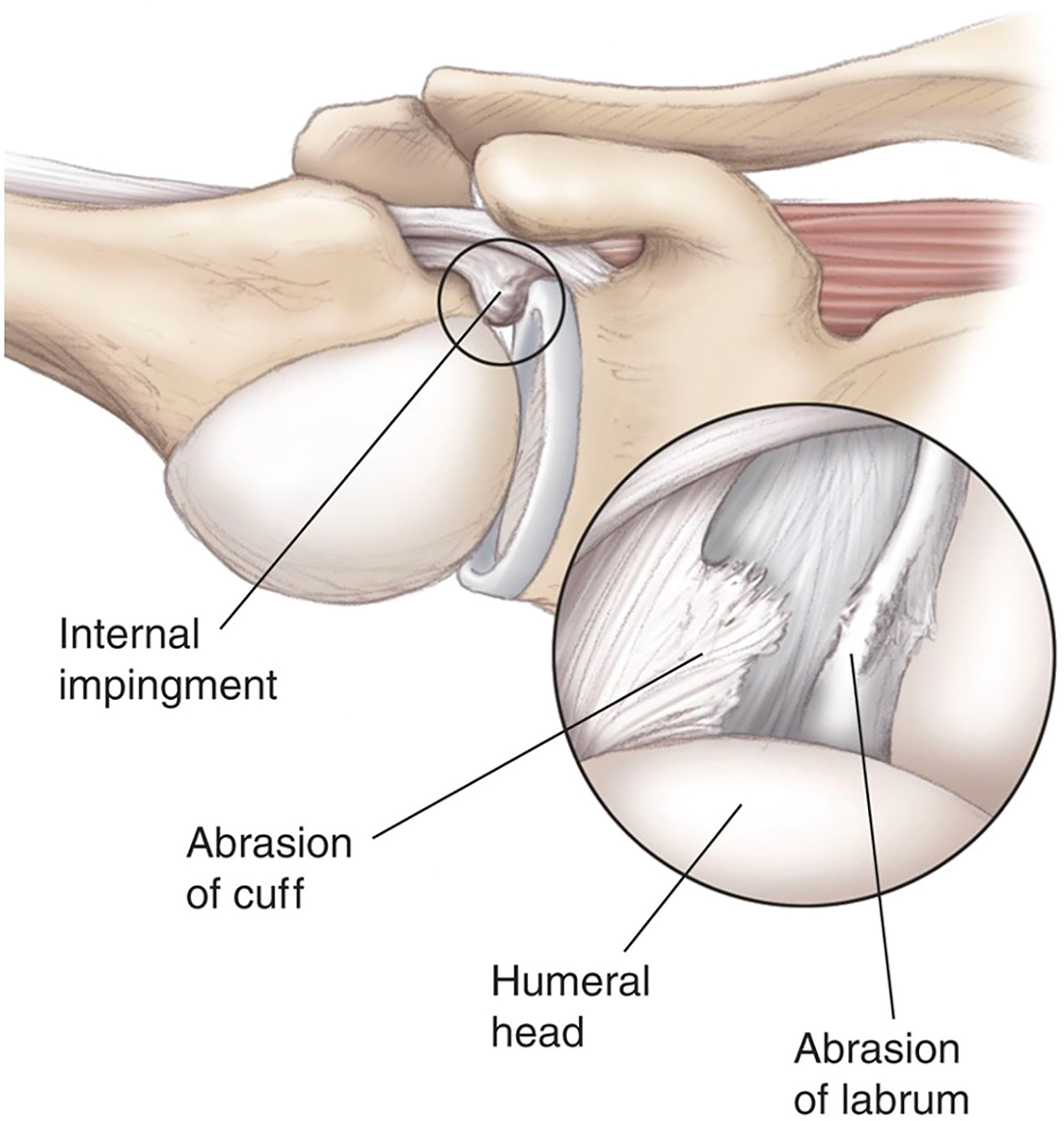
Initially observed by Walch and colleagues, the term internal impingement describes the natural phenomenon of contact between the articular surface of posterior supraspinatus and superior infraspinatus along the posterior superior glenoid when the arm is placed in 90° of abduction and 90° of external rotation. In an arthroscopic study, McFarland and colleagues noted a variety of arm positions can lead to impingement and it is the repetitive nature that leads to rotator cuff issues. Burkhart and colleagues viewed internal impingement as a natural variant with the shear and torsional forces experienced by the rotator cuff due to posterior capsular contracture. Ultimately, this leads to abnormal humeral head motion and a posterior superior shift of the center of rotation when the arm is placed in hyperexternal rotation. While total arc of motion could be preserved in GIRD, as the throwing motion progresses to the maximally abducted and externally rotated position, the contracted posterior capsule initiates a pathologic cascade. This cascade results in relative posterior superior translation of humeral head, loosening of the anterior inferior glenohumeral ligament, and placement of the undersurface of the posterior supraspinatus and anterior infraspinatus into contact with the posterior superior glenoid. (p1), It is important to note that asymptomatic rotator cuff tears are common in baseball players and considered adaptive for internal impingement ( Fig. 1 ). Sabick and colleagues reported the throwing shoulder in professional baseball pitchers experiences a degree of both repetitive angular velocity and forces across the joint that surpasses the torsional failure limit in human cadavers. Lesniak and colleagues, in the MRI study of asymptomatic major league pitches, reported a correlation between higher cumulative innings pitched and increased likelihood of rotator cuff tear, independent of symptoms. Partial rotator cuff tears in baseball pitchers may be asymptomatic as a result of these adaptive changes in contrast to the rare full-thickness tears which are more commonly associated to a single traumatic event, often seen in contact athletes. In fact, studies report more than 40% rate of completely asymptomatic partial articular lesions in professional pitchers. Therefore, the presence of positive imaging findings in asymptotic throwers may warrant no intervention or treatment.
The biceps is a common source of pain in baseball players. The studies focused on understanding biceps role within the shoulder can be divided into cadaveric biomechanical studies, EMG studies, and in vivo biomechanical studies. Cadaveric studies by Pagnani and colleagues and Itoi and colleagues showed that the LHB provided anterior stability to the glenohumeral joint in abduction, external rotation, and under load. , According to both studies, load on the biceps tendon increased in the setting of shoulder instability. Building on that, Rodosky and colleagues found that the LHB contributes to anterior stability by increasing resistance to torsional forces in the abducted and externally rotated position. After detaching the biceps from the labrum, the inferior glenohumeral ligament saw significantly increased strain. Youm and colleagues showed that a loaded biceps significantly altered glenohumeral (GH) translation, range of motion (ROM), and kinematics compared to an unloaded biceps. Last, Su and colleagues showed that biceps loading decreased superior glenohumeral translation in rotator cuff tears, regardless of the size of the tear.
Outcomes from EMG studies have been slightly more variable on the biceps’ role in the shoulder. Per Sakurai and colleagues and Chalmers and colleagues, even with the elbow immobilized, the LHB provided stability to the humeral head. , These studies highlighted the importance of the biceps as a dynamic stabilizer in the shoulder. In contrast, Levy and colleagues showed that the biceps only played a functional role in the shoulder when activated by elbow and forearm motion. Pertaining to baseball specifically, Jobe and colleagues evaluated biomechanics of pitching and found that biceps activates during 2 phases: during cocking to accomplish elbow flexion and again during follow-through to decelerate the forearm.
Evaluation
History
Evaluation begins with history, physical examination, and imaging. Players’ pathology often presents with diminished athletic performance and deep-seated shoulder pain with overhead activity. For pitchers, the impetus for seeking care commonly relates to decrease in velocity, strength, and location. Although bicipital groove pain with mechanical symptoms may be indicative of biceps pathology, overlap in symptoms with concomitant shoulder pathology may limit diagnostic accuracy and obscure clinical decision-making. It is important to discern a traumatic or pathologic tear from adaptive changes in the history based on the recall of a specific event preceding the symptoms.
Physical Examination
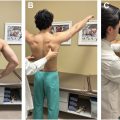
The physical examination begins with visual inspection of the entire shoulder girdle, exposed with the shirt off, with an emphasis to assess for side-to-side differences in the appearance of the shoulder, thoracic spine, scapula, and any areas of atrophy. Selective atrophy of the supraspinatus and/or infraspinatus fossa may indicate suprascapular nerve compression and often manifests similar to rotator cuff tear symptoms. Moreover, attention to scapular motion is critical for assessment of scapula dyskinesis in the throwing athlete, which presents with asymmetric position or protraction of the scapula with range of motion. Palpation of acromioclavicular joints, sternoclavicular joint, and biceps tendon follows as areas of potential point tenderness.
Following inspection, a side-to-side comparison of range of motion for forward elevation (in the scapular plane), external and internal rotation in the abducted position, external and internal rotation at the side, and abduction is performed (ideally in the supine position). Note differences in rotation as GIRD presents with decreased internal rotation in abduction in the throwing shoulder compared with the contralateral shoulder with preservation of total arc of rotation for both sides. Strength may also be simultaneously assessed in these planes of motion, again noting any asymmetry. Rotator cuff pathology may also be tested with provocative maneuvers for impingement which include Neer and Hawkins and lag signs, which are more indicative of massive cuff tears, atypical in the throwing athlete. It is important to note that rotator cuff injuries in the overhead athlete are generally not large enough to illicit weakness, but mild weakness may occur. Instead, these injuries more commonly manifest with impingement. Impingement can be external due to outlet narrowing of the supraspinatus (subacromial spur or coracoacromial [CA] ligament) versus internal where the undersurface of the supraspinatus contacts posterior superior glenoid, consistent with GIRD.
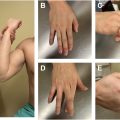
The most utilized test for LHB pathology is tenderness to palpation in the proximal biceps groove. It is important this is done on both sides simultaneously, as this can be a painful spot for many patients. Speed or Yergason test is done by having the patient forward elevate the shoulder against resistance while positioning the patient’s arm with elbow extended and forearm supinated. A positive test is when the patient localizes pain in the bicipital groove. More recently, the “3 pack” examination, defined by O’Brien, has been shown to provide a reliable and reproducible clinical assessment of the biceps-labrum complex. The examination is a combination of the following maneuvers performed in sequence: the active compression test, throwing test, and bicipital tunnel palpation. The active compression test (O’Brien sign) is performed by applying downward force against the patient’s resisted arm with the arm forward flexed to 90°, abducted 15°, and internally rotated such that the thumb points inferiorly. The maneuver is repeated with the palm facing upward. A positive test is indicated by deep-seated shoulder pain with the thumb pointed down that is subsequently eliminated or reduced with the palm facing upward. The throwing test is performed with the patient shoulder abducted to 90°, elbow flexed to 90°, and maximal external rotation (mimicking late-cocking position). The examiner provides isometric resistance countering the patient as they step forward with the contralateral leg and move into early acceleration throwing phase. Pain with examiner resistance is indicative of a positive test. Extra-articular bicipital tunnel disease, often poorly visualized on MRI and arthroscopically hidden, can be excluded by lack of tenderness to palpation and a negative active compression test.
Imaging
Standard radiographic evaluation should include Grashey, outlet, and axillary views of the shoulder to assess early degenerative changes, loose bodies, or bone reaction. Ultrasound may also serve as a convenient tool in the clinic setting for diagnosing some tears and biceps subluxation. In most cases, advanced imaging is necessary to clearly define the site of pathology when players are unable to return to prior performance levels. Noncontrast MRI is most often performed and can evaluate biceps pathology while also assessing for injuries to the rotator cuff, labrum, capsule, or articular surface. Given the high false-positive rate for intra-articular shoulder pathology in baseball players, it is important to correlate findings with a thorough history and physical examination.
Management
In regard to management of rotator cuff pathology, the mainstay initial treatment is nonoperative management. Nonoperative management for partial-thickness rotator cuff tears includes stretching of the posterior capsular tissues to address GIRD (sleeper stretches), strengthening programs for rotator cuff (including eccentric, plyometric exercises), periscapular strengthening, core and lower extremity exercises, improving flexibility deficits, optimizing training regimens (ie, pitching counts), restoring proper throwing mechanics, and injections. Optimizing training regimens includes cessation from throwing, typically for 6 week periods followed by a gradual return to throwing program for an additional 6 weeks. Location and type of injection (either corticosteroid or biologic) is dictated by the underlying pathology. Subacromial corticosteroid injections may provide relief for throwers with external impingement and bursal-sided pathology with goal to provide pain relief, reduce inflammation, and provide environment to restore proper throwing motion. Intra-articular corticosteroid injections are more indicated for articular-sided lesions. Biologic injections such as platelet-rich plasma (PRP) may also be considered for intra-articular pathology; however, literature remains sparse. Structured programs for rotator cuff injury (reinjury) prevention are also critical. Prevention begins with proper warm-up and strengthening of the core and kinetic chain along with a structured maintenance program. The Throwers Ten exercise program is organized, concise, and designed to exercise the major muscles of the shoulder complex necessary for throwing, focusing on improving endurance, strength, and power. ,
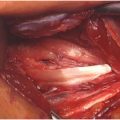
Operative treatment is reserved for those throwers who failed nonoperative management and those who were not able to adequately progress through a return to throwing program. There are important considerations when repairing the rotator cuff in the baseball athlete. The goal for surgical treatment of rotator cuff pathology in the baseball athlete is to respect the adaptive anatomic changes related to throwing aiming to avoid over-tensioning of the tendon as this will limit abduction and external rotation. For shallow articular sided tears, less than 50% of the footprint, arthroscopic debridement is indicated with the goal to debride the tear down to stable margins along with debridement of inflamed synovial tissue. These lesions are referred to as partial-thickness articular supraspinatus tear avulsion (PASTA) lesions. The concern regarding traditional repair in PASTA lesions is over-tensioning, as the lesions is more due to tissue loss than peel back phenomenon in non-thrower rotator cuff injuries. Lesions with delamination of the rotator cuff tear such that the articular side is detached and mobile from the bursal rotator cuff are referred to as partial-thickness articular surface intratendinous tears (PAINT) lesions ( Fig. 2 ). These lesions are managed with a side-to-side repair is indicated without anchoring tissue to the tuberosity ( Fig. 3 ). A subacromial evaluation and possible debridement is warranted; however, there is often no bursal rotator cuff pathology found. For deeper, near-full-thickness tears, traditional rotator cuff repair (RCR) to the tuberosity can be considered. Moreover, rotator cuff tears involving the rotator cable either anterior or posterior benefit from repair to the footprint.