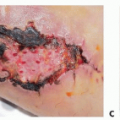
Reconstruction of Heel and Plantar Defects: Free Flap
Goo-Hyun Mun
Kyong-Je Woo
DEFINITION
Heel and plantar soft tissues perform a special role of weight bearing while walking or standing. The heel sustains up to 115% of body weight during slow walking and up to 260% of body weight during running.1
Heel and plantar defects may result from several causes such as trauma, diabetes, infection, peripheral vascular disease, frostbite injuries, and tumor resections.
The goal of reconstruction is aimed at not only providing stable wound healing but also achieving functional restoration of the salvaged limb and maintaining acceptable appearance.
ANATOMY
The weight-bearing plantar skin is a highly specialized part of the foot that is able to withstand and absorb the forces exerted during gait or running cycles. The epidermis and dermis are much thicker in plantar skin (“glabrous skin”) than in other parts of the body.
Subcutaneous fat in combination with the vertical fibrous connective tissue provides a cushioning effect to weight bearing.
The three arteries at the ankle level and their terminating branches in the foot that can be used as recipient vessels for free flaps include the anterior tibial-dorsalis pedis artery, posterior tibial-medial and lateral plantar artery, and peroneal-lateral calcaneal artery.
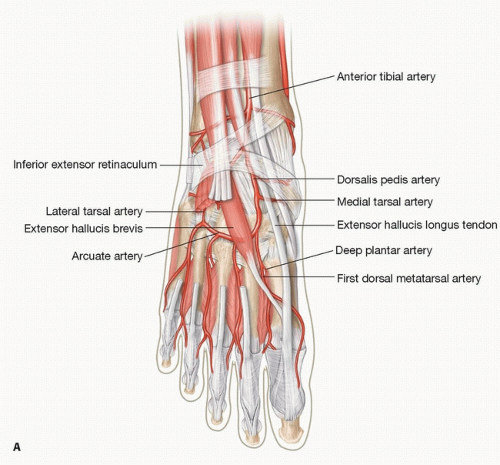
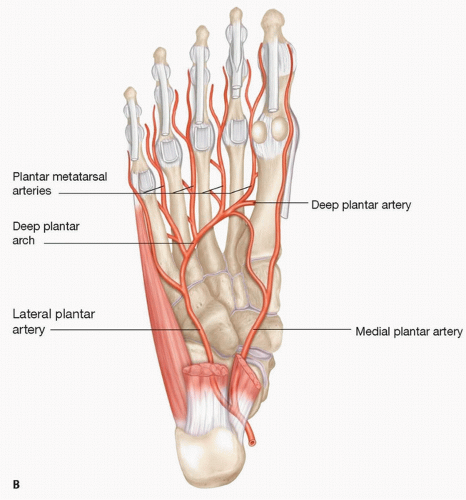
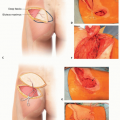
Anterior tibial-dorsalis pedis artery: the dorsalis pedis artery passes under the extensor retinaculum at the midpoint between the medial and lateral malleoli. It usually runs across and beneath the extensor hallucis longus (FIG 1A). It passes to the proximal end of the first intermetatarsal space, where it turns into the sole between the heads of the first dorsal interosseous to complete the plantar arch and provides the first plantar metatarsal artery
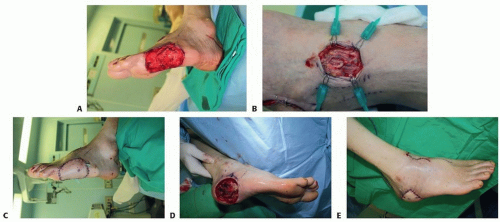
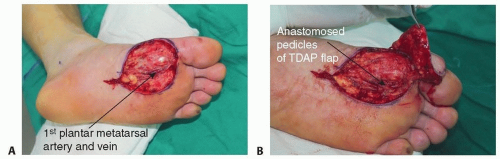
(FIG 1B). In heel and plantar reconstruction with a free flap, the dorsalis pedis artery can be reached for the recipient vessel by using a remote incision and subcutaneous tunneling (FIG 2). The first plantar metatarsal artery can be used in the plantar forefoot reconstruction (FIG 3).
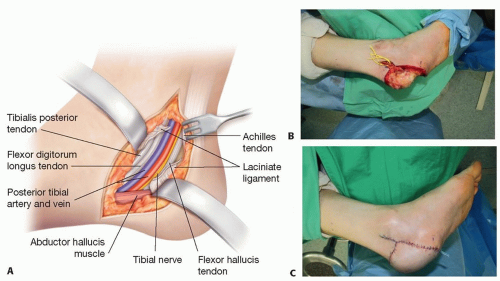
Posterior tibial-medial and lateral plantar artery: posterior tibial artery runs midway between the medial malleolus and the medial calcaneal tubercle under the laciniate ligament. It is located between the flexor digitorum longus and flexor hallucis longus tendons (FIG 4). The posterior
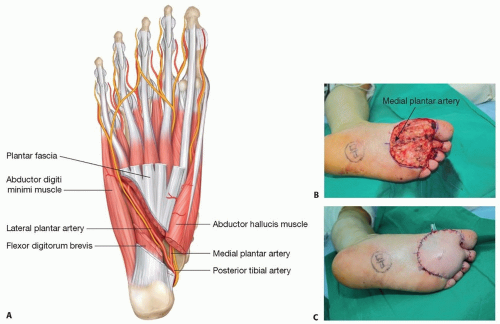
tibial artery divides into the medial and lateral plantar arteries under the origin of the abductor hallucis. While the medial plantar artery runs between the abductor hallucis and flexor digitorum brevis (FIG 5), the lateral plantar artery, being usually larger, travels from medial to lateral position under the proximal third of the flexor digitorum brevis and then continues distally between flexor digitorum brevis and abductor digiti minimi (FIG 6).
Peroneal-lateral calcaneal artery: peroneal artery terminates into lateral calcaneal artery around the lateral malleolus (FIG 7). The lateral calcaneal artery was introduced as a pedicle for local flap, but a recent anatomical study suggests that it could be used as a recipient blood vessels for free flap.2,3 The lateral calcaneal artery originates either from peroneal artery (80.3%), posterior tibial artery (13.1%), or a common branch from both the peroneal and posterior tibial arteries (6.6%) and runs between lateral malleolus and Achilles tendon.3,4
The principal superficial veins are termed long (great) and short (small) saphenous veins (FIG 8). The long (great) saphenous vein passes anterior to the medial malleolus, whereas the short (small) saphenous vein ascends from the lateral side of the foot. It ascends posterior to the lateral malleolus, passing along the lateral border of the Achilles tendon. A deep venous system runs near the corresponding arteries and develops communication with the great and small saphenous veins. Both deep veins of the corresponding arteries and the superficial veins can be selected as recipient veins in the foot.
PATIENT HISTORY AND PHYSICAL FINDINGS
A thorough medical history and examinations for sensation and presence of diabetes, peripheral vascular disease, and existence of osteomyelitis need to be obtained. Deformities of the foot and a postoperative rehabilitation plan should also be considered in the selection of reconstruction methods.
Vascular anatomy and patency must be evaluated. In this regard, noninvasive Doppler ultrasound exam is a simple and useful evaluation method. Recently, computed tomography (CT) or magnetic resonance (MR) angiography methods are also recommended for vascular imaging.
IMAGING
The authors routinely perform preoperative CT angiographic examination of the lower extremities, except when contraindicated.
Bone assessment includes plain radiography and bone scan or MR imaging for the diagnosis of osteomyelitis.
SURGICAL MANAGEMENT
For large and extensive heel and plantar defects, the free flap transfer procedure is preferred because it can provide a large amount of tissue with various tissue components
for obliterating deep and/or extensive wounds. The early and definitive reconstruction of compound defects leads to a dramatic improvement in the rate of lower extremity salvage and restoration of the weight-bearing function and normal gait pattern.
The final choice of most suitable flap depends on the surgeon’s preference and the patient’s needs. A form of durable, permanent, pain-free, and functionally and aesthetically satisfying coverage should be achieved in the heel and plantar reconstruction.
Free muscle flap versus fasciocutaneous flap: free muscle flap (rectus abdominis, latissimus dorsi, or gracilis) has been used commonly for extensive foot defects. A muscle flap has advantages, including the large amount of tissue availability, and ability to obliterate dead space especially in defects with irregular contours, where there is greater ease
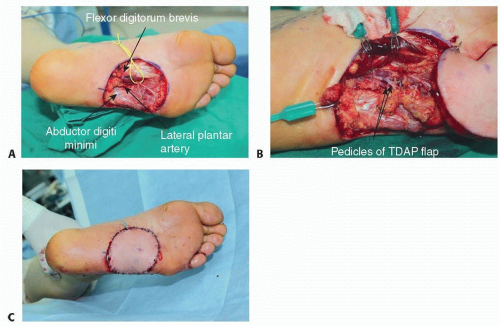
to form three-dimensional (3D) shapes.5 In contrast, recent clinical studies have demonstrated that fasciocutaneous flaps (anterolateral thigh, thoracodorsal artery perforator [TDAP] flap) provide a sufficient amount of bulk, large, and pliable skin flap, with acceptable donor site morbidities.6,7 The donor site morbidities caused by harvesting the muscle flap and additional donor site for skin graft can be avoided by using the fasciocutaneous flap.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree